Case #5
A 68-year-old edentulous male visited a dental office for evaluation of numerous bumps under his upper denture.
History
The patient stated that he had been aware of the bumps under his upper denture for approximately six months. The patient claimed that, during the past six months, the involved area did not appear to increase in size. When questioned about any irritation to the region, the patient commented that his upper denture had been constructed approximately four years earlier and no longer fit very well. The patient described the bumps as painless.
At the time of the dental appointment, the patient’s medical history was reviewed and included a history of coronary artery disease and hypertension. Medications at the time of the dental examination included nitroglycerin, as needed for angina, and Inderal LA. The patient’s past dental history, since full-mouth extractions approximately 10 years earlier, consisted of sporadic examinations, the construction of two sets of complete dentures, and denture adjustments.
Examinations
The patient’s blood pressure was slightly elevated; all other vital signs, however, were found to be within normal limits. Examination of the head and neck region revealed no enlarged or palpable lymph nodes. No significant or unusual findings were discovered during the extraoral examination.
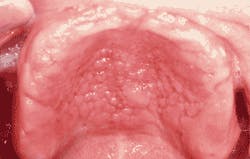
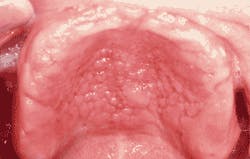
Intraoral examination revealed multiple, soft-tissue papillary growths in the area of the palatal vault (see photo). The mucosal surface of the papillary areas appeared intact and reddish in color. The papillary regions were described as painless when compressed.
Further examination revealed no other areas of involvement of the oral cavity.
Clinical diagnosis
Based on the information available, which of the following is the most likely clinical diagnosis?
❏ nicotine stomatitis
❏ inflammatory papillary hyperplasia
❏ inflammatory fibrous hyperplasia
❏ denture sore mouth
❏ verrucous leukoplakia
Diagnosis
■ inflammatory papillary hyperplasia
Discussion
Inflammatory papillary hyperplasia (also known as denture papillomatosis) is a common benign condition that occurs under a denture. Inflammatory papillary hyperplasia (IPH) is a reactive condition and is related to one or more of the following:
• Chronic trauma or irritation from an ill-fitting denture
• Poor denture hygiene
• The wearing of a denture 24 hours a day.
Inflammatory papillary hyperplasia is estimated to occur in 20 percent of individuals who wear dentures 24 hours a day. In very rare instances, IPH may occur in patients without dentures.
Clinical features
Inflammatory papillary hyperplasia may be seen in any individual that wears a complete or partial denture.
There is no sex predilection. Inflammatory papillary hyperplasia presents as numerous, small papillary projections of the mucosa that results in an overall pebbly or “cobblestone” appearance. Each papule is very tiny and measures less than 2-3 millimeters in diameter. When compressed, the papules are painless.
The mucosal surface of IPH is typically intact and appears normal in color or erythematous. Although IPH most often affects the tissues of the palatal vault, any area of palatal mucosa, including the maxillary edentulous ridges, may be involved. Less frequently, IPH may develop on the edentulous mandibular alveolar ridge. Inflammatory papillary hyperplasia is usually asymptomatic; some cases, however, are associated with denture sore mouth.
Diagnosis
Based on the clinical features, IPH is rarely confused with other papillary lesions. Occasionally, IPH may be mistaken for a condition of the hard palate associated with smoking such as nicotine stomatitis. The characteristic appearance of IPH and the history of an ill-fitting denture, however, is usually sufficient to establish a clinical diagnosis. In such cases, a biopsy is unnecessary. In cases where a clinical diagnosis cannot be definitively established, a biopsy is necessary. When examined histologically, IPH exhibits numerous papules covered by hyperplastic stratified squamous epithelium.
Treatment
Inflammatory papillary hyperplasia does not disappear spontaneously or regress with time. The treatment of choice for IPH is surgical removal. Options include surgical excision, curettage, electrosurgery or cryosurgery. In addition to surgical removal, the construction of a new denture or relining of the existing denture is necessary in order to prevent further irritation and subsequent recurrence of the lesion.
After treatment and denture fabrication or denture relining is completed, the patient should be urged to remove the denture at bedtime and to maintain good denture hygiene. In addition, the patient should be reassured that this lesion is reactive in nature and not malignant.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.