I have a little trick up my sleeve and so do you
Laurie Rowland, MS, RDH
Dental hygienists possess a deep understanding of the complex concepts related to periodontal health. It is understandable that patients are often perplexed when we try to explain the concepts that we have studied for years in a matter of minutes. As a dental hygienist in private practice, I was constantly searching for ways to communicate with patients effectively and efficiently—should I dust off my overly highlighted and tear-stained Wilkins textbook from hygiene school, search for a YouTube video, or find a plastic model of a tooth with the periodontium? Over the years, I investigated and experimented with numerous methods and often resorted to hunting down a blank sheet of paper and pen in a desperate attempt to illustrate concepts and connect with my patients. Because I am no Bob Ross, I had to find a better solution.
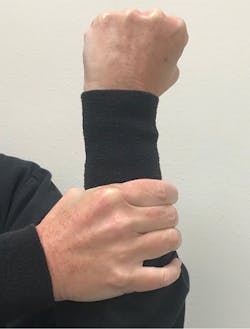
I finally had the breakthrough I was desperately seeking one day when all I could locate for a teaching tool was my own body. I removed my treatment gloves, raised the chair to an upright position, and raised my nondominant hand and arm, which I used to represent a tooth and the periodontium (figure 1).
Figure 1: Use the nondominant hand and arm to represent a tooth and its root.
With my hand in a fist, I explained to the patient, “This is the crown of your tooth, the part you can see when you look in the mouth.” The cuff of my lab coat represented the gum line around the crown of the tooth. I then pushed the cuff down under my wrist, which represented the cementoenamel junction (CEJ), and explained that my arm was the root of the tooth.
Using the index finger of my dominant hand, I had the patient imagine when a popcorn hull is stuck under the gums that it can only go so far because the tissue attaches to the root at some point under the gums . . . otherwise it could travel to their toes! (That’s just me trying to inject a little humor. Admittedly, I am no Tina Fey either.) I used my index finger to represent a periodontal probe being walked around the sulcus (figure 2). I explained that we take measurements around the entire circumference of the tooth, as the readings can fluctuate based on the level of bone and inflammation.
Figure 2: Use the index finger of the dominant hand to represent a periodontal probe being walked around the sulcus, which is represented by the cuff of the lab coat.
I pulled the cuff of my lab coat farther above my wrist to help the patient visualize how inflammation can cause the “gum line” to cover more of the crown of the tooth (figure 3). I also pulled the cuff down from my wrist, or CEJ, illustrating recession (figure 4). Turning my dominant hand into a toothbrush, I scrubbed the “gum line” vigorously to show the possible cause of the recession and explain the tooth abrasion that was present.
Figure 3: Pull the cuff of the lab coat above the wrist, which represents the CEJ, to show how inflammation can cause the gum line to cover more of the crown of the tooth.
Figure 4: Pull the lab coat’s cuff below the wrist to illustrate gum recession.
When discussing bone height and its relationship to the health and support of the tooth, I used my dominant hand to grab my wrist and show how stable the tooth is when the bone height is just under the CEJ, or wrist (figure 5). I then lowered my grasp on my arm and wiggled my arm to show how movement increases as the bone height decreases around the root (figure 6).
Figure 5: Using the dominant hand, grip the nondominant hand’s wrist to show the patient how a healthy bone height gives the tooth stability.
Figure 6: Lower the grasp on the arm and wiggle the arm to show how movement increases as bone height decreases around the root.
Seeing light-bulb moments occur when I gave this first demonstration convinced me that I had just found the easiest and, more importantly, the most effective way of communicating these concepts to my patients. Of course, the more I used the technique, the more effective I was in my presentation to patients. Now I am fully confident that I can transfer my knowledge effectively to any patient or caregiver in a manner that he or she can comprehend by using this simple demonstration.
Over the years of using my arm and hands to illustrate conditions, I have found that not only are patients engaged and attentive, but they have a clear picture in mind of the sometimes confusing concepts I am trying to explain. This basic understanding usually leads to patients asking more meaningful questions regarding their treatment and expected outcomes. Certainly, more technical or scientific resources can then be utilized, as patients are much more likely to be receptive and understanding once they have a solid base on which to build their knowledge.
As dental professionals, we are obligated to educate our patients about their current periodontal status, the ways we evaluate that status, and what we can do together to improve or maintain their oral health. The dental hygienist is the perfect member of the team to communicate findings from assessments and ensure that patients have enough information to make informed decisions regarding their treatment. Because every patient we see has a different knowledge base, we must individualize patient education, ensuring that even those with a low dental IQ are informed about all aspects of their periodontal condition in a way they can comprehend. Using lay terms, visuals, and concepts relatable to the patient, we can ensure that we are treating all those we serve with the utmost care.Laurie Rowland, MS, RDH, is a dental hygienist and educator with 19 years of experience. She earned her bachelor of science degree in interdisciplinary studies and her master of science degree in curriculum and instruction from Texas A&M University in College Station, Texas. In 1999, she received her dental hygiene license after graduating from the Blinn College dental hygiene program in Bryan, Texas. She is now a professor at Blinn College, where she serves as clinic coordinator and teaches preclinical dental hygiene, dental hygiene care, and dental hygiene practice.
About the Author
Laurie Rowland, MS, RDH
Laurie Rowland, MS, RDH, is a dental hygienist and educator with 19 years of experience. She earned her bachelor of science degree in interdisciplinary studies and her master of science degree in curriculum and instruction from Texas A&M University in College Station, Texas. In 1999, she received her dental hygiene license after graduating from the Blinn College dental hygiene program in Bryan, Texas. She is now a professor at Blinn College, where she serves as clinic coordinator and teaches preclinical dental hygiene, dental hygiene care, and dental hygiene practice.
Updated May 16, 2019