Meth Users
Survey pinpoints concerns dental professionals have about treating abusers of methamphetamines.
Crystal meth is a methamphetamine derived from its parent drug amphetamine. Amphetamine was used originally in nasal decongestants and bronchial inhalers. Crystal meth was first seen in South Korea and Taiwan. It came to the market as a legal appetite suppressant and was also used to treat attention-deficit hyperactivity disorder, narcolepsy, and depression. Today, it is a schedule II drug with a high abuse potential and limited medical use. It is available by prescription only and cannot be refilled. It is infrequently prescribed to temporarily address obesity.
Methamphetamine on the street, however, is most often culled up from underground labs, where the drug is cooked up in varying potencies and with differing purities. It usually appears as a white powder called crank, speed, crystal, candy, or tweek, or clear crystals usually called ice or crack. Meth is ingested by swallowing it, snorting it, or injecting it, all of which produce effects almost immediately.
A cheap, reliable, and available addiction
To obtain more information about methamphetamine use, I contacted a local recovery home. I conducted five interviews with men who were former meth addicts. All five men had used for at least 10 years and some closer to 20 years. These ex-addicts are desperately trying to regain control of their lives.
One man states proudly, “I’ve been clean now for 85 days. I’ve tried to stop before but always had a relapse every two weeks or so, but now, I’m on the winning side of a battle.”
Crystal meth tempts users with dramatic bursts of energy, talkativeness, and excitement. After ingesting meth, users immediately feel an intense rush, decreased appetite, decreased fatigue, boosts in alertness and confidence, and feelings of exhilaration or euphoria. Meth users don’t need sleep or food, and they can keep going on and on for hours on end.
The highs are so incredibly high, but the lows are so devastatingly low. Meth energy lasts six to eight hours, then slams the user into an exhausted, weak, drug-craving crash. This only leaves users wanting more. Meth is usually used in a binge/crash pattern. The average binge lasts three days before the user runs out of money or hook-ups and is forced into the painful crash.
Users choose meth because it is more widely available at lower prices than most other illicit drugs. It costs about one-fourth as much as cocaine and its high lasts 12 to 20 times as long. This drug of choice can also be easily manufactured with common household products. Methamphetamines are manufactured in laboratories everywhere. They are found at abandoned farms, country homes, and sometimes in the basements or bathtubs of homes in residential areas. Meth can be produced with readily available inexpensive materials such as over-the-counter cold medicine, fertilizer, battery acid, and hydrogen peroxide - making manufacturing impossible to control.
The telltale signs
Meth abusers can usually be detected by many telltale signs that ruin the abusers’ health. Many users compulsively repeat meaningless tasks for hours, or pick at imaginary bugs on their skin until it bleeds. Methamphetamine causes brain, heart, kidney, and liver damage among other physical effects. It quickly ruins a heavy user’s appearance. Lack of sleep and nutrition, as well as the effects of the toxic chemicals in the drug, ruin the complexion and waste away the body.
The body reacts to crystal meth the same way it reacts to danger. It floods the body with adrenaline, the same hormone that prepares it for emergencies. Adrenaline gives users a super-charge of strength and endurance. Meth gives users the ability to stay awake and do continuous activity with less need for sleep. Although users feel high and full of energy and their bodies keep going, a great deal of damage is being done to the body and brain.
Crystal meth first affects the central nervous system, including the brain. After using meth, a user’s nervous system is shifted into high gear. Neurotransmitters send “emergency alert” messages to the heart, the digestive system, the kidneys, the lungs, and the glands that make the body’s hormones. The eyes’ pupils enlarge, blood vessels constrict, and body temperature rises. Over time, stores of neurotransmitters become depleted, paranoia and anxiety become more frequent, and psychosis develops from too much dopamine, norepinephrine, and lack of sleep. Also, recent research has shown that long-term meth use destroys nerve cells in the brain that regulate dopamine, muscle movement, memory, and decision making. This damage can be widespread and permanent.
Crystal has many other effects on the body. Within the respiratory system, materials used to cut meth can block blood vessels in the lungs, and long-term use can permanently reduce the amount of air the lungs can take in. Within the circulatory system, meth causes the heart to beat faster and harder, veins and arteries to constrict, blood flow to reduce, and blood pressure to increase. The blood clots more readily to stop bleeding because the body thinks it might be hurt. Within the digestive system, meth stops or slows down the movement of the digestive tract. This slows down the breakdown of food and nutrients. Appetite and thirst decrease, causing concern for malnutrition, anorexia, weight loss, cramping, and dehydration.
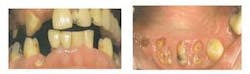
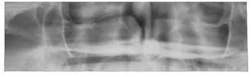
More clues inside the mouth
Some of the biggest telltale signs of meth users are not so well hidden inside of their mouths. Meth can cause serious problems in a user’s mouth. Meth users are not likely to brush and floss when they are high, and they only go to sleep and wake on average of every three days. Usually, when they are going to sleep they are so depressed they do not brush, so oral home care presents a major risk factor.
Crystal shrinks blood vessels, including the ones in the mouth - not enough blood nourishes the teeth and gums properly. With repeated shrinking, the vessels will not recover, thus causing dental tissue to starve and break down. The end result is tooth decay, gum disease, and bone loss.
Meth causes dry mouth, which leads to many problems. Some of the chemicals used to manufacture methamphetamine are caustic, meaning that they can burn the skin. These harmful chemicals will also come into contact with the soft tissue or mucosal lining of the oral cavity. Without saliva present to protect the oral tissues, severe inflammation, painful mouth sores, and ulcers can develop. Also, continuous friction between the tongue and the inside of the mouth, without saliva acting as a surfactant, can cause skin to become raw and irritated, which can lead to infection.
Without saliva, acids build up, lowering the pH of the mouth and causing the breakdown of the surface of the teeth. Meth users are notorious for trying to treat cottonmouth with lots of sugary soda, which only adds to the problem.
Feedback from dental peers about meth
There are currently no statistics on meth mouth, as the condition has come to be known, because addicts are reluctant to admit their drug use, but there are signs it is on the rise around the country.
In March 2005, I conducted telephone interviews with 150 dental professionals (75 dentists and 75 dental hygienists). They were all asked the same five questions: