Dental emergencies at school
By Jennifer S. Sherry, RDH, MSEd and Faith Y. Miller, RDH, MSEd
Treating playground injuries
School nurses often encounter emergencies related to the mouth. Beyond the recognition of oral disease such as decay, the school nurse needs to be ready to triage common dental injuries in the school setting. Preparation is key in order to properly manage a dental related emergency.
The health of the mouth and the teeth is integral to the overall health of the body. Disease or injury may make it difficult for the child to concentrate on his or her studies; thus, any immediate needs to alleviate dental problems should be addressed. Many diseases are noted by dental or other health professionals if they are trained to detect them at their earliest stages. If local school districts are fortunate enough to have school nurses, however, they are likely the first to see oral health problems. If school nurses are trained to inspect, recognize, and document oral health problems, children may get the much needed help and be more successful in their academic and social lives.
While most schools have a system in place to conduct oral health screenings — whether the nurses actually conduct the screenings or refer to an outside entity — the day-to-day management of such issues as dental-related emergencies may be more of a concern. Information on management may come from local dentists and perhaps dental hygiene programs that are in the area. In this case, collaboration with this type of program can be beneficial both to the school nurse and to the dental professional.
Dental Triage and Emergencies
If they get hurt at school, this can be a scary time for children. One-fifth to one-third of all children are affected by dental injuries by age 12, and prevalence of dental injuries continues to increase throughout adolescence. Dental injuries due to sports are likely to occur in the school setting (Krause-Parello, 2005).
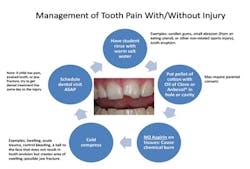
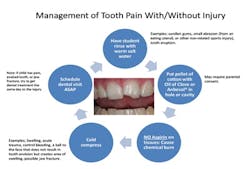
The key with oral injuries is to keep the child calm so one can assess the severity of the wound. The related figures included may be reprinted and used by the school nurse as a ready reference to react more quickly to the acute needs of the injured child (see Figure 1). Anecdotally, it is common for children to enter the school nurse’s office complaining of tooth pain without a specific injury.
Some helpful suggestions nurses can employ to assist children in their time of need are mentioned below.
It also may be a great idea for the school nurse to have a separate oral health first-aid kit readily available for emergency use. First, try having them swish with some warm salt water. If the child has an obvious cavity in a tooth, take a pellet of cotton with oil of cloves or Anbesol to help with the pain.
Please note that, before using any medicaments on a child, parental consent may be required. This is something that can be handled when the child is registered for school and kept on file. The parent should, however, be notified immediately if an injury occurs while the child is on school property, and allow the parent to make a decision on how urgent they feel the need is for the child to receive further treatment. Make sure not to use aspirin on the gum tissues. This will cause a painful burn and be worse for the child. Another item to try is a cold compress for pain control and attempt to schedule a dental visit as soon as possible.
Moderate to severe bleeding can occur due to an injury at school or on the playground. Apply pressure with sterile gauze and when bleeding subsides, use a cold compress. If the child experiences continued bleeding after 15 minutes, they must go to the dentist or emergency room.
The school nurse may suspect a jaw fracture due to an injury. Have the child bite together and assess the relationship of how the teeth fit together. Place a cold compress on the injured area and stabilize the jaw by tying a scarf or a neck tie around the head. This will help until the child can be seen by emergency personnel.
According to McIntyre (2009), if a child has an avulsed (knocked out) tooth, locate the tooth, if possible. Handle the tooth by the crown, not the root. Reinsert the tooth and hold it in place with sterile gauze. Or, if the tooth cannot be inserted, place it in saliva or milk until the child arrives at a dentist or emergency room. The American Academy of Pediatric Dentistry offers a flow sheet (see references for website address) titled, “Decision Trees for Management of an Avulsed Permanent Tooth.” The flow sheet contains two possible scenarios for management of avulsed teeth. Again, the images can be inserted into a notebook utilized by the nurse in such an emergency. However, they may not know which scenario is applicable; therefore, immediate dental treatment is necessary.
Other Dental Concerns
For treatment of canker sores, the school nurse may try Orabase with benzocaine, vitamin E oil, or an ice pack. The child will need to avoid salty, spicy, or acidic foods such as orange juice, spaghetti sauce, or bacon.
Children with braces or other orthodontic appliances are a common sight in most schools today. Frequently, a child with braces will be injured at school. The school nurse can use a tongue depressor to bend a wire away from the gum tissue or apply dental wax or gauze to the area. If there is a loose bracket, the best thing to do is to remove it so the child does not inhale it into the lungs.
Dental emergencies can occur at any time during a typical school day and need to be addressed efficiently and effectively by the school nurse on staff. Injuries and acute dental pain are problems that can arise, and the students should be treated and/or referred to a dentist for palliative care. The more successful the school nurse is in addressing the dental emergency, the more positive the outcome will be for the injured child. This mode of preparedness will assist in assuring a safe and healthy school environment. SF
Jennifer S. Sherry, RDH, MSEd, is an assistant professor in the School of Allied Health at Southern Illinois University in Carbondale, Ill. She can be contacted at [email protected]. Faith Y. Miller, RDH, MSEd, is an associate professor in the School of Allied Health at Southern Illinois University. She can be contacted at [email protected].
References
Association of State and Territorial Dental Directories (ASTDD). (2010). Best practice approaches for state and community oral health programs. Retrieved December 20, 2010, from http://www.astdd.org/docs/BPASchoolCSHP.pdf
Chipped tooth [image]. Retrieved December 10, 2010, from http://www.webmd.com/oral-health/mouth-problems-slideshow
Krause-Parello CA (2005). Tooth avulsion in the school setting. Journal of School Nursing, 21(5), 279-282.
McIntyre JD, Lee JY, Trope M, Vann WF. (2009). Permanent tooth replantation following avulsion: Using a decision tree to achieve the best outcome. Pediatric Dentistry, 31:2, 137-144(8).
American Academy of Pediatric Dentistry (2009). Reference manual. http://www.aapd.org/media/policies_guidelines/rs_traumaflowsheet.pdf, Retrieved May 24, 2011, from http://www.aapd.org/media/policies.asp
Web Resources
American Academy of Pediatric Dentistry http://www.aapd.org/media/policies.asp
Colgate Oral Health Resource Center http://www.colgate.com/app/CP/US/EN/OC/Information/Articles/Oral-and-Dental-Health-Basics/Common-Concerns/Canker-Sores-Cold-Sores-Infections/article/Oral-First-Aid-at-Home.cvsp
Colorado Department of Public Health and Environment http://www.cdphe.state.co.us/pp/oralhealth/EmergencyDentalFlipChart.pdf
Indiana State Department of Health http://ai.org/isdh/18730.htm
Oral Health Kansas http://www.oralhealthkansas.org/pdf/tipstricks/Tips%20and%20tricks%20-%20Dental%20First%20Aid%20Kit.pdf
Share Care http://www.sharecare.com/question/dental-first-aid-kit
Past RDH Issues