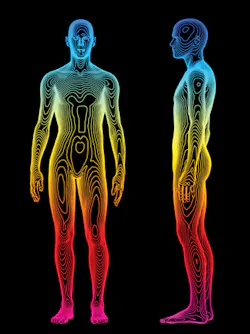
Hot or cold colors? Thermal imaging may provide additional diagnostic clues
Thermal imaging may provide diagnostic clues that may not appear with other resources
By Shirley Gutkowski, RDH, BSDH
The image on the screen is a black-and-white skeletal rendering of a tooth the patient has been dealing with his entire life. As one of the first permanent teeth in the mouth, its history was not stellar. Resin sealants were placed and replaced. The first prosthesis (an occlusal flowable composite) lasted just five years. At that time, it was replaced by a two-surface prosthesis that grew into a three-surface prosthesis. By the time the patient was 25, the tooth needed a crown; at age 32, recurrent decay forced a buccal resin. Then, at age 34, a root canal was performed. The rest of the teeth in the mouth are fine. Two other teeth have occlusal prosthetics. What happened to tooth No. 30? Well, the root canal therapy performed was successful for only three years before it started acting up. A second procedure was performed at age 45; the patient had a heart attack and the tooth was removed shortly after. Wait, what does that heart attack have to do with anything?
In the recent past there has been a huge wave of science supporting the link between periodontal inflammation and cardiovascular disease. Researchers have found periodontal pathogens in organs far from their normal habitat. Periodontal pathogens have been found in the heart, brain, placenta, amniotic fluid, and the lungs of stillborn infants. The bigger story is the system-wide inflammation due to the cardiovascular superhighway.
READ | Dental hygiene career options: Dental systemic thermographer
Inflammation is difficult to quantify and locate. Unless it is on the surface and obviously red and hot, there are very few ways to measure inflammation. Blood tests are great. Doing a test to measure C-reactive protein can give a clinician a great way to find inflammation somewhere in the body. As part of a blood panel for treating periodontal disease, high sensitivity C-reactive protein (hs-CRP) tests can give vital information. But hs-CRP tests are vague. They don't really tell where the problem lies. The inflammation can come from periodontal disease, early apical lesions, undetected cancers, sprained ankles, or adipose tissue.
But blood tests are not well received in the dental office. I'm not sure why, as the patient bleeds more during a dental procedure than any physician's procedure. Blood sampling can be a huge financial boon in the dental practice, but we just mop it up and toss it, much as we do with saliva. The drive to find less invasive diagnostics is on.
Bring the heat
Fluorescence in caries and decay detection is great. Fluorescence will show only surface inflammation, such as gingivitis. The answer to this crazy problem diagnosis of oral inflammation may be the yet unexploited feature of inflammation: heat. All inflamed tissues, by definition, are exothermic. The tissues give off heat. Even deep tissues give off heat. Did you know that a medical technology in the 1950s was developed and refined to where it can now detect temperature changes to within a 100th of a degree up to 3 centimeters below the surface with high accuracy?
This technology is called thermography. Since the 1950s, scientists have been measuring minute temperature changes in human tissue. Thermography has been proven to detect changes earlier than mammography. In traditional mammography, a mass must grow to a detectable size in order to show up on the screen-the difference between an early symptomatic lesion and one that shows up on radiographs. In cancer lingo, any measurable size is approaching late stage. Thermal changes in breast tissues occur long before the mass is detectable. False positives are rare and save thousands of hours in worry and heartache in tens of thousands of women with benign cysts and other artifacts apparent in the traditional mammography.
Although breasts are far afield of dentistry, thermography can help us detect early inflammatory changes in the oral cavity long before it shows up on the film. For instance, consider patients who return time and time again to say a tooth hurts or is bothering them, but radiographs find nothing. A thermograph may be able to help the doctor make an earlier diagnosis and start treatment earlier.
Victoria DaCosta, RDH, started a company to provide training about thermographic imaging.
When examining a thermograph, blue is cold. Green is roughly room temperature. Shades of red and white display areas of inflammation.
In a black-and-white thermal image, the darker colors are hotter.
Assessing the hot spots
Once certified in taking the thermographs, some things become obvious to the technician, such as extreme hot spots. A physician trained in reading the thermographs is next in the workflow; that practitioner will make a determination on the origins of the infection (i.e., the heat), the path it took to make the thermograph the colors it is, and what to ignore. While the inflammation is showing up on the dental thermograph, it could be passed on to the physician of record for further examination.
Dental practices have inferior diagnostics when compared to medical offices, which have access to labs, DNA testing, imaging, and so on. This has thwarted the pathway to a cohesive multidisciplinary approach to patient care. Very few dental offices have blood values to report; pocket-depth reading and bleeding on probing are historical at best and idiosyncratic at worst. X-rays are not good at measuring changes in soft tissue-at least dental x-rays are not. Compared to the advanced lab tests and imaging performed in medical settings, you can see why dentistry and medicine are still having trouble cooperating. Thermography, although a tool from the last century, has been keeping up with the times.
Where can a thermography machine be purchased? How much is it? Where can a hygienist learn how to take the images and doctors learn how to read them? Ah, grasshopper, you ask good questions. A good midrange thermography handheld camera can be anywhere from $1,000 to over $8,000. There are some that attach to smartphones, but beware-they are likely toys and useful only for party tricks.
Some of the cameras take images only in gray scale, and others are use a rainbow color palette. Then there is the version where everything but inflammation is in the gray scale; the inflammation shows up red. This is super simple, and more like an x-ray than a picture from an X-rated sci-fi movie.
Currently there are a number of places you can be trained in taking thermographic images. People with this type of certification can open their own imaging practice or work in a medical practice. The training takes about four weeks. One dental hygienist has opened up her own online training center; ThermaLinx is the company started by pioneer in oral-systemic science, Victoria DaCosta. Her training program gives dental hygienists the education and certification they need to start their own dental imaging practice so dentists can send referrals to them, or they can work in a dental practice taking thermographic images. Unless the dentist also takes a certification course in how to read the images, the thermographs must be sent off to be read.
There are many hygienists who can no longer work in a traditional dental hygiene setting. They hesitate leaving because they love patients. Providing thermographic imaging may make a transition easier. In the end, everyone wants to give patients insight as soon as possible into whatever condition they may be exhibiting. Dental hygienists, who are true prevention and minimal intervention leaders who understand the mouth/body connection, are in a perfect position to take up this type of training and offer a level of care currently unknown by traditional offices.
Thermographic images are quick, noninvasive, and specific, with low false positives or negatives. Unlike the vague answers from blood tests, thermographic images can be read immediately even by untrained clinicians before sending them off for a proper diagnosis by a qualified physician. It's real time, unlike perio charting. And there's no need to gather saliva. It's the best of all worlds. Tooth No. 30 in the imaginary example above will have a chance to be with its owner for the entire lifetime. The undetected inflammation could have been addressed before arterial plaques accumulated.
For more on the history of thermography, its limits, and future, log into crosslinkradio.com and search for "thermography" for interviews with leaders in this field. RDH
Shirley Gutkowski, RDH, BSDH, OMT, is the host of Cross Link Radio (crosslinkradio.com) and practices dental hygiene and orofacial myofunctional therapy. She is always on the lookout for strategies to prevent dental disease; the integration of oral and systemic health in Gutkowski's interviews is eye opening. She is also a lead coach at CAREERfusion (careerfusion.us), providing background and education in how dental hygienists can put their education and experience to good use.