Gluten Worries
The "staff of life" or a chronic poison?
by Josalyn Sewell, RDH, OMT
"Give us this day our daily bread." "Bread is the staff of life." "The best thing since sliced bread." "Bread always falls on the buttered side." "Know which side one's bread is buttered on." Bread is engrained (pun intended) into the American way of life.
We delight in the warm fluffy goodness of a hot dinner roll with melted butter. We can hardly eat salad or soup without the accompanying breadstick. We have creative ways of using bread for all meals and snacks throughout the day. But what happens when bread doesn't like us back? And I am not referring to the extra pounds in our midsection. For one in 133 Americans, bread is more of a chronic poison than the "staff of life."
Celiac disease
The National Foundation for Celiac Awareness states that celiac disease (also referred to as celiac sprue, nontropical sprue, and gluten-sensitive enteropathy) is an autoimmune disorder triggered by consuming a protein called gluten, which is found in wheat, barley, and rye. When a person with celiac disease (CD) eats gluten, the protein interferes with the absorption of nutrients from food by damaging intestinal villi. Damaged villi make it nearly impossible for the body to absorb nutrients into the bloodstream, leading to malnourishment and a host of other problems, including cancer, thyroid disease, osteoporosis, infertility, and the onset of other autoimmune diseases.
Accurately diagnosing CD can be very difficult, as the symptoms often mimic those of other diseases, including irritable bowel syndrome (IBS), Crohn's disease, intestinal infections, lactose intolerance, and depression. Eighty-three percent of those suffering from CD are undiagnosed or misdiagnosed. It takes an average of eight to 10 years for individuals to receive an accurate diagnosis. The only definitive means of accurately diagnosing CD is an intestinal biopsy, the gold standard for diagnosis. However, specific blood tests (serological testing) are an important indication of whether or not someone has celiac disease. In order for these tests to be accurate, it is important that the individual is eating gluten-rich foods as limiting or eliminating gluten would provide a false negative.
--------------------------------------
Consider reading:
--------------------------------------
Saliva testing, buccal biopsies, and breath tests are available but these tests are not as reliable. As the science improves, we may see dental professionals screening for CD in the future. Diagnosis may reach 50% to 60% (rather than 5% to 17%) by 2019 thanks to efforts to increase public awareness.1
What is gluten?
Wheat is approximately 10 to 15% protein; the remainder is starch. Gluten is what remains after the starch granules are washed from wheat flour. When protein is digested, it gets broken down in the stomach and small intestine into single amino acids that are readily absorbed by the small intestine. The gluten molecule is resistant to the enzymes that break down proteins, resulting in a long peptide chain, composed of 33 amino acids. This chain is not digested well by humans. It gets into the lining of the intestine, underneath the epithelial cells lining the villi. Some individuals develop an immunological reaction to this fraction, which results in inflamed intestines and destroyed villi.2
The spectrum of gluten sensitivity
In addition to celiac disease, individuals may have a wheat allergy or nonceliac gluten sensitivity. A wheat allergy is similar to any other food allergy. Symptoms of a wheat allergy include:
- Swelling, itching, or irritation of the mouth or throat
- Hives, itchy rash, or swelling of the skin
- Nasal congestion
- Itchy, watery eyes
- Difficulty breathing
- Cramps, nausea, or vomiting
- Diarrhea
- Anaphylaxis
For some people, wheat allergy may not be a lifelong disorder. It is more common in infancy and early childhood. Most children who have a wheat allergy also have other food allergies. Children usually outgrow wheat allergies between the ages of three and five. Celiac disease cannot be outgrown.
It is estimated that approximately 6% of the population may have nonceliac gluten sensitivity (NCGS). These individuals cannot tolerate gluten and experience symptoms similar to those with celiac disease but lack the same antibodies and intestinal damage as seen in celiac disease. Early research suggests that nonceliac gluten sensitivity is an innate immune response, as opposed to an adaptive immune response (such as autoimmune) or an allergic reaction. Individuals that fall under this sensitivity experience many non-GI symptoms like "brain fog," headaches, joint pain, and numbness in the fingers, legs, or arms. Symptoms typically appear hours or days after gluten is ingested. There are currently no tests that confirm NCGS. The only way to accurately determine if someone is sensitive to gluten is to try the gluten-free diet (National Foundation for Celiac Awareness).
Why the sudden increase in gluten sensitivity?
Why does there seem to be such an increase in gluten sensitivity after the thousands of years that wheat has occupied a prominent place at the table? Human interventions through hybridization methods have changed grain more in the last 50 years than in the last 5,000. The loaf of bread we make is different even than the one that came from our grandmother's oven – not in look, not in taste, but different biochemically. Why did scientists genetically alter wheat? Much of the world is starving and in order to combat world hunger there had to be a way to make more wheat at a faster rate. Dr. Norman Borlaug is considered the "Father of the Green Revolution" and was given the Nobel Peace Prize in 1970, the Presidential Medal for Freedom, and the Congressional Gold Medal for his work in creating high-yield dwarf wheat that did indeed help the issue of world hunger. He had solved two problems by producing a high-yield stalk that is shorter and stockier. A short stalk stays alive longer and takes less time to grow – it also uses less fertilizer.
Despite dramatic changes in the genetic makeup of wheat and other crops, no animal or human safety testing was conducted on the new genetic strains. Wheat + wheat = wheat, right? Wheat gluten proteins in particular undergo considerable structural change with hybridization. In one hybridization experiment, 14 new gluten proteins were identified in the offspring that were not present in either parent wheat plant.2 Dr. Borlaug is not the only person to change wheat. Thousands of experiments on wheat have been performed – some with success, and many without. The takeaway is to understand that the wheat we consume today is genetically and biochemically different than it was generations ago and may be the reason gluten sensitivity has become so common.
Oral manifestations of celiac disease
The Journal of Canadian Dentistry published "Oral Manifestations of Celiac Disease: A Clinical Guide for Dentists" in 2011. The following conditions were listed as possible oral indications of CD:
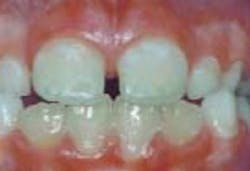
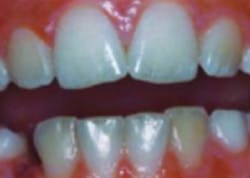
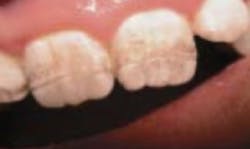
- Enamel defects
- Delayed eruption
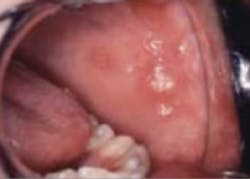
- Recurrent aphthous ulcers
- Cheilosis
- Oral lichen planus
- Atrophic glossitis
If celiac disease appears in children while the permanent teeth are developing (before age seven), abnormalities can occur in the dental enamel. "These defects are seen most commonly in the permanent dentition and tend to appear symmetrically and chronologically in all [four] quadrants, with more defects in the maxillary and mandibular incisors and molars. Both hypoplasia and hypomineralization of the enamel can occur. […] The exact mechanism leading to these defects is not clear, but immune-mediated damage is suspected to be the primary cause. Nutritional disturbances, including hypocalcemia, may also play a role."
While aphthous ulcers are often seen in other conditions – oral infections, immunodeficiency states, and Crohn's disease – the possibility of celiac disease should remain part of the differential diagnosis. Many people with celiac disease only have symptoms relating to oral and dental abnormalities.3
Role of the RDH
As hygienists, we have the special opportunity to screen for possible systemic conditions and help our patients understand how inextricably linked oral health is to systemic health. The JCDA lists six recommendations for dental professionals:
1. Consider celiac disease as a possible diagnosis in any patient with dental enamel defects, recurrent oral aphthous ulcers, or both.
2. Question about other clinical symptoms of celiac disease, including abdominal pain, diarrhea, weight loss, poor growth, anemia, and extreme fatigue. Remember that absence of these symptoms does not rule out celiac disease.
3. Inquire about the presence of other autoimmune diseases; especially type 1 diabetes and thyroiditis. The presence of these will further increase the probability of celiac disease.
4. Consider adding celiac disease to the list of disorders that you inquire about during family history screening. Having a first or second-degree relative with CD increases the likelihood of positive diagnosis.
5. If celiac disease is suspected, the dentist or dental hygienist may wish to coordinate laboratory testing with the patient's primary care physician or specialist.
6. Do not recommend a gluten-free diet to a patient suspected of having celiac disease without confirmation of the diagnosis.3
In addition to these recommendations I would like to add one more.
7. Pay attention to products used in the office and recommended to patients. While many dental products do not characteristically contain gluten, it is important to never assume that they are safe for patients with gluten sensitivity. The best choice is to use products that have been certified and labeled as gluten free.
Conclusion
Gluten sensitivity – celiac disease, nonceliac gluten sensitivity, or a wheat allergy – can be challenging to live with. Consider what it would be like to have to research every ingredient and read every food label before putting something in your mouth or on your skin. Knowledge is power, and I encourage you to continue to arm yourself with more information about gluten sensitivity and take the initiative to ensure gluten-free products are used in your practice. RDH
Josalyn Sewell, RDH, OMT, enjoys many aspects of a dental hygiene career, including clinical work, teaching, speaking, writing, and sales. She is a member of both the ADHA and CareerFusion. Josalyn's full-time position is in domestic management (stay-at-home-mostly-mom) in a rural town in the mountains of eastern Arizona. She blogs about what it is like to raise a child on the autism spectrum. You can find her blog at: autismaintforsissys.blogspot.com or on Facebook: Autism Ain't for Sissys.
References
1. Celiac Disease Awareness Campaign of the National Institutes of Health. Educational Material and Resources. Retrieved July 30, 2013 from www.celiac.nih.gov/materials.aspx.
2. Peter HR, Green MA. (2006). Celiac Disease: A Hidden Epidemic. New York, New York: Harper Collins Publisher.
3. Mohsin Rashid MZ. (2011). Oral Manifestations of Celiac Disease: A Guide for Dentists. Journal of Canadian Dental Association, 77, b39.
4. National Foundation for Celiac Awareness. www.celiaccentral.org. Retrieved July 25, 2013.
5. William Davis M. (2011). Wheat Belly. New York, New York: Rodale.
Symptoms of Celiac Disease
Though some individuals report no symptoms at all, there are over 300 symptoms associated with CD. Common complaints include:
- Abdominal cramping/bloating
- Anemia
- Constipation
- Diarrhea
- Energy loss
- Fatigue
- Infertility
- Irritable bowels
- Joint pain
- Recurrent aphthous ulcers or cracks in the corner of the mouth
- Dental enamel defects
- Weakness
- Weight loss
- Dermatitis herpetiformis
Treatment: gluten-free diet (GFD)
The only way to treat all forms of gluten sensitivity (wheat allergy, celiac disease, nonceliac gluten sensitivity) is to live on a gluten-free diet. This can be very challenging and very difficult for individuals, as gluten is found in more than just breads and pastas. Individuals must invest time in learning about gluten and its hidden forms and learn to consistently read food labels. Dining out can be especially difficult. Individuals with gluten sensitivity must avoid:
- Wheat
- Rye
- Bulgar
- Farina
- Graham flour
- Kamut
- Semolina
- Spelt
- Barley (malt, malt flavoring, malt vinegar)
- Bran
- Orzo
- Triticale (cross between wheat and rye)
As it is not always possible to see a list of ingredients for particular foods, individuals should avoid these foods (unless they are labeled gluten-free):
- Beer
- Dressings
- Couscous
- Tabbouli
- Gravies
- Sauces
- Candy
- Potato chips
- Tortilla chips
- Canned soup and broth
- Bouillon cubes
- Frozen or canned vegetables in sauce
- Restaurant or fast food French fries
- Baked goods
- Fried foods
Initially adapting a gluten-free diet can be intimidating and at times very frustrating. Over time it will become easier and feel less restricting. Foods that are safe include:
- Corn
- Potato
- Rice
- Fresh fruits and vegetables
- Meat
- Fish
- Poultry
- Most milk and dairy products
Past RDH Issues