Vision loss from MMP
Oral Pathology
Delay in pemphigoid diagnosis could impact eyesight
NANCY W. BURKHART, BSDH, EdD
When a patient presents with multiple, chronic, nonhealing ulcers or blisters, do you automatically consider mucous membrane pemphigoid (MMP)? The answer is probably: “No!”
MMP and pemphigus vulgaris should be on your differential list of possibilities. There are some other blistering skin diseases that also warrant consideration. According to The International Pemphigus and Pemphigoid Foundation (IPPF), “Pemphigoid is a group of subepidermal, blistering autoimmune diseases that primarily affect the skin, especially the lower abdomen, groin, and flexor surfaces of the extremities. Here, autoantibodies (anti-BPA-2 and anti-BPA-1) are directed against the basal layer of the epidermis and mucosa.”
The foundation reports that the average patient sees five health-care providers over a period of 10 months in search of a diagnosis. The IPPF also reports that patients did not believe that dentists/hygienists have in the past, given them much information or assistance toward a definitive diagnosis in most cases. Some even report a misdiagnosis was given. Since patients usually seek initial treatment for oral conditions within a dental office or clinic, this becomes very frustrating for the patient.
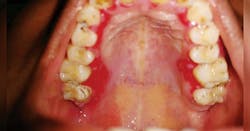
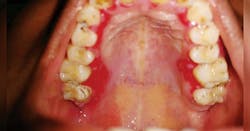
Figure 1: Palatal MMP. Courtesy of Dr. T.R. Gururaja Rao
The total body ramifications may worsen considerably as the months pass without any adequate treatment. There are two main types of pemphigoid: cicatricial pemphigoid and bullous pemphigoid.
One area of special concern for the patient is the fact that pemphigoid may affect mucous membranes, especially the eyes. This is termed ocular cicatricial pemphigoid. This type of autoimmune blistering disease may mimic other such diseases making a diagnosis difficult without additional tests. Often, a “wait and watch” approach is used and sometimes the disorder will become even more ulcerative and scarring may occur with the passage of time.
Why a delayed diagnosis?
What is the primary reason that diagnosis is delayed in dental offices? Similar oral/gingival characteristics may be caused by toothpaste allergy and other dental products, food allergy, discoid lupus erythematosus, lichen planus, factitious injury, oral facial granulomatosis and reactions to medications, just to name a few. The clinical term “desquamative gingivitis” (DG) is often used for this type of redness/ulceration that occurs on the gingiva. This is a clinical term, and it is often used for any type of oral redness that has a generalized appearance. DG may also be in all locations of the gingiva with various degrees of inflammation at any given time. DG is not a diagnostic term but a general term when a diagnosis is not known or given.
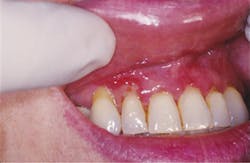
Figure 2: Gingival MMP. Courtesy Of Nancy W. Burkhart, RDH, EdD.
Who is the typical person that may be diagnosed with MMP? Usually MMP is found in older adults of either sex, but this rare, debilitating, autoimmune blistering disease may also be found on occasion in children as well. MMP usually occurs in the age range of 60 to 80 years of age, but may also be found in the fourth and fifth decades.
According to data (2017) from the Stomatology Center at The College of Dentistry, Texas A & M University in Dallas, the following information was taken from the records of 241 patients with MMP:
- The largest population were female, 3:1 over males
- Average age was 60
- 71% had more than one other medical problem
- 83% were taking a medication
- 61% were taking more than one medication
- 38.5% of women were post-menopausal
- 85% were diagnosed by mouth biopsies.
All 241 were evaluated for possible MMP eye lesions, and five were positive for such lesions.
The evaluation of the eyes is important if there is any indication of MMP. The oral desquamation, however, may be the first or only clue that the health-care provider is witnessing MMP. MMP may occur during or shortly after pregnancy and is termed, “pemphigoid gestationis.” The prevalence is 1 in 50,000 to 60,000 pregnancies.
The gingiva is involved in most cases (92.5%), and desquamative gingivitis often is the only oral feature of the disease (62.3%).
Causes of MMP
When affecting the mucous membranes, the disease is termed “mucous membrane pemphigoid.” The nose, esophagus, larynx, conjunctiva and genitalia, and anus may be affected. As noted with eye lesions, early diagnosis is crucial to limit scarring of the eyes, nose and the esophageal region. Esophageal lesions associated with MMP may cause “dysphagia” and cause extensive discomfort, limiting swallowing and eating capabilities.
In addition to the eyes, the cutaneous areas of the body can be affected and may be noted as “bullous pemphigoid.” This type of pemphigoid usually occurs in an older population within the 70 to 80 age range.
MMP is caused by antibodies that target the basement membrane and cause a weakening of the attachment of the underlying connective tissues. Multiple target antigens of MMP are identified in cell to basement membrane adhesion components by the presence of circulating autoantibodies in the patients’ serum. Bulla formation occurs in the subepithelial areas between the connective tissues and the basement membrane. The tissue is highly friable and it is not unusual to produce a “Nikolsky Sign” or stripping of the epithelium during any slight tissue manipulation. Sloughing of the tissue may occur during scaling or polishing and in severe cases, with just minimal manipulation.
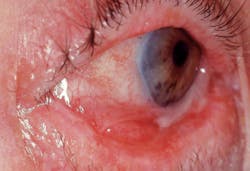
Figure 1 depicts the palatal lingual gingiva with extreme redness. Figure 2 depicts the gingival areas in a patient with MMP with epithelial stripping around the margin of #7. Figure 3 depicts the scarring of the eye and symblepharon/entropion and adhesion of the eye.
Diagnosis
MMP is diagnosed through specific testing to identify the clinical signs that are observed in the patient. MMP involves the basement membrane zone between the epithelium and connective tissues, and it is characterized by separation between the basal cells of the epithelium and the underlying connective tissue. A mild to moderate mixed inflammatory infiltrate is usually present in the lamina propria.
Direct immunofluorescence (DIF) reveals a linear pattern of complement (C3) and immunoglobulin G (IgG) along the basement membrane zone. Occasionally IgM and or IgA may be present in the linear pattern. Two tests are required: Conventional H&E histology is performed and, secondly, a DIF test. Tissue specimens are submitted in formalin for an H&E stain and the additional test termed DIF is submitted in a separate tissue specimen placed in what is termed Michel’s/Zeus solution. The importance of proper biopsy technique is crucial since there must be intact epithelium that is taken from an area overlying connective tissue. The combination of these two tests will usually confirm a diagnosis.
Figure 3: Scarring of the eye. Courtesy of Dr. T.D. Rees.
The International Pemphigus and Pemphigoid Foundation suggest that when either pemphigus or pemphigoid are suspected, the following questions are appropriate:
- Does the patient present with multiple, chronic, nonhealing ulcers or blisters?
- Are there lesions outside the mouth?
- Do lesions follow a minor trauma (Nikolsky Sign).
Ocular pemphigoid, as the name suggests, involves the eyes. The prime area that is most affected is the oral cavity but sometimes the first indication of MMP may be the eyes, which is then followed by oral tissue inflammation. Patients may complain of redness, tearing, burning, decreased vision, and/or a foreign body sensation. OCP may progress at any stage of disease.
The treatment of ocular pemphigoid has improved over the years and is being more recognized by health-care providers. Early treatment is needed before significant scarring occurs. In prior years, the patient could suffer severe damage to the eyes and often suffer vision loss because of the extensive scarring.
When a patient is suspected of MMP or pemphigus vulgaris, they should undergo an examination by medical specialists including an ophthalmologist, an otolaryngologist, and then followed very closely by dental specialists in oral medicine, oral pathology, and periodontology.
Ultimately, when maintenance is reached, a general dentist may be responsible for the maintenance of periodontal health. Hygienists need to be informed about the dental management of these patients and very well-versed in tissue changes related to MMP since they usually spend the most time with the patient during the maintenance phase of care. They are also in the front line as professionals who may identify these patients initially.
New studies and reports have identified “biological” agents, such as prednisone and rituximab, a B-Cell antibody treatment and IVIG (intravenous immunoglobulin therapy) as currently being used and found to be beneficial in the treatment of MMP and pemphigus vulgaris. Oral lesions are often treated with topical steroids, interlesional steroid injections, as well as short burst of corticosteroids. A full list of currently used corticosteroids and immunosuppressant therapy is available on the IPPF website.
Sometimes ocular scarring continues without the usual clinical appearances of redness or irritation (Williams, et al 2011). Long-term follow-up is needed in the treatment and monitoring of OCP by a professional team of specialists. Documenting any changes through digital images is very important and should be part of the patient exam process. Assisting patients in obtaining good oral habits will also improve the periodontal health of the patient and assist in controlling the overall MMP.
As always, listen to your patients and continue to ask good questions!
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics-stomatology at the Texas A&M College of Dentistry in Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/ and coauthor of General and Oral Pathology for the Dental Hygienist, which is in its third edition. She was awarded a 2016 American Academy of Oral Medicine Affiliate Fellowship (AAOMAF). She was a 2006 Crest/ADHA award winner, a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp, a 2017 Dental Professional of the Year through The International Pemphigus and Pemphigoid Foundation, and a 2017 Sunstar/RDH Award of Distinction Recipient. She can be contacted at [email protected].
References
1. Endo H, Rees TD. Clinical features of cinnamon-induced contact stomatitis. Compend Contin Educ Dent. 2006;27(7):403-9; quiz 410, 421.
2. The International Pemphigus & Pemphigoid Foundation. [email protected]
3. Rees TD, Burkhart NW. Desquamative Gingivitis (Internet). 2016. Available from: https:www.dentalcare.com/en-us/professional-education-course/ce481 (Accessed: 2017-11-3).
4. The Schirmer Test: Dental professionals should be aware of connection between dry eyes and dry mouth. RDH October 2016, page 48 Vol. 36, Number 10. http://www.rdhmag.com/articles/print/volume-36/issue-10/contents/the-schirmer-test.html.
5. Williams GP, Radford C, Nightingale P, Dart JKG, Rauz S. Evaluation of early and late presentation of patients with ocular mucous membrane pemphigoid to two major tertiary referral hospitals in the United Kingdom. Eye 2011; 25:1207-1218.
6. International Pemphigus & Pemphigoid Foundation. www.pempigus.org.