Bulimia
by Nancy W. Burkhart, RDH, EdD
My case study is a little different in format from my usual column. I have just attended the fifth annual "Nutrition and Health Program." The program was sponsored by the University of Arizona Integrative Medicine Program, and health-care providers from around the world were in attendance.
After attending this conference, I have a renewed sense of value as a health-care provider and an enhanced sense of the importance in the early detection of oral and systemic disease. The program was hosted in Phoenix, and the most well-known physician, Dr. Andrew Weil, was the course director for the program. I have been a fan of Dr. Weil for a long time and hold to his concepts in my personal life regarding total health. His approach is rather simple in many ways and focuses on healthy eating, successful aging, exercising, minimizing toxic exposure and utilizing stress reduction.
One statement that I heard more than once was, "If your grandmother cannot recognize the food or additive you are about to place in your mouth, you probably should not be eating it." Another was, "If you would not place the product in your mouth, do not use it on your skin."
Courtesy of Dr. Ronald Brown, Howard University
That is good advice for anyone! As I write this monthly column and as I coauthored our recent "General and Oral Pathology for the Dental Hygienist" textbook, I have often thought about how many diseases may have been caused by environmental factors, genetic components, overtaxed immune systems, or possibly inadequate nutrition at crucial times throughout life.
As I listened to many physicians asking questions during the conference, I thought how powerful we really are in dentistry. We have so much valuable time to talk to patients about general health issues. As licensed professionals, we have the power to disseminate great amounts of information to our patients — due to the fact that we have more time than any other health-care professionals! We can provide some key health information on many factors related to total health. Additionally, many patients return for multiple visits during the year. This fact is also unique in how it sets us apart from other health-care providers. And, do not forget that we do have a captive audience!
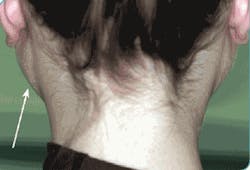
Courtesy of Dr. Doron Aframian, Hadassah, The Hebrew University
While listening at the conference, I tried to establish ways that I could add my new information to some of the seminars that I present to dental groups throughout the United States, as well as to my monthly Oral Exams column on oral case studies.
Courtesy of Dr. Doron Aframian, Hadassah, The Hebrew University
To make it even more interesting, I was at the Academy of Oral Medicine meeting in Scottsdale, AZ, the following week. Again, I listened to a lot of information relating to health. My ears perked up when I heard the editor of JADA, Dr. Michael Glick (a faculty member at A.T. Still University; as an associate dean in the medial school, he is responsible for creating an oral health care curriculum for medical students.), strongly comment that we should be providing general health information to our patients, helping them maintain optimal health.
This was one of the few times I had heard these comments expressed by someone in dentistry. I thought, "Did he attend the seminar I attended two weeks ago in Phoenix?" As an educator, this was all I needed to hear to send me on a mission.
The seminar in Arizona with Dr. Weil was one that is, of course, nutritionally focused for total health. My column today is not really about food; it is on eating disorders — specifically, bulimia nervosa. It is an important health-related issue for those of us in the dental community. The two most common types of eating disorders are anorexia nervosa and bulimia nervosa. This column will address bulimia nervosa with subsequent columns on other eating disorders. Although a nutritional component is part of all the eating disorders, the subject involves a much deeper problem involving relationships with food, body image, and control. The issue is far more reaching than the space allotted in my column and is usually a lifelong struggle for an individual.
Since we can recognize the signs of an eating disorder such as bulimia nervosa due to the devastation in the oral tissues, the dental community may be the one health-care provider who is in a perfect position to assist these patients in getting the early treatment that is crucial. Many signs of oral disease are also apparent externally in the case of the patient with anorexia nervosa.
Sometimes we forget to assess the total patient and to observe with all of our senses. It is reported that the earlier the eating disorder is discovered and treatment is rendered, the better the chance of a total recovery.
Epidemiology: Bulimia affects approximately 12 individuals per 100,000 population. The number is an estimated one since many individuals may practice bulimic behavior and never seek treatment. Some reports estimate that 1 percent of females are affected and 0.1 percent of males are affected by bulimia, and many who treat these patients suggest that the numbers are increasing.
Etiology: Although no one etiology exists for eating disorders, there are three main thoughts regarding the etiology:
- Brain disturbance with biochemical variations such as those associated with serotonin levels.
- Psychological problems such as compulsive disorders, mood disorders, poor coping skills, and unique personality profiles making the person more susceptible.
- Cultural pressures to appear thin and "perfect," and most of these individuals began dieting at an early age.
It is thought that the individual who is susceptible to an eating disorder may be pushed into the practice by cultural pressures such as the media, peer influences, and social problems. Others may be susceptible as well, but may be fortunate in having a strong support system and a high sense of who they are with high self-esteem.
Clinical aspects of bulimia: Unlike the patient who restricts food intake, the true bulimia patient eats a high quantity of food and then purges the stomach's contents in an attempt to restrict weight gain and also to control the behavior. Most bulimic patients appear extroverted and very normal in appearance. In contrast to patients who suffer with anorexia nervosa, patients with bulimia may be concerned about their appearance and usually will seek dental care — this is true until obvious signs of the disorder begin to surface.
As with all patients who have eating disorders, there is always the concern of being discovered. However, at the same time, there is a risk-taking aspect to their personality, and they may actually find the possibility of discovery invigorating.
The patient who practices bulimia may use laxatives, syrup of ipecac, enemas, diuretics, and excessive exercise in order to maintain a lower weight. The patient eats and then purges — sometimes multiple times a day — and may eat large quantities of food in a day. The finger or an object such as a toothbrush are usually inserted down the throat to induce vomiting. After a period of time, the finger may actually develop a callus that is called Russell's sign. After many episodes of purging, the individual is able to vomit by just contracting the stomach muscles. Because of the trauma of induced vomiting, the soft palate often becomes ulcerated, with obvious tears and broken capillaries.
Diagnosis: Bulimia is diagnosed after three months of the binge/purge behavior, but the oral signs often take years to develop. Additional diagnostic findings can be clinical signs of oral damage such as enamel loss, esophageal tears, hematomas, increased caries rate, loss of gag reflex, xerostomia, dentin sensitivity, salivary gland enlargement, and erosion. A new finding recently reported is the restriction of insulin in an attempt to reduce weight in women who are Type 1 diabetic. This is very serious and they are placing themselves at increased mortality.
In early bulimia, the teeth have a "sand blast" type of appearance with loss of mamelons and definition of the enamel. As the erosion progresses, the lingual of the anteriors begin to show dentin, leaving a fine ring of enamel on the edge of the lingual surfaces (see Figure 1). The dental practitioner will need to assume the role of investigator in trying to determine the cause of the erosion or any oral tissue damage. Working through the possibilities of erosion with the patient allows a differential diagnosis to be made (Burkhart et al., 2005). As changes occur in the salivary glands due to electrolyte imbalance and general metabolic changes, the sensitive acini structures of the salivary glands become enlarged (see Figure 2). This is due to what is termed sialosis and the acini contain larger and more numerous zymogen granules.
Careful palpation and visual inspection is important during the extraoral exam to determine this enlargement of the glands. As the enamel destruction progresses, amalgam islands begin to be apparent because the amalgam does not diminish, but the enamel around the restoration does dissolve (see Figure 3).
Treatment and prognosis: The subtle signs of eating disorders are often overlooked or ignored by both dentists and hygienists. Additionally, loss of tooth structure in disordered eating patterns is difficult to differentiate from erosion due to acidic types of food, oral habits, and environmental factors. Table 1 provides suggestions on preventing further damage to the oral tissues. It is important to assess the individual situation and get assistance through a team approach for the patient with disordered eating practices. This will involve the dental team, a mental health counselor trained in disordered eating practices, a nutritionist, and a physician. Approaching the patient is often difficult and clinical protocol has been suggested regarding dialogue (Burkhart et al., 2005). Each professional must assess his or her own style and each patient is different with regard to personality and social factors. Early intervention and referral is crucial for the long-term health of the patient.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry and Texas A & M Health Science Center in Dallas. Nancy is also a cohost of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is the coauthor of General and Oral Pathology for the Dental Hygienist, published by Lippincott Williams & Wilkins in Baltimore, which was released in October 2007. She can be contacted at [email protected].
References:
Burkhart N, Roberts M, Alexander M, Dodds A. Communicating effectively with patients suspected of having bulimia nervosa. JADA 136: August, 2005.
DeBate RD, Tedesco LA, Kerschbaum WE. Knowledge of Oral and Physical Manifestations of Anorexia and Bulimia Nervosa Among Dentists and Dental Hygienists. J Dent Educ 2005;69:346-54.
DeLong L, Burkhart NW. General and Oral Pathology for The Dental Hygienist. Lippincott, Williams & Wilkins. Baltimore, 2007.
Goebel-Fabbri AE, Fikkan J, Franko DL, Pearson K, Anderson BJ, Weinger K. Insulin restriction and associated morbidity and mortality in women with Type 1 Diabetes. Diabetes Care 31:415-419, 2008.
Hoek HW, Hoeken DV. Review of the prevalence and incidence of eating disorders. Int J Eat Disord 2003;34:383-96.
Web sites:
Mirasol Recovery Center
Tucson, AZ.
www.mirasol.net
National Eating Disorders Association
603 Stewart St. Suite 803, Seattle WA 98101
Business office (206) 382-3587
Referral Hotline 800-931-2237
[email protected]
Table 1
The following suggestions will limit or reduce the loss of enamel when obvious tooth destruction is recognized:
• The dentist can provide the patient with custom-made trays and 1.1 percent neutral fluoride gel. The patient should use the trays for five minutes daily; a good time is while taking a shower.
• After vomiting, the patient should rinse with 1 teaspoon baking soda mixed with 8 ounces of water to neutralize the acid. If baking soda is not available, simply rinsing with water is beneficial.
• Suggesting an over-the-counter 0.05% fluoride rinse is helpful in diminishing enamel loss.
• The patient should not brush the teeth for at least an hour after vomiting. The enamel becomes soft due to stomach acid.
• Using a tongue cleaner to remove acid from the papillae is crucial. The residue lies in the papillae and constantly bathes the lingual areas of the teeth. Encouraging the patient to drink water throughout the day will lessen the acidity in the mouth. Additionally, drinking any acidic beverage through a straw will keep the acid confined to the posterior part of the mouth.
• The importance of healthy foods should be stressed such as eating a low-sugar diet, and adding more foods such as cheese, vegetables, and sugarless gum (those that contain xylitol).
• Limiting nonabrasive dental products for maintenance appointments is important and the use of enamel promoting dentifrices is optimal.
•Intraoral photography will assist the practitioner in future comparison of damage or tissue repair.
Modified from Burkhart, et al. JADA 136:August, 2005, pg 135-136