Case #11
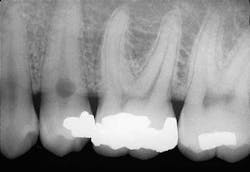
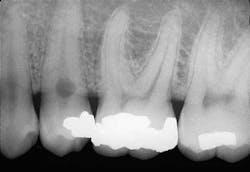
A 35-year old male visited a dental office for a routine checkup. Radiographic examination revealed a round radiolucency at the cervical region of tooth #29.
History
The patient denied any history of pain associated with the mandibular premolar area. The patient appeared to be in a general good state of health with no significant medical history. His dental history included sporadic checkups and routine restorative dental treatment.
Examinations
The patient's vital signs were all found to be within normal limits. Extraoral examination of the head and neck region revealed no enlarged or palpable lymph nodes. Intraoral examination revealed no abnormalities present.
Based on the clinical examination of the patient, selected periapical radiographs, bitewings, and a panoramic film were ordered and exposed. A review of the films revealed a round radiolucency at the cervical area of the tooth #29 (see film). No other abnormalities were noted on the radiographs.
Clinical diagnosis
Based on the clinical and radiographic information available, which one of the following is the most likely diagnosis?
• dental caries
• external resorption
• internal resorption
• hypophosphatasia
• cervical abrasion
Diagnosis
• internal resorption
Discussion
Internal resorption, as the name suggests, involves resorption of the internal surfaces of the tooth. Internal resorption occurs within the crown or root of a tooth and involves the pulp chamber, pulp canals, and surrounding dentin. Most cases occur in response to injury to the pulpal tissues, such as caries-related inflammation or physical trauma. In other cases, no precipitating factor can be identified. The resorption process may continue to take place as long a vital pulp tissue exists.
Clinical features
Internal resorption is a relatively rare finding. This process can occur at any tooth site that contacts vital pulp tissue. Internal resorption is typically asymptomatic and discovered during routine radiographic examination. Pain is sometimes a symptom if the resorptive process is associated with significant pulpal inflammation. For example, in cases where the pulp tissue expands, perforates the root surface, and extends into the periodontal ligament space, a pulpal infection results and the tooth becomes symptomatic.
Internal resorption may be seen in the deciduous or permanent dentitions. Usually a single tooth is involved. The maxillary central incisor is the tooth most often affected by internal resorption. Most cases of internal resorption are associated with the radicular portions of the teeth and are not apparent clinically. Although internal resorption may involve any portion of the pulp canal, the cervical region is most often involved. In such cases, the coronal pulp is necrotic while the apical portion remains vital. The area of destruction usually appears as a round or ovoid well-defined, symmetric enlargement of the pulp chamber or canal. If extensive internal resorption is present within the root of a tooth, the root may weaken and a fracture may result.
When internal resorption occurs within the pulp chamber and crown of a tooth, the resorption is apparently clinically — in such cases, the crown may exhibit a pink discoloration (also known as pink tooth of Mummery) because of the proximity of the pulp tissue to the tooth surface. The vascular pulp tissue when seen through the thin enamel is what gives the clinical crown a pink discoloration.
Radiographic features
Internal resorption that occurs within the crown or the root of a tooth appears as a round or ovoid radiolucency. The outline of the internal resorption may appear smooth and well-defined, or ill-defined and scalloped. In some cases, the resorptive process may be so extensive that the entire crown or width of the root may be involved.
Diagnosis and treatment
The diagnosis of internal resorption is made based on its radiographic appearance. Treatment for teeth affected by internal resorption is variable. Internal resorption may be successfully stopped if endodontic therapy removes all vital pulp tissue before it perforates into the periodontal ligament. Once such perforation occurs, the prognosis is poor. Extraction may be necessary for teeth extensively weakened by resorption, or for teeth with perforations, as well as those that do not respond to endodontic therapy.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.