New age of periodontal therapy
A.C.E your exam in regeneration dentistry
BY Susan Wingrove, RDH, BS
We are entering an exciting era in dentistry - regeneration dentistry. The time is now to educate on prevention and early detection of tissue and bone loss, as well as new advancements in periodontal therapy. Regeneration vs. repair dentistry changes the way we as clinicians evaluate and treat mucosal oral infections. The research, tools, and biologic products are now available to regenerate bone and tissue, not simply "manage and repair" it.
Periodontal therapy looks at the increased risk for certain systemic diseases due to patients' inflammatory response to the oral mucosal infection found in periodontal and peri-implant disease. Over 90% of adults over age 55 and greater than 70% of adults ages 35 to 44 are affected by periodontal disease. Now, with dental implants, clinicians must include peri-implantitis, which can affect 28% to 56% of patients in 12% to 40% of implant sites.1-4
Advancing the comprehensive exam is the first step to evolve in the regenerative dentistry era. It includes the traditional comprehensive exam along with protocols and tools to identify the optimal time for regeneration treatments.
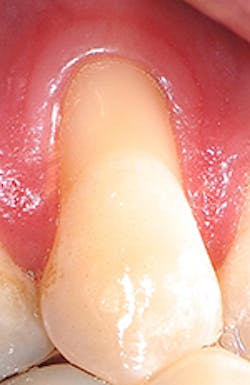
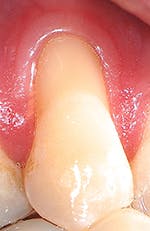
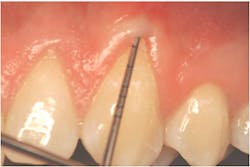
"Recession of the gingiva is becoming a prominent condition in the oral health of many patients and should be treated at its earliest detection," according to A.P. Saadoun in "Current trends in gingival recession coverage - Part I: the tunnel connective tissue graft."5 Saadoun also says the ideal time to correct gingival recession is at a Class I-II, which is less traumatic surgically for the patient, and which achieves predictable regenerative results (see Figures 1, 2).
Recent studies also show that early detection and treatment of grade II furcations are more important to the overall health of patients than previously reported. If a furcation evolves into a grade III, especially in the mandibular molars, it can lead to periodontal breakdown. Cementum pouches can develop with bacterial contamination that can serve as a nidus for recolonization and disease recurrence, or can increase the risk of furcation caries developing. There is also an association with the junctional epithelial attachment and lack of connective tissue attachment. Therefore, the progression of a grade II into a grade III furcation may increase the potential for deep, rapid bone loss within the furcation.6
To identify the optimal time for regenerative treatment, clinicians need a clear understanding of the PD Miller Marginal Tissue and the Glickman Furcation Classifications7,8 (see Tables 1, 2).
Advanced Comprehensive Exam (A.C.E.)
The new Advanced Comprehensive Exam (A.C.E.) includes the traditional comprehensive exam, with updates to evaluate for periodontal disease and peri-implant disease and mobility while focusing on the advancements in regenerative treatments.9 Evaluating for recession, attachment level, and furcations is not new, but the Wingrove A.C.E. elevates the importance of the periodic exam to a whole new level.
The A.C.E. starts with marginal tissue evaluation to identify true recession. Using a periodontal probe, take the first measurement from the cemento-enamel junction (CEJ) to the gingival margin on the facial and lingual, and record.
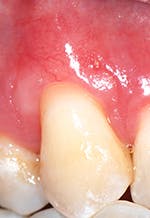
Secondly, gently retract the patient's lip or cheek to gain access, place the periodontal probe on the outside of the tissue, and measure from the gingival margin to the mucogingival junction, and record (see Figure 3).
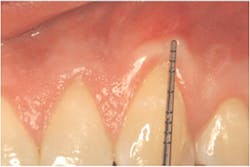
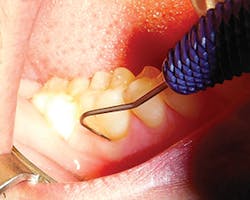
Thirdly, measure the clinical probing depth (pocket depth to the sulcus) (see Figure 4). To calculate the attached gingiva, subtract the probing depth from the outside measurement of the gingiva for the total width of of attached gingiva. Record the width of the attached gingiva and identify any teeth that need tissue regeneration, such as root coverage surgery (see Miller classification I-III, Table 1).
Report to the dentist any teeth with recession that also have loss of attached gingiva width of less than 2 mm to indicate that root coverage surgery is recommended.
To evaluate for furcation involvement, select a furcation probe (e.g., Nabers or ACE probe). The ACE probe is the next generation of probes, a straight furcation probe that is both flexible and more accurate with a newly designed periodontal probe on the other end that is designed for patient comfort (see Figure 5).
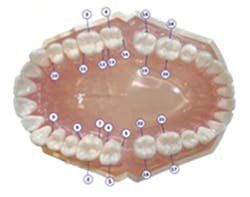
Insert the probe into the furcation locations, as shown on Figure 6. Measure and record any tooth numbers with a furcation grade (I, II, III, or IV). Refer to Glickman guidelines, and see Table 2. Focus on furcations grade I-II for the optimal time and grade III with at least one wall for regenerative treatment, such as guided bone rengeration (GBR) (see Figure 7). If the furcation progresses to a grade IV, the studies now recommend extraction and/or implant placement due to the oral-systemic risk to the patient.6,9
Report to the dentist any furcations with grade II-III and at least one wall present for possible GBR treatment.
Table 1: Miller Marginal Tissue Classification
Classification | Definition | Recommended Treatment |
Class I | Marginal tissue recession that does not extend to mucogingival junction. There is attached gingiva on the facial. There is no interdental recession. Complete root coverage is attainable. | Recommend root coverage surgery if there is sensitivity or root abrasion. |
Class II | Marginal tissue recession that extends to or beyond the mucogingival junction. Any gingiva present on the facial is unattached. There is no interdental recession. Complete root coverage is attainable. | Recommended root coverage surgery. |
Class III | Marginal tissue recession that may or may not extend to the mucogingival junction. There is interdental recession. Partial root coverage is anticipated. | Suggest root coverage surgery. Explain limitations of treatment. |
Class IV | Interdental recession is so severe both facially and interdentally that root coverage cannot be attempted. | Gingival augmentation surgery. |
Source: PD Miller Jr. A classification of marginal tissue recession 1985. Miller PD Jr. Personal Communication, 2014. | ||
Table 2: Glickman Furcation Guidelines
Grade / Class | Definition | Comment |
Grade / Class I | Probe enters the furcation area up to first black marking (1 mm-3 mm). | Identify and maintain. |
Grade/ Class II | Probe inserts to the first black marking (3 mm-6 mm) or enters the orifice. | Refer to specialist for regenerative treatment. |
Grade / Class III | Probe inserts past the first black markings (6 mm-9 mm). | Refer to specialist for regenerative treatment. |
Grade/ Class IV | Probe goes through the furcation past the orifice, visible on radiograph. Often referred to as "through and through." | Refer to specialist -options for extraction/implant. |
Source: Glickman I. The treatment of bifurcation and trifurcation involvement 1958, Wingrove S. Why revisit the comprehensive exam? 2014 | ||
Table 3: Periodontal Disease AAP Case Types: Localized ≤30% sites involved. Generalized ≥30% sites involved
Case Type | Definition | Clinical Attachment Loss (CAL) | Comments |
Case Type 0 | Clinically Healthy | No CAL | Maintain |
Case Type I | Early/Chronic Gingivitis | No CAL, ≤ 4mm Pseudopockets possible, no bone loss | Important to reverse and maintain |
Case Type II | Established Gingivitis/ Early Periodontitis | Slight CAL = 1-2 mm, BOP, ≤ 5 mm, no furcations, redness, suppuration | Radiographic: <10% attachment loss (slight/crestal), early attachment loss, SRP and/or antibiotic treatment |
Case Type III | Moderate / Chronic Periodontitis | Moderate CAL = 3-4 mm, ≤ 6mm, early furcations, redness, suppuration | Radiographic: 30% attachment loss (crown/root ratio) horizontal and/or vertical bone loss.Possible furcation, mobility. See specialist-regeneration treatment. |
Case Type IV | Advanced Periodontitis | Severe CAL = 5 ≥ mm, BOP, ≥ 7mm, advanced furcations, redness, suppuration | Radiographic: >30% attachment loss (crown/root ratio), major horizontal and/or vertical bone loss. Probable furcation, mobility.See specialist -regeneration treatment. |
Case Type V | Refractory Periodontitis | BOP, ≥ 7mm, advanced furcations, redness, suppuration, patient < 30 years old. | Radiographic: >30% bone loss. Aggressive periodontitis. Recurrent disease. Fails to respond to treatment. See specialist. |
Source: Armitage G, 2014 Commentary: Evolution and Application of Classification Systems for Periodontal Diseases - A Retrospective Commentary | |||
Periodontal Therapy treatment
Current statistics point to the urgency for dental professionals to identify and treat mucosal oral infections that have a confirmed oral-systemic connection in natural teeth and implants. Still, over 90% of patients with moderate to severe periodontal disease are treated with scaling/root planing (SRP) and/or antibiotics only. The other 7% to 9% are offered surgical treatments, and only 1% to 3% of patients are ever offered a regeneration procedure.10,11
Dental professionals hold the key role in identifying periodontal and peri-implant infections in the oral cavity. These infections act as a reservoir of pro-inflammatory mediators that enhance the inflammatory response to induce a systemic effect that can affect the overall health of the patient. New research has determined that tissue/bone loss from periodontal disease is caused by an inflammatory response to bacteria in plaque, not by bacteria alone.
Periodontal disease is now defined as an inflammatory reaction to a chronic bacterial infection that affects the tissue, bone, and supporting teeth. The immune, inflammatory process associated with periodontitis leads to apical migration of the epithelial attachment and ultimately to loss of periodontal soft and hard tissue. Now, with regeneration for both tissue and bone, the key lies in early detection and treatment.
Table 4: Peri-implantitis classification
Assessment | Classification of peri-implantitis | Comment |
Early | PD >4 mm bleeding and/or suppuration on probing* Bone loss <25% of the implant length** | Important to reverse and maintain |
Moderate | PD >6 mm bleeding and/or suppuration on probing* Bone loss 25%-50% of the implant length** | See specialist for regenerative treatment |
Advanced | PD >8 mm bleeding and/or suppuration on probing* Bone loss >50% of the implant length** | See specialist |
Note: *Bleeding and/or suppuration on two or more aspects of the implant. **Measure on radiographs ideally from baseline radiograph and at time of prosthesis loading to current radiograph. If baseline not available, the earliest available radiograph following loading should be used to current radiograph. | ||
Source: Froum SJ, Rosen PS. A proposed classification for peri-implantitis 2012 | ||
The Academy of Periodontology has outlined the case types for periodontal disease with a new focus on a regenerative treatment for moderate to advanced periodontitis, which provide long-lasting results for the patient (see Table 3).12
In addition to periodontal disease, dental implants need to be assessed and monitored for signs of peri-implantitis. Peri-implant mucositis manifests with symptoms of redness, swelling of the soft tissue, and generalized inflammation. It mirrors gingivitis in natural teeth, confined to the soft tissues only with no evidence of radiographic bone loss.
Peri-implant mucositis is reversible if detected early, with removal of the factors that are contributing to the inflammation. Peri-implant mucositis can be reversed and treatment very successful for patients with regular in-office implant maintenance and improved home-care.
Peri-implantitis begins with the same symptoms as mucositis and can be induced by occlusal stress, residue, bacteria, or a combination of these factors. A sulcular crevice develops around the implant that allows bacteria to migrate apically and infection to develop, and this ultimately leads to bone loss. The radiographic image appears as a saucer-shaped radiolucency surrounding the implant in 28% to 56% of implants after five years at 12% to 40% of implant sites (see Table 4).13
For periodontal and peri-implant disease treatment, the key is early detection. Regenerative treatments now allow clinicians to regenerate the loss of tissue and bone for optimal treatment results. Patients with moderate to advanced periodontal disease, type III or higher, are candidates for periodontal therapy. Peri-implantitis patients that are moderate to advanced, with PD >6 mm with 25% to 50% or more bone loss of the implant length, should seek guided bone regeneration treatment.
Repair vs. regeneration
The goal of periodontal therapy is the reestablishment of a healthy periodontium with restored form and function. Regeneration refers to the reproduction or reconstitution of a lost or injured part. Periodontal regeneration is the formation of new bone, new cementum, and a functionally-oriented periodontal ligament.
Repair is defined as healing of a wound by tissue that does not fully restore the architecture of the function of the part (e.g., scar tissue). Therefore, true regeneration, confirmed through histology, is the re-creation of structure and function of periodontium, new cementum, new periodontal ligament, and new alveolar bone.
To achieve predictable periodontal therapy treatment, a regenerative procedure is indicated that includes the use of bone grafting products (e.g., enamel matrix derivative, bone particles, membranes) for guided tissue and/or bone regeneration (GTR/GBR).15, 16 These treatments are designed to keep the unwanted cells out with a barrier, protecting the blood clot to allow for regeneration of periodontal apparatus (GTR) and bone (GBR). Studies confirm that regenerative periodontal procedures result in a higher gain of clinical attachment and probing depth reduction than traditional flap debridement for the treatment of intrabony and furcation defects.17-19
As the oral-systemic disease links are further defined, dental professionals need to consider the impact of periodontal therapy (regenerative treatments) for the patient's overall health. The A.C.E. propels dental professionals to the frontline of periodontal therapy and regeneration dentistry, with a real impact on total body health for patients. RDH
Susan S. Wingrove, RDH, BS, is an international speaker on the topics of implant maintenance, periodontal medicine, Advanced Comprehensive Exam (A.C.E.), and regeneration. She is the designer of the Wingrove Titanium Implant Set, ACE probes, and Queen of Hearts dental instruments. Susan is a published author on advanced instrumentation, regeneration, and implant dentistry for national and international dental journals, as well as the textbook, "Peri-Implant Therapy for the Dental Hygienist: Clinical Guide to Maintenance and Disease Complications" (Wiley-Blackwell).
References
1. Lemmerman KJ, Lemmerman NE. Osseointegrated dental implants in private practice; a long-term case series study. J Periodontol. 2005; 76(2): 310-319.
2. Attard NJ, Zarb GA. Long-term treatment outcomes in edentulous patients with implant-fixed prostheses: the Toronto study. Int J Prosthodont. 2004; 17(4): 425-433.
3. Lambrecht JT, Filippi A, Kunzel AR, Schiel HJ. Long-term evaluation of submerged and nonsubmerged ITI solid-screw titanium implants; a 10-year life table analysis of 468 implants. Int J Oral Maxillofac Implants. 2003; 18(6): 826-834.
4. Wingrove S. Peri-Implant Therapy for the Dental Hygienist: A Clinical Guide to Implant Maintenance and Disease Complications. John Wiley and Sons, 2013.
5. Saadoun AP. Current trends in gingival recession coverage - Part I: The tunnel connective tissue graft. Practical Proced Aesthet Dent 2006; 18(7): 433-8.
6. Blanchard SB, Derderian GM, Averitt TR, John V, Newell DH. Cervical enamel projections and associated pouch-like openings in the mandibular furcations. J Periodontol 2012; 83:198-203.
7. Miller PD Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985: 5: 8-13.
8. Glickman I. The treatment of bifurcation and trifurcation involvement. Clinical Periodontology, 2nd edition Philadelphia 1958.
9. Wingrove S. Why revisit the comprehensive exam? March 2014; O'Hehir University Oral Health Project Action Research Paper.
10. AAP Position Paper; Epidemiology of Periodontal Diseases. J Perio J 76:2005 1406-1419.
11. Loesche WJ, Grossman NS. Periodontal disease as a specific, albeit chronic, infection: Diagnosis and treatment. Clin Microbiol Rev 2001; 14:727-752.
12. Armitage GC. Commentary: Evolution and Application of Classification Systems for Periodontal Diseases - A Retrospective Commentary. J of Periodontol 2014: 85 (3); 369-371.
13. Nicola U, Zitzmann NU, Berglundh T. Definition and prevalence of peri-implant diseases. J Clin Periodontal. 2008; 35 (8 Suppl.): 286-291.
14. Froum SJ, Rosen PS. A proposed classification for peri-implantitis. Int. J Perio Restor Dent 2012: 10; 32 (5): 533-540.
15. AAP position paper on periodontal regeneration. J Periodontol Sept. 2005:76 (9): 1601-1622.
16. Caton J, Greenstein G. Factors related to periodontal regeneration. Periodontol 2000, 1993; 1:9-15.
17. Murphy K, Gunsoliey J. Guided tissue regeneration for the treatment of periodontal intrabony and furcation defects. A systematic review. Annals of Periodontology 2003:8(1) 266-302.
18. Needleman l, Worthington HV, Giedry-Leeper P, Tucker P. Guided tissue regeneration for periodontal intrabony defects. A review. Cochrane Database of Systematic Reviews. 2006 issue 2.
19. Venezia E, Goldstein M, Boyan BD, Schwartz Z. The use of enamel matrix derivative in the treatment of periodontal defect - A literature review and meta-analysis. Crit Rev Oral Bio Med. 2004: 15:382-402.