HYPERTENSION the silent killer
Hypertension - Once you have it, it’s yours for a lifetime. But with lifestyle changes, it can be treated and managed. Do you know your numbers?
Does this sound familiar? It doesn’t hurt, you feel no pain, and there are few symptoms, so why treat it? One would almost think I was discussing periodontal disease. But periodontal disease possibly will not kill you. Hypertension, with the same mantra, will. According to the U.S. Census Bureau and the National Health and Nutrition Examination Survey, approximately 65 million (one in three) Americans have high blood pressure, 8 percent more than the last decade. Almost 32 percent of those are unaware of their condition. Less than 60 percent of those diagnosed with hypertension are receiving treatment, with only one-third under good control. As with periodontal disease, once you have it, it is yours for a lifetime. Again, similar to periodontal disease, with lifestyle changes, it can be treated and managed.
Hypertension has been cited as the fourteenth cause of death in 2001 and contributed to countless other deaths. With much of the current health news focusing on Americans and obesity, it is no wonder that there is a huge increase in the numbers of hypertensive adults in this country. It also follows - with our aging population - more will be diagnosed in the future. The average American over age 55 will exhibit some form of hypertension. Those who do not have the numbers by age 55 have a 90 percent chance of developing it during their lifetime. The odds are truly against us.
What is hypertension, how do we live with it, and what can be done to treat it?
As we all remember from physiology class, blood pressure has two components: systolic pressure, which is the force within the arteries when the heart beats, and diastolic pressure, which is the force when the heart is at rest. Hypertension, or high blood pressure, occurs when there is too much resistance in the arterial system, causing increased pounding of blood throughout the system. This will ultimately cause damage to the heart via cardiac hypertrophy and possible heart failure. In addition, arterial damage will occur with thickening of the arterial walls and atherosclerosis, leading to possible aneurysms, cardiovascular disease, or strokes. High blood pressure will eventually damage organs such as the kidneys, brain, and eyes. Dizziness, headaches, fatigue, and tinnitus may occur as symptoms, but hypertension is usually asymptomatic.
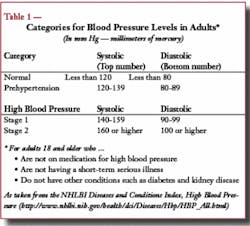
Since hypertension is a relatively silent disease, the only manner of testing is with a blood pressure reading. Historically, the National Classification System, created in 1997, defined high blood pressure as a systolic reading over 130 mm Hg and a diastolic reading over 85 mm Hg. Newer protocols, created by the National Heart, Lung, and Blood Institute’s National High Blood Pressure Education Program (NHBPEP) and the Joint National Committee (JNC),** were issued last year to update the regime now followed by physicians. A blood pressure of 120/80 was considered “normal.” The suggested new goal for normal is 115/75. Under the new guidelines, 120/80 is prehypertensive, which recognizes that even small increases in blood pressure lead to an added risk. This new category places 45 million adults in this range. Additionally, the indicators for prehypertension do not have to be both factors, but could be a rise in either of the components. Whereas diastolic numbers were focused on previously, systolic numbers are now looked at as the indicator of current and future disease, especially in adults over age 50. Now, high blood pressure is further broken down into two stages, with readings of 140/90 considered hypertensive. Again, when the systolic and diastolic components fall into two separate categories, the higher one is used as an indicator to classify the blood pressure (see Table 1).
Hypertension may have no causative factors, although there are several risk factors that may increase the chance of developing the disorder. Age is a critical factor. As we age, our vessels become less elastic and there is increased resistance for the blood to flow through the arteries, due to the increased force necessary. Obesity is clearly another risk factor. With increased weight and girth, the blood strains to pass through the system. A familial history of hypertension is also considered a key risk factor, with or without any other concurrent factors. A diet rich in salt, poor in potassium, high in fat, with an increased consumption of alcohol will also increase the risk. High levels of stress, smoking, and little to no exercise do not help the situation. For women, oral contraceptives may be linked to high blood pressure, especially in women who are overweight. Pregnancy may also increase blood pressure, especially during the last trimester. After menopause, women are more likely to have an increase in blood pressure. Finally, young black women have been shown to have a higher incidence (1:3) of hypertension than white women (1:4) (see Table 2).
There are several types or subclassifications of hypertension. Approximately 90 percent of all hypertensive adults have essential hypertension. This form is idiopathic, although most patients do have a familial history, and usually begins at the age of 30, but may occur later in life. Isolated systolic hypertension is the most common form of high blood pressure in the elderly. It is due to the arteriosclerosis and the concomitant increased need of pressure to accommodate blood flow from the heart. Historically, this was just looked upon as normal aging, but currently, it is treated more aggressively with medications.
Secondary hypertension is due to other medical conditions, as well as drug-related increases in blood pressure. An increase in blood pressure can be seen with polycystic kidneys, renal artery obstruction, coarctation or narrowing of the aorta, hyperfunction and hypofunction of the thyroid, hyperfunction and hypofunction of the adrenal cortex (Cushing’s syndrome and aldosteronism), pheochromocytoma (a tumor of the adrenal medulla, which secretes epinephrine and norepinephrine in addition to other chemicals), as well as sleep apnea. With the treatment of the primary medical issue, blood pressure may return to its normal level. Drugs that can elevate blood pressure include over-the-counter cold remedies, nasal decongestants, appetite suppressants, and NSAIDs. Prescription medications that may cause an increase in blood pressure include corticosteroids, tricyclic antidepressants, cyclosporine, erythropoietin, and COX-2 inhibitors.
White coat hypertension (which my husband has whenever he comes into my office) is due to anxiety of approaching a health-care professional. Most likely, our mere presence will raise the blood pressure of many folk! It usually occurs around physicians, but, as many patients have proved, this type of hypertension will often occur when a dental visit is imminent.
Labile hypertension will cause symptoms of headaches and tinnitus, due to the constant fluctuation of blood pressure. People affected with labile hypertension often react to emotional stress with an increase in blood pressure. Many of these patients are treated with antianxiety medications. These patients with part-time high blood pressure are at the same risk level of damage induced by the stress as a patient with full-time hypertension.
Malignant hypertension is characterized by sudden extreme rises in blood pressure. Symptoms may occur such as severe headache, apnea, angina, nausea and vomiting, blurred vision, seizures, and loss of consciousness. Although rare, it places the individual at a greater risk for stroke, heart failure, permanent kidney damage, hemorrhagic stroke, and cerebral edema, and should be considered a medical emergency. This form of hypertension may occur in less than 1 percent of the patients who already experience high blood pressure. It may occur with an abrupt stoppage of antihypertensive medication.
Approximately 6 to 8 percent of women will exhibit hypertension during pregnancy. Chronic hypertension may occur during the first 20 weeks. During the second 20 weeks, chronic hypertension may also continue, due to either essential or secondary hypertension. Patients experiencing chronic hypertension may have their blood pressure elevated postpartum. These women are at a higher risk for developing preeclampsia. Additionally, women in their second half of pregnancy may experience gestational hypertension due to estrogen increases. This form of hypertension will go away within 12 weeks postpartum. Preeclampsia, or toxemia of pregnancy, will cause tightening of the arteries throughout the mother’s body, especially in the placenta, in addition to blood clotting, causing high blood pressure. These patients will have an increased level of proteinurea (after 12 weeks) and exhibit edema. Seizures may occur. The only “cure” for preeclampsia is delivery of the baby (see Table 3).
Hypertension is treated in several ways. Depending on the level of the numbers, lifestyle changes may be the first line of defense (see Table 4). The prime goal would be to aim for a healthy weight. Monitoring fat intake, following a heart-healthy diet, limiting salt and sodium, and watching for hidden salts and sugars in processed foods will all assist in weight management. In addition, following daily recommendations for consumption of fruits and vegetables to ensure proper nutrition and eating foods high in omega-3 fatty acids help to maintain cardiac health. Decreasing the number of alcoholic beverages consumed on a daily basis will also assist in lowering blood pressure. And, of course, smoking cessation is crucial to good health.
The second goal would be to become more physically active. This is one of the hallmarks of a healthy lifestyle. Get off the couch. Walk. Run. Play a sport. Take the stairs. It doesn’t matter what you do to be active - just move. Following the recommendation of performing a minimum of 30 minutes of exercise a day will improve both your cardiovascular and mental health.
An additional method to assist in lowering blood pressure is stress management. Stress will ignite our “fight-or-flight” mechanism, thereby increasing our heart rate and blood pressure. During a stress episode, signals are sent to the hypothalamus from all over the body, and involuntarily, we react. The occurrence triggers the “fight-or-flight” survival response, mediated by the autonomic nervous system, the hypothalamus, and the endocrine system. Stress may be either physical (illness, injury, trauma, infection) or psychological. Regardless of whether the causative agent is actual or perceived, the body’s reaction is still the same.
Stress can affect bodily systems without having an offending physical presence, as is the case with anxiety. According to the Merriam-Webster dictionary, anxiety is “an abnormal and overwhelming sense of apprehension and fear often marked by physiological signs (as sweating, tension, and increased pulse), by doubt concerning the reality and nature of the threat, and by self-doubt about one’s capacity to cope with it.” Anxiety occurs because of fear or tension without any definitive cause but will elicit a response in the autonomic nervous system to release epinephrine to elicit the symptoms discussed in the definition. This definitive correlation between the mind and the body may affect our health.
We need to be able to manage our stress. Practicing relaxation techniques may sound hokey, but it has been proven to lower blood pressure and maintain calmness. Meditation, progressive muscle relaxation, visualization, and practiced breathing are all components of relaxation techniques. Expressing your feelings, removing stressors in your life that are removable (saying “no” on occasion), in addition to managing time more profitably, will all decrease your stress load.
When all of the above interventions of diet, exercise, and personal stress management do not reach the recommended goal, medications may be added to the protocol (see Table 5). Myriad medications are available, which are directed to different components of the hypertensive episode. Diuretics, which are usually the first medication of choice, may be utilized alone or in concert with another medication. They assist in eliminating sodium from the kidneys, which will eliminate water. This will reduce the volume of fluid passing through the arteries, hence lessen pressure on the arterial walls. Diuretics will also decrease edema, which results from congestive heart failure.
Angiotensin II, a hormone, causes the arteries to constrict. ACE (angiotensin converting enzyme) inhibitors decrease the level of angiotensin II circulating in the system, causing dilatation of blood vessels and allowing for a decreased resistance to blood flow. This drug will also inhibit cardiac stimulation and kidney absorption of sodium. ACE inhibitors are also used to treat symptoms of heart failure. Angiotensin antagonists (or angiotensin receptor blockers) prevent the angiotensin II from having an effect on the heart by blocking the action of the hormone, thereby eliciting a similar effect as the ACE inhibitors. They also suppress the renin angiotensin system. Both drugs prevent the blood pressure from rising.
Calcium channel blockers are also called calcium antagonists, because they stop the movement of calcium into the cardiac muscles and blood vessels, thereby relaxing the tissue as well as dilating peripheral arterial vasculature. Some of these medications will slow heart rate. Calcium channel blockers are also used to treat angina, tachycardia, and may be used for migraines. Click here to view Type of Medications Used to Treat Hypertension...