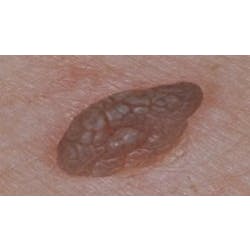
Have you ever been puzzled by red, inflamed tissue around a crown? What caused it and what can be done about it? Patients don't want to hear the word "replacement," and replacing it with a "better" crown may not even solve the problem. The problem may be caused by bacterial plaque accumulation, margin integrity, crown contour, metal sensitivity, or margin location. According to Dr. John Kois, a restorative specialist, the problem is location, location, location!
I recently attended a continuing-education course presented by Dr. Kois, titled "Managing the Restorative Periodontal Interface." Dr. Kois has authored many articles, but one I found particularly interesting was published in Periodontology 2000 in 1996 on this subject. He has done a very good job of explaining the concept of biologic width and thus the location issue of the crown margin. Let's look at the potential causes of inflammation around a crown, with specific attention to the biologic width and what a violation of this area means.
Plaque accumulation
If the irritation is caused by plaque accumulation, then it is not likely to be just one crown of a pair. For example, if your patient has crowns on both central incisors and only one is inflamed, is it logical to think the patient is effectively cleaning one crown and ignoring the other? Not likely.
The best way to find out is to debride the area, check brushing techniques, or recommend a power toothbrush and have the patient irrigate with water or an antimicrobial. If plaque accumulation is the problem, it should clear up in two weeks and remain healthy. If the problem is not plaque accumulation, the tissue will continue to be inflamed.
Margin Integrity
No margins are perfect, since microscopically there always is a discrepancy. Although measured in micro-millimeters, all margins are open. Bacteria measure only one to five micro-millimeters each, so a margin opening of 200 micro-millimeters allows plenty of room for bacterial accumulation.
But we have all seen stainless-steel crowns in place for 25 years with gaping margins that have not resulted in periodontal destruction. Based on these cases, it is clear that the virulence of the bacteria and the body's immune response are more important than the crown margin. Dentists always strive for the perfect margin, " ... but excellent margins may do more for the dentist emotionally than for the patient biologically," says Dr. Kois.
Contour
In general, the contour of an artificial crown should resemble that of the natural crown. However, artificial crowns are most often larger facial-lingually than the natural crowns. If tooth roots are close together, even slight deviations in contour will influence gingival health. Roots that are farther apart do not seem to be so easily influenced. We see this when a diastema is closed by changing tooth shape and contour. The general rule allows for a gingival bulge of no more than half a millimeter on the facial or lingual. This allows access for effective plaque removal. There always should be enough room between crowns to pass an explorer tip through the interproximal.
Metal sensitivity
Some metals will leach out of alloys used in crowns, especially nickel. Approximately 10 percent of the U.S. population is sensitive to nickel. Women are 10 times more likely to be sensitive to nickel than men. This is due to the common use of nickel in women's earrings and other jewelry. We may see the number of men with nickel sensitivities increase as earring use increases among men.
According to Dr. Kois, contact dermatitis linked to dental alloys is very rare. Some of the hypersensitivity may be neutralized by salivary glycoproteins.
Margin location
This is the important one. The margin of the crown should not violate the biologic width. If crown margins remain supragingival, there is no problem. However, for esthetic reasons, subgingival placement of the margin often is required. Just how far below the gingival margin the crown margin extends is the critical issue.
The dentogingival complex includes the connective-tissue attachment, the epithelial attachment, and the sulcus or pocket area. The biologic width, which always remains constant, is the distance from the base of the sulcus to the alveolar bone. The relationship between the epithelial attachment, the connective-tissue attachment, and the bone remains constant, no matter where it is on the tooth. The distance from the free gingival margin to the osseous crest most often will be 3 millimeters on the facial surface and 4 millimeters on the interproximal surface.
A crown margin should be at least 2 to 2.5 millimeters away from the osseous crest, or half a millimeter subgingivally. If a crown margin is placed too close to the bone, the tissue will react, triggering an inflammatory response. You would expect this inflammatory response to eventually destroy some bone, thus re-establishing the optimum 3-4 millimeter distance. But, it can take a very long time. The inflammation may last for years.
In estimating these measurements, Dr. Kois suggests a way to determine just where the bone is located, since visually we can't see it. He suggests a simple technique of "periodontal sounding." The area is anesthetized and the probe is inserted into the sulcus through the epithelial attachment, through the connective tissue, until bone is felt. The measurement from the gingival margin should be at least 3 millimeters all along the facial and 4 millimeters all along the interproximal. Interestingly, if just one spot - for instance, on the line angle - is less than 3 or 4 millimeters, gingival inflammation will be evident around the entire facial margin. The margin of the crown must follow the underlying contour of the osseous crest and not interfere with the prescribed distance.
There are several reasons why this biologic width may be violated when a crown prep is made. If the tooth has fractured, the remaining structure may be so close to the bone that the dentist must extend the preparation deeper to gain access to sound tooth structure. Sometimes, a crown is placed after removing an old restoration, which left margins that require the preparation to be deeper than desired. Existing caries extending onto the root surface and resorption defects may also require extension of the preparation into the dentogingival zone. Traumatic injury and iatrogenic insults also explain violations of the biologic width. Sometimes, the dentist makes a mistake estimating the location of the osseous crest and places the margin too close to the bone.
Solutions to crown margins placed in violation of the biologic width are not always simple. If a small area is detected at the line angle, the bone can be recontoured directly through the attachment without raising a flap. If the violation involves the entire margin, correction may involve osseous resection or orthodontic extrusion of the tooth and placement of a new crown. It's better to prevent the problem than to correct it.
Next time you see red, puffy gums around a crown, put on your detective hat and see if you can determine the cause!
Trisha E. O'Hehir, RDH, BS, is a senior consulting editor of RDH. She also is editor of Perio Reports, a newsletter for dental professionals that addresses periodontics. The Web site for Perio Reports is www.perioreports.com. She can be reached by phone at (800) 374-4290 and by e-mail at [email protected].