That is a beautiful implant restoration. Now what?
This is a question that should be asked by all implant patients immediately after the implant restoration is finalized. And the dentist and hygienist must both be prepared to answer in depth. Although it is true that implants enjoy a high survival rate, (1) it is just as true that implants — if not cared for properly — suffer from a high rate of peri-implant disease. (2) Restorations around natural teeth have taught us various methods of in-office debridement and treatment protocols. We, as a dental profession, are also well-skilled at demonstrating proper home care to patients with fixed restorations. Unfortunately, this art form has been lost with implant restorations. Too many patients leave the office after implant crown insert with the thought that “Now that I have my implants, I don’t have to see the dentist anymore.” (Figs. 1 and 1a)
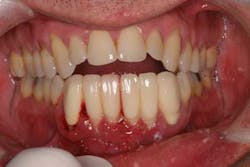
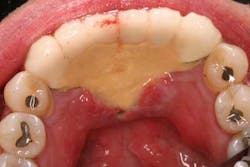
Figs. 1 and 1a: The buccal and lingual view of a patient with a fixed bridge supported by implants from Nos. 22 through 27. The patient disappeared for a year after insert with a chief complaint of “gum soreness.” He claimed, “Nobody told me how to clean this.”
We know from the literature that many of the pathogens encountered around natural teeth are the same ones we are dealing with when it comes to implants and their restorations. (3) In addition, we also know from the literature that peri-implant breakdown occurs more frequently and more rapidly when an assault occurs when compared to natural teeth because of the differences in attachment apparatus. (4) It is because of this rapid destruction that careful scrutiny and surveillance is paramount to long-term survival when dealing with implant dentistry. Many studies have demonstrated that with careful follow-up and strict hygiene regimens, teeth that were deemed questionable at the beginning of the study — and probably would have been extracted today — were able to be maintained and stayed in the patient’s mouth. (5)
If we extrapolate that data and insert it into a modern dental practice, there is no reason why we can’t have similar results with implant fixtures. Being a hygienist in a periodontal practice, most of my patients are on a three-month recall. Most of our recall protocols are based on literature suggesting that patients who are placed on three-month recare schedules typically perform better than those seen at longer intervals, and they also tend to keep their teeth for longer periods of time. (6) Because many patients who receive implant therapy in my office are patients with previous histories of periodontal disease, most implant patients are put on this three-month recall visit until they demonstrate good home care and/or absence of disease progression. The mantra remains if they lost their teeth to periodontal disease, they certainly can lose their implants to peri-implant disease.
During a typical implant maintenance visit, my surveillance consists of recording probing depths, noting bleeding upon probing/suppuration, noting presence of mobility, recording the amount of keratinized tissue present, noting the soft-tissue texture and color. In addition, radiographs are taken in a standardized method if warranted. After the clinical exam is completed, dental maintenance is performed with proper armamentarium.*** At the end of the visit, oral hygiene instructions are given. This may take anywhere from five to 20 minutes depending upon the complexity of the implant restoration and the level of home care demonstrated by the patient. I typically recommend ultra-soft toothbrushes/mechanical toothbrushes along with automated interproximal cleaning devices. (Fig. 2)
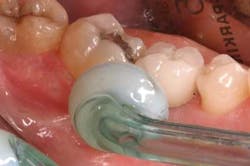
Fig. 2: Interproximal irrigator, Sonicare Air Flosser, being used by hygienist to demonstrate to patient how to clean a posterior single-tooth implant restoration overcontoured on the distal leading to a food trap.
If the patient still manages to perform poorly with home care, a separate visit just to review and demonstrate home care may be warranted. The cliché “An ounce of prevention is worth a pound of cure” certainly holds true in implant dentistry.
*** A full description of implant maintenance armamentarium, along with treatment modalities and methods, will be presented by the author at RDH Under One Roof in a seminar titled “Recognition, Prevention, and Treatment of Implant Complications: A Hygienist’s Role.”
Author bio
Rebekah A. Duffy, RDH, has been a hygienist in private practice for more than 10 years. She has lectured and written articles involving peri-implant maintenance and soft-tissue considerations. She currently works in a periodontal practice in New York City, N.Y.
References
1. Esposito, Hirsch, Lekholm, Thomsen. Biological factors contributing to failures of osseointegrated oral implants I. Success criteria and epidemiology. Eur J Oral Sci 1998;106:521-557.
2. Berglundh T, Persson L, Klinge B. (2002). A systematic review on the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. Proceedings from the 4th European Workshop on Periodontology. Journal of Clinical Periodontology 2002;29(Suppl), 197–212.
3. Leonhardt A, Berglundh T, Ericsson I, Dahlén G. Putative periodontal pathogens on titanium implants and teeth in experimental gingivitis and periodontitis in beagle dogs. Clin Oral Implants Res 1992; 3:112–119.
4. Koka S. The implant-mucosal interface and its role in the long-term success of endosseous oral implants: a review of the literature. Int J Prosthodont 1998; 11:421-432.
5. Hirschfeld I, Wasserman B. A long-term survey of tooth loss in 600 treated periodontal patients. J Periodontol 1978; 49(5):225-237.
6. Wilson TG Jr. Maintaining periodontal treatment. J Am Dent Assoc. 1990; 121(4):491-494.