Dental strategies for osteoporosis drugs
By Lynne Slim, RDH, BSDH, MSDH
A recent two-day whirlwind trip to New York City left my head spinning as I sought to comprehend the complex world of prescribing behavior by physicians who write prescriptions for bisphosphonates and RANK-L inhibitors.
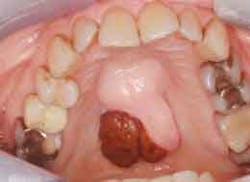
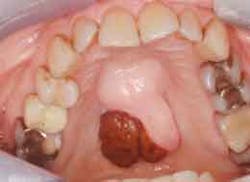
I was the only dental hygienist in a large lecture hall filled mostly with oral surgeons who were grappling with comanagement and prevention strategies for patients who are at risk of drug-induced osteonecrosis of the jaws (DIONJ). The guest faculty presenters (Robert Marx, DDS, and Richard Kraut, DDS) continued to roll out case studies of individuals (horrifying images of necrosed maxillas and mandibles) who fell victim to these offending drugs.
In last month's column, I introduced some new drugs besides oral and IV bisphosphonates that have been implicated in DIONJ pathogenesis. Oral health-care professionals need to appropriately comanage treatment protocols related to these drugs with the osteoporosis-prescribing physician.
A multidisciplinary approach to patients who are treatment planned to take oral or intravenous nitrogen-containing bisphosphonates or one of the new drugs (see Table I) should consult with an appropriate dental professional who is familiar with prevention and management protocols.1,2 Dental hygienists may want to read the American Association of Oral and Maxillofacial Surgeons (AAOMS) 2014 position paper/update on medication-related osteonecrosis of the jaw.1
In a position paper by Marx, Broumand, and Tursun at the University of Miami's division of oral and maxillofacial surgery, the authors emphasize an important point: stable oral health and careful management of all drugs known or suspected to cause DIONJ now or in the future is the best preventive measure.2 Classic preventive measures such as eliminating periodontal inflammation, treating dental caries, and removing hopeless teeth should be done before the offending drug is prescribed, since it reduces many of the initiating events that result in DIONJ.2
-------------------------------------------------------
Other articles by Slim
-------------------------------------------------------
Prevention strategies for osteoporosis-treated patients
Prevention strategies for those patients treated for osteoporosis must take into consideration the half-life of the following drugs: oral bisphosphonates, subcutaneous denosumab, and IV bisphosphonate drugs approved for osteoporosis. Neither bisphosphonates nor denosumab drugs enter or become incorporated into the teeth themselves. So treatment such as prophylaxis, restorations, crowns, bridges, nonsurgical root canal treatments, and nonsurgical periodontal treatment that does not place excessive pressure on alveolar ridges is considered safe.2
For patients who take alendronate (Fosamax), residronate (Actonel, Atelvia), and ibandronate (Boniva), Marx and Kraut recommend a presurgical nine-month drug holiday before any dento-alveolar surgery in order to support clinical healthy healing. In addition, they recommend a follow-up (postsurgical) three-month drug holiday, which can assist, for example, in normal bone regeneration and maturity, including osseointegration of dental implants.2
Drug holidays from bisphosphonates or denosumab should be initiated only by the prescribing physician. Non-bisphosphonate and non-denosumab alternatives may be suggested and used during the drug holiday instead. A multicenter, double-blinded prospective study in 2006 showed that patients with drug holidays as long as five years had no fracture risk for the treated osteoporotic patient.3
In September 2011, the FDA published a document suggesting that patients with low risk of fracture may be good candidates for discontinuing bisphosphonate therapy after three to five years.4 According to the Marx et al. position paper, the FDA recommendation is derived from the agency's exhaustive review of drug company-sponsored studies showing that there is no evidence of further fracture risk reduction beyond three years of taking a bisphosphonate and that, after five years, complications from bisphosphonate therapy rise significantly.2
Data from Marx et al. indicate that patients who take zoledronate 5 mg IV once yearly (Reclast) are at significant risk beginning with the fourth yearly dose due to the 11-year half-life of the drug and its accumulative effect. Elective alveolar bone surgeries may be best deferred until nine months after the most recent dose and three months before the next planned dose.2 If a patient has switched to Reclast after having taken an oral bisphosphonate for many years, the patient is at higher risk for DIONJ. Reclast loads the bone rapidly with 140 times the amount of a single dose of an oral bisphosphonate. A drug holiday of longer than nine months may be recommended.2
Most of the time, DIONJ associated with an oral bisphosphonate or denosumab can be effectively managed with 0.12% chlorhexidine and an intermittent course of systemic antibiotics along with a drug holiday alone or followed by surgery.2 The University of Miami database finds a 50% resolution rate for DIONJ with a drug holiday of nine months alone.2 About 40% of subjects required alveolar debridement/local alveolar resection with a nine-month drug holiday.2 Ten percent required a continuity resection of the mandible or a partial submucosal maxillary resection and a sinusostomy after a nine-month holiday consideration. Drs. Marx and Kraut also use a test called CTX that assesses the level of bone resorption. Serum cross-linked C-telopeptide of type I collagen (CTX) is a marker of osteoclastic activity.5 It is still unknown at this time whether or not this particular test can predict the risk of developing DIONJ.5
Denosumab (Prolia) has a much shorter half-life and therefore, a shorter drug holiday of six months is considered adequate.2
Once bisphosphonate- or denosumab-associated DIONJ (diagnosed in patients with osteoporosis) is treated and resolved, dental implant osseointegration can be expected as long as the drug holiday is continued for at least three months after the dental implants are placed.2
Dental hygienists should share this valuable information with general dentists and specialists and incorporate it into patient assessment and treatment planning whenever possible.
References
1. http://www.aaoms.org/members/resources/aaoms-advocacy-and-position-statements/
2. Marx RE, Broumand V, Tursun R. University of Miami, Division of Maxillofacial Surgery. Position paper on drug-induced osteonecrosis of the jaws. April 15, 2014. (unpublished)
3. Black DM et al. Effects of continuing or stopping alendronate after five years of treatment: the fracture intervention trial long-term extension (FLEX): a randomized trial. JAMA 2006 Dec 27; 296 (24): 2927-38.
4. http://www.fda.gov/ForConsumers/ConsumerUpdates/ucm309688.htm
5. Lee CY, Suzuki JB. CTX biochemical marker of bone metabolism. Is it a reliable predictor or bisphosphonate-associated osteonecrosis of the jaws after surgery? Part II: a prospective clinical study. Implant Dent. 2010 Feb; 19(1): 29-38.
LYNNE SLIM, RDH, BSDH, MSDH, is an award-winning writer who has published extensively in dental/dental hygiene journals. Lynne is the CEO of Perio C Dent, a dental practice management company that specializes in the incorporation of conservative periodontal therapy into the hygiene department of dental practices. Lynne is also the owner and moderator of the periotherapist yahoo group: www.yahoogroups.com/group/periotherapist. Lynne speaks on the topic of conservative periodontal therapy and other dental hygiene-related topics. She can be reached at [email protected] or www.periocdent.com.
Past RDH Issues