Lip pits: Have you seen them?
by Nancy W. Burkhart, RDH, EdD
[email protected]
Your patient today is a 39-year-old male who is in your practice for a scheduled dental appointment. In the past, he has not had dental treatment except on an emergency basis. He tells you that he has noticed a “hole” in the corner of his mouth. He says that he thinks that he may have injured the area. Since he plays a lot of sports, he believes that he may have accidently hit the area during his sports activities.
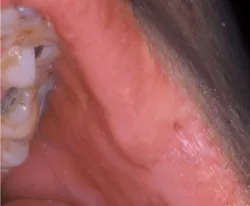
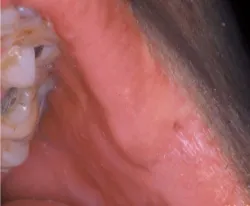
As you examine the commissure of his mouth, you see what he is calling to your attention (see Figure 1). There is a small indentation without any inflammation. You palpate the area and do not detect any growth, firmness, or exudate from the pit. When you insert a probe, you can actually measure about 3 mm in depth. The pitted area is simply a commissural lip pit.
Although lip pits are a benign entity, most clinicians are somewhat baffled by their first encounter with this rather rare developmental anomaly. Lip pits are referred to as “blind caves” that are epithelial-lined with stratified epithelium. Commissural lip pits may occur as an isolated defect or they may be in association with other developmental disturbances such as preauricular sinus.
Lip pits occur unilaterally or bilaterally. Ducts from minor salivary accessory glands may drain into the pits, and the clinician may be able to express saliva from the opening. The failure of fusion in the embryonic union of the maxillary and mandibular processes is cited as the possible etiology of lip pits (Neville et al. 1995). The population percentage is 12 to 20% in adults but much less in children (0.2 to 0.7% of the population).
The question still arises as to whether they are developmental or congenital. Studies by Freudenberger et al. 2008, found 8% of a population of 2,182 neonates demonstrated commissural lip pits, as well as 11% with ankyloglossia. This study would question whether there is more of a congenital history rather than a later developmental origin.
Along with the commissural lip pit, the congenital lip pit that is found in the midline of the lip is another such entity. These are classified as paramedian lip pits and are present as indentations on the lower lip on either side of the midline, occurring during embryonic development. In addition, van der Woude syndrome features an inherited autosomal dominate trait resulting in cleft lip and palate. A recent article on van der Woude syndrome may be found at: www.ijdr.in/text.asp?2011/22/1164/79988.
Van der Woude syndrome is an autosomal dominant disorder that occurs in about one of every 1,500,000 people in conjunction with cleft lip and cleft palate. Sarode et al. 2011 reported a 7-year-old boy with a cleft lip that was corrected at age 18 months. The patient complained of nasal regurgitation and nasal twang.
Evaluation of siblings also revealed ankyloglossia along with the patient being examined. Placing gutta-percha in the lower pits allowed evaluation of the defects. The pits and missing teeth, along with fused deciduous teeth confirmed a diagnosis of van der Woude syndrome.
Another disorder associated with paramedian lip pits is popliteal pterygium syndrome (popliteus muscle, tibia, femur, and knee) that is characterized by pterygia (webbing), cleft lip and cleft palate, genital abnormalities and banding of upper and lower jaws, and oral webs.
The major problem, with both para-median lip pits and commissural lip pits, is the cosmetic concerns/issues. In the case of commissural lip pits, the pits may be deep enough to retain saliva and cause recurring infection because of saliva pooling within the pit. Most patients with commissural lip pits are usually not noticed unless called to the patient’s attention or an infection occurs. In surgery connected to van der Woude syndrome, surgical excision of the lower lip pits, and accessory glands as well as reconstruction of the lip, nose, and correction of other abnormalities is performed (Bozkurt M et al. 2009).
As always, keep listening to your patients and always ask good questions!
References
Bozkurt M, Kulahci Y, Zor F, Kapi E, Yucetas A. Reconstruction of the lower lip in Van der Woude syndrome. Ann Plast Surg. 2009: 62(4): 451-55.
Eisen D, Lynch DP. The Mouth: Diagnosis and Treatment. Mosby; St Louis, 1998.
Freudenberger S, Santos Diaz MA, Bravo JM, Sedano HO. Intraoral findings and other developmental conditions in Mexican neonates. J Dent Child. 2008; 75(3): 280-86.
Neville BW, Damm DD, Allen CM, Bouquot JE. Oral and Maxillofacial Pathology. 1995. W. B. Saunders Co. Philadelphia.
Sarode GS, Desai RS, Sarode SC, Kulkarni MA. Van der woude syndrome with an unusual intraoral finding. Indian J Dent Res [serial online] 2011 [cited 2011 Sep 8];22:164-5. Available from: http://www.ijdr.in/text.asp?2011/22/1/164/79988">www.ijdr.in/text.asp?2011/22/1/164/79988
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and co-author of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. Her website for seminars is www.nancywburkhart.com.
Past RDH Issues