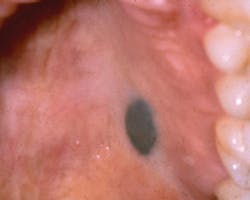
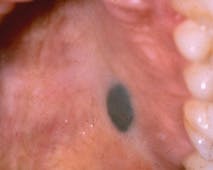
The Blue Nevus or Malignant Melanoma?
by NANCY W. BURKHART, BSDH, EdD
Pigmented oral lesions occur periodically in patients, and the origin must be identified. Additionally, the malignancy potential must be assessed and a treatment plan developed. The source of a pigmented lesion may be from a foreign body such as imbedded metal (for example, amalgam, graphite injury, or a gunshot wound), long-standing chronic irritation, physiological disease states (Addison's disease, for example), hormonal fluctuation, and the use of medications or from an acquired benign or malignant entity.
The color of the pigmented area will vary depending upon the location and the depth of the lesion within the tissues. Those found deeper within the tissue such as the blue nevus appear black to dark blue because of what is termed the Tyndall effect. Melanin particles deep within the tissue cause light to be reflected and to be passed through the overlying tissues. The long and short wavelengths of a pigmented lesion promote the color that is seen clinically. Therefore, some pigmented lesions appear very dark, while others will vary in the intensity of their color. This is true for the blue nevus.
Etiology--The blue nevus is a benign, melanocytic lesion that is often referred to as the pigmented nevus, melanocytic nevus, or nevomelanocytic nevus of acquired origin. Nevi, in general, may be either congenital or developmental. The most common intraoral type of nevus is the intramucosal nevus followed by the blue nevus. The blue nevus is usually asymptomatic, considered benign, with color variations of gray, brown, slate-blue, and blue-black in color and rarely measures over 6 mm.
In the early stages, the blue lesion may have characteristics similar to the deadly melanoma. The nevus, in general, is often seen on external skin surfaces, but they are uncommon in intraoral tissue. The blue nevus is found in the palate in two-thirds of cases followed by the buccal mucosa. Several types or variants of the blue nevus such as the plaque-type blue nevus (Fistarol and Itin, 2005) and the epithelioid blue nevus (Pinto et al., 2003) versions have been documented in the literature.
Blue nevi are usually classified as either "common" that occur most often orally or they may be "cellular" types. Although the blue nevus is considered benign, these pigmentations have the potential to become malignant in some cases. However, there is controversy regarding this theory and most often malignancy occurs in the above mentioned "cellular" types. Diagnosis and confirmation are usually the main reasons for removal. Malignant melanoma has been reported to arise with the cellular blue nevi. In addition, there is always the possibility that what is seen clinically is a malignant melanoma and not a blue nevus.
Pathologists are able to determine the diagnosis and the type of blue nevus during histology evaluation. Confirming the tissue histology and diagnosis is important in the follow-up period after removal of the lesion. This is especially crucial when malignant cells are present.
Method of transmission: The nevus is not transmitted from one person to another in either external skin or intraoral forms.
Epidemiology--The intramucosal nevi are the most commonly occurring nevi in the mouth followed by the second most common type of nevus, the blue nevus. The blue nevus accounts for 19% to 36% of all oral nevi or approximately one third of those occurring in the oral tissues. The literature on the subject indicates that the intraoral nevus occurs in all age groups, but typically in the third to fifth decade of life (Santos et al., 2011). The intramucosal nevus is usually found on the buccal mucosa. A recent case study by Lai et al. (2012) reported a blue nevus in the pharyngeal mucosal area of a 58-year-old woman. This is another reason for careful inspection of the postpharyngeal area of the mouth.
Pathogenesis--The nevus in general occurs from nevus cells in the epithelium, the basement membrane, connective tissue, or in combination of these sites. Depending upon the location in tissue layers, several classifications of a nevus are possible: the intramucosal type, the blue nevi, compound nevi, or junctional nevi. The nevus originates from the proliferation of melanocytes. Within the classification of the blue nevus, several types are recognized and diagnosed by the pathologist: Common (most frequently occurring); cellular form; and combined nevus suggesting several forms.
Common forms of the blue nevus are benign and rarely recur intraorally. Cellular forms may behave aggressively and may recur. The cellular form is the most likely to become malignant.
Perioral and intraoral characteristics: The blue nevus is usually well circumscribed and slightly raised. The blue-back color of the lesion makes its appearance very noticeable when viewed in the palate. When found on the buccal mucosa, the possibility of an amalgam tattoo is more probable and must be considered. In this case, radiographs will often confirm the presence of amalgam fragments and negate a biopsy in most instances.
Extraoral characteristics: Blue nevi occur on the skin of the hands, feet, and buttocks. Generally, all types of nevi occur externally on skin surfaces and are rarely found in oral tissue.
Distinguishing characteristics: The location is a key factor when found in the palate region. The smooth, circumscribed, slate blue color is also a consideration. Microscopically, the blue nevus is readily diagnosed and classified with key characteristics. In all cases, a microscopic evaluation is needed to confirm a suspicion of a blue nevus and to rule out frank malignancy.
Significant microscopic characteristics: Tissue specimens exhibit proliferation of oval-shaped and spindle-shaped melanocytes with dendritic extensions that are heavily pigmented. The cells are seen deep within the lamina propria and parallel to the surface epithelium.
Dental implications--When a blue nevus is suspected, the clinician would remove the lesion because of the rare possibility of malignant transformation or confusion with the deadly melanoma. The lesion is always recorded, documented in a three-dimensional format such as 5x3x1mm. Intraoral images provide additional documentation for the lesion before removal.
Why is a definitive diagnosis needed? Several other lesions should be considered along with the blue nevus. Confusion may occur with satellite metastases from malignant melanoma; therefore, a correct a diagnosis is crucial. Several conditions would be considered with this lesion and histological confirmation is needed. The two more serious considerations are malignant melanoma and Kaposi sarcoma, although in most cases, a thorough health history would place Kaposi sarcoma lower on the list in a differential diagnosis. Diascopy (using a glass slide with applied pressure) is beneficial to rule out vascular type lesions such as the hemangioma.
- Amalgam tattoos
- Hemangioma
- Blue nevus
- Melanoma
- Kaposi's sarcoma
Treatment and prognosis -- Surgical removal with histological evaluation is always performed with these lesions because of the difficulty in clinical identification and the potential for malignancy. Santos (2011) suggests that the palate is susceptible to chemical and physical risk factors that promote carcinogenesis. This may be even more of a risk factor for patients who use tobacco and alcohol.
Since the blue nevus is usually small, it is easy to remove completely during a biopsy, but larger lesions may be more extensive. A dental professional may be the first and often the only person to recognize a blue, pigmented area in the mouth. Our light sources and loupes with magnification give us a supreme advantage in detecting even small lesions. Swift and accurate diagnosis is extremely important for the long-term health of the patient. RDH
As always: Keep asking good questions and always listen to your patients!
References
Pinto A, Raghavendra S, Lee R, DeRossi S, Alawi F. Epithelioid blue nevus of the oral mucosa: A rare histologic variant.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2003;96:429-36.
Delong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist 2nd Ed. Lippincott, Williams & Wilkins, Baltimore. 2012.
Fistarol SK, Itin PH. Plaque-type blue nevus of the oral cavity. Dermatology 2005;211:224-233.
Ojha J, Akers JL, Akers JO, Ashraf M, Hassanein AM, Nadim M, Islam NM, Cohen DM, Bhattacharyya I. Intraoral cellular blue nevus: Report of a unique histopathologic entity and review of the literature. Cutis 2007;80:3;189-192.
Santos T de S, Frota R, Martins-Filho PR, Cavalcante JR, Raimundo Rde C, Andrades ES. Extensive intraoral blue nevus – case report. An Bras Dermatol. 2011; 86 (4supl 1):S61-5.
Fistarol SK, Itin PH. Plaque-Type Blue Nevus of the Oral Cavity. Dermatology 2005;211:224-233.
Lai WS, Hsu CH, Lee JC, Chu YH. Extensive blue nevus of the pharynx. Indian J Dermatol Venereol Leprol [serial online] 2012 [cited 2013 Mar 1];78:376-7. Available from: http://www.ijdvl.com/text.asp?2012/78/3/376/95467
Figure 1: Courtesy of Dr. Michael Kahn from: Delong L. & Burkhart NW. General and Oral Pathology for the Dental Hygienist 2nd Ed. Lippincott, Williams & Wilkins, Baltimore. 2012.
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com.
Past RDH Issues