Local Confidence: Regain that confident feeling about anesthesia
by Laura J. Webb, CDA, RDH, MS
Dental hygienists who do not have regular opportunities to provide local anesthesia may lose confidence in their abilities, which can result in avoiding the use of local anesthesia in treatment planning. This, of course, leads to fewer opportunities to refine technique. Since the provision of local anesthesia is an important service for our patients, we need to remain current and confident in its administration. We can maintain confidence and competence by following these simple steps:
Review the anatomy
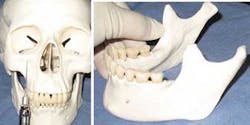
Pull out that old skull from hygiene school. If you don't own one, consider buying one (Figure 1a). This is essential for hands–on learners. I bought my first one a few years ago when I began making my own images for CE courses. I always have one on–site for participants to work with. The anatomically correct, 3–D skull is far more advantageous for feeling and seeing anatomy and practicing angulation than looking at pictures. Decent skulls can be purchased for about $100. When I ordered mine, I wrote to the company and explained that I required a skull that accurately reflected the maxillary and mandibular landmarks (lingula, mandibular foramen, inner ridge, mental foramen, infraorbital foramen, anterior palatine foramen, nasal palatine foramen, etc.) and a removable mandible (Figure 1b). Color–coding and labeling was not important to me. What the company recommended was exactly what I needed.
Review product updates
Several new products are available that improve operator (and patient) comfort during administration of local anesthetics. In addition, not all products are created equal, so it is important to familiarize yourself with those products that make administration of local anesthesia reliable and comfortable for both the operator and patient.
New syringes
Ask your dental products distributor representative to show you some of the great, new, lightweight, smaller syringes that improve tactile feel and control. The smaller, oval–shaped thumb rings reduce excess gap to make aspiration easier. Septodont USA has developed three lightweight syringes — standard, fusion–size (midsize), and petite (Figure 2a). The needle adapters are machined into the steel barrels to eliminate loosening, and the cartridge "window" extends the length of the barrel. Miltex has developed a Hi–Light Petite Syringe (Figure 2b) with smaller wings and an oval thumb ring. Because I have small hands, I was not comfortable with the "winged" style syringes until I tried these newer models. What a difference! Be aware that some of the smallest syringes do not allow for full expulsion of the cartridge, but less than a stopperful remains.
Cartridges
Cartridges vary, so use quality products. Some stoppers do not allow for easy engagement of the harpoon and can stick to the glass, requiring quite a bit of pressure that may result in loss of control.
Needles
Needles with metal hubs must screw down tight to avoid loosening, and often the bevel or syringe window is out of position. Plastic hubs adapt well to most syringes, and also to those that are stripped or have defects. They are easy to rotate for aligning the bevel and are less likely to remove the syringe hub. The literature supports the use of 25 gauge and 27 gauge needles to ensure less deflection, lower needle breakage, and more reliable blood aspiration than 30 gauge needles.2,5 For many years, studies have shown that patients are unable to perceive a difference in comfort between 25 gauge and 30 gauge needles.2,5
Investigate anesthetic agents
It is important to keep current on local anesthetic agents and maximum recommended doses (both manufacturers' recommendations and review of the literature for experts' recommendations). Agent selection for nonsurgical periodontal therapy procedures should be based on length and type of procedure, the patient profile, and the need for hemostasis. Lidocaine remains the "gold standard" in the U.S., with articaine gaining popularity due to its rapid onset, quick diffusion through tissue resulting in profound anesthesia, the availability of a 1:200,000 epinephrine formulation, and its faster rate of biotransformation. Several recently published studies discuss the advantages and safety of articaine.3,4,6,7,8,9
Four percent prilocaine plain is useful for those rare patients who present with absolute contraindication to vasoconstrictors because it is the only nonvasoconstrictor, intermediate acting (with block anesthesia), local dental anesthetic available in the U.S.1,2,5,6
Assess personal techniques
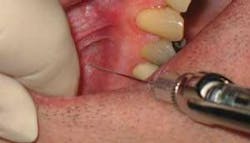
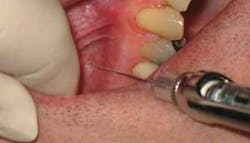
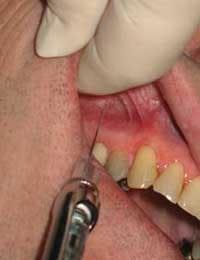
Regularly assess your injection techniques and practice on the typodont/skull if you do not have the opportunity to give injections regularly. Common clinical errors include insufficient retraction (Figure 3, photo courtesy of LJW Education Services), poor lighting, improper angulation, needle movement at target, premature/rapid deposition, poor thumb position for aspiration, needle movement during aspiration, and weak fulcrum.
Take a formal course annually
Local anesthesia update courses are available in a variety of formats (online, DVD, and traditional lecture, some with hands–on components) and can be helpful in providing important new information and assisting with rectifying common errors. The opportunity to discuss techniques and practice them with colleagues is priceless.
Rehearse before injecting
Before giving an injection to a patient, you should visualize the anatomy and each step of the process and then proceed with the injection, reiterating the steps (silently) as you proceed. This is the method used to teach students, and the way many successful clinicians implement techniques. Take your time during administration. Proper preparation and careful attention to technique contribute to safe and successful administration.
Thirty years ago I began providing local anesthesia to my patients. Now I can't imagine practicing without it. Through the years colleagues have remarked it was the one skill that challenged them the most due to infrequent use. I have learned through teaching and working in private practice settings that even the most experienced clinicians should take time to frequently reassess their skills and stay current with armamentarium and techniques. The provision of local anesthesia for patients is not difficult, but it does require maintenance of skill and evidence–based practice.
References
- American Dental Association 2008 (Poster) Pain Control in Dental Care.
- Darby M, Walsh M. 2003 Dental Hygiene Theory and Practice 2nd ed. Saunders.
- Haase A, Reader A, Nusstein J, Beck M, Drum M. Comparing anesthetic efficacy of articaine versus lidocaine as a supplemental buccal infiltration of the mandibular first molar after an inferior alveolar nerve block. JADA, Vol 139 Sept. 2008: 1080–1093.
- Hersh E, Giannakopoulos H, Levin L, et al, The pharmacokinetics and cardiovascular effects of high–dose articaine with 1:100,000 and 1:200,000 epinephrine. JADA Vol 1337 Nov 2006: 1562–1571.
- Malamed S. 2004 Handbook of Local Anesthesia 5th ed Elsevier.
- Malamed S. Local Anesthetics: Dentistry's Most Important Drugs, Clinical Update 2006. CDA Journal Vol 34 (12) December 2006: 971–976.
- Moore P, Boynes S, Hersh E, et al. The anesthetic efficacy of 4% articaine 1:200,000 epinephrine. JADA Vol 137 Nov 2006:1572–1581.
- Pogrel MA. Permanent Nerve Damage from Inferior Alveolar Nerve Blocks; CDA Journal, 35 (4) April 2007: 271–273.
- Wynn R, Bergman S, Meiller T. Paresthesia associated with local anesthetics: A perspective on articaine. Pharmacology Today Nov–Dec 2003.
About the Author
Laura J. Webb, CDA, RDH, MS, is an experienced clinician and educator who owns LJW Education Services (www.ljweduserv.com). She provides educational methodology courses and accreditation consulting services for DH/DA education programs and CE courses for professionals. Laura frequently speaks on the topics of local anesthesia and nonsurgical periodontal instrumentation.