A Physical Approach To TMD
A Physical Approach To TMD
by Cathy Hester Seckman, RDH
When a patient complains of a popping, clicking joint or a persistent morning headache, a simple posture test can show him or her how correct posture influences the jaw joint.
Try this experiment. Sit on the edge of a chair and slump over. Now round your shoulders like a person with really bad posture. Open your mouth, and note how far it opens.
Now sit up very straight, with your pelvis tucked and centered, your sternum facing forward, and your head and shoulders upright and neutral. Open your mouth again. Notice that it opens wider? What does this exercise tell you? It points out very nicely that posture and temporo-mandibular joint function are related.
We use our jaw almost continuously for eating, talking, and expressing emotion, not to mention yawning and sneezing. When we overuse it by clenching and/or grinding our teeth, the result is temporomandibular disorder.
TMD is the name given to a group of symptoms that cause pain and dysfunction in the head, face, and jaw. Symptoms can include orofacial pain, restricted jaw function, clicking or stiffness in the joints, headaches, limited jaw opening, tinnitus, or ear, neck, and shoulder pain. Pain may be worse in the morning, and it may be cyclical.
TMD is the result of pressure on the facial nerves due to muscle tension, injury, or bone abnormalities. Sex and age are reliable indicators of TMD. Seventy percent of adults report at least one symptom of TMD, and most are women between the ages of 20 and 50. No one knows exactly why women have TMD more than men, but some medical experts suggest high estrogen levels may play a part. Stress may also be a factor, as women in this age group tend to lead high-stress lives.
We all know the standard treatment for TMD — soft diet, moist heat, over-the-counter anti-inflammatory medication, no chewing gum, and let's make an appointment to check the occlusion.If none of these help, nearly all dentists have a favorite type of mouth guard or splint they can recommend.
Surgery is another accepted treatment for TMD, but few patients need to, or are willing to, go to such drastic measures to treat a popping, clicking joint that sometimes hurts and sometimes doesn't. There are other, less well-known treatments for TMD. Believe it or not, one of these treatments is botox. Dentists at the Institute for Head and Neck Therapy in Pickering, Ontario, report a 90 percent success rate in TMD patients after injecting purified Botulism toxin. Injections are made at specific points in facial, head and neck muscles. The institute claims the injections improve pain, function, mouth opening, tenderness to palpation, and bite force.
The practice of yoga, along with a program of stress reduction that might include biofeedback or meditation, helps some people relieve TMD symptoms. Experts recommend yoga asans (exercises) that emphasize proper posture and alignment to take strain away from the jaw and allow it to rest.
Physical therapy is a treatment that is gaining ground and has seen considerable success. A study in Austria in 2002 determined that 76 percent of TMD patients who had been treated with exercise and physical therapy three years earlier were symptom-free and needed no further treatment. Insurance carriers cover physical therapy prescribed by a physician or dentist for TMD, but precise wording of the diagnosis is necessary.
George Summers, MPT, of East Liverpool, Ohio, has been working with local dentists to treat TMD sufferers. "I saw a need for some option that would complement treatment of symptoms," Summers says. "We work on the causes of TMD, identifying those causes and correcting them. The first thing I look at is posture. Typically, a person with TMD is a woman who has lost control of her core — the lower abdominal and gluteus muscles — which sometimes goes back to pregnancy. But even young kids can have poor balance and core strength."
When core muscles do not properly support the body, the pelvis can tilt, leading to increased lumbar lordosis (improper forward spinal curvature in the small of the back). When the pelvis tilts abnormally, the rest of the body tries to compensate. The shoulders may move back, the thorax may bend forward, and the head may rise to allow better vision.
It's easy to see that with parts of your body tilted hither and yon in ways nature never intended; your poor TMJ gets the worst of it. "When the shoulders are rounded forward," Summers says, "that really puts stress on the temporo-mandibular joint. The entire area gets congested."To correct the problem, Summers begins at the core.
"Treatment is individualized for each patient, and we take a whole-body approach. We may start at the hips, the ribs, or the thoracic outlet, and work up. It all depends on the needs of that particular patient."
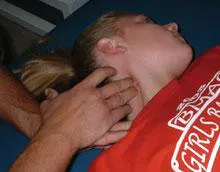
He said that typical TMD therapy begins with releases of soft tissue. "We do myofascial releases of the back, pelvis, lumbar, and thoracic muscles, as well as the muscles inside and outside the mouth. We manipulate each muscle from origin to insertion, eventually allowing them to slide over each other as they were meant to do."
Summers may also use iontophoresis, a form of electrical stimulation that propels a prescribed medication, such as a steroid, into an affected area. "It's like getting a shot without a needle," he says.
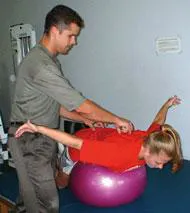
Summers' goal is to re-educate the patient's brain and muscles into proper postural position. After the releases, stretching is the next step, to provide full range of movement for the newly-freed muscles. Strength training, which encourages the muscles to maintain proper position, follows.
Summers also guides patients through each level of core strength testing. "Once they're able to do a Level 1 exercise correctly for a certain number of repetitions, we move to Level 2. There are seven levels altogether."
He typically sees 80 percent improvement in TMD symptoms after a course of therapy.
The American Academy of Orofacial Pain recommends physical therapy as an "effective and conservative treatment" for TMD. The next time a patient complains of a popping, clicking joint or a persistent morning headache, the simple posture test at the beginning of this article can show them how correct posture influences the jaw joint. Because treatment is so individualized, Summers was reluctant to recommend one exercise for everyone to improve TMJ function.
But he did say this: "Raise your sternum. Make sure it's facing forward at all times. Feel the muscles in the middle of your back. They should be tight, holding you upright."
Cathy Hester Seckman, RDH, is a frequent contributor who is based in Calcutta, Ohio.