Mobile Education: A mobilized dental clinic still relies on patient education about oral care
By Katie Melko, RDH, MSDH
Did you know that over 51 million school hours are lost each year due to dental-related illness, or that 23% of children aged two to 11 have never been seen by a dentist?1 I find this shocking. Why wait until you or a family member are in an emergency dental situation? Tooth pain is one of the most excruciating things I have experienced, and I wouldn't wish it on anymore.
Access to care, one of the main reasons patients don't make it to the dentist before a small problem turns into an emergency, is a leading driver of these kinds of statistics. Having no insurance is another. That is why mobile dental programs help bridge the gap with both of these issues. A public health mobile dental clinic travels to multiple locations and offers reduced prices, which makes it affordable and convenient for patients who struggle with finances and transportation.
A mobile dental clinic moves from location to location, providing services to families, and yet still some people don't take advantage. Why? Fear, which I'll explore in this article. Some of the locations these clinics visit are homeless shelters, senior centers, soup kitchens and pantries, health fairs, events, veteran care centers, daycares, and schools; each of these places has a different workflow to help meet the needs of the environment. I have seen mobile dental programs make a huge impact for those who receive care.
I work in a mobile dental program. We transport the equipment from place to place and use a ProCart, chair, Statim, Nomad, and cart. With these supplies, we are able to provide great services. We spend anywhere from two weeks to months in one place depending on the need and enrollment there. We provide radiographs, prophylaxis, fluoride, and sealants. Patients are given oral hygiene instruction and oral health aids to help improve their mouths and overall health. We provide referrals to our sites or local dental offices in areas where we don't have a site nearby.
Challenges to care
One of my goals as a mobile dental hygienist is to spend time educating people in the community on the importance of regular oral health care and how it can help emergent situations within the oral cavity. The problem lies in getting patients restorative care after their preventive treatments. The mobile program offers only preventive services at this time and refers to the main clinic for restorative needs. Most mobile clinic patients don't have the means of transportation or can't afford to pay for the restorative care. There may be gaps in the patients' understanding of oral disease. For example, some patients don't understand that they have a cavity because they don't feel any pain. Early diagnosis and prevention helps clinicians catch issues when they are small, which decreases the chance of infection. This is why educating the community and patients on oral health care, nutritional counseling, and caries development is crucial for behavior modification and increased patient compliance.
The patients I have cared for tell me that they probably would not have signed up for a dental cleaning if they weren't staring right at me. It isn't at the top of their priorities, even though they know they need it. Some of the people I serve are appreciative of the services provided; some are not so kind. Patients are frustrated with all aspects of their lives and the limited access to the treatment that they need. It is hard to work in public health because of the vast variety of people that I encounter, dealing with many different issues. Some are drug and alcohol abusers or recovering addicts; some are immigrants; some have lost their jobs and became homeless when they had nowhere to turn. It is important to remain open and understanding because you never know what patients have been through, and even the smallest act of kindness can make a world of difference. I often remind myself to stay positive, remember to smile, and no matter what, provide acts of kindness. Being negative and judging doesn't get you anything but anger. In this field, you have to stay flexible and open-minded, or it becomes very emotionally draining.
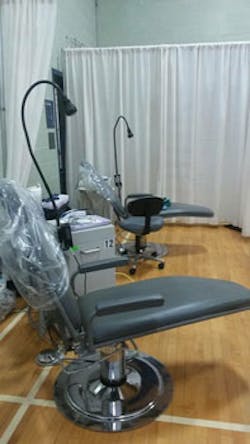
A mobile dental clinic is set up for an event at a homeless shelber.
Another challenge is language barriers; my mobile program uses an interpreting service (LanguageLine) to improve patient communication and compliance and reduce fear. Most patients are just scared of being misunderstood or have never had a dental cleaning before and are apprehensive of the appointment. The interpreting service is a great tool to make sure the clinician and the patient are on the same page. Culture competency is more important than ever before with the increased immigration to the United States. Being able to work effectively in cross-cultural situations is imperative to make the patients feel comfortable and to increase patient compliance and understanding of treatment and oral health care.
Special considerations for pediatric patients
The stories I hear when I'm at a school or daycare are so funny and make it all worthwhile. Kids tell me about losing their teeth, how they don't want to be like their dad or mom because they are missing a bunch of teeth, their experiences with the tooth fairy-and all those darn things kids just say in general! Seeing those patients leave smiling and thankful is all I need and it brings joy. Once a child asked me, "How long do you have to come here to learn how to clean teeth?" I said, "I already went to school and got my dental hygienist license." He said, "Then why are you in school cleaning my teeth if you already know how? I come here because I'm learning . . . What's your reason?" The child didn't realize I was working there like the nurse does. It was really funny and reminded me that children see things so differently.
It is a great feeling when I show scared, crying children that the clinic isn't scary and can even be fun. Seeing them laugh and enjoy the cleaning is indescribable; children who grow up fearing the dentist usually end up avoiding dental care as adults as well, so it is important to help remove that fear and create a safe environment for children. After an appointment with one such scared child, I saw her walking down the hall. She started waving excitedly and telling her friends, "That's my dentist I was telling you about yesterday. You should go!" Even though she called me a dentist (I tell children all day that I'm a dental hygienist), I was really happy that she was smiling and telling other children about her good experience.
As I mentioned, working with children in daycare and school settings is very rewarding because helping to shape the future of a child is an amazing feeling. A child's pain can impact his or her future. When a person has a toothache, he or she struggles to eat, sleep, and function. Malnourishment from not eating because of pain, or not sleeping because of pain, causes the child to struggle with everyday tasks. A child is 20% less active when suffering from tooth pain. I see many children with a completely "bombed out" dentition; their speech and confidence are impacted because of this, and they struggle to concentrate on their studies.
Sometimes I see immigrant children who have never had dental treatment before, ranging from ages five to 19. They tell me that they share their toothbrush with a grandfather or sibling, etc. Their parents can't afford floss, toothbrushes, and toothpaste. They don't want to tell their parents they need more treatment because it will cost money. The program I work with charges $30 for x-rays, prophy, and fluoride, and $25 for sealants for families who don't have insurance coverage for their children. It's reasonable and convenient, but many of these children never make it to our clinic for exams and restorative work or extractions for multiple reasons: money, transportation, lack of communication, and fear. Parents may not realize that the child's insurance covers restorative care. Some of this is because of parents not being educated on the importance of caring for baby teeth, some is negligence, and some of it is that parents don't understand what the insurance actually covers.
Educate, educate, educate
So how do we as clinicians fix this issue? Educate! Education is the first step in anything you want to achieve. Providing preventive treatment is great, but nothing happens until we get patients in for exams or restorative treatment. Programs like this are amazing and underutilized-again, because of the lack of understanding or knowledge that the program exists. I think that advancing the scope of practice for hygienists who want to do more in public health can provide so much more for the community.
This is where advanced dental therapists (ADTs) could make a huge impact in access-to-care issues. This certification and degree would provide help for so many underserved patients. Hygienists would be able to treat, relieve pain, and help provide regular care to these patients all while educating on the importance of oral health care and its connection to overall health. The ability to prescribe fluoridated toothpaste, mouth rinses, and antibiotics could make a huge impact in these children's lives.
Public health dental care is one of my passions as a clinician, and I will continue to strive to bridge the gap in oral health access to care. RDH
Katie Melko, RDH, MSDH, is a public health hygienist at Community Health Center Inc. She graduated from Fones School of Dental Hygiene at the University of Bridgeport in 2016 with an MSDH. She sits on three workgroups, two for ADHA and one for NBDHE, and has practiced dental hygiene since 2009.