Pleomorphic adenoma
by Nancy W. Burkhart, RDH, EdD
[email protected]
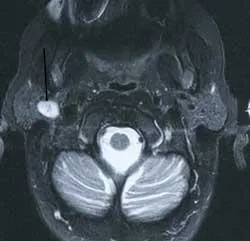
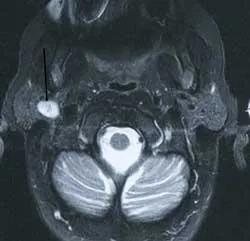
Britta is your patient today and she has been a patient of record in your practice for a number of years. Recently, Britta had an automobile accident. During the accident, she hit her head on the steering wheel of the car. It was suggested during treatment at the emergency room that she have a scan of her head to be certain there was no unseen injury. The scan showed no evidence of damage from the automobile accident but did reveal that she had a tumor in the parotid area. At a later date, the tumor was diagnosed through biopsy as a pleomorphic adenoma (see Figure 1).
Epidemiology: The pleomorphic adenoma is the most common benign salivary gland tumor, accounting for 53 to 57% of parotid tumors and 44 to 68% of submandibular tumors. It is followed by the second most common benign salivary gland tumor, Warthin's tumor. Pleomorphic adenoma tumors occur in the major salivary glands of the parotid and the submandibular region. These tumors may also be found in the palate, affecting minor salivary glands. In order of frequency, the parotid gland is followed by the submandibular gland and finally the minor salivary glands.
A slight female predilection is noted and usually occurs in the 30 to 50 year–old age group. However, all age groups may be affected.
Etiology: The pleomorphic adenoma is a slow–growing, non–ulcerative benign neoplasm that arises from the proliferation of glandular epithelium and myoepithelial cells. Some evidence exists indicating that there may be alterations of the chromosome 8 in the development of this tumor as well.
Clinical features: Typically, these tumors arise as firm masses that are slightly compressible. They appear more firm when found in the palate. Evidence exists of transformation in some cases to carcinoma (termed carcinoma ex–mixed tumor). The tumor is encapsulated and some cells have been found to be neoplastic and extend through the capsule, increasing the risk of recurrence.
The term “pleomorphic” is used to describe the highly variable microscopic appearance of this tumor. Originally, “benign mixed tumor” was used to describe the mixed nature of the tumor, which may include metaplastic cartilage, fat, bone, etc., in addition to the glandular epithelial component. However, the tumor is not truly arising from two different germ layers, as the term “mixed” might imply. The term “mixed tumor” is still used by some pathologists and dental educators and is often interchanged with pleomorphic adenoma by many. The majority appear to prefer pleomorphic adenoma because of the lack of clarity regarding the origin when using benign mixed tumor (see Figure 2).
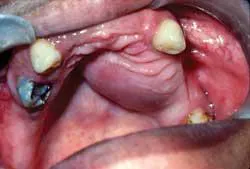
Perioral and intraoral characteristics: Clinically, the pleomorphic adenoma will manifest as a slow–growing, painless, mobile mass when found in the lower lobe of the parotid gland. Swelling in the area of the angle of the mandible may be noticed clinically by the patient. The tumor may also be found in the palate and in this location, the growth appears as a bulbous, nonulcerated, firm lesion.
Significant microscopic characteristics: The tumor is encapsulated by thick connective tissue, but portions may also extend into salivary tissue. This contributes to unclear margins during biopsy and difficulty in removal of the entire tumor. The tumors may have varying histological appearances consisting of ductal and myoepithelial cells in various stages of development and this fact alone makes a diagnosis very difficult in some cases due to limited or selected tissue samples. Batrani et al. presented a case where there was misinterpretation in diagnosis of a mucoepidermoid carcinoma in a 16–year–old female.
Differential diagnosis: Other tumors that are often considered are myofibroma, lymphoma, mucoepidermoid carcinoma, metastatic disease, leiomyoma, schwannoma, adenocarcinomas, and lipoma. Ewings sarcoma and osteosarcoma might be considerations in the palatal region as well, but are very rare. Malignant salivary tumors should always be considered as well.
Treatment and prognosis: Complete removal of the tumor is the main objective with minimal disruption to the facial structures and nerves. A superficial parotidectomy, removing the lobe of the gland containing the tumor is performed. When occurring in the palate, some bone may need to be removed along with the actual tumor.
When the pleomorphic adenoma is found in the parotid gland, facial nerve involvement is a consideration and the parotid gland may need to be partially removed. The facial nerve is identified and the branches located in order to decrease the likelihood of damaging them when removing the tumor. Because of the rate of recurrence, patients should be monitored and followed closely. Xerostomia may or may not be a problem for the patient depending upon the extent of salivary gland tissue that has to be removed or altered. As with all xerostomia, discomfort from dryness and increased risk of caries are considerations.
References
Batrani M, Kaushai M, Sen AK, Yadav R, Chaturvedi NK. Pleomorphic adenoma with squamous and appendageal metaplasia mimicking mucoepidermoid carcinoma on cytology. Cytojournal 2008 Feb 12;6:5.
Delong L, Burkhart N. General and Oral Pathology for the Dental Hygienist. Lippincott Williams & Wilkins. Baltimore. 2008.
Guo SP, Cheuk W, Chan JK. Pleomorphic Adenoma with Mucinous and Squamous Differentiation: A Mimicker of Mucoepidermoid Carcinoma. Int J Surg Pathol. 2009 May 14th.
Orzechowska–Wylegata B, Jedrzejewski P, Wylegata E, Steplewska K. Recurrent benign pleomorphic adenoma of the lacrimal gland — a case report.
Thorac A. Cardiovasc Surg. 2009 Feb;15(1):42–5.
Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. WB Saunders Company, Philadelphia. 1995.
Taylor TR, Cozens NJ, Robinson I. Warthin's tumor: a retrospective case series. Br J Radiol. 2009 May 11.
Yim YM, Yoon JW, Seo JW, Kwon H, Jung SN. Pleomorphic adenoma in the auricle. J Craniofac Surg 2009 May;20(3):951–2.
Tobon–Arroyave S, Florez–Moreno G, Jaramillo–C´ardenas J, Arango–Uribe J, Isaza–Guzman D, Rendon–Henao J, Expression of hMLH1and hMSH2 proteins in pleomorphic adenoma of minor salivary glands: Relationship with clinical and histologic findings. POPCAD Research Group. Oral Surg Oral Med Oral Pathol Oral Radiol and Endod 2009; 108:227–236.
About the Author
Nancy Burkhart, RDH, EdD, is an adjunct associate professor at Baylor College of Dentistry. She is a co–host of the International Oral Lichen Planus Support and co–author of General and Oral Pathology for the Dental Hygienist.