Do you remember the glands of Blandin and Nuhn?
Anna is your patient today. She is home for the summer after her first year of college. Her visit is for a maintenance appointment, but she tells you that she has noticed a growth on her ventral tongue for several years now and has become concerned because the growth has gotten larger within the past several months. She often traumatizes the growth while eating and has noticed that it appears much more irritated than when she first noticed the tissue change.
She has taken several images using her cell phone and shows you the appearance of the growth four months ago. You agree that it has grown significantly since the image on her phone was made.
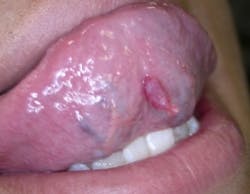
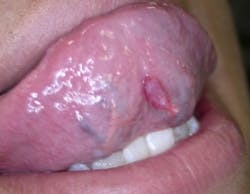
As you examine the lesion, you note that it is soft, exophytic, somewhat moveable, a slightly blue/red hue, somewhat irritated but painless. You do not detect any exudate (see Figure 1).
Is this a mucocele? Mucoceles are quite common lesions of the oral mucosa and originate from the rupture of a salivary duct and extravasation of the mucin into the surrounding tissues. Mucoceles occur in most areas of the mouth, including the floor of the mouth. But do they occur on the ventral surface of the tongue? Three areas are relevant with regard to the tongue, and the tongue does contain salivary gland tissue.
The three salivary glands of the tongue:
• The glands of Weber along the border of the lateral tongue — These glands are pure mucous secreting glands. These open into the crypts of the lingual tonsils on the posterior tongue dorsum.
• The glands of von Ebner surrounding the circumvallated papillae — These glands drain by means of small ducts into the base of the cleft between the foliate papillae. These are pure serous glands.
• The glands of Blandin and Nuhn embedded in the musculature of the anterior ventral tongue. These glands are mixed mucous and serous glands. The glands drain by means of five to six small ducts that open near the lingual frenum in the location of the fringed fold known as the plica fimbriata.
The growth presented here originates from the mixed mucous and serous glands that are embedded within the musculature of the anterior tip of the tongue (Hayashida et al. 2010). The glands of Blandin and Nuhn are not lobulated, nor are they encapsulated.
This is the second most commonly occurring mucocele. Over 70% of mucoceles occur in the minor salivary glands throughout the mouth — except the gingiva — and predominately occur on the lower lip. The mucocele is from the severance of a duct with mucous spilled over into the connective tissue.
Some researchers believe that these mucoceles on the ventral tongue area are more common than originally thought, but are not seen clinically very often because of the location in the mouth (Jinbu et al. 2003) as well as their tendency to rupture prior to discovery.
Because of their location, the patient may not notice the lesions. Unless the dental professional performs a thorough exam, the lesion may be missed. In some cases, they also resolve on their own. The growth may appear circumscribed, exophytic, somewhat fluid-filled but firm, with a blue to reddish color. These lesions do not contain an epithelial lining needed to classify them as a true cyst.
Most cases are reported in individuals under the age of 20 years old, who often report some trauma to the tissue prior to discovery. Jinbu et al. 2003 reported that 21 out of 26 patients in their study were females. It is suggested that because the lesion is thin-walled and close to the surface, they often rupture on their own and are never reported. Mucoceles are usually preceded by trauma such as blunt force, chewing, etc. Secretions are spilled into the connective tissue, and an inflammatory response is initiated with a tissue repair response. The resulting histological diagnosis is mucus extravasation phenomena.
These lesions are surgically removed. Sugerman and Savage (2000) caution that leaving any of the gland residue in the tongue increases the possibility of a recurrence and misdiagnosis as well. In obtaining the clinical diagnosis, it is helpful to aspirate some fluid to determine if there is mucous within the lesion.
Differential diagnoses may include pyogenic granuloma, polyps or squamous papillomata, and lymphangioma depending upon the clinical appearance.
The choices presented by Adachi et al. (2011) are normally surgical excision with evacuation and removal of the servicing mucous gland. Larger lesions may involve the following alternatives, depending upon the individual lesion: marsupialization, cryosurgery, laser ablation, and micro-marsupilization.
Good maintenance and follow-up are the optimal treatment recommendations. As always, keep asking good questions and always listen to your patients.
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ ADHA award winner. Her website for seminars is www.nancywburkhart. com.
References
Adachi P, Soubhia AMP, Horikawa FK, Shinohara EH. Mucocele of the glands of Blandin-Nuhn — clinical, pathological and therapeautical aspects. Oral Maxillofac Surg.2011;15:11-13.
Hayashida AM, Zerbinatti DCZ, Balducci I, Cabral LAG, Almeida JD. Mucus extravasation and retention phenomena: a 24-year study. BMC Oral Health;2010; 10:15 http://www.biomedcentral.com/1472-6831/10/15">http://www.biomedcentral.com/1472-6831/10/15.
de Camargo Moraes P, Bonecker M, Furuse C, Thomaz LA, Teixeira RG, Cavalcanti de Araujo V. Mucocele of the gland of Blandin-Nuhn: Histological and Clinical Findings. Clin Oral Invest.2009; 13:351-353.
Jinbu Y, Kusama M, Itoh H, Noguchi T, Matsumoto K, Wang J, Noguchi T. Mucocele of the glands of Blandin-Nuhn: clinical and histopathological analysis of 26 cases. Oral Surg Oral Med Oral Pathol Oral Radio Endod. 2003;95: 467-70.
Sugerman PB, Savage NW. Mucocele of the anterior lingual salivary glands (glands of Blandin and Nuhn): Report of 5 cases. Oral Surg Oral Med Oral Pathol Oral Radio Endod. 2000; 90:478-482.
Past RDH Issues