The glowing dental hygienist
Fluorescence is moving diagnosis forward at warp speed
by Shirley Gutkowski, RDH, BSDH, FACE
There's no dentistry like no dentistry. The dentist and dental hygienist members of the World Congress of Minimally Invasive Dentistry share that vision. While it may make some dentists cringe, it's the battle cry of most dental hygienists. Professionals focused on prevention find it difficult to sit back and acquiesce to enamel breakdown. Their goal is to have patients without any type of filling or prosthesis. It is possible to reach that goal.
Using proper language is one of the keys to practicing preventively. Referring to fillings as prostheses or to decay as necrotic enamel is a start. Far into the future people may no longer need health-care providers to remove necrotic enamel and replace it with a totally inferior man-made product to approximate the dimensions set forth by nature. Similarly, we no longer have patients lined up to have limbs amputated because of ill-managed diabetes. Really think about what dentistry has become. Patients don't even visit their dentists for a soft tissue lesion, which leaves oral cancer diagnostics to physicians who don't have the effective screening tools that dentists have.
How can dental hygienists, as the practice prevention specialists, deliver preventive care that is cost effective for the practice and the patient? The fitness industry boasted sales of $19 billion in 2008 to prevent obesity and many other diseases. Does anyone know how much is spent on dental hygiene from the practice side?
The tools dentists and dental hygienists have available to them to detect and prevent disease are increasing dramatically. It's gotten so where there are now two or three items in each detection and prevention category, and about five years ago there was only one. In some cases the category didn't even exist. Saliva monitoring comes to mind as a good example. For a long time Ivoclar had one of the only saliva testing systems around. A person provided a sample of saliva, and the sample was incubated to grow out the identified cariogenic pathogens.
That was the saliva testing standard for decades. Dentists and dental hygienists had no time in their days to actually do lab tests for a disease they could treat with their eyes closed. After all, the only treatment was a filling. The prevention mindset seemed to be about three things: adding more fluoride, teaching the modified Bass technique, and finger wagging about flossing. The thought of managing the causative agents was simple - "brush and floss them outta there."
Some dentists and dental hygienists knew that pH was a big factor in caries management, not just plaque management. They incorporated litmus paper into their regimen, doing it simply and educationally chairside.
Saliva testing became more simplified with the GC America Check Buffer. The system incorporates the buffering test and a test for the pH, differentiating between stimulated and unstimulated saliva. There is no overnight testing. The dental market initially resisted, but eventually came around. Other companies have brought similar products, such as the CariFree ATP reader, to market, and now there is more to choose from, all in the last decade.
We can test saliva chairside for cario/perio pathogens, and even the presence of human papillomavirus (HPV). Perio and HPV are still lab tests; the saliva must be sent out and the results are returned later. And we can use fluorescence to instantly detect cariogenic pathogens, as well as lesions in the enamel.
Fluorescence is the science of light interacting with biological and inert materials. Once a certain wavelength light hits a biological material, it does one of two things - reflects/refracts, or stimulates the biological material to glow.
Reflection is when the light bounces back. It's like the episode of "The Big Bang Theory" where the Uber Geeks pulse a laser at debris left on the moon by one of the lunar landing teams, and measure the time it takes for the light to return to their little rooftop machine. Reflection can measure distance and proof of lunar landing.
Refraction is the change in direction of a wave of light passing through a medium. Surgeons who provide LASIK surgery must take into consideration the effects the vitreous humor in the eye has on the laser when doing the procedure. Another example of refraction is when oral health-care providers use transillumination to look for decay or fractures in teeth. Light will travel down the healthy enamel rods and, to the human eye, the light will look normal and straight. If the enamel is broken down, the light will not look normal, and the eye will see a dark area where the light is refracted.
Fluorescence
Fluorescence is a light signal. Organic compounds, which are carbon-containing, fluoresce when illuminated by a specific wavelength. Molecules of organic material absorb the smallest possible bits of light, called photons, at one wavelength of color and become excited and jump around. The organic molecules change shape as they store the energy of the photons. Using this stored energy, the molecules emit new photons in different colors. That's the fluorescent glow.
American doctors and scientists began investigating the uses of fluorescence in medicine in the 1920s. By the 1940s they found that drugs like Atabrine, an antimalarial drug, fluoresced at certain ultraviolet wavelengths.
Around the 1950s, the technique gave rise to many new uses for fluorescence in medical research. NIH's Dr. Robert Bowman developed a sensitive instrument called the spectrophotofluorometer (SPF), which allowed scientists to use fluorescence as a way to identify and measure tiny amounts of substances in the body. Fluorescence is used today in AIDS research and the Human Genome Project.
Fluorescence microscopes use sensitive electronic cameras to observe a three-dimensional view of how cells function. Lasers are a focused type of light used in selective excitation of fluorescence in many tiny regions inside living cells. This technology also has the ability to detect events lasting less than a trillionth of a second in proteins. (For more in-depth information about the history of fluorescence, visit http://history.nih.gov/exhibits/bowman/intro.html.)
In dentistry we use a wavelength of light to cause biomasses, mucosa, and enamel to glow. More accurately, the material being illuminated absorbs some colors and not others. Knowing which colors will be visible to the human eye gives the clinician an idea of what is happening on the tooth. One of the early uses of fluorescence technology in dentistry is still in use today, the DIAGNOdent. The focused light causes the bacterial byproducts on the tooth to glow. That glow is quantified by the little machine and a reliable, repeatable number is displayed. ViziLite and VELscope also use fluorescence to detect changes in the soft tissue.
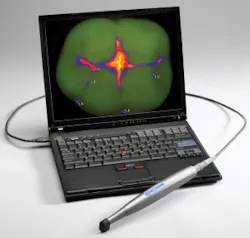
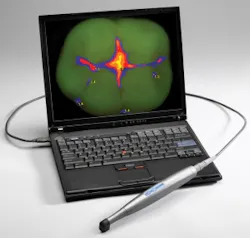
Last year, fluorescent technology was kicked into warp speed by a handheld, intraoral, cameralike device called Spectra. Not only does the software give precision information about the bacteria on the tooth, it also gives density readings so the reparative clinician can better know how much damage the tooth has sustained by the cariogenic bacteria.
Using the broad light footprint, the clinician can capture the whole tooth and replicate the capture time after time. This is achieved by an ingenious disposable hood that focuses the light, gathers the light, and allows the clinician to have the same light-to-tooth measurement every time. Although light cannot penetrate prostheses, it can give the clinician measurements of health around the margins of prostheses such as amalgams, crowns, and bridges. The color is read by the handpiece and displayed on the screen like a Doppler radar reading. The biomass is visually displayed in one of two colors regardless of where it is on the tooth. Cariogenic bacteria are represented by the color red. Noncariogenic bacteria are green.
For the restorative dental hygienist, this science is true movement forward. There is finally a way to detect whether a pit or fissure is ready for a sealant. A quick Doppler photo of the tooth can reveal cariogenic bacteria that may remain after the first attempt to remove it with a prophy brush. We all know what happens if a tooth is ill prepared for a traditional resin sealant - sealant bomb. Decay under the resin material can progress to where the tooth may need root canal therapy.
Air polishing has long been recommended as the first cleaning step in preparing a tooth for sealant application. Using the Spectra and fluorescence, a clinician can detect the cariogenic mass in the fissure, clean it with an air polishing medium such as sodium bicarbonate, calcium carbonate, or NovaMin, and see the results in real time. The clinician can then either proceed with the etching step, or re-treat with the air polish or microsurgery with air abrasion or fissurotomy bur before etching and placing the appropriate sealant material.
Current research has identified nearly 800 different bacteria that live in the mouth. Each has a reason to be there - to break down the tooth, keep other bacteria in check, or manifest as breath only a mutt could love. Some bacteria need to be cultivated, some need to be removed, and I recently heard a speaker mention that bacteria should be domesticated. We have a LOT of work to do!
We could culture all of our patients' oral bacteria. But we know that biofilm brings a new wrinkle to how bacteria live in a society. Which is not to say that culturing is not helpful/beneficial. We can make good sound clinical decisions by knowing what lives in the biofilm; researchers are developing hooks to hang our collective hat on when we talk about dealing with this or that biofilm; and fluorescence technology can help us do that more and more.
The days of dental hygienists flying blind are over. We used to enter into the periodontal space and root around with an explorer, probe, or curette to remove the biological waste, hard deposits, and food debris. On the crown of the tooth, oral health-care providers assumed anything on the surface of the tooth was cariogenic or periogenic. The disappearance of stain, a cosmetic concern, was the endpoint of any procedure on the crown of the tooth.
We now have many more options for using our sight to accurately do our job than ever before. Together, accurately focused lights attached to our foreheads, high vac suction, magnification loupes, and fluorescence make it easier to tell the difference between good and bad plaque, and make the oral health-care provider more effective. And we don't need to be Uber Geeks to practice that way.
Shirley Gutkowski, RDH, BSDH, FACE, is the technology coach at CareerFusion (www.careerfusion.net), and author and publisher of The Purple Guide series of books for dental hygienists' career development, www.rdhpurpleguide.com. She can be reached at [email protected].