Case #4
by Joen Iannucci Haring
A 60-year-old male visited a dentist for an initial exam and routine checkup. Oral examination revealed a gingival lesion between the lower canine and first premolar.
History
The patient first noticed this gingival growth approximately one year earlier. When questioned about any change in size, color, or texture of the lesion, the patient stated that he was not aware of any such changes. No history of trauma to the affected area was reported by the patient. The patient denied any pain or discomfort associated with the lesion.
At the time of the dental appointment, the patient appeared to be in an overall good state of health. The patient's medical history was reviewed and included no significant positive findings. The patient's past dental history included regular dental examinations and routine dental treatment. The patient's last dental appointment was two years earlier for a dental prophylaxis.
Examinations
Physical examination of the head and neck areas revealed no enlarged or palpable lymph nodes. The patient's vital signs were all found to be within normal limits. No significant extraoral findings were noted.
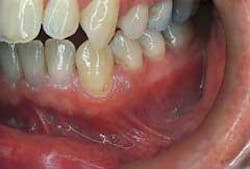
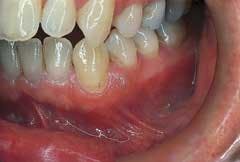
Intraoral examination revealed an elevated pinkish-translucent swelling on the attached gingiva between teeth #21 and #22 (see photo). The lesion appeared as a broad-based, compressible growth and measured approximately 0.5 centimeters in diameter. A smooth surface texture without ulceration or hemorrhage was noted. The teeth adjacent to the lesion were pulp tested for vitality and both teeth tested vital. Further examination of the oral soft tissues revealed no other masses present.
The patient was referred to an oral surgeon for an excisional biopsy. Histologic examination of the tissue revealed a cyst lining consisting of flattened epithelial cells and a connective tissue wall that exhibited rests of dental lamina.
Clinical diagnosis
Based on the appearance of the lesion and the information presented, which of the following is the most likely diagnosis?
o mucocele
o lateral periodontal cyst
o peripheral ossifying fibroma
o parulis
o gingival cyst of the adult
Diagnosis
• gingival cyst of the adult
Discussion
The gingival cyst is a cyst of odontogenic origin. (The term odontogenic means arising in tissues that give origin to teeth.) The gingival cyst of the adult is developmental and arises from remnants of the dental lamina. Of all the odontogenic cysts that exist, the gingival cyst is considered to be uncommon.
Clinical features
The gingival cyst of the adult is most often seen in individuals in the fifth and sixth decades of life. There is no sex predilection. The gingival cyst typically appears as a small, well-circumscribed swelling with a smooth surface texture. The lesion is broad-based. The color may be pale pink, translucent, or bluish. The gingival cyst is a slow-growing lesion and usually measures less than 0.5 centimeters in diameter. When palpated, the gingival cyst feels compressible. This lesion is asymptomatic.
The gingival cyst, as the name suggests, is found on the gingiva; the attached gingiva, free gingival margin, or interdental papilla areas may be involved. The gingiva of the mandible is involved more often than the maxilla, and the facial gingiva is more frequently involved than the lingual areas. In 60 to 75 percent of cases, the mandibular canine-premolar region is the area most often involved.
The gingival cyst of the adult is the extraosseous (occurring outside of bone) counterpart of the lateral periodontal cyst. The lateral periodontal cyst occurs within bone and has histologic features identical to the gingival cyst. The gingival cyst and the lateral periodontal cyst also share a common histogenesis, as well as similar age predilection and location.
Diagnosis and treatment
Based on the clinical appearance of the gingival cyst, there are several lesions that may be considered in the differential diagnosis. The gingival cyst may resemble a mucocele, a peripheral ossifying fibroma, or a parulis. A biopsy and histologic examination of the tissue is necessary in order to establish a definitive diagnosis.
Histologically, the gingival cyst of the adult exhibits a thin, stratified epithelial cyst lining and a fibrous connective tissue wall that exhibits remnants of the dental lamina. No inflammation is seen in the connective tissue wall.
The gingival cyst does not spontaneously disappear or regress with time. As with all odontogenic cysts, the gingival cyst must be removed. The treatment of choice is surgical excision. Following removal, this lesion should not recur.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.