by Nancy W. Burkhart, RDH, EdD
[email protected]
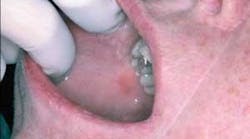
Your patient today is a 34 year-old female who has made an appointment to determine the etiology of an erythematous patch on her right buccal mucosa. She noticed this painless, nonulcerative red area approximately a year ago, but decided to wait until she established a dental office and could make an appointment.
As you evaluate the area, you notice that the erythematous lesion is adjacent to an amalgam restoration. The patient had the restoration placed about 14 months ago — before a job relocation.
After assessing the restoration and later replacing the amalgam with a non-metal restoration, the lesion subsided. It was determined that the cause was due to a sensitivity to the metal components in the restoration or a “contact lichenoid reaction” (see Figure 1).
Etiology: Lichenoid reactions may be caused by sensitivity to amalgam restorations, metal sensitivity such as to orthodontic wires, partials, etc. But other products may cause a hypersensitivity reaction as well in individuals. Crowns and composite restorations may even suggest a lichenoid reaction in sensitive patients.
Items such as medications that are given for the treatment of systemic disease states, such as lupus erythematosus and graft vs. host disease, may produce what is termed “lichenoid mucositis.” The drug-induced lichenoid reactions are the most common cause of lichenoid lesions.
Dental products may cause lichenoid reactions as well. Individuals may be sensitive to the tartar control agents in toothpaste, cinnamon-containing foods, additives (see “Toothpaste allergy,” RDH, June 2007), preservatives and flavoring agents such as balsam of Peru (Torgerson, 2007), and spearmint, wintergreen, peppermint, etc., found in mints and gum. Because dental products generally contact all areas of the mouth, any lesions that occur are most often displayed throughout the mouth as opposed to the contact lesion in the case study.
In the case presented, the reddened area is in contact with the amalgam restoration. The tissue reaction may be around adjacent tissue or possibly at the gingival margin if the restoration extends into the gingival tissue.
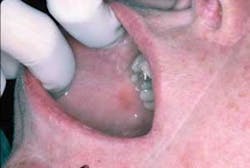
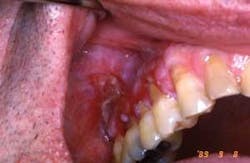
Dispersion throughout the mouth is also found in lichenoid reactions from the use of medications such as non-steoidal anti-inflammatory drugs and anti-high blood pressure medications. Figures 2 and 3 are from a patient who was taking Naprosyn. After discontinuing the medication, the tissue in Figure 3 was noticeably less inflamed. The patient took Tylenol during the two-week period and was later prescribed a different NSAID.
Pathogenesis: Pathologists may refer to “lichenoid reactions” in pathology reports and may also use the terms “lichenoid mucositis” or “chronic mucositis with lichenoid features.” The reason for this is because there are not enough distinctive features that make the lichenoid reaction a definitive diagnosis for true lichen planus. Therefore, the diagnosis may be lichen planus or a lichenoid reaction depending upon how clearly consistent the features may be in a tissue sample — or put another way, how altered the characteristics may be from frank lichen planus.
A patient who is taking multiple medications may be offered the standard treatment for lichen planus, which is normally a regimen of topical corticosteroids. If the treatment does not offer signs of response, the practitioner would want to consider the possibility of a “lichenoid drug induced reaction.” At that time, the possibility of an offending agent may be considered or the possibility of a drug-induced reaction. Often, determining the possibility of a lichenoid reaction when multiple medications are being used by the patient is one of trial and error.
By providing as much information about the patient and the history of the lesion to the oral pathologist, the greater the probability is of obtaining a more definitive diagnosis. Patch testing assists the pathologist in reaching a diagnosis. Patch tests performed by a dermatologist may determine the reaction of the patient to certain metals, flavoring agents, or other possible environmental agents.
Extraoral characteristics: Skin lesions and hypersensitivity reactions appear as classic cutaneous lichen planus lesions denoted by purple, polygonal plaques that are pruritic in nature (see “Lichen Planus,” RDH, February 2007).
Perioral and intraoral characteristics: Conventional idiopathic lichen planus is usually found bilaterally. Contact lichenoid reactions such as the one presented in the case study are found unilaterally because of direct contact with the tissues. However, when the individual is consuming a product such as one that is dispersed throughout the mouth, the tissue’s surface may be affected in total. Lesions may be white, red, or in combination — just as in true lichen planus.
Distinguishing characteristics: Lichen planus may be clearly differentiated in cases where the patterns are very suggestive of the classic lichen planus features, both clinically and microscopically. However, lichenoid reactions may sometimes be close enough in characteristics to be labeled lichen planus, when they may, in fact, be an allergic response.
Myers et al. 2002 made the observation that this could impede or prevent further investigation of the lesions. The clinician may decide that no other investigation may be needed since “it is lichen planus,” and the lesions are treated as such. The reverse may occur when the diagnosis is vague and not identified as true lichen planus, and the clinician may search further for a more definitive diagnosis. The authors cite a rendered diagnosis in 20 cases of oral lichen planus as often containing terminology in the diagnosis as “possible” or “probable” rather than definitive in nature.
Microscopic features: The tissue sample associated with lichen planus exhibits degeneration of the basal cell layers and an increase in lymphocyte infiltrates. The basal cell layer typically has a bulbous or “saw tooth” appearance. Degenerating epithelial cells, or Civatte bodies, are observed. Civatte bodies, which are observed microscopically, are eosinophilic ovoid bodies that are apoptotic (dying cells) or necrotic keratinocytes (epithelial cells that ultimately keratinize) at the basement membrance.
Reports associated with lichenoid reactions include various findings such as subepithelial infiltrate that is diffuse and extends deeply. Additionally, reports of increased eosinophils that are also found in allergy-type reactions, parakeratosis and increased plasma cells. There are no definitive diagnostic criteria at present for lichenoid reactions, and tissue samples will vary.
Differential diagnosis: Multiple, complex drug regimens and combinations of medications in one patient may account for the “lichenoid” type reactions that continue to be reported. New medications are constantly produced and prescribed, making it very difficult to isolate offending medications in an individual who is taking multiple medications at a given time. It is known that allergic type responses may be observed at any time in life, and, as new medications are constantly introduced, the side effects may not be known for some time. Every individual may react in different ways to all medications or combinations of these new products.
Treatment and prognosis: The treatment of lichenoid reactions depends upon the offending agent. Sometimes, if the problem is due to a drug-associated lichenoid reaction, simply changing the patient to another medication may be all that is needed. This is never suggested without the consultation of the patient’s physician. In some cases, the patient may not have the option of substituting medications, so this sometimes is not a simple solution.
Providing as much information as possible to the pathologist who reads any biopsy is extremely important. Providing a list of all medications, allergies, dental products, or flavoring agents that the patient is using, a good description of the health history, previous diseases, and a slide (digital or even a print) is beneficial. If a slide is not available, a complete description of the lesion, including the exact location, is welcomed.
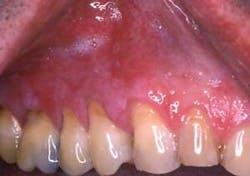
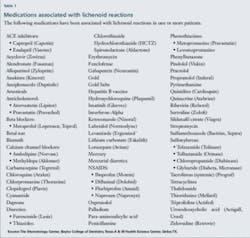
We often forget to ask specific questions when taking health histories and linking pertinent health information about the patient. A good example is a case study presented in The New England Journal of Medicine in 1996. The case was that of a 24 year-old man who consumed approximately 200-300 ml a week of Goldschlager, an Italian cinnamon schnapps containing tiny flakes of gold, during the period of one year. The patient developed skin lesions very similar to lichen planus. Gold is one of the agents that when given as a therapeutic agent (see list of medications in Table 1) will induce a lichenoid skin reaction. Serum and urinary gold levels were measured and confirmed a high range of gold in this patient. Measurable levels remained even at three months after the patient ceased consumption.
This case study is interesting because, even though we may ask about alcohol consumption, it would be rare for a clinician to ask about the type or brand of alcohol. In this particular case, it was highly beneficial to know the brand. The gold flakes in this liquor also contained a cinnamon flavoring agent that could have compounded the symptoms as well. Gold flake liquor is commonly used in Europe, but appears to be gaining popularity in the United States (see Figure 4).
Having the patient keep a two-week diary of everything that they eat or place in the mouth will allow the clinician to search for patterns. Environmental agents may be part of the scenario as well. We are constantly bombarded with so many chemicals, detergents, fragrances, preservatives, and new products. It is often difficult to determine a specific agent. A list of any dental products, including mouth sprays, is also suggested.
The patient could try other products without flavoring agents or some of the known additives that may produce problems in certain individuals. An astute clinician can truly make a difference in the life of the patient — listen to your patients and continue to ask good questions.
For more information on lichenoid reactions and oral lichen planus go to: http://bcd.tamhsc.edu/outreach/lichen/
References
McCartan BE & Lamey PJ. Lichen planus-specific antigen in oral lichen planus and oral lichenoid drug eruptions. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2000;89:585-7.
Myers SL, Rhodus NL, Parsons HM, Hodges JS, Kaimal S. A retrospective survey of oral lichenoid lesions: Revisiting the diagnostic process for oral lichen planus. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002;93:676-81.
Russell MA, King LE, Boyd AS. Lichen Planus After Consumption of a Gold-Containing Liquor. New England Journal of Medicine. 1996, Feb 29(334)9: 603.
Thornhill MH, Pemberton MN, Simmons RK, Theaker ED. Amalgam-contact hypersensitivity lesions and oral lichen planus. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2003;95:291-9.
Torgerson RR, Davis MD, Bruce AJ, Farmer SA, Rogers RS 3rd. Contact allergy in oral disease. J Am Acad Dermatol 2007;57:315-21.
Wright J. Diagnosis and management of oral lichenoid reactions. J Calif Denta Assoc. 2007 Jun;35(6);412-6.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry and Texas A & M Health Science Center in Dallas. Nancy is also a cohost of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is the coauthor of General and Oral Pathology for the Dental Hygienist, published by Lippincott Williams & Wilkins (2007). Nancy presents seminars on oral pathology subjects nationally. She can be contacted at [email protected].