The trouble with breathing
by Sheri B. Doniger, DDS
Breathing. We can't live without it. Yet some of our patients are affected by two major pulmonary diseases — asthma and chronic obstructive pulmonary disease — that may have an impact on our time with them. We also need to be aware of how these health issues may affect our treatment protocols.
Asthma is a worldwide problem that affects both adults and children, costing more than $16 million dollars. It affects an estimated 7.2 percent of the world's population, with 6 percent occurring in adults and 10 percent in children. In the United States, it affects 5 percent, or 17 million people. This is a 27 percent increase from 1993 to 1998. The highest incidence occurs in children younger than 18, and this decreases with age.
The asthmatic condition
Asthma affects quality of life. People who suffer from asthma lose time from work and school. Asthma attacks cause unscheduled visits to the physician and may alter lifestyle experiences. Outdoor activities may need to be curtailed or eliminated to accommodate asthmatic individuals. Asthma is the most common chronic illness for hospitalizations among children. The good news is that the bronchioconstriction of asthma is partially reversible, either spontaneously or with treatment.
In people without asthma, air is passed through the respiratory system from the nose and mouth, through the trachea to the branching bronchi. These bronchi are constantly splitting into smaller components, finally ending in approximately 300 million alveoli, where gas exchange occurs. The airway is usually self-protected via mucocilillary clearance. Airborne particles are trapped with respiratory epithelium that contains mucous-secreting cells. Some cells also have cilia that sweep debris toward the mucous-retaining cells. The mucous is eventually expelled from the body through either coughing or swallowing. The internal walls of the bronchi contain muscles that are autonomically controlled, which is another self-protective device.
The respiratory system, with the assistance of the immune system, counteracts all the infectious, toxic, or particulate agents that enter the system. The bronchi are capable of several methods of self-protection. They can call up inflammatory cells from the circulatory system that will directly phagocytize, or attack organisms via cytotoxic secretory enzymes. The bronchial wall is also capable of swelling to constrict passages from further access of offending materials. The mucous that is secreted via the respiratory epithelium also contains the invaders. Finally, the airway may be constricted.
The immune system is composed of three parts: antibodies, inflammatory cells, and inflammatory mediators. The two main components of the immune system are the humoral and cellular response. Antibodies are proteins that identify and bind to foreign particles (antigens), then alert the rest of the immune system to eliminate the substance.
There are five types of antibodies produced by the B-lymphocyte cells, and each type has specialized functions. IgE is the antibody directly involved in the allergic immune response. The antigen (or allergen) stimulates the IgE. Inflammatory cells consist of either granular or non-granular (lymphocytes). The most important granular cells in asthma are the mast cells and eosinophils. Additional inflammatory mediators such as histamine, leukotrieines, prostaglandins, platelet activating factor, additional enzymes, and cytokines are also components of the immune system response.
Asthma develops from airway inflammation. The reaction occurs when no serious infection, toxin, or invading particles begin the inflammatory response in the bronchi. The airways become inflamed due to direct response of the immune system to stimuli, which would not normally cause a response. This sets off the cascade of immunologic responses leading to the immune-mediated process that leads to inflammatory changes in the airway (eosinophil recruitment and airway edema). Histologically, the airway exhibits plasma leakage causing edema and thickening in the bronchial wall. The excess mucous secretion can block the airways. Smooth muscles contract more to protect the airways, therefore decreasing air exchange capability. The bronchi become hyper-reactive and exhibit constriction. All this prevents proper airflow into the lungs.
Asthma is usually diagnosed via clinical features such as recurrent episodes of wheezing (predominately on exhalation), breathlessness with exercise or activity, breathlessness with wheezing, dyspenea, chest tightness or soreness with coughing or deep breathing, early morning cough, and nighttime breathlessness or wheezing. Airflow limitation is also a symptom.
Asthma is usually worse at night and is exacerbated in the presence of allergens, cold air, and exercise. Laboratory tests to diagnose asthma include many pulmonary function tests (spirometry, peak expiratory flow rate) in addition to allergy skin tests, blood tests, and X-rays.
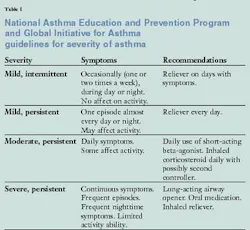
Asthma has four levels of severity (see Table 1). The classifications are based on symptoms and lung function prior to medical intervention.
There are also many varieties of asthma:
• Seasonal asthma is usually connected to the common cold.
• Cough-variant asthma has a cough as the primary symptom. This type occurs mainly at night and without wheezing, and affects more children than adults.
• Occupational asthma occurs due to inhaled chemicals or antigens over a long period of time during the workday. Patients are sensitized to the specific agents and exhibit symptoms to those agents. Some may also develop additional triggers. Removal of exposure to these occupational sensitizers usually returns the patient to normal.
• Nocturnal asthma usually occurs during the night and is considered characteristic uncontrolled asthma.
• In patients with exercise or athletically induced bronchioconstriction, the symptoms of asthma occur either during or shortly after vigorous exercise. Exercise may trigger an asthma attack in patients with any type of uncontrolled asthma.
• Asthma symptoms may also be triggered by aspirin or any non-steroidal inflammatory. This accounts for 5 to 10 percent of all patients and primarily affects adults. Some asthma patients may not respond to corticosteroid treatment.
Asthma may be treated by inhaled or oral forms of medication. The inhaled delivery system can be either a metered dose device that uses a chemical propellant to expel the medication out of the inhaler, or a dry powder that is breath activated. If a patient is unable to use the inhaler, he or she may use a nebulizer, which is a compressor-driven device that converts the medication to a mist, similar to a humidifier.
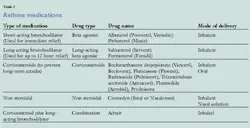
Asthma medications are either relievers or controllers. Relievers are rescue drugs that are short acting and used for quick relief. Controllers are long acting but can't be used to treat an asthma attack (see Table 2). Oral corticosteroids are used in a five to ten day course to reduce inflammation and mucous production in severe and persistent asthma. Newer drugs such as leukotriene inhibitors (Accolate and Singulair) are being used to block leukotrienes, which are chemical mediators that lead to the restricted airways and inflammation. Theophylline such as Slo-Bid and Theo-Dur can be taken orally to manage nocturnal asthma.
The role of the health-care provider
Eliminating triggers is an important step in reducing the number and severity of asthma attacks. Avoiding contact with cigarette smoke, being aware of pollen counts and air pollution readings, altering activities such as exercise, and avoiding cold air are a few things that will reduce asthmatic triggers. Since the common cold, flu, or allergies may trigger an asthma attack or make asthma worse, flu and allergy shots are recommended. Medical office personnel need to be aware of flowering plants, overpowering scents due to air fresheners, and possible material allergies that could trigger a patient's attack.
Patients may have different inhalers to treat symptoms — one for short-term relief and one for long-term airway opening. The long-term asthma controllers are prescribed for night relief. Physicians frequently request that patients pre-treat with medications (either albuterol or cromolyn) before exposing themselves to any potential asthma-inducing event.
Medical history updates should be performed at every patient's dental visit. Patients should be questioned concerning recent changes in health status, medication changes or hospitalizations. It's also important for patients to bring all of their inhalers to an appointment. The inhalers should be easily within reach during all dental treatments. When we request an update of their medical conditions, we must also ask if they have recently used their asthma medication. We must also consider that anxiety may be a trigger for an asthma attack; therefore, it is better to be proactive and have the inhalers handy.
Three dentally related side effects of the inhaled asthma drugs can occur:
• Dry mouth or xerostomia is common. The cause of xerostomia is twofold. Patients tend to be mouth breathers due to their inability to get a full breath, and the direct action of the medications (especially corticosteroids) causes a decrease in salivary flow. Higher caries level may result in these patients. Meticulous oral hygiene and fluoride regimens should be followed, in addition to drinking copious amounts of water to maintain the oral cavities moisture levels.
• With use of corticosteroid inhalers, erythematous or acute atrophic oral candidiasis infection may occur. This appears as a red diffuse lesion where the spray hits the soft palate.
• Irritation from the inhaler rarely exhibits as reddish macular lesion (angina bullosa hemorrhagica) in the soft palate region. These are blood blisters that diminish when use of the inhaler is stopped. On rare occasions, drug toxicity affects are noted and the offending medication is changed.
Chronic obstructive pulmonary disease
Chronic obstructive pulmonary disease (COPD) is a permanent obstruction of airflow from the lungs. It is a slowly progressive disease during which loss of lung function occurs. According to the World Health Organization, COPD was the fourth leading cause of death worldwide in 2000. It also ranks fourth in the United States. Due to pollutants, it's expected to move into third place by the year 2020.
COPD results from long standing bronchitis, chronic obstructive bronchitis, or pulmonary emphysema, often caused by smoking or air pollution. Chronic obstructive pulmonary disease shares symptoms with both chronic bronchitis and emphysema, which include chronic cough and sputum production. Shortness of breath is also pathonmemonic and may be the first indication of the disease (see Table 3).
Since there is no cure for COPD, treatment is designed to relieve the symptoms and improve the quality of life. Treatment modalities include oxygen therapy if blood levels of oxygen are low, anticholinergic or symphathomimetic bronchodilators, antibiotics, mucolytics, and corticosteroids.
Lifestyle alterations such as smoking cessation and avoiding smoke-filled areas are suggested. Other recommendations include proper exercise, drinking at least eight glasses of fluid a day, use of a humidifier at home, and changing the work environment to decrease the exposure to irritants or pollutants.
For COPD patients, dental procedures may need to be altered with respect to time spent in treatment and inclination of the dental chair. Again, it's prudent to remind the patient to take all medications and have inhalers available in the operatory during any procedures. Air abrasion may be contraindicated. Discussing lifestyle factors such as smoking and exercise enriches the patient's knowledge and informs the practitioner about possible referrals to additional health care workers.
Breathing is something most of us take for granted. When taking every breath is a challenge for one of our patients, we need to be aware of treatment factors that may make the patient more comfortable in both body and mind.
The author wishes to thank Dr. Deeba Masood and Mr. Jeff Gartman for their invaluable assistance in writing this article.
Sheri B. Doniger, DDS, practices in Lincolnwood, Ill. She graduated from the University of Illinois College of Dentistry in 1983 and obtained her bachelor's degree in dental hygiene from Loyola University of Chicago in 1976. She can be reached at (847) 677-1101 or [email protected].
References available upon request.