Traumatic injury from an electric socket
by Nancy W. Burkhart, RDH, EdD
[email protected]
Your patient is a 47-year-old male, Henry, who reports today for a yearly maintenance appointment. Henry has had a change in his insurance coverage and consequently had to find a practice on his new list of providers. Since you have not seen him as a patient before, you provide a new patient exam, complete with a medical history, charting, periodontal probe readings, and radiographs, since he has not had any for five years, as well as a thorough extra- and intraoral exam. He appears to be a normal, healthy male with no problems reported regarding his teeth or oral health.
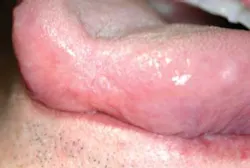
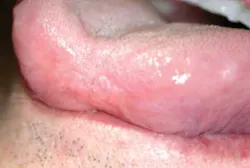
Figure 1: The slide depicts a shortened tip of the tongue. Small, sessile, coalescing smooth tissue segments are present due to a traumatic injury that occurred over 40 years earlier.
As you begin to inspect the oral tissues, you notice that the dorsal tongue, including the tip, has a shortened and somewhat concave appearance. The contour, surface area, and papillae do not appear normal (see Figure 1). Your first instinct is that this finding is from a prior injury and probably one that occurred long ago since the tissue is nonulcerated, smooth, and completely healed.
Upon questioning the patient, you discover that the injury did indeed occur long ago when the patient was three years old. As a child, he placed his tongue in a light socket. Fortunately, his parent was close by and was able to get medical assistance right away to stop the bleeding and administer care. The patient reports no problems with this area of the tongue such as tingling, numbness, or pain.
Traumatic injuries occur frequently, and we often need to identify them as current or prior injuries, asking appropriate follow-up questions to sort through the possibilities.
On the initial inspection, the tissue might appear as a fibrotic growth, such as a fibroma (fibrous connective tissue). However, since the patient was able to relay the history related to the tissue trauma, it was rather easy to determine that the area was scar tissue related to a previous injury. Many times the circumstances involving the etiology are as important as recording a description of the lesion. Appropriate communication with the patient is highly important.
Digital photography
Digital photography is vital to lesion documentation. With digital photography, we are able to gain a better perspective of the lesion, and we are able to compare future changes in existing lesions. As an example, this is especially true for conditions such as lichen planus (and other mucosal diseases), morsicatio buccarum (chronic cheek chewing) and morsicatio labiorum (chronic lip chewing), where there is a wide range of both surface destruction and sometimes color changes. Lesions that cover large areas of tissue are very difficult to adequately describe and compare in future evaluations.
Before the technology that we now utilize, written descriptions were our only source of documentation. However, comparison of previous lesions recorded through digital photographs are easy to assess and a better representation than handwritten descriptions (these are only as good as the person who records the findings, and these can be subjective).
Documentation, measurement, and recording findings are still a vital part of the permanent record of all patients and very important for those offices who do not use digital technology at all. Descriptions are most important because they help the practitioner sort and categorize specific types of lesions in order to prioritize a differential diagnosis. An example would be of a verrucous lesion that would be in a different etiology category than a smooth, fibrotic lesion (see "Determining lesion etiology").
Taking an excellent health history, and performing a complete extra- and intraoral exam is crucial in early cancer detection. No amount of documentation is meaningful if there is no decision making and referral that follow questionable observations by the practitioner.
As with any discovery of a lesion in the mouth, a biopsy should always be performed when the practitioner is concerned that the lesion is possibly malignant. If there is uncertainty regarding the etiology such as one that may have a frictional component, the patient should be monitored; if after a two week period, a determination of etiology has not been established, or the lesion still persists, a biopsy is the gold standard. The patient should receive a biopsy in your office or be referred to an oral medicine specialist, an oral pathologist, or an oral surgeon. If there is suspicion that you may be dealing with a serious lesion initially such as cancer or a precancerous condition, the practitioner should not hesitate to refer the patient or perform the biopsy at that time. Sometimes it is wise to establish an appointment for two weeks and then let the oral surgeon or pathologist assess the area at that time. If the biopsy is needed, it can be performed at that time.
It is always a pleasant surprise for the patient if they discover that a biopsy will not be needed and the lesion is no longer present. In office tests detecting color changes of abnormal tissue such as chemiluminescence or direct fluorescence, visualization can be helpful in making a decision or encouraging the patient to have the gold standard, which is a biopsy.
Keep asking good questions and always listen to your patients.
References
Burkhart NW, DeLong L. (2009). The Intraoral and Extraoral Exam (CE 337). Available at: http://www.dentalcare.com/en-US/getCourseList.do.
DeLong L, Burkhart N. General and Oral Pathology for the Dental Hygienist. Lippincott, Williams & Wilkins. Baltimore. 2008.
McCann A. Describing Soft Tissue Lesions of the Oral Cavity, Dental Hygiene News, 5,9, Spring, 1992.
Siegel M, Murrah V, Aloise D. Head, Neck and Oral Cancer Examination. MedEdPORTAL; 2009. Available from: http://services.aamc. org/30/mededportal/servlet/s/segment/mededportal/?subid=7768.
Determining lesion etiology
Communication in etiology determination
1. Has the patient noticed the ulceration, excess tissue, or reddened area in the specific location that has been noticed?
2. Show the patient the area with a mirror, as you discuss the findings.
3. Has this occurred before?
4. At what intervals does this occur, and how long does it last?
5. Has the patient noticed any "triggers" that caused the lesion to appear or reappear?
6. Do any foods, alcohol, hot liquids, or dental products cause any change in the lesion/lesions?
7. If the area of concern is from a previous injury, ask the patient about the details, approximate date of the injury, and document your findings with written data and digital photographs.
8. If patients are unable to recall a prior injury, it is appropriate to ask them if they might have any idea what the cause might be. This sometimes starts a thought process in motion and may help to determine a cause. (See October 2010 RDH column, "Similar lesions, yet only one is benign.").
Documentation
a. What is the location of the lesion?
b. Is the lesion single or multiple?
c. What is the size of the lesion? Use a probe to measure the lesion and describe the shape and borders of the lesion.
d. What is the color of the lesion? Colors assist in a differential diagnosis by allowing the practitioner to separate possible etiology (such as vascular lesions from traumatic lesions). Lichenoid reactions from medications should be considered.
e. Is the lesion raised or depressed?
f. Is the lesion a vesicle, bulla, or pustule (containing pus)?
g. Is the lesion plaque-like, ulcer-like, or is it a solid, smooth lesion? Perhaps it may have a verrucous surface (wart-like or shaggy appearance).
h. Is the lesion pedunculated (stalk-like) or is it sessile (flat or slightly raised)?
i. Is there pain, tingling, numbness, or any sensation associated with the lesion?
j. Does the lesion feel worse during chewing, biting, or swallowing?
k. Is there swelling associated with the lesion in this area of the mouth or lymph nodes? Checking the cervical lymph nodes, auricular, occipital nodes, and Virchow's node (left side in the clavicle area) are all a part of a total oral cancer exam.
l. Do you observe any stony, hard nodes?
m. Do you observe any soft, movable but enlarged nodes?
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and co-host of the International Oral Lichen Planus Support Group http://bcdwp.web.tamhsc.edu/iolpdallas and co-author of General and Oral Pathology for the Dental Hygienist. Her Web site for seminars is www.nancywburkhart.com.
Past RDH Issues