Breaking it down
This focus on the hygiene appointment centers on the patient introduction and chief complaint, vitals, radiographs, intraoral cameras, and caries detection.
by Lisa Dowst-Mayo, RDH, BSDH
The "practice management" for the dental hygiene appointments frequently or always involve these steps:
- Patient introduction
- Chief complaint
- Vitals, based on current AHA guidelines
- Radiographs, based on ADA recommedations
- Intraoral camera use
- Laser caries detection
Your personal introduction can set the tone for your entire patient appointment. I like to walk out to the waiting room empty-handed (i.e., no chart in my hand), greet my patient by name, shake his or her hand and give him or her a huge smile. I have noticed that a simple smile goes a long way to help break the tension and anxiety a patient may be feeling and also makes my patient feel welcome and appreciated.
According to the Diagnostic and Statistical Manual of Mental Disorders (DSM), 5-15% of the American population is diagnosed with "dentophobia." This is a disorder of extreme anxiety that causes people to completely avoid the dentist. Aside from this extreme diagnosis, there are many patients with differing degrees of anxiety associated with a dental visit. A smile can be a small thing for us, but it can be a huge thing for someone who is anxious in the dental office, especially for a patient who is crying as he or she simply opens the door to the office!
-------------------------------------------------
Other articles by Dowst-Mayo
- Dental practice offers skin services too in spa setting
- EXPECTATIONS OF WAGES
- Dental hygiene lasers: Why you should use lasers
-------------------------------------------------
A nice "Ritz-Carlton" trick is to greet your patients by name even if you have never met them before. For anyone who has ever been lucky enough to stay at the Ritz-Carlton hotel chain, you know what I am talking about. The hotel chain has an employee standing curbside to open your door when you pull up. The employee greets you by name, shakes your hand, and thanks you for your stay at the Ritz Carlton. I have often wondered how the employees of this grand hotel execute this customer service trick so successfully. They make each patron of the hotel feel very important and prestigious. In a small dental office, this trick is very simple to pull off; all you have to do is discreetly check with the front desk to see which patient is yours if you are unsure, then greet your patient by name and shake their hand.. It seems like such a simple thing, but it really goes a long way with patients; they will be impressed that you took the initiative to know who they are, and that gesture makes them feel like VIP clients.
I suggest avoiding "cattle-calling" at all times. "Cattle-calling" is the term consultants use to refer to the practice of reading a name off a chart, standing at the door to the waiting room, and never making eye contact with the patient. It's the "follow me" response from clinicians. This technique is not very social or polite and does not make the patient feel wanted or important to you.
CHIEF COMPLAINT
This can be a tricky conversation for hygienists because some patients like to talk a lot and would ramble on for hours if you let them. They would tell you about each and every dental experience they have had since they were three years old if you don't learn to shut that tendency down politely. With that said, this really is one of the most important components to a hygiene visit. By acknowledging your patient's chief complaint and letting him or her know how important their concern is to you, he or she will feel heard and valued in the practice.
There are a few key components to obtaining a chief complaint successfully that can make or break this portion of an appointment. One is utilizing active listening and the other is staying the captain of the ship and keeping control of the conversation. You need to ask the questions and not let the patient ramble on or get off on a tangent that doesn't really pertain to their chief complaint. This can be tricky because you have to find a way to take control, all the while making patients feel heard and reassuring them that their needs are important to you. It's a kind of song and dance you will need to master or your schedule can become quickly derailed. I promise, the longer you do this job, the better you will get at this technique.
Here's a trick I use frequently: When I have patients who have relayed their chief complaints but seem to be veering off track with their dental stories, I will stand up and start getting my X-ray equipment ready in the room -- all while still actively listening and making eye contact with them. I have found this is a good nonverbal way of letting patients know I have other things I need to do. Most of the time when I position the X-ray sensor by their mouths with my gloves on, patients will say, "I better be quiet so you can get to your job, right?" I internally scream "YES" but externally say, "That's probably a good idea so we can get to looking at this tooth that is bothering you."
VITALS
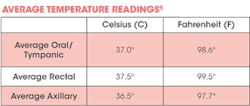
Vitals include temperature, respirations, pulse, and blood pressure.
Temperature -- Factors that can alter body temperature from normal ranges include exercise, beverages, food, smoking, environmental temperature, pathologic state, infection, dehydration, hyperthyroidism, myocardial infarction, starvation, hemorrhage, physiologic shock, or time of day.5 The highest temperatures will occur in the high afternoon and early evening; the lowest will occur during the early morning and during sleep.5,8 Common locations for measuring temperature in the dental office are orally (under the tongue), on the forehead, or in the inner ear. Hospitals may use the axilla (the armpit) or rectum.
Respirations -- It is advised that you measure patients' respirations over a one-minute period. Do not let them be aware that you are assessing their breathing; this may alter how they normally breathe in and out or it may prompt them to hold their breath. One complete respiration is defined as one breath in and completely out. Increased respiration can be caused by, but is not limited to: work, exercise, excitement, nervousness, strong emotions, pain, hemorrhage, and shock.5,8 Decreased respiration can be caused by, but is not limited to: sleep, certain drugs, or pulmonary insufficiency.5,8
A subnormal reading for an adult is ≤ 12 respirations per minute; ≥ 28 is accelerated; and ≥ 60 is considered extremely rapid and dangerous.
Pulse -- There is no absolute normal pulse rate. Tachycardia is an abnormally elevated heart rate (>110 beats per minute) and bradycardia is an abnormally slow heart rate (<60 BPM). Increased pulse can be caused by, but is not limited to: exercise, strong emotions, stimulants, extremes in heat/cold, eating, or heart disease.5,8 Decreased pulse can be caused by, but is not limited to: sleep, depressants, fasting, quieting emotions, or low vitality from prolonged illness.5,8 In the dental office, it is recommended to determine patients' pulse rate by palpating their radial pulse over a one-minute period.Sites for measurement include:
1. Radial pulse: wrist
2. Temporal artery: on the side of the head in front of the ear
3. Facial artery: at the border of the mandible
4. Carotid pulse: used during cardiopulmonary resuscitation
5. Brachial pulse: used for an infant
Blood Pressure -- Different states govern how often and at what age a dental provider should obtain a blood pressure. Refer to your individual state board for questions regarding blood pressure frequency and age recommendations. Factors that can affect blood pressure can include, but are not limited to: age, race, systemic diseases, weight, pain, tobacco, alcohol, caffeine, gender, exercise, stress, diet, time of day, oral contraceptives, or medications.5,8 The American Heart Association reports the following information on blood pressure:
X-RAYS
In 2012, the American Dental Association Council on Scientific Affairs published "Dental Radiographic Examinations: Recommendations for Patient Selection and Limiting Radiation Exposure" policy. It can be accessed online at www.ada.org.
The tables prepared for the ADA's radiographic recommendations cover a variety of situations, ranging from the new patient to the recall patient. In the ADA's report, they also state, "Recommendations are subject to clinical judgment and may not apply to every patient. They are to be used by dentists only after reviewing the patient's health history and completing a clinical examination."
INTRAORAL CAMERA (IOC) PICTURES
This part of an appointment is not done in all offices; however, with the digital age upon us, many offices are starting to incorporate intraoral camera use. The phrase "a picture is worth a thousand words" means a lot in dentistry. IOC pictures can aid in patient acceptance and understanding of treatment recommendations as well as insurance claims. When a dentist can provide a picture of a decayed tooth, it becomes harder for an insurance company to argue that a filling or a crown was not indicated.
Many offices now take what is referred to as "smile pictures" of their patients. These pictures normally consist of occlusal arch pictures, cheek-retracted open bites, closed bites, and side bites. This can aid in discussions involving orthodontic needs and relating malocclusion to the overall health of the dentition.
There are many intraoral cameras on the market today for taking individual tooth pictures; some offices are even using iPhones or iPods to take pictures. These pictures are fantastic for demonstrating fractures, decay, and chipped fillings for the patient. Many doctors report increased treatment plan acceptance when they started incorporating photography into their practices. As the doctor I used to work for in private practice (Dr.Tiffini Stratton, DDS) before I became a full-time educator says: "When a patient can see their decay or fracture, they can now take ownership of it. It's not me telling them what they need; it's them seeing it for themselves. It puts the dental issue back in the hands of the patient."
Intraoral photography can also add a unique touch with patients. Many of my patients compliment the technology in my office and feel very secure with the doctor's diagnosis. It adds a bit of "Ritz-Carlton" care to my appointments by offering something that is novel and different to patients without charging them for the service – like when the Ritz puts a chocolate on your pillow or fresh flowers in a vase in your room. It's the extra bit of flare that separates the ordinary hotel chains from the extraordinary, or the ordinary dental office from the exceptional.
LASER CARIES DETECTION
For an office looking to expand its technology and add a unique piece to its armamentarium, laser caries detection may be a good fit. I educate my patients on our laser caries detection like this: "Instead of poking at the grooves of your teeth with a sharp, pointy instrument, our office utilizes a piece of advanced technology called the DIAGNOdent. It is a diode laser designed to pick up the fluorescence (or presence) of bacteria in the grooves and fissures of your teeth. It can assist the doctor in determining whether or not your tooth has a cavity developing. It helps us catch cavities when they are small, even too small to show up on a radiograph yet, and allows us to perform more conservative dentistry." This can be another "Ritz-Carlton" service for patients. They are always impressed by our office's use of technology and many times have been grateful that I am not using "the pointy thing" they don't like or are scared of!
There are a couple of products on the market for caries detection through fluorescent laser technology. The two I have experience with are Kavo's DIAGNOdent and Dentsply's MidwestCaries ID. They have different features but can both help assist the clinician with identifying what may be occurring inside grooves, pits, and fissures of teeth. These products do NOT diagnose decay; a doctor diagnoses decay through visual, tactile, or radiographic assessment. This piece of equipment can be a nice adjunctive aid for doctors who wish to utilize it. According to Kavo's website, "altered tooth substances and bacteria fluoresce when they are exposed to a specific wavelength of light." In summary, when a tooth has a carious lesion, it will exhibit fluorescence against a 655 nm diode wavelength and will register a reading of abnormal on the DIAGNOdent. The Midwest Caries ID has a nice feature of changing colors and sound in response to abnormal findings. You can find more information on both these products at www.kavousa.com or www.professional.dentsply.com.
Don't forget to offer your "Ritz-Carlton" patient care and experience!
Lisa Dowst-Mayo, RDH, BSDH, graduated magna cum laude from the Caruth School of Dental Hygiene at Baylor College of Dentistry in 2002 with a bachelor's degree in dental hygiene. She has held numerous leadership roles in the tripartite of the American/Texas/Dallas Dental Hygiene Associations. She is an author, clinician, educator, and enthusiastic public speaker. Lisa is a dental hygiene instructor at Concorde Career College in San Antonio, Texas. She is a cofounder of the company Diamond Dental Education that provides CE courses for dental professionals in Texas. She can be contacted through her website: www.lisamayordh.com.
References
1. AAP. "Parameter on Periodontal Maintenance." J Periodontol. 2000;71:849-850.
2. AAP. "Parameter on Comprehensive Periodontal Examination." J Periodontol. 2000;71:847-848.
3. Calley K, Hodges K. "Automate Your Probing Process." Dimensions of Dental Hygiene. Feb 2011;73:2686-2688.
4. Cleveland J, Junger M, Saraiya M, Markowitz L, Dunne E, Epstein J. The connection between human papillomavirus and oropharyngeal squamous cell carcinomas in the United States. Implications for Dentistry. JADA. August 2011;142(8):915-924.
5. Darby M, Walsh M. "Dental Hygiene: Theory and Practice." 3rd ed. St. Louis, MO: Saunders Elsevier, 2010.
6. Huff K, Stark P, Solomon S. "Sensitivity of Direct Tissue Fluorescence Visualization in Screening for Oral Premalignant Lesions in the General Practice." Gen Dent. Mar-Apr 2010;58(2):126-9.
7. Messadi D. "Diagnostic Aids for Detection of Oral Precancerous Lesions." Int. J. Oral Sci. June 2013;5(2):59-65.
8. Wilkins E. "Clinical Practice of the Dental Hygienist." 11th ed. Philadelphia, PA: Lippincott, Williams and Wilkins, 2013.