Lipoma
by Nancy Burkhart, RDH, EdD
Presentation: Your patient today is a 29-year-old male, named Mr. Michael Ramsey. Michael is a new patient and your treatment plan today is to complete a medical history, establish a full-mouth set of radiographs, and perform an intra- and extraoral exam with charting of all findings and existing restorations. You also routinely make intraoral photographs of any existing noteworthy findings for future reference and comparison of changes.
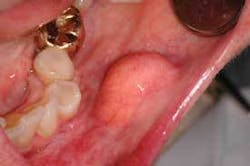
Notes and findings: Michael’s job requires frequent travel to other countries and he plays basketball when possible with a local team. His medical history includes a recent foot surgery due to a sports injury. He takes a multivitamin, along with omega-3 daily. His concern today is that he has not been able to get a dental appointment for the last six months due to his schedule, and is in desperate need of an exam and prophy. He tells you that he is aware of a swelling in the buccal mucosa region that does not seem to recede (see Figure 1).
Clinical impressions: The patient reports that the swelling in the mouth has been present for possibly a year, and he believes that it has grown significantly in the last few months. Michael tells you that, on occasion, he traumatizes the tissue while eating and this lesion can become very ulcerated.
Diagnosis: Lipoma
Etiology: This neoplasm is considered to be the most common soft tissue tumor and can occur in any tissue or organ of the body. One to 4 percent of lipomas occur intraorally and they may be confused with the fibroma when found intraorally in some locations of the mouth. Some researchers and clinicians believe that the lipoma may be more common, but often not reported or noted. The lipoma is found on the buccal mucosa and may be found in the floor of the mouth as well. In a study by Furlong (2004), statistical data confirmed 125 oral lipomas, with 91 tumors occurring in males, 33 in females, and one case in a subject of unknown gender. The mean age was 51 years old. These tumors are rarely reported in children. The site most commonly reported was the oral parotid, followed by the buccal mucosa. Other regions of occurrence were the lip, submandibular region, tongue, palate, vestibule, and floor of the mouth. The mean size of the tumor was 2.2 centimeters with a range of 0.5 to 8.0 centimeters. The observed tumor was usually reported to be present 3.2 years before the actual diagnosis.
Method of transmission: The lipoma is not contagious nor is it transmitted in any other form from one person to another. Patients will often ask this question when newly diagnosed with any type of oral disease or lesion.
Pathogenesis: Lipomas are slow-growing, benign, painless lesions with an exophytic (extending outward) growth pattern. The lesion is a soft tissue, broadly based tumor of adipose tissue with an unknown etiology. Some cases report an occurence of blunt force or soft tissue trauma to the area preceding the development of external lipomas (Aust, et al., 2007). Approximately two years on average elapse between soft tissue trauma and the development of the lipoma. Lipoma is a benign neoplasm of adipose cells, but has a malignant counterpart called liposarcoma.
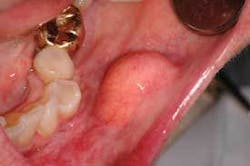
Perioral and intraoral characteristics: Intraorally, lipomas appear as superficial, smooth-surfaced, soft, palpable masses, which often impart a yellowish color to the overlying mucosa (see Figure 2). Note the size of the lipoma and the yellow lobules of adipose tissue evident in this lesion.
Extraoral characteristics: Lipomas do occur on cutaneous surfaces, appear as soft, moveable nodules, and vary in color depending upon the individual pigmentation and the location of the swelling.
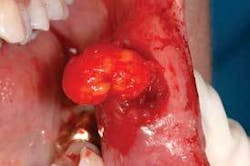
Distinguishing characteristics: Oral lipomas are described as having a soft yellow hue with a normal intraoral tissue appearance but appear to be elevated (see Figure 3). Note that the yellow lobular material in the specimen has been removed. Confusion occurs sometimes with the fibroma, which is composed of fibrous tissue and much more firm.
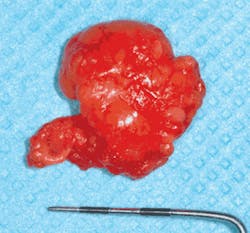
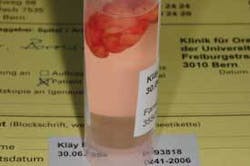
Significant microscopic features: Typically, lipomas are covered by a thin layer of epithelium with normal looking adipose tissue, but may contain cells that appear larger and greater in number. The lobules of mature fat cells are surrounded by a fibrous capsule and are found in a loose fibrous stroma. There is usually little inflammation in the specimen. Interestingly, biopsies of the specimen will float in fixative due to the amount of adipose tissue (see Figure 4).
Differential diagnosis: Lipoma must be differentiated histologically from its malignant counterpart, liposarcoma, which must be surgically removed, treated, and carefully followed. Other tumors, such as the granular cell tumor and mixed tumors, a mucocele, neurofibroma, and a traumatic fibroma, may have similar appearances (Regezi, et al., 2003) and should be considered.
Treatment and prognosis: Surgical removal of the lipoma is the treatment of choice and recurrence is not a factor when the lesion is a lipoma. The lesion is removed during a biopsy procedure in order to assure that the growth is not lipoma’s malignant counterpart, liposarcoma, or another more serious lesion. A dental professional should follow patients closely in order to facilitate the early discovery of any recurrent lesions.
The dental hygienist can be instrumental in early detection of oral lesions and oral cancer, and instrumental in the overall health of their patients.
Careful observation and follow-up of any suspicious lesion can save a life.
References
Aust MC, Spies M, Kall S, Gohritz A, Boorboor P, Kolokythas P, Vogt PM. Lipomas after soft tissue trauma: are they real? Analysis of 31 cases. Br J Dermatol. 2007 Jul;157(1):92-9. Eupub 2007 Jun 6.
Furlong MA, Fanburg-Smith JC, Childers EL. Lipoma of the oral and maxillofacial region: Site and subclassification of 125 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004 Oct;98(4):441-50.
Harnisch H, Altermatt HJ, Bornstein MM. Intraoral lipoma in the region of the mental nerve-report of a case and review of the literature. Schweiz Monatsschr Zahnmed. 2007; 117(4):372-86.
Redelingjuys IF, du Preez LA. Lipoma of the floor of the mouth: report of an unusually large lesion. SADJ. 1998 May; 53(5):245-6.
Regezi JA, Sciubba JJ, Jordan RC.K. Oral Pathology: Clinical Pathological Correlations. 4th ed. Saunders, St. Louis, MO. 2003.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry and Texas A & M Health Science Center in Dallas. Nancy is also a co-host of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is a co-author of General and Oral Pathology for Dental Hygienists, published by Lippincott Williams & Wilkins in Baltimore, which will be released in October 2007. She can be contacted at [email protected].