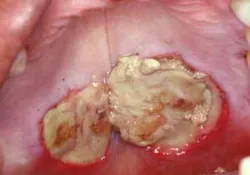
Necrotizing sialometaplasia
by Nancy W. Burkhart, RDH, EdD
[email protected]
Morris is seeking treatment for an ulcerlike lesion in his palate. Morris is 29 years old, and uses alcohol and tobacco on a daily basis. He reports no significant health history, but uses antacids daily, and his diet is extremely poor. Morris is unemployed and tells you that he feels stressed most of the time since he is behind in all of his obligations.
He inquires about an area in the palate (see Figure 1). The lesion is of great concern to him because he has noticed that the size has continued to increase over the past month. Morris does report an injury with a pen to the palate a few weeks ago. He tells you that he was walking with the pen in his mouth and lost his balance. He does report that he was consuming alcoholic beverages at the time. The dentist suggests referring Morris to an oral surgeon for a biopsy. The biopsy report indicated that the lesion was necrotizing sialometaplasia.
Necrotizing sialometaplasia. From DeLong L and Burkhart NW. General and Oral Pathology for the Dental Hygienist. Lippincott Williams and Wilkins. 2008.
- Etiology: The cause of necrotizing sialometaplasia is not known, but it is usually preceded by trauma. It is locally destructive, with inflammation to an area of tissue resulting in damage and ischemic necrosis. This may occur not only in the salivary glands but also in sinus/nasal tracts and the respiratory tract.
The salivary gland tissue is damaged, resulting in a disrupted blood flow to the tissue, which causes ischemia. The affected tissue infection is not contagious, usually localized to one specific area of the mouth and is self-limiting. The trauma causes that have been implicated have been dental injections, tissue trauma such as the example presented in this case study, previous surgery, and ill-fitting dentures, causing trauma or irritation.
- Epidemiology: Men are reported to develop necrotizing sialometaplasia more often than women by a 2:1 ratio. The palatal salivary glands are involved in 75% of cases, and the submandibular and sublingual glands are rarely involved (but there are reported cases that do involve these areas). The initial lesion may present as a tissue swelling and within several weeks develop into the crater-like lesion presented in the case study.
- Pathogenesis: The initial cause is unknown, but necrotizing sialometaplasia is due to restriction of blood supply or damage to the salivary tissue. The lesion usually occurs at the juncture of the hard and soft palate. Because of the damaged appearance of the tissue, the patient may be extremely anxious after noticing this lesion. Tooth brushing of the lesion may produce exudate or bleeding, adding to the frightening appearance.
These lesions are not malignant, but the presence of more serious disease states must be ruled out.
- Perioral and intraoral characteristics: Necrotizing sialometaplasia may occur in stages. Initially, the lesion may present as either a unilateral or bilateral swelling with tender or dull sensations and subsequently progress to the ulcerative appearance presented in the case study. Ultimately, the lesion can appear quite large and ulcerated, with well-demarcated margins. The center core appears ulcerative with a raised appearance in some areas and depression in other areas of the lesion. The lesion has a thick yellow to gray fibrinous covering that is very characteristic of the entity.
- Differential diagnosis: Necrotizing sialometaplasia may resemble several other entities and may be difficult to diagnose depending upon the appearance of the specific lesion both clinically and microscopically. Other considerations may be syphilitic gummas, mucoepidermoid carcinoma, deep fungal infections, and squamous cell carcinoma.
All of these considerations may exhibit a similar clinical appearance. Additionally, in poorly controlled diabetes and medically compromised patients, a similar appearance may occur due to fungal infections and mucormycosis.
- Significant microscopic features: The salivary gland tissue appears necrotic, exhibiting an inflammatory appearance, necrosis of the acini structures, and metaplasia of the ductal epithelium. The lesion may mimic salivary gland neoplasms and, specifically, malignant entities such as mucoepidermoid carcinoma and squamous cell carcinoma. Differentiation both clinically and microscopically is needed to confirm a diagnosis.
Misdiagnosis may occur in specific instances, resulting in radical and unnecessary surgery with adjunct treatments such as radiation therapy. A diagnosis confirmation by two pathologists is suggested since correct diagnosis is extremely important. An opposing diagnosis may occur as well in that a diagnosis of mucoepidermoid carcinoma and squamous cell carcinoma may be rendered when the lesion is actually necrotizing sialometaphasia.
- Treatment and prognosis: Analgesics may be needed, as well as elimination of alcohol and tobacco when usage is noted. There is no surgical intervention, but a biopsy with microscopic evaluation is needed to rule out other more serious disease states so that early intervention may be taken.
The lesion usually heals after several weeks without any treatment. In some cases, though, the tissue may take months to fully respond. A bland baking soda and water mixture is often suggested along with analgesics. Diet counseling and nutritional evaluation is crucial as well.
References
Cawson RA, Binnie WH, Eveson JW. Oral Disease — clinical and pathologic correlations. Wolfe Publishing 1994.
DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. Lippincott, Williams & Wilkins. Baltimore, 2008.
Eisen, D, Lynch DP. The Mouth. Mosby, St. Louis. 1998.
Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. W.B. Saunders Co. Philadelphia. 1995.
Regezi JA, Sciubba JJ, Jordan RCK. Oral Pathology: Clinical Pathologic Correlations. Saunders, St. Louis. 2003.
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and co-host of the International Oral Lichen Planus Support Group http://www.bcd.tamhsc.edu/outreach/lichen/ and coauthor of General and Oral Pathology for the Dental Hygienist. Her Web site for seminars is www.nancywburkhart.com.