Ankyloglossia: Are You Paying Attention?
by Nancy W. Burkhart, BSDH, EDD
The lay public frequently refers to ankyloglossia, a congenital oral anomaly, as "tongue-tied." The public often assumes that someone who exhibits a speech impediment may be "tongue-tied."
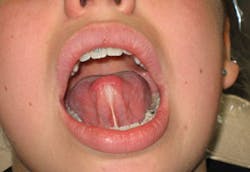
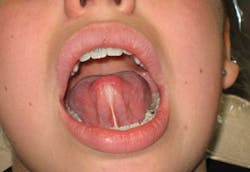
Ankyloglossia involves the lingual frenum, also referred to as frenulum (see Figure 1). Generally, the tip of the tongue is anchored to the floor of the mouth in varying degrees of attachment. Frenum tongue-ties may occur in both the anterior and mid-tongue areas. Usually, the tighter the attachment, the more involved simple tasks such as eating and speaking will be affected.
-----------------------------------------------------------------------
Other articles by Burkhart:
-----------------------------------------------------------------------
Nursing mothers who have trouble breastfeeding will usually be the first to discover the tight frenum attachment while trying to solve the feeding issues that arise. New Jersey in October 2012 introduced legislation to make it mandatory that all infants be evaluated for ankyloglossia. The bill states that ankyloglossia is overlooked, and the effects on infants include problems with breastfeeding. The bill makes mention of other issues that occur later in life such as the affect of structure and appearance of the face, teeth, and oral function. Long-term consequences of digestion, speaking, and kissing are also mentioned within the bill. Surgical correction seven days after birth is suggested. The bill now awaits further consideration and proponents are hoping for passage.
Kimberly Benkert, RDH, BSDH, MPH, COM, FAADH, provides orofacial myofunctional and muscular TMD therapeutic services in suburban Chicago. She is certified in orofacial myology and owns three office locations providing these services within the Chicago area. Kimberly commented that surgical procedures could safely be completed 24 to 72 hours after birth. This is a critical time for nursing mothers and babies who breastfeed.
Benkert states, "Infants with lingual and labial frenum issues often have difficulty latching onto the breast, expressing milk, and making a seal to nurse correctly and without excessively ingesting air. Frenum issues are often missed if a complete oral assessment and exam are not completed at birth.
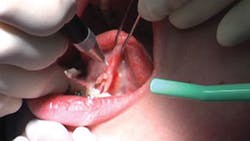
"The nursing mother assumes they are having difficulty with nursing and opt for using a bottle. Every infant should be assessed before leaving the hospital. That is the best time to do a labial and /or lingual frenectomy with the least amount of post-operative distress to the child (see Figure 2). Nursing within 90 minutes after the procedure stimulates the healing process and almost always demonstrates immediate improved functionality.
"Addressing lingual and severe labial frenums at birth aids in the feeding/eating for the infant, and reduces risk factors related to sleep disordered breathing and sleep apnea. It allows the posture and positioning of the tongue, lips and jaws to develop more normalized function since they can move freely and without restriction. This is significant to the growth and development of the face, palate, and stimulation of nasal breathing with lips closed properly and the tongue serving as a natural muscular hydrostat."
A study by Sethi, et al. (2013), found that 77% of mothers who had babies with ankyloglossia reported improvement with breast-feeding following frenulotomy. Other causes for difficulty in breast-feeding may have occurred as well, but 40 out of 52 mothers saw an improvement in these problems within two weeks of the procedure.
Edmunds et al. (2013), conducted a study on the experiences of mothers who attempted to breastfeed an infant with tongue-tie. The mothers described an experience that was not anticipated. Health professionals were described as having limited knowledge of tongue-tie and its effect on breastfeeding, thereby limiting any advice that they could provide to the mothers. Following the release of the frenum attachment in these infants, breastfeeding was greatly improved.
A growing number of studies indicate that some speech misarticulations are caused by a tight frenum, and varying degrees of tightness may affect those speech sounds (phonemes). The sounds produced by the frontal part of the tongue are: D, J, L, N, S, and T, along with TH, SH, and CH. Most sounds can be produced with a restricted tongue, but patients may need to speak slower to be comprehended. In most cases, an adequate palatal tongue rest posture may not be achieved as the child grows, thereby affecting the shape of the palate and swallow pattern.
A procedure called a frenectomy is performed to eliminate the restrictions of both the tongue and the tethered attachments extending into the muco-periosteal insertion and the alveolar process. Eliminating this "tie" increases mobility and improves function. A frenotomy is another reference to this procedure where the frenum was clipped or cut to free the movement of the tongue.
Laser procedures significantly reduce healing time and eliminate the need for sutures in the nonkeratinized movable oral mucosa. Suter & Bornstein (2009) make the observation that, because almost no prospective studies for surgical interventions are present, it is difficult to make suggestions with regard to methods that may be optional or suggestions on which tongue ties need to be surgically eliminated or left to observation.
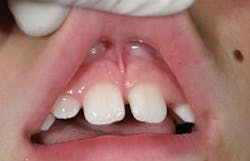
The labial frenum may be a thick pronounced band of tissue that produces a separation of the maxillary central incisors, causing a diastema (see Figure 3). This tight maxillary frenum may prevent complete lip closure, and this promotes nasal breathing. The diastema may also occur on the mandibular anterior facial and lingual teeth as well, depending upon how high the frenulum is attached to the gingival ridge.
The individual may have problems sticking out their tongue or moving it from side to side. Usually, the patient is unable to protrude the tongue past the edge of the lower gingival or mandibular incisors. An even more extensive procedure may be performed in cases where the frenum is too thick called a frenuloplasty. Specific scores are assigned to designate the frenulum thickness, attachment to the tongue, and the frenulum attachment to the floor of the mouth.
Some researchers have reported a decrease in severity as the child grows and oral development progresses. Perhaps stretching or in some cases rupture of the frenum may occur throughout development of the individual. Since many cases are never documented, the exact number of those affected is unknown.
Long-term tongue restriction can affect home care because the individual may have problems reaching the posterior teeth when brushing.
Benkert states, "The biggest oral hygiene issues with a restricted lingual frenum is impacting food and bacteria into the dentition during rest, chewing, swallowing and speaking along with the lack of self-cleansing movements of the tongue to reach/retrieve food particles due to functional restrictions."
Marge Foran, RDH, is a therapist specializing in orofacial myofunctional therapy and works with patients who have ankyloglossia in Montana. She made the following comment regarding ankyloglossia:
"Ankyloglossia is one of several contributing factors of orofacial myofunctional disorders. If the lingual frenum is restricted, the limited movement of the tongue may influence the normal growth and development of the oral and nasal cavities and impact muscle patterns and function. This may have many lifelong consequences ranging from difficulty wearing dentures, compensatory speech habits, orthodontic relapse, swallowing disorders, ineffective oral cleansing, and difficulty playing some wind instruments to name a few. A tight lingual frenum has a potential impact on the intrinsic and extrinsic muscles of the tongue.
"In the area of TMD and sleep disordered breathing, it is important to evaluate the lingual frenum. A dysfunctional oral muscle patterning of the tongue and orofacial muscles may influence these disorders or conditions. At any age, it is recommended that a consult occur with an orofacial myofunctional therapist prior to a surgical procedure. Therapists trained in the science of orofacial myofunctional therapy will prescribe home-based daily exercises to avoid scarring post-operatively which ensures that the tongue remains flexible and toned."
The scope of practice for orofacial myofunctional therapists include:
- Elimination of non-nutritive sucking habits (thumb, finger, pacifier, etc.)
- Elimination of parafunctional habits. Examples include orofacial habits, nail biting, tongue sucking, lip, cheek and tongue biting, as well as bruxism, clenching, and muscle bracing (if you are a dental hygienist)
- Abnormal orofacial rest posture problems and functional patterns of the tongue, lips, and jaw.
- Abnormal neuromuscular muscle patterns associated with inappropriate mastication, bolus formation, bolus/food transfer, and deglutition
- Abnormal swallowing patterns (dysphagia-oral and pharyngeal phases, commonly referred to as "tongue thrusting")
- Functional movements of the tongue, lips and jaw for speech patterning
Dental professionals should be aware of the complications that could occur with ankyloglossia since any questions that are asked by patients concerning the mouth are usually directed to the dentist or hygienist first. Patients who may be having trouble breast-feeding may mention this during a routine dental appointment. A patient who obviously has the anomaly may present with some of the described problems associated with ankyloglossia.
Brochures, websites and contact information may be given to the patient. Practitioners who specifically treat ankyloglossia may be found by checking with local periodontists, oral-maxillofacial surgeons and ENT specialists in your city, or with the Academy of Orofacial Myofunctional Therapy. Treatment/assessment for ankyloglossia with varying protocol is found worldwide and may involve oral surgeons, general dentists and periodontists, physicians, dental hygienists, orofacial myofunctional therapists, and speech-language pathologists.
Are you paying attention to ankyloglossia? As always, continue to ask good questions and always listen to your patients.
Author's note: A special note of appreciation to Kim Benkert and Marge Foran for guidance in writing this column.
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com.
References:
Benkert KK. (2012) Orofacial Myology-The function junction: utilizing nature's bio-adaptability of soft and hard tissues. J Orthodontics & Dentofacial Orthopedics.2012; 12(3): 28-40.
Edmunds JE, Fulbrook P, Miles S. Understanding the experience of mothers who are breastfeeding an infant with tongue-tie: a phenomenological study. J Hum Lact. 2013; 29(2): 190-5.
Merdad H, Mascarenhas AK. Ankyloglossia may cause breastfeeding, tongue mobility, and speech difficulties, with inconclusive results on treatment choices. Journal of Evidence-Based Dental Practice. 2010;10(3):152-3.
Sethi N, Smith D, Kortequee S, Ward VM, Clarke S. Benefits of frenulotomy in infants with ankyloglossia. Int J Pediatr Otorhinolaryngol. 2013 May; 77(5): 762-5.
Suter VG, Bornstein MM. Ankyloglossia: facts and myths in diagnosis and treatment. J Periodontol. 2009Aug; 80(8): 1204-19.
Past RDH Issues