Taste distortions in dental patients
Your patient today is 70-year-old Carl who has been in your practice for over 20 years and has maintained excellent home care with no dental problems of concern. He has no periodontal problems and presents regularly every six months for an exam and prophy. Today, however, he is complaining about some taste changes and xerostomia, and wants your opinion about these changes.
A curious case
He has tried to brush his tongue and is now using a tongue cleaner. As you assess the situation, you notice that his health history has changed, and he is taking some medications that were not previously on his medical form. His physician has prescribed Capoten (captopril tablets) that is classified as an ACE inhibitor for hypertension. The dosage recommended for Carl is 25 mg b.i.d. He has been taking this medication for two months now and complains about the need to season his food more heavily.
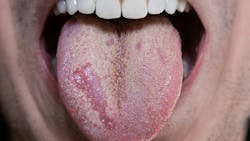
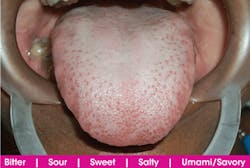
Patients with hypertension may have higher recognition thresholds for salty flavors. A decline in perception for salty flavors may induce elderly patients to season their foods with excessive amounts of salt. Could the medication or hypertension be contributing to his taste change and xerostomia complaint? Since it has been some time since a patient presented with complaints about taste changes, you may have forgotten where various taste sensations occur in the mouth and the probable causes for such changes (see figure 1).
Taste occurs throughout the mouth within the taste buds and specifically in the taste receptors. Taste changes (gustatory changes, relating to taste or tasting) are very difficult to ascertain, and they are not easily determined or solved by the dental clinician. Taste and smell are highly subjective to each individual, and patients are often referred to special clinics for a complete workup. Assessing taste disturbances is very time consuming for a clinician, but the dental professional may be instrumental in suggesting further evaluation to patients when a taste disturbance is suspected and not easily identified.
Dividing taste disorders into qualitative and quantitative disorders
Qualitative disorders involve what is termed:
- Parageusia -- A changed perception of taste quality.
- Phantogeusia -- Perception of taste without a stimulus. The person perceives a constant taste such as metallic, bitter, or salty.
Parageusia and phantogeusia are sometimes complaints expressed by patients within a dental practice.
Figure 1: The five taste sensations may occur throughout the tongue. Saliva mixes with foods and flavors dispersing them to various locations on the tongue surface. Note the very prominent fungiform papillae.
Qualitative measures are based on the perception of the patient, and these are very individualized to each person. Both olfaction (smell) and gustation (taste) play significant roles in the perception of taste sensations. Sensations occur in the taste buds/receptors found in the tongue, soft palate, pharynx, uvula, upper third of the esophagus, lips, cheeks, and epiglottis.
The role of taste buds
Humans have around 10,000 taste buds located in the papillae and each papilla may have hundreds of taste buds. Taste buds are replaced every 10 days, and saliva plays a huge role in taste since the flavors are carried to all parts of the mouth. Saliva acts not only as a lubricant, but also as a dissolvent as it dilutes strong concentrations. The taste sensation is not recognized until it is mixed with certain chemicals when dissolved in saliva and then detected by the receptors in the taste buds.
Some disorders that may present with taste changes are multiple sclerosis, depression, thoracic disorders, and epilepsy. Additionally, kidney and liver conditions, endocrine conditions, cancer, and gastrointestinal diseases are noted as having altered taste sensations. Taste disorders often go unrecognized in the elderly patient and may indicate some undiagnosed disease processes.
Quantitative measures involve the following:
- Hypergeusia -- Gustatory hypersensitivity
- Normogeusia -- Normal gustatory sensitivity
- Hypogeusia-gustatory hyposensitivity -- Reduced ability to taste
- Ageusia -- Complete loss of taste
The five main flavors that occur in taste acuity:
- Salty (sodium chloride and other salts)
- Sweet (sugars)
- Sour (acids)
- Bitter (alkaloids)
- Umami (savory)-amino acids (Umami means "delicious essence")
- All other flavors are combinations of these five primary tastes, plus accompanying olfactory and taste sensations.
What the tongue can tell you
Imoscopi et al. (2012) report that being able to differentiate healthy products from those that may cause harm to the body is a defense mechanism of the body. Specific taste sensations promote a "safe sense" as opposed to a "danger sense" by the human or animal. This is a bodily defense mechanism to assist the human or animal in avoiding food that may be poisonous or spoiled and may cause sickness or death. The ability to differentiate a sour taste enables the individual to limit the ingestion of acids from food and beverages so that the body may maintain the right acid-alkaline homeostasis.
Chinese medicine evaluates taste functions as an indication of disease or health states. A bitter taste may indicate liver or gallbladder issues including hepatitis. The bitter taste may also be associated with cancer since many cancer patients lose their sense of taste to sweets and become more sensitive to bitter.
A sweet taste may indicate stomach or pancreatic problems due to an overproduction of salivary amylase. This is common in diabetic patients. A salty taste may indicate kidney issues. A sour taste may indicate gastritis, ulcers, or gallbladder problems. A diminished taste may indicate a problem with intestinal inflammation or a variety of gastrointestinal tract diseases.
The color of the tongue is an indicator of the condition of the blood in the body. If the constituents of the blood change even slightly, the tongue color will also change. The vitality, movement, and moisture are also evaluated during an exam. If a patient is complaining of any taste change, specific components are closely examined.
Taste buds are found on the tongue with three particular groups of papillae containing numerous taste buds: The circumvallate, foliate, and fungiform papillae. Large evident fungiform papillae on the tongue may indicate that the person may be what is termed a "supertaster" and experiences a heightened sense of taste (see Figure 1). Supertasters are more likely to suffer from burning mouth syndrome. On the opposite end of the spectrum, "subtasters" have fewer fungiform papillae and can tolerate more spicy foods. They are also less likely to have burning mouth syndrome.
The olfactory epithelium of the nasal cavity plays a huge role in taste sensations as well. Malaty et al. (2013) state that over 95% of perceived taste disorders reported by patients are caused by olfactory (sense of smell) loss, rather than gustatory (taste) loss. Patients have a difficult time distinguishing between the two, and both olfactory and gustatory are intertwined in our perception of taste. The most common olfactory contributors to taste dysfunction are allergic rhinitis, chronic rhinosinusitis, upper respiratory infections, head trauma, neurodegenerative diseases, and medications. Cranial nerves also play a huge role in taste conduction. Cranial nerves l (olfactory), Vll (facial), IX (glossopharyngeal), and X (vagus) are tested in gustatory disorders.
Poor oral hygiene and candidiasis may alter taste perception. In elderly populations, poor nutrition and poor hygiene related to diminished dexterity may be factors that contribute to this loss or change in taste that is a complaint with many patients. Inadequate or defective partial and full dentures may cause trauma, and affect the tissue as well as interfere with taste sensations.
Other causes may be xerostomia, periodontal disease, dental products, upper respiratory problems, and tumors in not only the mouth but the nose as well. Many medications are responsible for taste alterations and the elderly are consuming these medications at a rapidly growing pace. Some common medications associated with taste disorders are cardiovascular medications, NSAIDs/corticosteroids, psychotropic medications, antibacterial agents, and metabolic agents.
The assessment of gustatory function should be a part of any comprehensive examination. Taste changes in the elderly may result in weight loss, malnutrition, and a loss of appetite, leading to other chronic disease states. In the case presented involving Carl, both his taste changes and the dryness that he reports may be due to the cardiovascular medication that he has been prescribed. Although the dosage is low, the effects are very subjective with each patient.
The probability of your patient complaining of a change in their perception of taste is great. The population is aging, more medications are being prescribed for patients, and more additives are present in our food supply. We are also bombarded by environmental chemicals daily that may alter taste sensations as well. When the quality of life is affected for your patient, perhaps a referral to a smell and taste clinic may be warranted.
As always, continue to ask good questions and always listen to your patients.
References
- DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 2nd edition. Wolters Kluwer-Lippincott, Williams & Wilkins. Baltimore, 2013
- Chi T. Dr. Chi's fingernail and tongue analysis. 3rd ed. Chi's Enterprise, Inc. Anaheim, CA. 2010.
- Fark T, Hummel C, Hahner A, Nin T, Hummel T. Characteristics of taste disorders. Eur Arch Otorhinolaryngol. 2013; 270: 1855-1860.
- Imoscopi A, Inelmen EM, Sergi G, Miotto F, Manzato E. Taste loss in the elderly: epidemiology, cause and consequences. Aging Clin Exp Res 2012; 24:570-579.
- Malaty J, Malaty IAC. Smell and taste disorders in primary care. Am Fam Physician. 2013;88(12):852-859.
Editor's note: This content was originally published in 2015 and as been updated as of August 2025.
About the Author
Nancy W. Burkhart, EdD, MEd, BSDH, AAFAAOM
NANCY W. BURKHART, EdD, MEd, BSDH, AAFAAOM, is an adjunct professor in the Department of Periodontics-Stomatology, College of Dentistry, Texas A&M University, Dallas, Texas. She is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/) and coauthor of General and Oral Pathology for the Dental Hygienist, now in its third edition. Dr. Burkhart is an academic affiliate fellow with the American Academy of Oral Medicine, where she also serves as chair of the Affiliate Fellowship Program Committee. She was awarded the Dental Professional of the Year in 2017 through the International Pemphigus and Pemphigoid Foundation, and she is a 2017 Sunstar/RDH Award of Distinction recipient. Her professional interests are in the areas of oral medicine and the relationship between oral and whole-body health, with a focus on mucosal disease and early oral cancer detection. Contact her at [email protected].