The Immunocompromised Dental Hygiene Practitioner
The Occupational Safety and Health Act of 1970 (OSHA) heralded a new era during which a federal program was designed to protect the national workforce from job-related injury, illness or death. In 1987 these regulations added guidelines for dentistry, and in 1992, the Bloodborne Pathogens Standard went into effect. Today’s clinical practices protect clients and teams by applying OSHA regulations.
The incidence of immunocompromised individuals, including health care workers, is rising, mainly because of increased survival rates for various types of immunosuppressed conditions.1 Examples of some immunocompromised conditions include cancer, organ transplantation, certain chronic diseases and HIV.
By adhering to the ADHA Code of Ethics, dental hygiene practitioners help prevent oral diseases and improve the public’s overall health. But what happens when the oral health professional becomes chronically ill and immunocompromised? What are the various questions employers raise, and what rights do employees have in this situation? How does the immunocompromised hygienist determine if it is safe to return to the workplace?
Immunocompromised hygienists, also referred to as immunosuppressed or immunodeficient, are at increased occupational risk for exposure to certain infections in clinical practice, and are obligated to avoid transmitting infectious agents to their patients. The Centers for Disease Control and Prevention (CDC) distinguishes immunosuppressed people from healthy ones by the existence of immune deficiencies due to immunologic disorders (i.e. human immunodeficiency virus infection or congenital immunodeficiency syndrome), chronic diseases (i.e. diabetes, cancer, emphysema, or cardiac failure), or immunosuppressive therapy (i.e. radiation, cytotoxic chemotherapy, anti-rejection medication, or steroids).2 These individuals have a high risk of infection caused by airborne or waterborne microorganisms, and a subset of people is severely neutropenic for prolonged periods of time (i.e. absolute neutrophil count ≤500 cells/mL). Individuals with neutropenia get infections easily and often. Most of the infections occur in the lungs, mouth, throat, sinuses and skin.
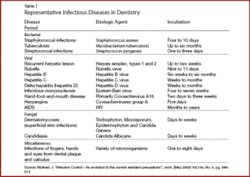
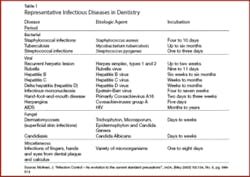
Today’s health care workers, especially dental hygiene practitioners, are routinely exposed to microorganisms and bodily secretions. Evidence reveals that repeated exposure to microorganisms in blood and other secretions results in a higher incidence of certain infectious diseases in health care workers3 (see Table 1). “The potential for health care workers to develop infectious disease after accidental exposure to clients’ blood or bodily secretions has served as the cornerstone for development of infection control precautions during the past 200 years.”3
Untreated dental unit waterlines (DUWLs) have shown to be a source for pathogenic bacteria, fungi, and protozoans. Practicing hygienists who work with equipment that produces aerosols may be exposed to a variety of pathogens, in addition to those generated by untreated dental unit waterlines. “Qualitative and quantitative analysis of the makeup of dental aerosols would be extremely difficult, and the composition of aerosols probably varies with each patient and operative site. However, it is reasonable to suppose that components of saliva, nasopharyngeal secretions, plaque, blood, tooth components and any material used in the dental procedure, such as abrasives for air polishing and air abrasion, all are present in dental aerosols.”4
Because both large and small particles may contain blood elements with viral particles, the ADA recommends large-bore high-volume evacuators with the use of any equipment that produces contaminated aerosols or splatter5 (See Table 2). Although high-speed evacuation has been proven to reduce dental aerosols by more than 90 percent, manipulating a high volume evacuation while using the ultrasonic scaler can be quite difficult. Pre-procedural rinses help reduce airborne patient materials such as blood and saliva, and operator masks offer some protection; however, few practitioners realize that aerosols or droplet nuclei may stay in the air for up to 30 minutes after a procedure.4
The dental hygienist commonly removes his or her mask at the end of a procedure to discuss treatment, give post-operative instructions, and dismiss the client. Since aerosols are still present in the operatory after the mask is removed, the hygienist is exposed to contaminated air. In addition to aerosols produced by ultrasonic scalers, those produced by air polishers contain not only patient materials and water, but sodium bicarbonate. Research reveals that aerosol particles smaller than five micrometers, such as those generated during air polishing, can penetrate the operator’s facemask and be inhaled6 (See Table 3).
What is the “top line” of defense?
The Advisory Committee on Immunization Practices (ACIP) and the Hospital Infection Control Practices Advisory Committee (HICPAC) recommends the following vaccinations for health care workers:
• Influenza
• Hepatitis B
• Measles, mumps and rubella
• Varicella
Most hospitals have a system for tracking the receipt and verification of vaccines and immune status.7 The CDC has vaccination recommendations for health care workers, including immunocompromised hygienists (See Table 4). Individuals who are receiving immunosuppressive therapy may not always obtain the expected immune response from Hepatitis B vaccinations, and sometimes an additional dose of vaccine is required.8 If FluMist is administered as an influenza vaccine, family members should avoid close contact with the immunocompromised person for at least 21 days. Health care workers should refrain from contact with severely immunosuppressed clients for seven days after the vaccine.9
PPE and other environmental issues
What are some precautions that immunocompromised dental hygienists should take to reduce the risk of infection?
■ It is important for hygienists to follow OSHA recommendations concerning use of masks, eyewear and gowns. There are no “super” gloves, masks or gowns that can withstand bombardment by all chemicals and pathogens. The FDA, OSHA and other regulatory agencies regulate many aspects of these products, and share information through newsletters and bulletins from professional associations and manufacturers. It is imperative that both healthy and immunocompromised dental hygienists follow the 2003 CDC Guidelines for Infection Control in Dental Health Care Settings. (http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm)
■ OSAP has published valuable information on the strengths and weaknesses of the various glove materials. (See Table 5) A comparison of latex, nitrile, and vinyl gloves indicates varying reliability. Latex and nitrile gloves have shown a failure rate of 0 percent to 4 percent directly out of the box, and 1 percent to 3 percent after manipulation.10 Although vinyl gloves have a comparable failure rate directly out of the box, the higher failure rate of 12 percent to 16 percent is very risky for even the healthiest users.
■ Hygienists should become familiar with the symptoms and diagnoses of skin reactions associated with frequent hand washing and glove use. Nitrile gloves provide better tear resistance, and have an advantage over natural rubber latex gloves in that hypersensitivity to latex proteins can be avoided.
■ Hand washing is the single most critical procedure available for reducing the risk of transmitting organisms to clients and health care workers.11 Alcohol-based hand disinfectants have superior antimicrobial activity compared to medicated and non-medicated soaps, and are generally better tolerated by clinicians.12 An antimicrobial soap or alcohol hand rub should be used before each surgical procedure.11 The CDC recommends traditional hand washing if hands are visibly soiled.11 Hand lotions that contain petroleum can increase glove permeability and should not be used during the workday. Also, when using lip balm on client’s lips, a non-petroleum lip product should be used because petroleum-based balms may increase glove permeability.
■ Masks, eyewear and lab jackets are effective only if worn properly. Make sure masks fit properly and are changed when they become wet.11 In addition, OSAP recommends masks that fit across the bridge of the nose with a filtration of 95 percent for particles three to five microns. http://www.osap.org/general/redirect.htm?pdf=ICIP-2003-02.pdf.
■ Manufacturers can provide in-depth information about personal protective equipment and will respond to any needs long after the purchase of their equipment.
■ OSHA guarantees every health care worker the right to a safe environment. Immunocompromised dental hygiene practitioners should assess potential workplaces for OSHA compliance before accepting an assignment. Infection control protocol should be discussed during the job interview, and positions should be considered only after the hygienist visits the dental practice. Besides personal protective equipment, hygienists should pay close attention to equipment and surface disinfection, infection control procedures and training, chemical and sharps safety, and dental unit waterline safety issues. Dental units that are directly plumbed to municipal water sources should be retrofitted with a self-contained water system.
■ Infectious tuberculosis (TB) presents a significant risk to the immunocompromised practitioner and has a greater risk of progressing or re-activating once the individual has been exposed or infected. All dental health care workers who have contact with patients should have a baseline tuberculin skin test (TST) at the beginning of employment. Thus, if an unprotected occupational exposure occurs, TST conversions can be distinguished from positive TST results caused by previous exposures.11 Overall, the U.S. has seen a reduction in TB and Multidrug-Resistant TB. In the most recent report from the CDC (2003), 12 states and Washington D.C. reported rates above the national average, and 24 states reported low incidence. However, 19 states reported an increase, and three of those (California, New York, and Texas) accounted for 42.5 percent of the 2003 national total.13
■ Even though airborne pathogen transmission cannot be prevented by compliance with OSHA standard precautions, pre-procedural mouth rinsing by patients with a long-lasting antimicrobial agent like chlorhexidine gluconate or essential oils can reduce the level of oral microorganisms generated during ultrasonic scaling (ADA manual reference). Hygienists should keep masks snugly fit on the face as long as possible after ultrasonic instrumentation. Remember that aerosols can hang around for up to 30 minutes after they are initially generated.
■ In addition to precautions about possible infectious contamination, clinicians and employers should consider the possible pathogenic and carcinogenic potential of the chemicals used in dentistry. All clinicians, especially immunocompromised clinicians, should read the label and heed the warnings from various manufacturers listed on the MSDS sheets in the dental practice.
Discussion
Immunocompromised dental hygiene practitioners are ultimately responsible for monitoring their own health. They should consult a physician to determine whether or not an acute or chronic medical condition might affect job performance. Work restrictions are sometimes made based on the mode of transmission and the length of infection of the disease.
The Americans with Disabilities Act of 1990 was established to protect the rights of people with disabilities. It makes it unlawful to discriminate in employment against qualified individuals with disabilities, and requires most employers to make “reasonable accommodations” to remove obstacles to continued employment.14 As Americans live longer, fuller lives due to improved medical technologies, many hygienists are able to return to work following life threatening and chronic diseases. The legal rights of employees and employers and the health risks of both clients and hygienists must be considered on an individual basis. Even a common infection like shingles may not pose a threat to the immunocompetent hygienist, but may prove deadly to the immunocompromised one. Immunocompromised hygienists must divulge occupational risks to their personal health care providers so the physicians can identify potential risks and recommend precautions.
References
1 Glasmacher A., et al.: Heterotrophic plate counts and drinking water safety, Bartram, A., ed. London, IWA Publishing, 2003.
2 Anderson E., Vaccination and the immunocompromised health care worker - a team approach. Clinical Rounds, Hospital Links, 2004:52(3):97-99.
3 Molinari, J.(May 2003). Infection control - Its evolution to the current standard precautions. JADA, Vol.134, pg. 569-574.
4 Harrel, S.K., Molinari, J. (April 2004). Aerosols and splatter in dentistry. JADA, Vol.135(No.4), pg. 429-437. Retrieved date January 13, 2005, from http://saturn.bids.ac.uk/cgi-bin/ds_deliver/1/u/d/ISIS/15318413.1/ada/jada/2004/00000135.
5 Harrel, S.K., Barnes, J.B., Rivera-Hidalgo. (September 1998). Aerosol and splatter contamination from the operative site during ultrasonic Scaling. JADA, Vol 129, pg. 1241-1249.
6 Muzzin, K.B.; king T.B.; Berry, C.W. (September 1999). Assessing the clinical effectiveness of an aerosol reduction device for the air polisher. JADA, Vol. 130, pg. 1354-1359.
7 Anderson E., Vaccination and the immunocompromised health care worker - a team approach. Clinical Rounds, Hospital Links, 2004:52(3):97-99
8 Flumist. 2004. Online. Internet. Available www.flumist.com
9 Flumist. 2004. Online. Internet. Available www.flumist.com
10 Rego, A.; Roley L. (1996-2005). In-use barrier integrity of gloves: latex and nitrile superior to vinyl. Retrieved March 2, 2005, from http://www.latexallergyresources.org/ResourceManual/section8/in_use_barrier.cfm.
11 CDC Guidelines 19 December 2003. Guidelines for Infection Control in Dental Health-Care SettingsOnline. Internet. Available http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm
12J.C. Lucet, M.P. Rigaud and F. Mentre et al., Hand contamination before and after different hand hygiene techniques: a randomized clinical trial, J Hosp Infect 50 (2002), pp. 276-280.
13 CDC, Executive Commentary. Tuberculosis in the United States. Retrieved date March 1, 2004, from http://www.cdc.gov/nchstp/tb/surv/surv2003/PDF/ExecCommentary.pdf.
14 National Kidney Foundation. Employer’s Guide. 13 May 2004. Online. Internet. Available http://www.kidney.org/atoz/atozItem.cfm?id=58.