Macroglossia and the disease implications
It has often been said that “The eyes are the window to the soul.” However, practitioners of both Eastern and Western medicine often say, “The tongue is an indicator of health within the whole body.” These two philosophies of medicine share a similar belief that the condition of the tongue will indicate what other issues a patient may be harboring within the body.
The practitioner of Eastern medicine will usually view several areas of the body before going any further in their assessment of a patient. Those areas are the pulse, the tongue, and the nails of the patient. In Western medicine, those areas are assessed as well, but often only if the patient complains of some issue related to those locations and not as an intricate part of an initial assessment. And, of course, sometimes the obvious may be very difficult to miss, such as an enlarged tongue. This column focuses on the importance of tongue enlargement and calls attention to serious entities that may involve tongue enlargement, whether obvious or subtle.
The tongue is vital in speaking, eating, and general well-being. Diseases often manifest symptoms within the tongue in the early stages. The examination of the tongue may lead to many suspect etiologies that will need deeper inspection and analysis. Increased use of oral photography has assisted in this respect since comparison can be made with prior dental visits.
Patients often approach a dental professional when the tongue appears red, white, ulcerated, painful, or generally depicts an unhealthy appearance. The lips and the tongue promote a sense of disease to the patient when there is an abnormal appearance that may be noticed by others. Appearances that suggest poor health diminish self-confidence and contribute to psychological problems for the patient. This is especially true for those in close relationships with others and those who have regular contact with the public, such as individuals who must speak in work-related fields. Some patients report dysphagia and articulation issues, and this alone will bring them to a dental practice for evaluation. When daily activities and personal interaction are affected, the patient will seek answers.
Reamy et al. describe macroglossia as an abnormal enlargement of the tongue compared with the mouth and jaws.1 Down syndrome is an example. Melville et al. describe “true macroglossia which exhibits abnormal histology with clinical findings, and relative macroglossia in which normal histology does not correlate with pathologic enlargement.”2
Amyloidosis is a known association with macroglossia and is caused by systemic amyloidosis that may be secondary to multiple myeloma. Amyloidosis is the buildup of an amorphous protein called amyloid that is found in various tissues. These proteins are in the form of abnormal insoluble fibers called amyloid fibrils that are found in the extracellular space in the tissues of the body. Amyloidosis can occur as an isolated disease termed primary amyloidosis or as a secondary illness termed secondary amyloidosis.
Dawoud and Ariyaratnam report a case study of a 63-year-old female presenting with restricted tongue movement.3 In a recent case presented by Maturana-Ramirez et al., a 73-year-old female was diagnosed with mutation of hydrophilic molecules resulting in water being trapped, producing edema in the tongue.4 Some symptoms of hypothyroidism as described by Melville et al. include cold intolerance and amyloidosis of the tongue also associated with multiple myeloma.2 The authors caution that a full oral exam with soft-tissue palpation is important to the diagnosis of all disease states. The patient presented in this case study was diagnosed with multiple myeloma and amyloidosis.
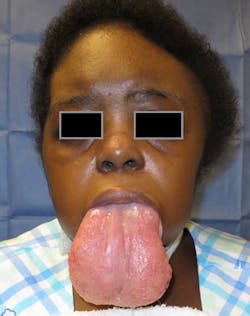
An extreme case of macroglossia was recently published by Melville et al., in which the tongue was enlarged due to acquired myxedema (see etiology above) as the primary etiology.2 Melville describes the myxedema as a decrease in thyroid hormone, sweating, weight gain, fatigue, obstructive sleep apnea, congestive heart failure symptoms, and decreased mental function. The surgeons performed a wedge glossectomy on this patient, producing good results (figures 1 and 2).
Figure 1: Macroglossia due to myxedema (Courtesy of Dr. J. C. Melville)
A substantial number of systemic conditions have been associated with macroglossia. Disease states that may cause macroglossia fall into two categories: acquired or congenital/hereditary. In young children, macroglossia may produce problems with tongue mobility, and in older children, it may result in eating problems and speech dysfunction.5
Neville et al. lists the following congenital and hereditary causes: vascular malformations, lymphangioma, hemangioma, hemihyperplasia, cretinism, Beckwith-Wiedemann syndrome, Down syndrome, Duchenne muscular dystrophy, mucopolysaccharidoses, neurofibromatosis type 1, and multiple endocrine neoplasia type 2B.6
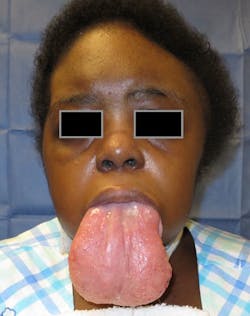
Figure 2: Patient (in figure 1) after a wedge resection of the tongue, preserving the hypoglossal and lingual nerves (Courtesy of Dr. J. C. Melville)
Acquired causes of macroglossia include: edentulism, amyloidosis, myxedema (as depicted in figure 1), acromegaly, angioedema, myasthenia gravis, amyotrophic lateral sclerosis, carcinoma, and other tumors. Because of this wide realm of possible causes, additional testing and observation are usually needed. With each of the entities listed, the tongue may have a smooth appearance or a pebbly, papillary, or fissured appearance.
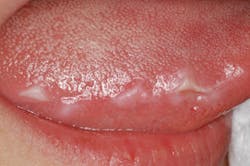
Macroglossia may be a factor in sleep apnea (this is secondary to macroglossia), and more information has been gained in the past few years on the subject. Figure 3 depicts tooth indentations that are the result of a patient who does not have enough space in the resting region of the oral cavity, and the tongue is pressing against the lower anterior teeth. The normal resting position of the tongue is behind the maxillary anterior teeth. As the tongue enlarges, for whatever reason, the indentations become more obvious. Edema, as stated previously, may evolve from various sources, and the enlargement may be sudden or sometimes very subtle. The patient may be the first to notice changes in the tongue related to movement, speech, soreness, or surface changes.
Figure 3: Indentations caused by the tongue resting/pushing against the teeth due to the decrease in space
Palpation, oral cancer exams, and general assessment are needed at each dental visit. The lateral borders of the tongue are a risk area for oral cancer. Examining the tongue with retraction and palpation are crucial in the oral cancer exam. The floor of the mouth and the oropharyngeal areas are high-risk areas, and they require careful examination. Any deviation from normal deserves special consideration, and a cause must be determined.
As always, continue to ask good questions, and always listen to your patients.
References
1. Reamy BV, Derby R, Bunt CW. Common tongue conditions in primary care. Am Fam Physician. 2010;81(5):627-634.
2. Melville JC, Menegotto KD, Woernley TC, Maida BD, Alava I 3rd. Unusual case of a massive macroglossia secondary to myxedema: A case report and literature review. J Oral Maxillofac Surg. 2018;76(1):119-127. doi: 10.1016/j.joms.2017.06.033.
3. Dawoud BES, Ariyaratnam S. Amyloidosis presenting as macroglossia and restricted tongue movement. Dent Update. 2016;43(7):641-642,645-647. doi: 10.12968/denu.2016.43.7.641.
4. Maturana-Ramírez A, Ortega AV, Labbé FC, de Moraes Ê, Aitken-Saavedra JP. Macroglossia, the first manifestation of systemic amyloidosis associated with multiple myeloma: Case report. J Stomatol Oral Maxillofac Surg. 2018. pii: S2468-7855(18)30133-2. doi: 10.1016/j.jormas.2018.06.009.
5. Glick M. Burket’s Oral Medicine. 12th ed. Shelton, CT: People’s Medical Publishing House; 2014.
6. Neville BW, Damm DD, Allen CM, Chi AC. Oral and Maxillofacial Pathology. 4th ed. St. Louis, MO: Elsevier; 2015.
Additional reading
1. DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 3rd ed. Baltimore, MD: Wolters Kluwer; 2018.
2. Burkhart NW. The tongue: A window to other organs. RDH. 2011;31(5). http://www.rdhmag.com/articles/print/volume-31/issue-5/columns/the-tongue-a-window-to-other-organs.html.
NANCY W. BURKHART, EdD, BSDH,
AFAAOM, is an adjunct associate professor in the Department of Periodontics-Stomatology, College of Dentistry, Texas A&M University, Dallas, Texas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/) and coauthor of General and Oral Pathology for the Dental Hygienist, in its third edition. Nancy was awarded an affiliate fellow status in the American Academy of Oral Medicine in 2016. She was awarded the Dental Professional of the Year in 2017 through The International Pemphigus and Pemphigoid Foundation and is a 2017 Sunstar Award of Distinction Recipient. She can be contacted at [email protected].