The 'C' tattoo
The C-word appears on skin too, and hygienist recounts her experience with skin cancer
BY Vicki L. Munday, RDH
What do you think of when you hear the "C" word? Is it breast cancer, oral cancer, or one of the many other types of cancer that people are diagnosed with every day?
My personal story is one of skin cancer on the top of my head. I had a small, dry scalp area that I had picked at for a few years, thinking it was nothing more than a patch of dry skin. During a routine physical I mentioned an area on my left forearm that concerned me because the freckle was odd looking. I was referred to a dermatologist, who performed a full body scan and told me the freckle was nothing to worry about, but that I had several areas of actinic keratosis, which is a common type of sun damage.
----------------------------------------------
Additional reading
- Surgeon General's Call to Action to Prevent Skin Cancer
- Seriously, how meticulously do you check for oral cancer?
- Skin cancer leaves mark on athletes
----------------------------------------------
I asked about the dry skin on my face, thinking it was part of menopause, and I was informed it was precancerous and needed to be frozen off with liquid nitrogen. I asked about the dry spot in my hair and was told the same thing. So I had three areas frozen with liquid nitrogen. They turned red, and it felt like the skin was boiling about two layers deep. This was the day before the WSDHA Symposium in April, where I had a booth for OralID, and I was introducing Eric Statler, an oral cancer survivor and dear friend.
I was told to return to the dermatologist in four weeks if all three areas did not disappear. The spot on the top of my head did not go away, so I underwent a punch biopsy, which coincidentally was done the day before the PNDC meeting, where I was a sales rep for both PDT and OralID. My results came back squamous cell carcinoma. I was referred to a surgeon who does MOHS surgery - Gail de Imus, MD, FAAD, FACMS, at the Everett Clinic. I had a consultation and scheduled surgery for June 30.
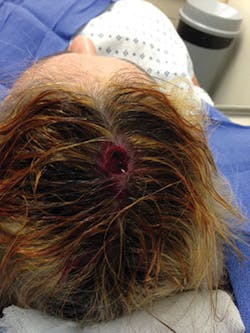
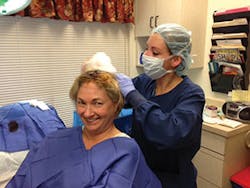
I checked in at 7:30 a.m. and got home by 4 p.m. The procedure was done in an office surgery suite with local anesthesia. The surgeon cut, a biopsy was done, and she cut and repeated the process until clean margins were achieved. She had told me to be prepared to spend the day. I had my Kindle, phone, magazines, and water bottles with me. I asked them to take photos during the procedure so I could share them on Facebook and educate others. Doctor de Imus takes photos for her patients, so it was no big deal to take additional ones on my phone.
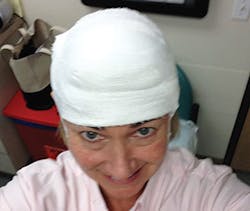
The final hole in my head measured 12 mm by 15 mm, and looked to be 4 mm deep. After I was sutured up, they dry washed my hair to get most of the blood out, wrapped my head in gauze, and then taped it down. I looked like I was wearing a turban with white sideburns made of wide tape. I added my "Floss Chick" baseball hat to complete the look and headed to the pharmacy. They handed me one prescription, and the other had to be emailed to the pharmacy. Forty minutes later I had one prescription in hand and was informed they would text me when the other one was ready. So much for going home and taking a pain med and relaxing.
I went home and posted the photos on Facebook and waited for a text from the pharmacy. About an hour later I went back and picked up my antibiotics. Back home again, I took some Tylenol and tried to relax. I was told to sleep sitting up for several days. Two pillows under my head and a pain pill, and I went to bed. Day two my face was swollen and my body felt very tired. I was scheduled to work two days that week and had to cancel.
One week later I was still tired, but I went off to work wearing a scrub hat to protect my head from all the lovely bacteria that floats around in a dental office. At my 10-day postop check, my doctor was not thrilled with the healing, and opted to leave the sutures in place. Three weeks postsurgery, I was put back on antibiotics and told to stop putting antibiotic ointment on my scalp in order to let it dry out and scab over. Now, a little over one month postsurgery, I just got the sutures removed.
According to my dermatologist, whom I will see again in six weeks, my future will include chemical peel-type treatments on my scalp and some blue light therapy. I have several seborrheic keratoses, which are a common benign growth that need to be monitored. These growths are generally genetic, and I have my father to thank for them. They are more common with age and/or a rapid change in estrogen levels, such as pregnancy or stopping estrogen therapy. For me they are age-related. The most common places for them to appear are on the scalp, face, neck, and upper chest. Melanoma, which can be deadly, and seborrheic keratoses look very similar. Both can grow rapidly, darken, bleed, and itch, so I will be monitoring them closely. Knowing what to look for is important (see "Abnormal Mole").
I have been sharing my journey through skin cancer with patients, who look at me funny when I appear in the operatory with a scrub hat on. So not only am I doing an oral cancer screening, but I'm doing my best to encourage people to apply sunscreen and practice safe sun exposure. As a health-care provider, I believe it's important to educate and share experiences with patients. This makes it more real when it's personal.
I had a conversation with a gentleman I used to date, and he shared photos of his skin cancer surgery on the back of his head. It was basal cell but huge. He had to see a plastic surgeon to close up his surgery site.
Living in the western half of Washington State, where it often rains or the days are gray, is no excuse for not being proactive with sun protection. If you ever see me with a tan, it will be from a bottle from this point forward.
Abnormal Mole A is for asymmetrical: One half of the mole does not match the other. B is for border: The mole has an irregular, ragged, or blurred edge. C is for color: The mole is varied from one area to another, has shades of tan, brown, D is for diameter: The mole is wider than a quarter inch or small but growing. E is for evolving: The mole is changing in terms of size, shape, shades of color, or |
I encourage everyone to have a full-body skin scan once a year with a dermatologist, not just your regular medical doctor. There is a huge difference! Just like when doing a screening for oral abnormalities, visual is only so good, but adding fluorescence technology gives us the edge for early detection and treatment. As with all cancers, early detection and treatment save lives! RDH
VICKI L. MUNDAY, RDH, is a 1992 graduate of Shoreline Community College. She is currently president of LVS2SMILE Dental Hygiene Services, where she represents several dental products under her business license. She is the founder of Smiles for Veterans, which provided $13,000 in free dental care to homeless and low-income veterans in November 2014. She is a 2014 recipient of the Sunstar/RDH Award of Distinction.