Overweight Evidence
Will dental professionals need to calculate BMI impact on perio risks?
BYStacy McCauley, RDH, MS
When dental hygienists think of risk factors related to periodontal disease, several likely come to mind: poor oral hygiene, genetic predisposition, smoking, and diabetes ... just to name a few. A new area of periodontal risk research that is gaining tremendous momentum relates to obesity. As this research evidence continues to mount, dental professionals will be compelled to consider not only how patients' body mass index (BMI) influences their overall health, but also how BMI influences patients' periodontal disease risk.
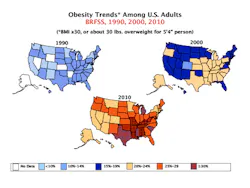
Based on national statistics, adult obesity rates have more than doubled, from 15% in 1980 to 35% in 2010.1,2 And, if we include both overweight and obese BMI classifications in those estimates, that number jumps to approximately 68% of the U.S. adult population.3 In 2013, revised guidelines related to BMI classifications were published by a consensus report from the American Heart Association, the American College of Cardiology, and The Obesity Society. Based on these new classifications, the determination of obesity is as follows: A BMI classification of 25 to <30 = overweight, BMI scores of 30 to <35 = Class I obese, scores of 35 to <40 = Class II obese, and a BMI score > 40 is now considered Class III obese or extreme obesity. To calculate your own BMI, visit nhlbi.nih.gov/health/educational/lose_wt/BMI/bmicalc.htm.
Figure 1
Without question, the "obesity epidemic" has yielded devastating consequences. The impact has been felt not only on the health and wellness of Americans, but also on the health and wellness of the U.S. economy. The current statistics from the Centers for Disease Control and Prevention (CDC) estimate the medical cost of obesity in the United States at $147 billion annually.4 Each year, the Robert Wood Johnson Foundation and the Trust for America's Health publish How Obesity Threatens America's Future to examine strategies for addressing the obesity crisis. In their most current analysis, the estimates for Americans' health over the next 20 years is grim if current obesity rates continue on their current trajectory.5 They predict that:
• Obesity rates for adults could reach or exceed 44% in every state and exceed 60% in 13 states
• The number of new cases of type 2 diabetes, coronary heart disease, stroke, hypertension, and arthritis could increase 10 times between 2010 and 2020 and then double again by 2030
• Obesity-related health-care costs could increase by more than 10% in 43 states and by more than 20% in nine states.
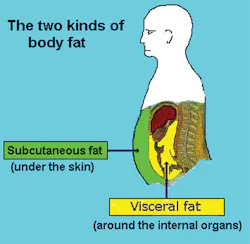
The CDC statistics are shocking. As dental professionals, we see this every day in our own practices. Without question, the patient population has become increasingly overweight. And, these overweight and obese patients continue to get sicker and sicker, presenting with diabetes, hypertension, and heart disease just to name a few. As we think about obesity and its role in overall health, it is important to distinguish between excess visceral fat and excess subcutaneous fat. Subcutaneous fat is found just underneath your skin, the "pinch an inch" kind of fat, commonly found on hips and thighs. Visceral fat or "hidden belly fat" is found around the internal organs, deep within the torso, wrapping itself around the heart, liver, and other major organs. Individuals with apple-shaped physiques tend to have more visceral fat. Although carrying any type of excess body fat is generally considered unhealthy, understanding why visceral fat is more detrimental to your health is important.
------------------------------------
Additional reading
- Low pH, soft drinks, decay, and obesity
- The benefits of xylitol for your dental patients are numerous
- Dental hygienists can make a difference in people's heart health
------------------------------------
Visceral fat has been linked to a long list of adverse health conditions, including:
• High blood pressure
• Stroke
• Heart disease
• High cholesterol
• Diabetes
• Breast cancer
• Dementia
• Periodontal disease
One of the main reasons visceral fat is of concern is the role it plays in inflammation, a physiologic process tied to many common chronic diseases, including periodontal disease. When visceral fat increases, the individual's omentum (fat layer covering abdominal organs) grows rapidly. As the omentum grows, it begins to act as an endocrine organ, secreting inflammatory cytokines into the bloodstream. These cytokines and interleukin-6 are known to be risk factors for heart disease as well as periodontal disease infection.7 They also have a harmful effect on blood pressure and the blood's clotting ability. High amounts of visceral fat in the body lead to increased LDL or "bad cholesterol" and a decrease in HDL or "good cholesterol." It also results in insulin resistance whereby blood glucose levels rise. This can lead to diabetes. Individuals with excess visceral fat (omentum/belly fat) are constantly bombarded with these ever-increasing levels of inflammatory cytokines, putting them into a state of cumulative, chronic inflammatory burden. It is thought that these inflammatory cytokines and the subsequent cumulative inflammatory burden may directly injure the periodontal tissues and/or reduce blood flow to the periodontium, thus promoting the development of gum disease. Figure 2 differentiates between visceral fat and subcutaneous fat.
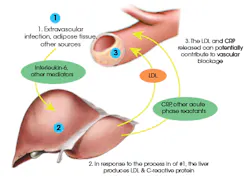
In Figure 3, the interplay of periodontal disease-associated cumulative inflammatory burden (chronic inflammation) and obesity-associated inflammatory burden are detailed. Both conditions are widely recognized as sources of low-grade inflammation in the body. As depicted in the illustration, the liver produces higher levels of LDL (bad cholesterol) and C-reactive protein (CRP) in response to stimuli from obesity (primarily visceral fat) as well as periodontal disease infection (extravascular infection). CRP is a known risk factor associated with cardiovascular disease,8 diabetes,9 hypertension,10 cancer,11 inflammatory bowel disease, Crohn's disease,12 obstructive sleep apnea,13 and periodontal disease,14 just to name a few. The liver's chronic production of CRP in response to obesity and/or periodontal disease not only puts stress on the body's vital organs, but also likely puts the individual at risk for other comorbid conditions. When we fully understand the physiological response to obesity and periodontal disease infection, it makes sense why we see so many chronically sick patients in our practices. Essentially obese/overweight individuals' bodies are being subjected to inflammatory warfare 24 hours a day, 7 days a week, 365 days a year.
What does the current science tell us about the relationship between obesity and periodontal disease? Does the science support the hypothesis that obesity is a risk factor for periodontal disease? Hein and Batista state, "From a biological standpoint it seems indisputable that obesity impacts processes that involve inflammation, including but not being restricted to periodontitis."15
According to the American Academy of Periodontology (AAP), periodontal disease is caused by bacteria and a susceptible host. The risk factors classifying a patient as being a susceptible host are:16
1. Age - Studies indicate that older people have the highest rates of periodontal disease. Data from the CDC indicates that more than 70% of Americans 65 and older have periodontal disease.
2. Smoking/tobacco use - Studies have shown that tobacco use may be one of the most significant risk factors in the development and progression of periodontal disease.
3. Genetics - Research indicates that some people may be genetically susceptible to periodontal disease. Even with good oral hygiene habits, these individuals are more likely to develop periodontal disease and manifest a more aggressive form of the infection. Identifying these individuals with genetic testing before they even show signs of the disease and getting them enrolled in periodontal therapy early may help them keep their teeth for a lifetime.
4. Stress - Research has revealed that stress is linked to many serious health conditions such as hypertension, cancer, and numerous other health problems. Stress is also a risk for periodontal disease. Studies demonstrate that stress can make it more difficult for the body to fight off infection, including periodontal diseases.
5. Medications - Some drugs, such as oral contraceptives, antidepressants, and certain heart medication can affect oral health.
6. Clenching/Grinding - Excess force on the supporting tissues of the teeth could speed up the rate at which periodontal tissues are destroyed.
7. Other systemic diseases - Certain systemic conditions may worsen the condition of gum disease such as diabetes, cardiovascular disease, and rheumatoid arthritis.
8. Poor nutrition and obesity - A diet low in important nutrients can compromise the body's immune system and make it harder for the body to fight off infection. Because periodontal disease begins as an infection, poor nutrition can worsen the condition of the periodontium. In addition, research has shown that obesity may increase the risk of periodontal disease due to the inflammatory burden that it causes in the body.
When one considers the myriad of obesity-related illnesses, many of which have high mortality rates, the need for immediate action to stop this crisis from reaching a point of no return is now. According to the CDC, obesity-related illnesses include, but are not limited to:6 • Coronary heart disease • Type 2 diabetes • Cancers (endometrial, breast, and colon) • Hypertension • Dyslipidemia (for example, high total cholesterol or high levels of triglycerides) • Stroke • Liver and gallbladder disease • Sleep apnea and respiratory problems • Osteoarthritis • Gynecological problems (abnormal menses, infertility) |
While not all periodontal disease risk factors are modifiable, being able to identify those that are can help dental professionals better customize their patient education and create more individualized treatment plans. Recently, the Philips CARE (Customized Assessment and Risk Evaluator) tool was introduced as a free online risk assessment patient education resource (philipsoralhealthcare.com/care). In a comprehensive periodontal risk assessment, dental hygienists would include the following: findings from the periodontal evaluation (pocket depths, bleeding on probing, radiographic bone loss), estimate of the patient's obesity risk, and the calculated risk determination from CARE.
It has been suggested that obesity is second only to smoking as the strongest risk factor for inflammatory periodontal tissue destruction.17 In an interesting study in the Journal of Clinical Periodontology, researchers evaluated more than 1,000 individuals to determine if there was a relationship between waist circumference (WC), body mass index (BMI), and other indicators of obesity, and the development of periodontal disease. They concluded that the greater the BMI, waist circumference, and visceral fat area (VFA), the greater the number of sextants with periodontal disease.18 A 2014 study published in the Archives of Oral Biology looked at the influence of an atherogenic cholesterol-rich diet on periodontal disease in female Wistar adult rats. The rats were assigned to either a control group or an experimental group where they were fed a diet high in cholesterol, saturated fat, and calories. Two weeks into the study, the researchers placed ligatures around the left first molar to induce experimental periodontitis. The alveolar bone loss of experimental periodontitis was magnified by the ingestion of an atherogenic diet high in saturated fats and cholesterol.19 Another interesting consideration related to obesity and periodontal disease risk is whether obese patients are less likely to respond favorably to periodontal therapy.
In a recent study published in the August 2014 issue of Journal of Periodontology, researchers assessed two groups of chronic periodontitis patients. Twenty-four nonobese chronic periodontitis patients were enrolled into the control group, and 24 obese chronic periodontitis patients were enrolled into the experimental group. Both groups were evaluated at three months and six months post-SRP. Although both groups showed improvements in clinical indices (probing depth and BOP), the nonobese patients demonstrated the greatest reduction of probing depth.
A multipronged approach to supporting obese periodontal patients provides the best chance at addressing inflammation from both a systemic level as well as a local level. Smoking, stress, and lack of sleep certainly influence how burdened the immune system is. In all patients, but especially in overweight and obese individuals, nutrition plays a critical role in the inflammatory burden. Implementing nutritional counseling during the dental hygiene appointment is key to obesity prevention as well as obesity treatment strategies. To help reduce systemic inflammatory burden, hygienists can provide patients with recommendations related to pro-inflammatory and anti-inflammatory food choices.
Across the board, we all should be avoiding pro-inflammatory foods (highly processed, low quality packaged foods). These have been shown to spike inflammation while suppressing our immune system. For overweight and obese periodontal patients, this becomes even more important. Just treating their localized inflammation through SRP alone may not be as successful if their body is being burdened by a pro-inflammatory diet. A low-inflammatory diet rich in antioxidants, Omega 3's and Omega 6's, helps support the immune system, providing systemic support for healing. Brightly colored fresh fruits and vegetables (kale, red peppers, strawberries, blueberries, etc.) are loaded with antioxidants. Antioxidant-rich fruits and vegetables also help to suppress inflammation. Foods rich in Omega-6's and Omega-3's such as wild-caught salmon, shrimp, walnuts, and chia seeds are just a few examples of foods that can help support the immune system while suppressing systemic inflammation.20,21
There are several excellent online resources available to further educate ourselves and our patients about anti-inflammatory food choices.
• drweil.com
• arthritistoday.org
• integrativemedicine.arizona.edu
Along with the dietary strategies to control systemic inflammation detailed above, one must also address localized inflammation through oral hygiene products. Power toothbrush technology is an excellent first-line recommendation to include when diagnosing and treatment planning periodontal therapy (SRP) and periodontal maintenance in obese and overweight individuals. This is especially important for extremely obese individuals, as dexterity becomes an increasing problem. When dexterity is impacted, flossing can be difficult. A mechanized interdental cleaning device, such as Sonicare AirFloss, is an excellent adjunctive aid to assist with biofilm disruption in individuals with dexterity issues. Finally, one might also consider recommending a chemotherapeutic oral rinse designed to control inflammation for our patients with obesity-related periodontal risk factors.
In order to reverse this frightening obesity trend, being mindful of obesity prevention before it becomes a whole-body crisis is the best strategy. As dental hygiene moves into the next 100 years, it is likely that obesity's role in our patients' health will continue to become more evident.
As a known risk factor for serious oral health and overall health diseases, the obesity conversation must stay top of mind as we provide dental hygiene services to our patients. At the core of this topic is the startling fact that once obesity and periodontal disease have commenced, their systemic effects are serious and vast. In many cases, the comorbid conditions manifested from obesity and/or periodontal disease leave consequences that can be permanent and may also contribute to serious outcomes such as loss of teeth, loss of limbs, and loss of life.
With the current obesity and periodontal disease epidemic, the time is now to integrate this information into clinical practice. Think about how you might be able to integrate this information into your current standard of care. How will you include a patient's obesity status in your periodontal risk assessment? How will you advise patients about pro-inflammatory and anti-inflammatory food choices? How will you help support inflammation control for obese patients via home-care products? The potential impact dental hygienists have on improving oral and systemic health for patients is immeasurable. Every patient encounter we have is an opportunity for us to empower someone to improve health for a lifetime. RDH
Stacy McCauley, RDH, MS, is an adjunct assistant professor at UNC Chapel Hill, where she also received her master's degree. Stacy brings over 20 years of dental industry experience including clinician, corporate dental business, and most recently as a coach with Inspired Hygiene, a national consulting firm in Charlotte, N.C. (www.inspiredhygiene.com). Interested in booking Stacy McCauley for your next CE event? Email her at [email protected].
References
1. National Center for Health Statistics. Prevalence of overweight, obesity and extreme obesity among adults.
2. Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of obesity in the United States, 2009-2010. NCHS data brief no 82. Hyattsville, MD: National Center for Health Statistics, 2012.
3. Flegal KM, Carroll MD, Ogden CL, et al. Prevalence and trends in obesity among U.S. adults. Journal of the American Medical Association, 1999-2008;303(3):235-41, 2010.
4. Finkelstein EA, Trogdon JG, Cohen JW, Dietz W. Annual medical spending attributable to obesity: Payer- and service-specific estimates. Health Affairs 2009;28(5):w822-w831.
5. www.healthyamericans.org
6. http://www.cdc.gov/obesity/adult/causes/index.html web data accessed 8/5/14.
7. Khosravi R, Ka K, Huang T, el al. Tumor necrosis factor-alpha and interleukin -6: potential inter-organ inflammatory mediators contributing to destructive periodontal disease in obesity or metabolic syndrome. Mediators Inflamm 2013:2013:728987,.http://dx.doi.org/10.1155/2013/728987.
8. Danesh J, Wheeler JG, Hirschfield GM, Eda S, Eiriksdottir G, Rumley A, Lowe GD, Pepys MB, Gudnason V (April 2004). C-reactive protein and other circulating markers of inflammation in the prediction of coronary heart disease. N. Engl. J. Med. 350(14):1387-1397.
9. Pradhan AD, Manson JE, Rifai N, Buring JE, Ridker PM C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA July 2001;286(3):327-34.
10. Clearfield MB. C-reactive protein: a new risk assessment tool for cardiovascular disease. The Journal of the American Osteopathic Association Sept. 2005;105 (9):409-416.
11. Lu H, Ouyang W, Huang C. Inflammation, a key event in cancer development. Molecular Cancer Research. Apr. 2006;MCR 4(4):221-233.
12. Liu S, Ren J, Xia Q, Wu X, Han G, Ren H, Yan D, Wang G, Gu G, Li J. Preliminary case-control study to evaluate diagnostic values of C-reactive protein and erythrocyte sedimentation rate in differentiating active Crohn's disease from intestinal lymphoma, intestinal tuberculosis and Behcet's syndrome. Am. J. Med. Sci. May 2013;346 (6):467-572.
13. Latina JM, Estes NA, Garlitski AC (2013). The relationship between obstructive sleep apnea and atrial fibrillation: A complex interplay. Pulm Med 2013: 621736.
14. Paraskevas S, Huizinga JD, Loos BG. A systematic review and meta-analyses on C-reactive protein in relation to periodontitis. Journal of Clinical Periodontology 2008;35(4):277-290.
15. Hein C, Batista E. Obesity and cumulative inflammatory burden: A valuable risk assessment parameter in caring for dental patients. Evidence-Based Dental Practice, Supplement. 2014;14(1)17-26.
16. http://www.perio.org/consumer/risk-factors
17. Nishida N, Tanaka M, Hayashi N, Nagata H, Takeshita T, Nakayama K, et al. Determination of smoking and obesity as periodontitis risks using the classification and regression tree method. J Periodontol. 2005;76:923-928.
18. Han D, Lim S, Sun B, et al. Visceral fat area-defined obesity and periodontitis among Koreans. J Clin Periodontol. Feb. 2010;37(2):172-179.
19. Macri E, Lifshitz F, Ramos C, et al. Atherogenic cholesterol-rich diet and periodontal disease. Arch Oral Biol. Jul. 2014;59(7):679-686.
20. Kagalwalla AF, Shah A, Li BU, et al. Identification of specific foods responsible for inflammation in children with eosinophilic esophagitis successfully treated with empiric elimination diet. J Pediatr Gastroenterol Nutr 2011;53:145-149.
21. Adamo AM. Nutritional factors and aging in demyelinating diseases. Genes Nutr 2014:9:360.