State Spotlight on Utah: Direct access and the dental hygienist
Editor’s note: Join us for the final installment in our series highlighting direct access to dental hygiene services. Over the last year, we have journeyed across the country discovering the many types of nontraditional and independent roles dental hygienists can hold. Today, we turn the spotlight on Utah where recent legislation allows dental hygienists to provide direct services in collaboration with a dentist. To learn more about the ways in which dental hygienists are providing direct services in your area and throughout the country, visit the National Mobile Dentistry Conference website at nmdconference.com.
The American Dental Hygienists’ Association (ADHA) defines direct access as the ability of a dental hygienist to initiate treatment based on their assessment of a patient’s needs without the specific authorization of a dentist, treat the patient without the presence of a dentist, and maintain a provider-patient relationship.1
When was the last time you told your story?
There is power in telling a story. Some stories fill up our history books and many are passed down from generation to generation, becoming deeply embedded in our personal practices and community traditions. For as long as humans have existed, we have told stories in order to remember the past, understand the present, and shape the future.
Over the course of the last year, RDH magazine has invited me to help dental hygienists from across the country tell their stories about providing direct access to dental patients in previously unconsidered contexts. These stories were often filled with passion and sometimes pain, but most of all they demonstrated the incredible ability of dental hygienists to discover personal happiness and professional fulfillment beyond the walls of the traditional operatory. We hope that as you listen to the stories shared here in this series, you might be inspired to consider new ways to explore your own story—and courageously shape the future of your career.
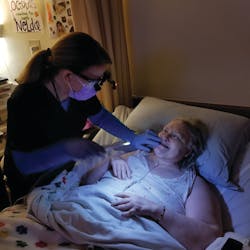
One of the most frequent questions dental hygienists ask me is if it is possible to provide direct care in their state, and if so, how can they get started. To help answer this question, let’s listen to Staci Stout, BSDH, RDH, (figure 1) tell the story in her own words of how she began her journey, inspiring many and becoming a pillar in Utah’s direct access movement.
What inspired you to begin a journey of providing direct access to care?
In 2014, I was nominated president-elect of the Utah Dental Hygienists’ Association (UDHA). That year, we prepared a bill to change the Utah Dentist and Dental Hygienist Practice Act to allow for direct access to dental hygiene services. Because we faced opposition from the dental association, we hired a lobbyist and started collaborating with other allies. During my presidency the next year, we were able to pass the legislation!
This new legislation allowed the dental hygienist to work under a collaborative agreement with a licensed Utah dentist. Thanks to this, I began a quest to educate our state’s professionals to help direct access become a reality for underserved communities.
In the fall of 2015, we offered our very first dental hygiene clinic in an elementary school—a pivotal moment for us! We treated 64 patients and provided dental hygiene assessments, oral health education, oral cancer screenings, periodontal care, and fluoride applications. More than half of the patients had untreated decay, 12% had urgent needs such as pain or active infection, and some had never seen a dentist before. This was a huge success and proved how integral our care was for the community.
At that point, I was invited to speak at the Utah Assisted Living Association’s annual conference and was subsequently approached by a facility that wanted me to set up an oral health program for its residents. It was then that I applied for and won my first grant, the ADHA Institute for Oral Health (IOH) Wrigley Company Foundation Community Service Grant. With this funding, I was able to provide oral health care to facility residents, educate the administration and staff on the importance of oral health, collect data to help improve access legislatively, and help dental hygienists learn to provide place-based care.
During that year, we provided care to 54 residents and found that 65% had untreated decay in addition to broken teeth, root fragments, periodontal infection, and tooth abscesses. Not surprisingly, almost 70% of the residents did not have regular access to an oral health-care provider due to mobility issues. At the close of the project, a dental hygienist was assigned to the assisted living residence to continue care. The bottom line is we now have strong evidence that this population, among others, is being neglected when it comes to oral health care.
In 2017, I was able to secure a second Wrigley grant to provide care in subsidized senior housing. We collaborated with Senior Charity Care Foundation and brought in dental hygienists from the UDHA to provide preventive care to 48 residents, supplementing the mobile restorative program already in place. Thanks to the success of these two programs, the Utah Department of Health approached me to collaborate with Senior Charity Care Foundation on a large grant to provide a year of preventive and restorative oral health care to 10 nursing homes and 600 residents.
That same year, I also created a school-based oral health program. To launch the program, we partnered with the school administration, the United Way community coordinator, and a dentist from a nearby dental assisting school. After agreeing to complete two pilot programs the first year, we then expanded into four elementary schools, a middle school, and a high school. In this program, dental hygienists provide preventive services to students, a dentist completes an exam via teledentistry, and we provide oral health education in the classroom. It is encouraging to know we will have an impact on these children for their entire school experience.
I’m excited to share my story and more about the logistics of our operations at the National Mobile Dentistry Conference. I am presenting with Dr. Tanner Clark on the relationships of collaborative practice and streamlining the mobile dental hygiene practice to increase efficiency and production.
Why is it important for dental hygienists to provide direct care to patients?
As an educator, I understand what is required of a dental hygiene graduate. Dental hygiene students learn necessary skills to provide place-based care, treat advanced periodontal disease, educate different patient populations, and handle a medically compromised patient. Sadly, after students become licensed, they are often underutilized and lose many of their best skills. I think it’s important for dental hygienists to have opportunities to use what they know in any setting they desire. It’s a win-win for the professional and for the populations that need the care.
Can you own a dental business?
How does reimbursement work?
The nursing home project reimburses our organization through a grant. The dentist and dental hygienists are paid a daily or hourly rate, and the grant pays for equipment and supplies. The school programs are reimbursed through both private and Medicaid insurance. The assisted living and subsidized senior housing project was reimbursed through a grant and is also fee-for-service.
How do you acquire patients?
In school settings, we send applications to the parents in back-to-school packets at the start of each year. In nursing home settings, the director of nursing or care coordinator invites the residents to participate. The resident, family, or legal guardian completes the necessary documents and consents prior to their first appointment. I have also advertised at senior expo events, state association meetings, and radio programs.
What three tools can you not live without?
My favorite things are my fold-up wagon, my portable Cavitron unit, and my portable dental chair (figure 3). My wagon helps me transport the heavy equipment to and from the clinic site, my Cavitron allows me to remove calculus and food debris to provide periodontal treatment, and my portable dental chair allows me to maintain best ergonomic practices to protect my body.
What obstacles have you faced in your journey?
Recently, we attempted to pass legislation to allow for direct reimbursement but ended up running out of time during the legislative session. We have also attempted to enact a “dental hygiene diagnosis” in our dental practice act, because a dental hygienist should be able diagnose periodontal conditions in order to formulate a treatment plan. Unfortunately, we received opposition from the dental association, fearing that the dental hygienist and dentist would contradict each other in their diagnoses.
What would you change about your current role, if anything?
I would like to find a way for the programs I work with to be self-sustaining. If the programs could access regular funding, it would benefit the patient, and the provider would have an incentive to provide care. Chasing grants and other types of funding is a full-time job and significantly detracts from the amount of patient care we can provide.
What individuals or organizations have supported you on this journey?
I have been mentored throughout my career by many amazing dental hygienists. In school, Joy Gall and Frances McConaughy were two of my professors who had a significant impact on my future path. Lori Brogna and Karol Aldrich have both been mentors in my career. Laura Green has been my right hand as I served as president of the UDHA, and Danyelle Evans and Brenda Armstrong have been a huge inspiration to me with their unwavering energy and commitment to our profession. There are so many others, and I wish I could name them all! Recently, I have been inspired by groups I’m involved in on Facebook, including I Heart Mobile Dentistry, Trapped in an Op, and the Dental Peeps Network.
What is your ultimate professional goal?
My ultimate goal is to have an oral health professional available in every school, senior community, long-term care facility, community health center, hospital/medical clinic, pediatric office, and anywhere else where there is need. Providing routine oral health education and preventive care will make a positive impact in the health of our communities. I also want to continue to empower dental hygienists to seek out opportunities to provide care in alternative settings. Dental hygienists deserve a voice in how and where they practice. My passion is to help make that happen!Where do you think you will be in 10 years?
Good question! I would like to see school-based programs (figure 4) expanded across my state and initiated in other areas of the nation. I would also like to see senior communities and other facilities have a fixed, in-house dental hygienist. To make that happen, I see myself working with hygienists and organizations locally, nationally, and internationally to implement place-based oral health care by utilizing telehealth communication, streamlined processes, and to create an empowered team.
What advice would you give to someone who wants to begin a similar journey?
Networking and collaboration with colleagues as well as local and national leaders will open many doors. Connect with those in your community and with those who are on similar paths. I have learned so much from clinical volunteer experiences both at home and in Africa and Haiti.
Summary of direct access2,3
Title: Possible via two different pathways:
- Public health dental hygienist
- General supervision
Setting limitations:
- Public health dental hygienist—Includes homebound patients, schools, nursing homes, assisted living facilities, community health centers, federally qualified health centers, mobile dental clinics
- General supervision—Not specified
Patient population limitations:
- Collaborative practice authorization—Not specified
- General supervision—Patients of record
Scope of practice limitations:
- Collaborative practice authorization—Local anesthesia and nitrous oxide inhalation permitted under indirect supervision only
- General supervision—Not specified
Written collaborative agreement needed?
- Collaborative practice authorization—Yes
- General supervision—No, though procedures must be authorized by the supervising dentist and the dentist must be available for consultation
In-person evaluation by a dentist required?
- Collaborative practice authorization—Dentist must have examined the patient within the preceding six months prior to receiving dental hygiene services
- General supervision—Not specified
Dental hygiene diagnosis defined? No
Prescriptive authority? No
Supervision of dental assistants permitted? Yes
Direct reimbursement allowable? No
Minimal clinical hours or additional courses required?
- Collaborative practice authorization—None
- General supervision—None
Editor’s note: You may contact Staci Stout, BSDH, RDH, by email at [email protected], or visit these websites: smartsmiles.dental, seniorsmiles.dental, and prosmiles.dental.
References
1. Direct access states. American Dental Hygienists’ Association website. https://www.adha.org/resources-docs/7513_Direct_Access_to_Care_from_DH.pdf. Updated January 2020.
2. Dentist and Dental Hygienist Practice Act. Title 58, Chapter 69. https://dopl.utah.gov/laws/58-69.pdf. Published 1953. Updated May 14, 2013.
3. Variation in dental hygiene scope of practice by state. Oral Health Workforce Research Center website. http://www.oralhealthworkforce.org/resources/variation-in-dental-hygiene-scope-of-practice-by-state/. Published 2015. Updated January 2019.
About the Author

Melissa Turner, BASDH, RDHEP, EFDA
Melissa K. Turner, BASDH, RDHEP, EFDA, was honored as a 2024 Marquis Who's Who in America recipient. She is Senior Executive Consultant at Cellerant Consulting Group and spearheads the Cellerant Best of Class Hygiene Awards. She is a founding board member of the American Mobile & Teledentistry Alliance, cochair of the Oral Health Prevention Summit, and serves on the executive board of the Dental AI Association. Known as @thetoothgirl, she is the cofounder of The Denobi Awards and the National Mobile & Teledentistry Conference.