The Saga Begins
by Karen Kaiser, RDH
A long time ago, in a hygiene operatory far, far away ... Turmoil has engulfed the sulcular arena and the inflammatory process is well underway. This diabolical quest to take control of the periodontal pocket has left the fearless, yet outnumbered, Jedi whites to retreat.
Hoping to resolve the matter with a blockade of antibacterial warfare and therapeutic approaches, the gingival galaxy finds the deadly anaerobes present a resistant stronghold and become a veritable force of chronic concern. The greedy pathogenic biofilms have produced a matrix and proliferated in the region. While the gingival congress debates the matter, the immune system secretly guards the pocket peace, still unsure which coalition the lymphokines will choose. To settle the conflict and bring justice to the unhealthy pocket, a new force is called upon to vaporize the assiduous pathogenic bacteria and secure the zone.
Enter the diode soft-tissue laser.
Inflammatory episode
The periodontal pocket is filled with bacterial invaders. Ineffective protocols to reduce and remove these pathogenic bacteria (irritant plaque) within the soft tissues prompt an inflammatory response of epic proportions. Initially, an increase in the leukocyte fleet will be observed in the sulcus, connective tissues and adjoining epithelium galaxies. There will be a flood of crevicular fluid mediators within the sulcus, transporting enzymes (collagenase, hyaluronidase, lysozyme and cytokines). Left unchecked, these enzymes will infiltrate the connective tissues — the origin of gingival inflammation.
Biofilms form on the farthest reaches of living tissues. During the initial hostile takeover, removal of the factors allowing the progression of the inflammatory response must be removed to stop the progress before it becomes further established. To halt the distress of the lesion, non-calcified plaque masses and mineralized deposits that have formed on the hard side of the pocket must be resolved. Once the inflammatory process is full blast, clinical manifestations will be seen in the permeated tissues. When tender, irritated tissues are disturbed, they begin to bleed. In time, the collagen fibers will be destroyed in the infiltrated area.
Tissues under attack
As the alien bacterial activity commences, ulceration and consequent thinning of the epithelium will follow. As the action unfolds, proliferation of capillaries result in tissue redness or even a blue appearance from sluggish blood flow in the area. This color change first appears in the papilla, then spreads to the gingival margin, creeping onward to the attached gingiva. The threat looms as inflammation from the gingival tissues to the supporting periodontal tissues penetrate and destroy fiber attachment and raze cortical plate bone. With the destruction of connective tissue attachment and bone, the formation of a periodontal pocket will ensue. Left unchecked, the junctional epithelium (coronal portion) detaches from the root surface and consequently causes periodontal attachment loss. Healthy gingival connective tissues provide a strong defense against the inflammatory response. Concentrated collagen fiber tissues, in optimal condition, can "slow the flow" of destructive fluids in the tissues.
With all the bacterial factors considered, a soft-tissue laser can deliver a means to combat and disturb the inflammatory process by ablating the pigmented pathogenic biofilm. The soft-tissue laser was shown in studies to effectively maintain reduction of P. gingivalis and P. intermedia, two bacteria considered to be the most harmful periodontal pathogens, for 90 days following the laser use. Using a laser can effectively reduce and inhibit the decolonization of bacteria, preserving the attachment tissues and improving the clinical indices. (Neill ME, Mellonig JT. Prac Perio Aesth Dent 1997) Disturbing and reducing the destructive assembly of bacteria by using a laser can rescue the tissues from disease formation by weakening the bacteria's aptitude to cause disease.
Mission log
Perhaps some may find using a laser to be intimidating and close to rocket science. However, hygienists who routinely use a soft-tissue laser find it to be an essential component in the treatment of periodontal disease. Moreover, following a strict safety protocol with procedural parameters greatly enhances treatment success. Utilizing a soft-tissue laser in dental hygiene is very rewarding — especially when you consider the benefit provided to the patient — periodontal pocket biofilm reduction. Attending approved proficiency courses provides necessary laser fundamentals and hands-on training to achieve a level of comfort with laser dynamics.
Laser therapy is performed in conjunction with initial therapy, root planing and scaling. The mineralized deposit layers are laden with bacterial endotoxin that must first be removed on the hard side of the pocket. The subgingival hard surface must be devoid of calculus by means of mechanical (manual/ultrasonic) instrumentation. Calculus can be a haven for pathogenic biofilm to rapidly multiply.
Preparing to initialize
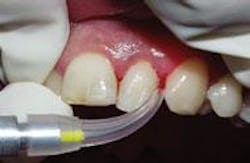
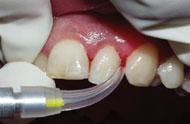
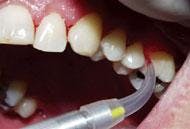
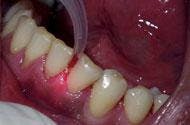
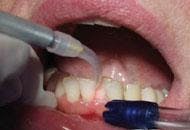
There is a relatively short learning curve with the laser. The diameter of the laser fiber is similar to a periodontal probe. The clinician uses a hand-held wand with an optic fiber in the sulcus. When employing the laser, the fiber traces the sulcular area and remains in full contact with the diseased tissues. The fiber is maneuvered inside the sulcus with the same sweeping, crosshatching motions hygienists use with curettes ... with the important exception of avoiding the root surface. The laser operator moves the wand rapidly and with purpose on the tissues in an erasure-like fashion, erasing the destructive bacteria. With experience, this motion becomes decisive and technique-driven to remove diseased tissue.
For the beginning clinician, keep in mind that discomfort can be triggered by improper technique. Allowing the laser fiber to remain stationary or move too slowly through the sulcus causes heating of the tissues and generates undesirable and unintended collateral tissue damage. This creates patient sensitivity. Ensuring that the laser wand is kept moving while in contact with tissue will alleviate this dilemma.
For relief after the laser procedure, apply Gelclair, a bioadherent gel, available through Butler/G.U.M., to the newly lased tissue. This gel provides soothing relief to the oral tissues with a pleasant taste that patients appreciate. The gel has gentle protective enzymes and launches pain right into orbit.
A soft-tissue laser accomplishes this deadly blow to the pathogenic bacteria through pigment-seeking energy. Light energy is changed into heat and absorbed by the target tissue. The laser interacts with tissue in different ways. Diode laser interaction is energies absorbed by hemoglobin and melanin.
Ablation of the target tissues, or vaporization of the diseased tissue, best occurs when the energy emitted from the laser is absorbed and converted to heat. Adequately absorbed laser energy optimizes the ablation effect. Hygiene applications for this focused energy are utilized during gingival curettage or bacterial reduction measures. Ablation is desirable to vaporize the necrotic tissue found in the diseased periodontal pocket. The laser energy eliminates the diseased tissue via the fiber. When the fiber is initiated by touching it to articulating paper, a photothermal effect is optimized. The colonized rods and spirochete bacteria don't stand a chance against a photo-initiated fiber. In addition, the more soft tissue components found at the treatment site, the better for this vaporizing process to occur.
Exploring a distant horizon
With conventional instrument curettage on the soft side of the pocket, the reverse cutting surface of the curette provides the harsh removal of tissue without the benefits of hemorrhage control. In contrast, laser fiber curettage removes the epithelial lining to achieve vaporization of pathogenic bioburden, thus changing the pocket environment. When using the lasing procedure for sulcular debridement, pathogenic debris and necrotic tissue will accumulate on the tip. Accumulating bioburden must be wiped from the laser tip to ensure the fiber has maximum focused energies and has not become damaging to adjacent tissues.
Using a laser seals off capillaries, minimizing procedural bleeding. When therapists perform scaling and root planing and then utilize an adjunct like a soft-tissue laser, they have the added assurance that the treated pocket is nearly sterile when the patient is dismissed. Also, it is comforting to know that you are not sending them out of the operatory bleeding.
May the force be with you
Bacterial reduction is all about lessening the bacterial population in the sulcus. Bacterial reduction is a procedure using an uninitiated fiber tip, not necessarily to remove tissue from the pocket, but to disinfect the pocket with increased light energy after root planing and gingival curettage procedures. Diode lasers emitting a continuous wave for 15 seconds per site at between 600 and 800 mWs will achieve this reduction.
One study of bacterial reduction using a diode laser (Moritz A et al., Lasers Surg Med 1999) selected two patient groups with periodontal disease. The first group received only scaling and root planing. The second group received scaling and root planing on the initial visit, and laser therapy (bacterial reduction) on the second visit. The study concluded that the laser group demonstrated a significant lessening of bacterial population.
The purpose of any soft tissue therapy program is to stabilize the tissue and promote periodontal health. Using low level laser therapy as a component of hygiene services, biofilm can be minimized and diseased sulcular epithelium can be easily removed.
When the call to arms requires more influence than the Jedi whites can muster, launch your treatment success by using fiberoptic laser energy to achieve the desired clinical outcome. Lasers are the wave of the future — make it a mission to integrate a soft-tissue laser into your dental hygiene practice.