HPV: To test or not to test
by Nancy W. Burkhart, RDH, EdD
[email protected]
The dental practitioner has a responsibility to examine and assess the oral tissue status of all patients. Usually, we are happy to report that the tissue is healthy and no further treatment is necessary. Ethically, our role in assessment is both an understood practice as well as a legal one each time we interact with our patients.
Within your practice, what is the expected role in assessing and relaying advice/recommendations to our patients? Do we rely strictly on scientific evidence with evidence-based protocol? Do we trust the developers/promoters of dental products to provide information to us? Do we relay personal opinion from colleagues, or do we reject opinion-based information? Do we search the scientific literature for current information, or call our colleagues and company representatives and obtain a consensus of what the best options may be for dissemination of information?
We have all been in these situations. With busy practices, it is very time consuming to sit down and evaluate all the literature. Anyone who has been faced with a medical decision for a loved one or ourselves may actually feel exhausted while trying to sort through all of the options, treatments, and advice – some of which may even be at odds within specific group specialties in the way treatment is rendered. It can be very daunting, draining us both mentally and physically. So how do we approach this dilemma?
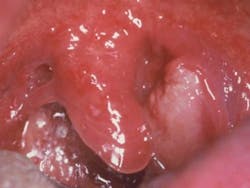
For some time, we have known about the detrimental effects of alcohol and tobacco products and the role of both in the etiology of oral cancer. Counseling a patient on discontinuing these products has become commonplace. Most of the population knows that these products are detrimental, but we still try to provide both current and factual information to our patients. Recently, considerable information has been published about the human papillomavirus (HPV) status of the patient. Both hygienists and dentists are being asked about HPV (specifically HPV 16) and its connection to oral cancer. HPV has been correlated with cancer at the base of the tongue, the oropharynx, and tonsil. Although we know that the correlation is present and oral exams are performed periodically, these areas are difficult to assess and do not appear as the typical oral tissue changes that we have been able to detect during oral cancer exams. These cancers are not easily detected through visual exams, palpation in early development, and by using some of the early cancer detection devices on the market while in early stage. Most of these cancers are detected in a late stage because the tonsillar tissue, particularly the tonsillar crypts, have many crevices and tissue surfaces that are hidden from the practitioner's view. Some individuals have disease states hidden in the tissues.
By the time the problem is observed and detectable changes are observed in the lymph nodes, the stage is much higher and usually at a Stage III or IV. Although it is so important to check the posterior areas of the mouth, it is not uncommon to find that tonsillar regions are neglected.
For many years, dentistry did not even consider this "their area of expertise or responsibility" and the examination was left to the medical community. Students now are taught to check this area thoroughly while in dental schools, and we now know that the tissue in this area of the mouth is highly linked to HPV. Because of the lack of clear visible oral lesions, the palpation of cervical lymph nodes and close examination of these areas is crucial.
An excellent oral exam video has been produced by Dr. Michael Siegel and Dr. Valerie Murrah (see references). Dr. Siegel and Dr. Murrah demonstrate the exam with a thorough focus on the cervical lymph nodes and the oropharynx.
What do we really know about HPV?
A recently published letter written by Dr. Mark W. Lingen (2010) addressed the issue associated with the saliva test that is being offered in dental offices with on-site training by representatives of the company manufacturing the test. In the paper, he states that it appears that this test "is a test looking for a disease." He additionally questions whether knowing if one is HPV positive really means anything that is clinically significant for the patient.
Most of the time HPV is cleared from the body through its own immune system. If the person is tested again at a later date, the results in most cases will be negative. Some individuals who have ongoing positive results could be more susceptible to oral cancer.
Essentially, we really do not know very much as to how this entity behaves in all individuals. We cannot predict in whom the virus will persist.
Overall, we do know that some individuals are more susceptible to certain disease states and cancers. As an example, we know that some individuals in their eighties and nineties have smoked all their lives, and yet they do not develop oral or lung cancer. Why is one individual affected and not another? Clearly, there are multiple factors playing a role in the development of disease states, and this may be genetically and environmentally influenced. Dr. Lingen also suggests that those reading his article may want to peruse a published article by Dr. Jaeschke et al. on a user's guide to the medical literature. It is instructive in how to use an article promoting a diagnostic test (see references).
With the continued rise of oral cancer in the under 40-year-old age group without known risk factors, what do we really know about HPV?
- We know that we are seeing oral cancer in the younger age groups (under 40 years old) with no historic risk factors, such as tobacco and alcohol.
- We are finding posterior of the mouth cancer at advanced stages with often occult primary lesions in the oropharynx, base of the tongue, and tonsillar tissue. Most of the time these do not produce the historic surface lesions we are accustomed to finding. Neck palpation for hard, painless, fixed nodes is becoming increasingly important as a component of the oral exam.
The CDC estimates that 20 million Americans are currently infected with HPV. This number is constantly changing as new data becomes available.
- 50% of sexually active adults will be infected with HPV in their lifetime.
- The National Cancer Institute estimates 36,540 oral cancers in 2010 with 7,880 subsequent deaths within the United States. These numbers vary with some of the large research institutes conducting current research.
I recently presented a seminar on mucosal diseases at a national meeting and introduced some ideas of my own. I found that I really could not even answer my own questions based on the research I read. Consequently, I then turned to open dialogue with those whom I knew had studied the literature on the subject. Unfortunately, I was less clear after assessing the information than I was at the start of my search. If I was not completely clear, what would I tell patients or students who asked the following?
- Does kissing transfer the HPV and make the other person susceptible to oral cancer? How much of a deep passionate kiss do you need to transfer the HPV? How would you even begin to test this assumption?
- Is a child at risk if the mother is HPV positive?
- Can HPV be transferred if the mother tastes her baby's food before giving it to the child? Since this is a rather common practice, should we be concerned about contagion? This is always a question that a patient will ask when diagnosed with any disease state.
- Is an HPV positive person more at risk if he/she uses tobacco and alcohol together? Or, is one more of a risk than the other? Is a person who may be genetically susceptible to cancer more affected by the trio of alcohol, tobacco, or HPV?
- Is the HPV an entity that can be harbored for years and then reappear? If you are in a relationship, does this open up the questions of fidelity? And, how do you help the patient answer this question, or can you possibly provide any answers?
- Do you test all patients, or just some known high-risk groups?
- Do you check adolescents who may or may not admit to sexual activity? Do you talk to the parent first before even asking? What would be the reaction of a parent? As you know, adolescents and even some much older individuals do not consider oral sex to be "true" sex, so your phrasing and communication is crucial.
- Do you recheck a positive patient again and at what intervals?
- Who should talk with the patient? How confidential is the information?
- Do you check the entire family for HPV? Do you check at intervals?
- Do you test patients for HPV who have had a previous oral cancer at every appointment?
- Does the constant bleaching of teeth (practiced by many under 40 years of age) affect the oral tissues in some individuals, and does HPV affect this tissue after or during bleaching?
- Does GERD and frequent heartburn make the tissues more susceptible to HPV in some individuals – possibly those with a genetic predisposition?
Finding the answers to our questions about HPV
I have pondered these questions for several months now and discussed all these questions with many colleagues who have expertise in oral medicine and pathology. I don't know the answers to these questions in the depth needed to make clear recommendations. Frankly, I am amazed at how fast the dental/dental hygiene community has embraced the addition of promoting HPV testing in the dental office without knowing the answers to many important questions related to HPV.
We must do our own critical thinking about new information and the ramifications of that information for our patients. It is clearly never a sound idea to automatically discount information because it is new and maybe not in line with our current thoughts or those of our trusted fellow professionals. Progress in research is based on innovation, analysis, and critical thinking.
I, for one, believe that we have in some ways lost touch with the promotion of innovation and critical thinking. They are intertwined. Most people who are in research and education have a strong innovative side and those people who go into specialty areas in dentistry often have an investigative/innovative side as well. So what are we to accept and to believe and how do we assess new information? And, when is there enough evidence-based information to suggest new protocol to our patients?
Steven Berlin Johnson, in his new book, "Where Good Ideas Start," states that alcohol was used as a "cure all" in early English history. We know that there is a depressant effect to alcohol. As time progressed, it was found that the new coffeehouses in England provided not only the stimulant brew of coffee, but it was determined that the arousal of ideas was prevalent as well. I am not suggesting that we all drink coffee and sit around discussing our ideas, but open pathways for discussion are key.
This promotion of discussion and sharing ideas goes back to early years when Ben Franklin led discussion sessions and the "Junto Groups" of like-minded craftsmen and townspeople came together to discuss the topics of the day.
Any time you have a group of people who gather and discuss ideas, new information is shared and new ideas flourish. The Internet has provided the opportunity in which discussion board participants post questions, relevant ideas can be debated, and critical thinking is promoted. This is true for many of us in the dental community where it is so easy to accept ideas from others in our profession. But we need to raise these questions, listen to other views, and critically analyze information. The Internet has provided a sounding board where patients, researchers, practitioners, and family members come together, ask questions, and discuss areas of concern.
An Internet site and discussion board was founded by Brian Hill of the Oral Cancer Foundation, Inc., and Brian is an oral cancer survivor himself. His organization provides educational materials, lectures and discussion postings for those who have been diagnosed with oral cancer. The group also supports family members dealing with oral cancer.
Brian has been instrumental in calling attention to the screening process and the importance of the oral exam, along with its role in early detection. He has been instrumental in the discussion of the role of HPV in oral cancer and calling attention to the risk factors for oral cancer with the distribution of educational materials. The Web site for the foundation is: http://www.oralcancer.org", and a section of the site is devoted to HPV.
It is interesting that so little time is spent trying to provide information on nutrition and lifestyle modifications that clearly impact the health of all patients. Yet, dental personnel are being asked to counsel patients about sexual practices and personal medical information with regard to HPV status. If we do provide this counseling, what are the long-term ramifications?
A phenomenon in the medical field is known as "white coat syndrome." Patients experience and test very high for blood pressure readings when they enter a medical office. Cardiologists are aware of this phenomenon, even among regular patients. We know how powerful the mind is, and there is no doubt that some disease states can actually develop due to prolonged stress and are termed "health anxiety." The mind-body connection is very strong. Are we really ready to deal with all the psychological problems that may develop in our patients when given test results for HPV status? And, as Dr. Lingen so eloquently stated, do we really have enough information and what do the results really mean anyway?
Lastly, are we creating more problems than we are attempting to solve? Asking questions, discussing issues, and assessing the evidence is always necessary.
Keep asking good questions and always listen to your patients!
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and co-host of the International Oral Lichen Planus Support Group http://www.bcd.tamhsc.edu/outreach/lichen/ and coauthor of General and Oral Pathology for the Dental Hygienist. Her Web site for seminars is www.nancywburkhart.com.
REFERENCES
Burkhart, NW. Squamous cell carcinoma of the tonsil. RDH November 29:11 2009.
Johnson S. Where good ideas come from: The natural history of innovation. Riverhead Books, New York. 2010.
Lingen MW. Editorial in Oral Surg Oral Med Oral Pathol Oral Radiol Endod 110:3, Sept.2010.
Jaeschke R, Guyatt GH, Sackett DL. Users' guides to the medical
literature. III. How to use an article about a diagnostic test. What
are the results and will they help me in caring for my patients?
The Evidence-Based Medicine Working Group. JAMA 1994;
271:703-7.
Ryerson AB, Peters ES, Coughlin SS, Chen VW, Gillison ML, Reichman ME, Wu X, Chaturvedi AK, Kawaoka K. Burden of potentially human papillomavirus-associated cancers of the oropharynx and oral cavity in the US, 1998-2003. Cancer Nov 15:113 (10 suppl) 2901-9.
Siegel M , Murrah V, Aloise D. Head, Neck and Oral Cancer Examination. MedEdPORTAL; 2009. Available from: http://services.aamc.org/30/mededportal/servlet/s/segment/mededportal/?subid=7768.
http://www.cancer.gov/cancertopics/types/oral
http://www.cdc.gov/eid/content/16/11/1671.htm
Past RDH Issues