Synergy and the patient-provider relationship, part 3
Solutions to 5 potential problems hygienists can use to defuse difficult situations
By Ronald E. Goldstein, DDS, and Yemia White, RDH, BSDH
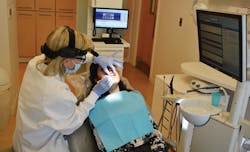
Figure 1: Hygienist Cheri Robinette has placed key intraoral photos of potential problem areas for Dr. Goldstein to review with the patient.
Editor’s note: This is part three of a three-part series. Part one appeared in the November 2017 issue, and part two appeared in the January 2018 issue of RDH.
No doubt dental hygiene is one of the most important and rewarding parts of the dental profession. And yet, like all professions, it is not without its problems. So, in our final article in this series, we will deal with some of the most recognizable problems and potential solutions.
The first and most serious problem can occur when your training or moral compass interferes with your dentist employer. Although dialogue can help in many situations you may well be in a mismatch situation, and may be better off seeking another office to work for. The second problem sometimes occurs with staff, including the dentist’s assistants. These type of situations can usually be worked out, because most often the problem is either jealousy or miscommunication. The basic need in most all these situations is mutual respect for everyone’s important role in the office team.
PROBLEM 1
Hygienist finds caries… dentist does not.
Depending on the dentist’s schedule, sometimes it is better for the doctor to examine a hygiene patient before the start of a restorative procedure. When this happens, the hygienist may not have had time to gather all of the information needed for diagnosis. For example, bitewing x-rays may have been taken but not individual or full mouth X-rays, photos, or DIAGNOdent readings. The hygienist may have just begun treatment and, therefore, has not fully assessed all the areas of potential concern. In some cases, this can result in the hygienist finding a problem area after the doctor has already completed the exam. It is not uncommon for the hygienist to find a carious defect that might or might not show up on the x-ray.
Figure 2: Since this patient was sensitive during her last probing, Gail Heyman, RDH, is using a more comfortable ColorVue probe.
In this scenario, the dentist may have two or three patients being treated, is running behind schedule, and is rushed for time and says, “I will check the area in six months when the patient returns.” Now you are conflicted since you feel the area might get worse in six months, especially since your explorer went in deep around an older restoration.
Solution: Convey the severity of your finding. If this dilemma occurs and the dentist has to return to check an area, explain to the dentist that you found an area that was undetected because it was not apparent on the radiograph but you discovered it after further exploration. Inform the patient that you see an area of concern, and let he or she know the dentist will return for reexamination. Ensure x-rays and multiple intraoral photos are on the monitor for the dentist to see. When the defect is hard to find, this will always help the dentist locate exactly where the lesion is. The dentist can review the information collected, and have the patient reappointed for treatment (see Figure 1).
Conversely, if the area is not an acute concern, the patient has outstanding treatment, and is scheduled for treatment in the next week or two, the area can be rechecked when the patient returns. This is only recommended if the dentist is not at a stopping point with his or her patient, and your patient cannot wait for the dentist to return.
In some instances, if time is limited and the patient works or lives nearby, they are more than willing to return to have the dentist recheck the area at a time that is convenient for them.
Overall, we try to address our patient’s needs during his or her scheduled visit, but on occasion, if we feel it necessary to reevaluate an area of concern, most patients don’t object to this. Our goal is for both of us to work together to protect our patient’s teeth and surrounding structures for a lifetime.
PROBLEM 2
The picky patient
Your “picky” patient is contemplating getting a new smile, but you are concerned your patient may have unrealistic expectations about treatment outcomes. During a recent hygiene appointment, your patient expressed he or she has seen multiple dentists because “none of them knew what they were doing.” You grow more concerned that the patient may eventually have the same “issue” with your office.
Solution: Inform your dentist about the conversation you had with the patient. This will allow the dentist to ask more detailed questions about the patient’s expectations, determine whether or not they are realistic/obtainable, and perhaps gain insight about the patient’s previous dental experiences.
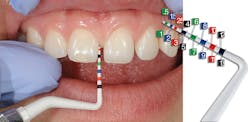
Figure 3: The new Goldstein Colorvue Probe (Hu-Friedy) was judged by 100 patients to be 61% more comfortable than metal probes.
Figure 4: The Colorvue Probe has 0.5 mm increments up to 3 mm and 1 mm increments up to 13 mm for more precise measurements.
If the patient has unrealistic expectations about treatment, and your dentist feels he or she may not be able to meet the patient’s expectations, it is the dentist’s responsibility to convey treatment outcomes as realistically as possible or refer the patient to another practice.
Proceeding with treatment will ultimately be the dentist’s decision but the conversation between the patient and the hygienist gives more insight to this dilemma. In our office, we have had patients referred specifically to transform their smile because of our reputation in esthetic dentistry. In most every case, once we have achieved the desired esthetic results, we send the patient back to the referring office so their hygienist can help maintain the results. However, we do ask the patient to let us check them once annually, if possible.
PROBLEM 3
Declining x-rays
A 35-year old female, patient of record, presents for her six-month recare appointment. She is in good health, has healthy gingiva, and a low caries index. The patient is scheduled to update bitewing radiographs but declines to have them taken citing she doesn’t want to be exposed to the radiation.
Solution: Don’t take it personally. A rejection, especially if it pertains to a professional recommendation, may be somewhat disconcerting, but most times it is not because the patient does not value your recommendation.
Inquire why the patient declined the x-rays. More than likely it will be based on something the patient has read in the newspaper, magazine, or even on the internet. The fact is there have been so many articles warning consumers of the dangers of radiation that unrealistic fears can and do arise. It is a good idea to have copies of scientific articles, and even the ADA’s stand on x-rays readily available. According to the ADA guidelines for radiation exposure, an adult recare patient, “With no clinical caries and not at increased risk for caries, should have posterior bitewing examination at 24-36 month intervals.”1
Other reasons for declining x-rays could be because of health, financial, or discomfort concerns. If a patient discloses that they have financial restrictions, it’s important to let the patient know that as a provider your utmost concern is for his or her health. Insisting on x-rays after a patient has declined may seem pushy to the patient, so communicate in a manner that is neutral. The last thing a patient should feel is he or she is being “sold” treatment. Discuss the situation with your dentist, document it in the chart and have the patient sign a refusal form.
PROBLEM 4
Declining probing due to discomfort
A 54-year old male patient of record presents for a periodontal maintenance appointment and asks not to be probed because it hurts.
Solution: Express your sorrow for the patient’s discomfort and reassure him that you have a newer more comfortable probe since his last visit. In a survey of 100 patients 61% “preferred the Goldstein Colorview Probe over a metal probe, citing it was gentler to the tissue”2 (see Figures 2-3).
In addition, applying topical anesthetic to the tissue may help ease discomfort associated with probing. In this scenario the patient is returning for periodontal maintenance, so he’s had a history of periodontal therapy. Remind him of the time and money invested in achieving optimal health and reconfirm your being committed to helping him maintain those results.
Of equal value is educating the patient. Discuss the steps that are involved in assessing the periodontal soft tissue. Careful observation includes assessing “color, contour, consistency (fibrotic or edematous), purulence (suppuration), amount of keratinized plus attached gingiva, probing depths, bleeding on probing, clinical attachment levels, presence and severity of gingival recession,”3 which enable the provider to accurately monitor and treat disease progression.
A discussion about scientific evidence that correlates with oral-systemic health issues may resonate with the patient as well. Again, if a patient refuses treatment, ensure he or she signs a refusal form so that information is well documented in the chart, but he or she should not be made to feel bad about their treatment decision. By maintaining the patient in the practice future appointments allow for discovering if the situation continues to get worse. We have patients that eventually do change their mind and allow us to continue with state of the art treatment.
PROBLEM 5
Mother of patient declines fluoride treatment
A 13 year-old adolescent patient of record presents for six-month recare appointment. The medical history is reviewed with the patient’s mother before treatment begins. The mother grants permission to complete bitewing x-rays, prophylaxis, and examination. However, she does not want her child to have fluoride. It is noted, after bitewing x-rays, that the child has several areas of incipient, proximal decay.
Solution: In this scenario, it is important to discuss findings and the mother’s concern regarding fluoride with the doctor prior to examination. This way, the doctor is aware of the mother’s concern and during the examination does not start the conversation by saying, “Mrs. Jones, we can try to remineralize these areas with in-office fluoride and home fluoride treatments.”
The above approach can cause the mother to feel defensive and also appear as though the hygienist did not communicate the mother’s concerns adequately. Instead, the doctor can begin the conversation with, “Mrs. Jones, typically when we see early signs of incipient lesions, we try a conservative approach to remineralize the enamel, which hopefully can prevent the future need for a restoration but involves the application of topical fluoride. Now I understand you have some concerns about fluoride, so are there any questions you’d like to ask me about it?” At this point the patient’s mother can express her concerns with the doctor who can provide his or her perspective on the use of fluoride. In some instances of possible allergy or even if the patient still refuses topical fluoride, an alternate route can be chosen even if it may not be your first choice. For instance, selecting products with recaldent or xylitol may help decrease the risk for tooth decay.
The problems we have covered in this series have all happened in our practice, but we have successfully dealt with them with a positive attitude. We never argue with a patient. Instead, we indicate that we understand the patient’s objection and nicely try to present research to show why we feel certain procedures, techniques, or materials are important.
And, our motto is, “The patients are always right…even when they are wrong!” In 99% of the time, we can and have reached an agreeable compromise.
Ronald E. Goldstein, DDS, is a clinical professor of oral rehabilitation at the Dental College of Georgia at Augusta University, in Augusta, Georgia; adjunct clinical professor of prosthodontics at Boston University Henry M. Goldman School of Dental Medicine; and adjunct professor of restorative dentistry at the University of Texas Health Science Center at San Antonio, Texas. Dr. Goldstein has long been considered the “architect” of modern esthetic dentistry and wrote the first comprehensive textbook, Esthetics in Dentistry, in 1976, which is now in its third edition. His consumer book, Change Your Smile, is in its fourth edition and has subsequently been published in 12 languages worldwide.
Yemia A. White, RDH, BSDH, is a registered dental hygienist in the dental practice of Goldstein, Garber, & Salama, located in Atlanta, Georgia. Ms. White is an author and researcher, as well as a member of the American Dental Hygienists’ Association and the Georgia Dental Hygienists’ Association.
References
1. Dental radiographic examinations: Recommendations for patient selection and limiting radiation for patient selection and limiting radiation exposure. American Dental Association. Council on Scientific Affairs. US Department of Health and Human Services. Public Health Service. Food and Drug Administration. http://www.ada.org/~/media/ADA/Member%20Center/FIles/Dental_Radiographic_Examinations_2012.pdf. Updated 2012. Accessed February 1, 2017.
2. White YA, Robinette CK, Bahry A. Probe selection: a hygiene team’s review of periodontal probes considers several factors. RDH. 2016;36(12):62-63.
3. Esfandiari N. Effective measurements for predictable aesthetic success. Dentistry Today. 2017;36(11):122-125.
4. Sweeting LA, Davis K, Cobb CM. Periodontal treatment protocol (PTP) for the general dental practice. J Dent Hyg. 2008;82(Suppl 3):16-26.