Case #6
by Joen Iannucci Haring
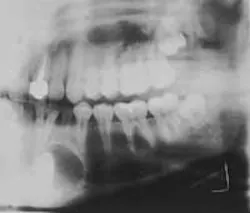
A 15-year-old male visited a dentist for a routine checkup. Radiographic examination revealed a large lesion in the left mandible.
History
The patient denied any history of signs or symptoms associated with the left mandibular canine region. The patient appeared to be in a general good state of health, with no significant medical history. The patient's dental history included regular dental examinations and routine dental treatment.
At the time of the dental appointment, the patient was not taking medications of any kind.
Examinations
The patient's vital signs were all found to be within normal limits. Examination of the head and neck region revealed no enlarged or palpable lymph nodes. Examination of the oral soft tissues revealed no unusual findings. No bony abnormalities were noted.
Radiographic findings
The patient's most recent bite-wing radiographs were taken one year ago, and the most recent panoramic radiograph was taken three years earlier. After a thorough clinical examination and a review of the patient's medical and dental histories, a panoramic radiograph and four bite-wing films were ordered.
Examination of the panoramic radiograph revealed a large, well-defined radiolucency with faint, scattered radiopaque flecks. The lesion was seen surrounding an impacted mandibular canine (see radiograph).
Clinical diagnosis
Based on the clinical and radiographic examination available, which of the following is the most likely diagnosis?
o cementoblastoma
o cementifying fibroma
o calcifying odontogenic cyst
o dentigerous cyst
o adenomatoid odontogenic tumor
Diagnosis
• adenomatoid odontogenic tumor
Discussion
The adenomatoid odontogenic tumor (AOT) is a benign odontogenic tumor of epithelial origin. The AOT accounts for approximately 3 to 7 percent of all odontgenic tumors. This neoplasm evolves from elements that are normally involved in the formation of teeth.
Clinical features
The AOT is most often seen in individuals within the ages 10 to 19. Females are affected twice as frequently as males. The AOT usually occurs in association with the crown of an impacted tooth and is found in the anterior region twice as often as the posterior region. The maxilla is involved more frequently than the mandible. The most common location for the AOT is around the crown of an impacted maxillary incisor or canine. The AOT is a slow-growing, solitary lesion. Pain is usually not a feature. Bony expansion may or may not be present.
Radiographic features
The AOT may appear as a radiolucent lesion or a mixed lucent-opaque lesion with well-defined borders. The AOT often appears as a radiolucency with faint, scattered radiopaque calcifications. In the early states of development, the AOT may first appear as a radiolucency. Over time, radiopaque foci are likely to develop. The size of the AOT is variable. The location is usually anterior. When viewed on a dental radiograph, the AOT is typically seen in association with an impacted tooth incisor or canine. The AOT cannot be diagnosed from its radiographic appearance alone.
Diagnosis
Biopsy and histologic examination of the lesion is necessary to make a definitive diagnosis. Histologically, the AOT exhibits numerous duct-like structures and masses of cuboidal and spindle-shaped epithelial cells. The duct-like structures are characteristic for the AOT. The term "adenomatoid" means resembling a gland (histologically, a gland exhibits duct-like structures). Small calcifications may also be seen histologically; in which case, the radiographic appearance would include radiopaque foci.
Lesions that may be considered in the differential diagnosis for the AOT include the dentigerous cyst and the calcifying odontogenic cyst.
Treatment
The AOT must be removed. Surgical enucleation is the treatment of choice. The tumor can be easily removed from the surrounding bone because of its capsule. The AOT does not recur following removal.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.