by Lynne H. Slim, RDH, BSDH, MSDH
[email protected]
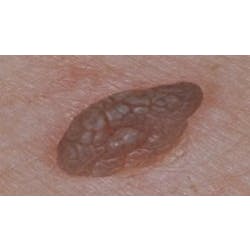
A 74-year-old woman enters your operatory as a new patient. While performing a comprehensive periodontal exam, you discover atypical gingival inflammation of the mandibular anterior sextant, but she also presents with a burning tongue and some distinctive skin lesions on her hands. It's been a long time since you glanced at your favorite oral pathology textbook, but you already suspect a mucosal disease.
Periodontal therapists (and I use this term loosely to include hygienists, dentists, and periodontists who are passionate about evidence-based periodontal therapy) see a small number of patients with mucosal diseases. For example, oral lichen planus, a chronic mucocutaneous disorder, affects about 1% to 2% of the general population, and occurs more often in individuals over the age of 50. Lichen planus also occurs in children but at a lower rate.
I recently spent some time with a former student while sharing a hotel room in Chicago during the Chicago Midwinter Meeting. Nancy Burkhart, BSDH, EdD, is the co-author of "General and Oral Pathology for the Dental Hygienist" (Lippincott, 2007). She is also the founder of the International Oral Lichen Planus Support Group (1997-present). In addition to being RDH magazine columnists, Nancy and I are MacBook "addicts," and in between catching up on e-mails in our hotel room, I decided to pick her brain about mucosal diseases, especially since baby boomers (also referred to as aging hipsters) make up the fastest growing age group in the U.S.
Nancy's definitely not an aging hipster, but like me, she's a baby boomer with porcelain skin, beautiful green eyes, and an inquisitive mind. Here's some great insight and evidence-based information from Nancy that will help you better assess these conditions.
Can you discuss the prevalence of oral mucosal diseases in adult patients?
The International Oral Lichen Planus Support Group (IOLPSG) deals primarily with people who have oral lichen planus. This disorder can have other factors associated with it and other disease states such as pemphigus vulgaris, pemphigoid, lupus, Crohn's disease, Sjogren's syndrome, and periodontal diseases.
Every person presents with a different profile. Many times a patient has been seen by a periodontist or treated as a perio patient in a general dental practice. When the tissue does not seem to respond, the dentist considers other possibilities, or in most cases the patient researches his or her own symptoms to look for answers. The patient usually discovers the IOLPSG because lichen planus has either been recently diagnosed or has been a constant problem. Sometimes the problem is recent, and other times a patient may have had the unresolved problem for over 30 years.
Patients who present with oral lichen planus and skin lesions might have multiple disease states. The long-term effects of chronic diseases often take a toll on patients, and psychologically can cause feelings of loss and detachment. This is especially true when there are outward signs of a mucosal disease that may present on the lips or gingiva. Many times the tissue will appear bright red and patients will be self-conscious about interacting with others.
They may believe that they are complaining to professionals who do not understand or who tend to dismiss their concerns. Dentists and hygienists enter their profession with certain personality profiles that gravitate toward closure. Patients become frustrated and so do the oral care providers. With chronic disease states, the process is often ongoing and not easily solved. At the stomatology clinic, the statement, "If your problems were that easily solved, someone would have 'cured' your problem long ago!" can often be heard.
Treatment consists of trying certain procedures and adapting to patients' needs. Corticosteroids are often used to get the tissue under control, and the amount is reduced after a period of time. Chronic ulceration or inflammation is never good, so controlling the inflammation is paramount. In general, skin diseases often overlap and are not diagnosed purely by clinical evaluations. A biopsy is needed to differentiate. In addition, a procedure called direct immunofluorescence demonstrates the presence of fibrinogen at the basement membrane.
Other skin diseases have different patterns, allowing the pathologist to make a definitive diagnosis. We have had a number of patients contact us, and after referring them to an oral care professional, the diagnosis has been oral cancer. They may have been diagnosed with lichen planus originally, but somewhere along the way the tissue changed. Practitioners sometimes follow patients for years without any resolution and assume they are still dealing with lichen planus. But over time, there may be a change and the lesion may become oral cancer.
What's the difference between a lichenoid mucositis and lichen planus?
Sometimes certain features are not present when read by the pathologist, and the specimen has what is termed lichenoid mucositis. The tissue may have some features of lichen planus, but the diagnosis of the features is not clear enough to make that determination. Lichenoid features may be from medication-related factors. Often the specimen may have microscopic features such as spongiosis, apoptotic keratinocytes, lymphoid infiltrates, eosinophils (often found in allergy-affected tissue), and chronic ulceration. Not just medication, but dental products and materials will sometimes cause lichenoid mucositis. Since lichen planus often resembles a hyperactivity reaction, the diagnosis of a good pathologist is very important in assessment. True oral lichen planus includes hyperkeratosis, basal cell vacuolization with apoptotic keratinocytes, and liquefaction of the basal cell layer. There is a dense lymphocytic infiltration at the basal cell layer. When clear features are not present, a lichenoid mucositis diagnosis is often given, or one that indicates that the features of lichen planus are not diagnostic to call it by that name.
Sometimes adult patients present with long-term, atypical, chronic gingival inflammation. Which oral mucosal diseases exacerbate gingival inflammation? Many skin disorders masquerade as lichen planus, such as allergy-related problems, pemphigus, pemphigoid, lupus, or combinations of disease states. A patient may have diabetes or some other chronic disease state that complicates treatment. Allergies to metals, flavoring agents, food additives, and environmental agents make a diagnosis difficult, and patch testing is often needed to determine the offending agents.
Are patients with oral mucosal diseases more likely to have noted hypersensitivity to food additives or other triggers?
Patients diagnosed with lichen planus complain about certain foods that may trigger gingival problems or irritate the tissue. This will vary with patients, and what caused problems for one person may not affect another. I have answered thousands of e-mails since 1997 (origin of the IOLPSG) and have heard just about everything from apples, citrus fruits, wine, salsa, tomato-based products, flavoring agents, spices, toothpaste agents, mouthrinses, and much more as the cause for lichen planus. Interestingly, only a few products appear to be consistent with most patients.
What products/procedures should be avoided when treating patients with oral mucosal disease?
Patients do well with toothpastes that have few to no flavoring agents. Tartar control toothpaste appears to cause problems for most patients. We have found that either Biotene original or some children's toothpastes work well. If rinses are recommended, Biotene mouthrinse is usually tolerated. Dryness is often a problem and the Biotene gel is a good product. Patients should keep a log of foods and environmental agents so that patterns of offending products can be examined. Sometimes patients have difficulty with cinnamon products or food preservatives.
We have a list of suggestions for recall visits on our Web site, http://bcdwp.web.tamhsc.edu/iolpdallas/, and we believe that some patients with extensive inflammation need altered treatment protocols. Air polishers are too harsh, so the preferred techniques are thin ultrasonic tips/inserts on low power settings, or hand-scaling techniques with rounded curettes. With mucosal disease states, the stripping of the epithelium is the most noticeable characteristic. When patients have periodontal disease in addition to a mucosal disease, quadrant scaling is easier on them since their mouth is usually very sensitive. The literature supports frequent prophy/scaling at three-month intervals. Patients should be checked for candida at each recall visit since this commonly occurs with the use of corticosteroids.
Lynne Slim, RDH, BSDH, MSDH, is an award-winning writer who has published extensively in dental/dental hygiene journals. Lynne is the CEO of Perio C Dent, a dental practice management company that specializes in the incorporation of conservative periodontal therapy into the hygiene department of dental practices. Lynne is also the owner and moderator of the periotherapist yahoo group: www.yahoogroups.com/group/periotherapist. Lynne speaks on the topic of conservative periodontal therapy and other dental hygiene-related topics. She can be reached at [email protected] or www.periocdent.com.
Past RDH Issues