Lupus Erythematosus
by Nancy Burkhart, RDH, EdD
Your patient is a 26-year-old woman, Mary Turner, who was just recently diagnosed with discoid lupus erythematosus (DLE). She has not been to a dental office in a few years, but is in your office today on the recommendation of her physician. Currently, she is using a topical corticosteroid cream for the skin lesions, and she is aware of some oral lesions. Mary is not taking any other medications.
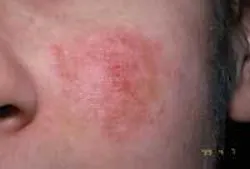
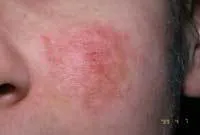
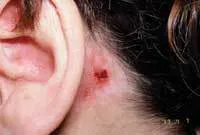
Extraoral exam: As you begin your extraoral exam, you notice that Mary has some obvious skin lesions. She has a reddened area that reaches from her nose across the malar process (malar rash) on both sides of the face. This is known as a “butterfly rash” and the name is derived from its “butterfly wing” shape (see Figure 1). As you continue your examination, you notice that Mary has an irritated area behind her right ear that appears to be a healing lesion and has probably been scratched (see Figure 2). Skin lesions occur with lupus in both the “discoid” and “systemic” forms. The “butterfly rash” is very characteristic of discoid lupus.
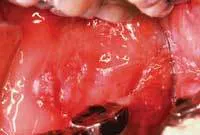
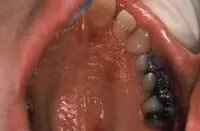
Intraoral exam: The mucosa appears ulcerated, very red and the patient complains of dryness and burning. The palate has some mixed red and white patches and some lesions even extend into the soft palate and tonsillar pillar region (see Figure 3 and Figure 4).
Diagnosis: Lupus erythematosus (DLE)
Etiology: Lupus erythematosus is an autoimmune disease that has a genetic component. In such conditions, there is a breakdown in the normal immune surveillance mechanisms leading to a loss of normal self-tolerance (Rubin, 2001). Consequently, as with most autoimmune type III hypersensitivity reactions, multiple organs may be affected because antibodies are formed against self-antigens. Viruses such as the Epstein-Barr virus, hormones, genetic predisposition, and certain medications have been suggested to contribute to onset of the disease.
Epidemiology: Lupus affects approximately 1,500,999 Americans in one of two forms of lupus. It occurs predominately in females in the 30 and over age range (90 percent). The Lupus Foundation of America (2007) estimates the disease is more common in African Americans, Latinos, Asians, and Native Americans, and the incidence is higher in Europe and Australia when compared to the United States.
Lupus is classified into two major groups and a diverse range of subtypes depending upon the severity:
• Discoid lupus erythematosus (chronic form DLE) accounts for 70 percent of the cases, and oral lesions are present in up to 30 percent of patients.
• Systemic lupus erythematosus (acute form of SLE) represents approximately 10 percent of cases. Drug induced lupus accounts for 10 percent of all cases and other autoimmune disease states such as scleroderma (a connective tissue disease) may be found in approximately 10 percent of all cases.
Pathogenesis: Discoid lupus affects the skin and oral membranes while systemic lupus may profoundly damage other major body organs. Lupus may affect all major organs in the body, including the skin, kidneys, and joints.
Oral tissues may be affected in any type of lupus with the buccal mucosa, gingiva, vermilion border, palate, and labial mucosa most affected. Other mucosal tissues may also be involved, including the nose and eyes. Salivary flow may be diminished and oral candidiasis is often a problem. Alopecia (hair loss) is common in patients with more severe manifestations. The skin may be photosensitive and patients are encouraged to avoid sun exposure. Additionally, patients with lupus may experience Raynaud phenomenon and arthritis is very common.
Dental implications: Vegetations on the heart valves (Libman-Sacks endocarditis) may occur and some authorities have suggested antibiotic pre-medication for invasive dental procedures. However, the American Heart Association (2007) has recently published new guidelines, and prophylactic antibiotic coverage for dental procedures is only recommended under specific circumstances, even in patients with systemic lupus.
Consequently, medical consultation is very important in management of patients with the systemic form of the disease. Mixed red and white lesions with or without ulcerations may occur on the oral mucosa, gingiva, and lips. The gingival tissue is often described as desquamative with a general description of soreness. When oral lesions are present without skin lesions, diagnosis may be delayed because of the difficulty in distinguishing oral lupus lesions from other entities such as lichen planus, pemphigoid, and pemphigus (Orteu, et al., 2001). After diagnosis of early lesions, the patient is usually treated with the same protocol as other mucosal diseases.
Differential diagnosis: Oral mucosal disease states that may have a similar appearance may include:
- Lichen planus
- Pemphigus
- Pemphigoid
Since both lichen planus and pemphigus may exhibit skin lesions as well, the diagnosis can only be made through biopsy and immunofluorescence. Blood test and systemic evaluations are needed to confirm a diagnosis of systemic lupus.
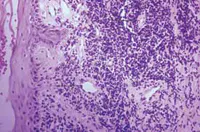
Microscopic features: Inflammatory infiltrations of lymphocytes are dispersed around blood vessels. Inflammatory cells are also found in the connective tissue and the basement membrane. Immunofluorescence testing is recommended since it is often difficult to differentiate lupus microscopically from other mucocutaneous diseases. Immunofluorescence test findings may be nonspecific, but they serve to rule out other disease entities and on occasion may be definitive (see Figure 5).
Treatment and prognosis: Patients with lupus may be on medications such as systemic steroids and other anti-inflammatory medications. Lupus is a chronic, progressive disease, and treatment is directed toward relief of symptoms with control of damage to the major organs. Controlling the inflammatory process is the main goal, with kidney damage and renal failure as a major concern.
In the dental office, patients with lupus are treated best with frequent recall visits, control of oral inflammation, and identifying trigger mechanisms. Dental treatment procedures should be performed as gently as possible in order to minimize tissue disruption. Hand scaling may be preferable to other techniques. Use of a soft-bristle toothbrush and mild dental products (toothpaste and mouthrinse) should be recommended.
Because of photosensitivity, the lips may exhibit scaling, dryness, and sometimes a white appearance. A lip balm with an SPF may be beneficial. Remember that patients with systemic lupus may be taking systemic steroids and/or other anti-inflammatory medications such as aspirin or NSAIDS. Consequently, these patients may be at risk of developing adrenal insufficiency and bleeding disorders. In these situations, medical consultation is extremely important before performing routine dental treatment procedures.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry and Texas A & M Health Science Center in Dallas. Nancy is also a co-host of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She is a co-author of General and Oral Pathology for Dental Hygienists, published by Lippincott Williams & Wilkins in Baltimore, which will be released in October 2007. She can be contacted at [email protected].
References
American Heart Association Guidelines available at Web site: DOI:10.1161/CIRCULATIONAHA.106.183095 with hard copy in Circulation 2007. Reprints available by calling (800) 242-8721 (United States only), Reprint #71-0407.
Lupus Foundation of America (www.lupus.org).
Orteu CH, Buchanan JA, Hutchinson I, Leigh IM, Bull RH. Systemic lupus erythematosus presenting with oral mucosal lesions: easily missed? Br J Dermatol. 2001 Jun; 144(6):1219-23.
Plemons, JM, Gonzales TS, Burkhart NW. Vesiculobullous diseases of the oral cavity. Periodontology 2000. 1999; 21:158-175.
Rubin, E. Essential Pathology. Third Edition. Lippincott Williams & Wilkins, Baltimore. 2001.
Regazi J, Sciubba J, Jordan R. Oral pathology-clinical pathologic corrections. 4th ed. St. Louis: WB Saunders, 2003.