Morsicatio buccarum, labiorum, and linguarum
by Nancy W. Burkhart, RDH, EdD
[email protected]
As you review the health history, Edward is taking several medications. For the past few years, he has been prescribed omeprazole (20 mg.) for GERD, and also takes medication for seasonal allergies. He is a nonsmoker and occasionally drinks alcoholic beverages.
Edward has no other significant health history findings. He exercises but reports that he eats a lot of processed foods and also fast foods because of his schedule. Edward is concerned that the white, raised patches on his inside cheek area are malignant.
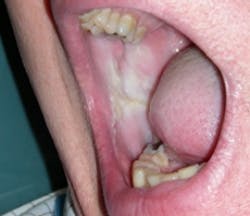
After completing your extraoral exam, you begin to inspect the lip tissues and the buccal mucosa. The tissues in the buccal mucosa areas appear thickened, keratinized, and somewhat striated (see Figure 1). Edward has extreme tissue damage along the occlusal plane and also in the lip area next to the wet line tissues. You alsoDiagnosis: Morsicatio buccarum and morsicatio labiorum.
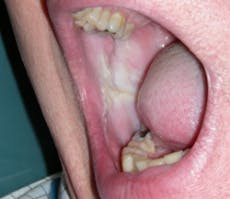
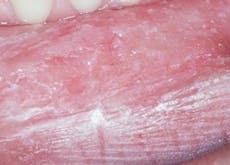
Morsus in Latin means bite. Morsicatio buccarum is biting or chewing of the buccal mucosa; morsicatio labiorum is chewing the lip area (see Figure 2) and morsicatio linguarum is chewing on the borders of the tongue (see Figure 3). The habit may be chewing, biting, or chronic pressure of the tissues. Thicker areas of keratosis may be observed as noted in Figure 3 when the patient continually causes an assault on the oral tissues.
Etiology: Chronic trauma to the tissue causes a defense mechanism to occur in the body. The tissue responds to friction by producing keratin and becoming thickened in what is termed hyperkeratosis. Depending upon the degree of trauma, the tissue may also become ulcerative and eroded in areas. Tissue in the wet areas of the body become whiter in color, just as the skin does when kept in water too long.
Epidemiology: The evidence of trauma may be present at select times and with varying degrees depending upon lifestyle factors and stress levels of the patient. The dental practitioner may notice hyperkeratosis during some exams and may not observe the characteristics at other times. Some patients may be chronic cheekPerioral and intraoral characteristics: The hyperkeratosis is usually found in the line of the occlusal plane on the tissue that contacts the teeth. The mucobuccal folds are usually not affected by the trauma because they are not contacted by the teeth and not in the line of occlusion. The inner lip areas may be a source of irritation as well (morsicatio labiorum) and traumatized by the incisor teeth.
Distinguishing characteristics: The location and clinical appearance usually are diagnostic in almost all cases. Frequently, the patient is aware of the habitual chewing. Depending upon lifestyle factors and stress-related responses by the individual, the appearance of the tissue will vary.
Significant microscopic features: Hyperkeratosis is present. Biopsy is not necessary unless the areas appear different or become more intense, or fall out of what is considered a normal range. An incisional biopsy may be needed to differentiate lesions that appear out of a normal range. The specimen will denote hyperkeratosis with surface bacterial colonization.
Dental implications: Any chronic type of irritation is not a healthy state and may indicate underlying problems such as stress or anxiety disorders. The determination of the source of the problem may help the patient with his/her long-term health, in general.
Differential diagnosis: Linea alba may sometimes be very distinct and produce a heavy occlusal line. White sponge nevus is also a consideration in extreme cases. Because of the abrasion and ulceration in some cases of chronic cheek chewing, deviation from the usual pattern is always a concern, especially if the patient is using tobacco and alcohol.
When assessing morsicatio linguarum, the association of HIV infection and hairy leukoplakia may be considered as well. In some cases, biopsy and further testing may be warranted.
Treatment and prognosis: The clinical suggestions adjacent to this article may help to alleviate the problem and serve as practical suggestions for treating morsicatio buccarum or other frictional areas of concern. As with all extraoral and intraoral lesions, evaluation and monitoring is crucial. In some cases, chronic irritation over time may develop into dysplasia or frank carcinoma. Again, chronic irritation and inflammation in the body should be taken seriously and a conscious effort made to assist the patient in discontinuing unhealthy habits.
As always, keep asking good questions and always listen to your patients.
References
Damm DD, Fantasia JE. Bilateral white lesions of buccal mucosa. Morsicatio buccarum. Gen Dent. 2006; Nov-Dec, 54(6): 442-444.
Delong L, Burkhart N W. General and Oral Pathology for The Dental Hygienist, Lippincott, Williams and Wilkins, Baltimore, 2008.
Neville B, Damm DD, Allen CM, Bouquot JE. Oral and Maxillofacial Pathology. W.B. Saunders, Philadelphia. 1995.
Regezi J, Sciubba J, Jordan R. Oral pathology — clinical pathologic correlations. 4th ed. St. Louis: W.B. Saunders, 2003.
Nancy W. Burkhart, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and co-author of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. Her website for seminars is www.nancywburkhart.com.
Clinical suggestions for morsicatio buccarum, morsicatio linguarum, or morsicatio buccarum, labiorum, and linguarum
- First, show the patient the area of concern. Determine if the patient is aware of the morsicatio buccarum, morsicatio labiorum, or morsicatio linguarum. Give the patient a hand mirror and use the dental lighting to observe the area together.
- Try to determine whether the patient is chewing on the area at night, during the day, or at other specific times. Professionally produced night guards may be beneficial for patients who are performing the habit at night. Often, the patient may also exhibit evidence of bruxism as noted by tooth surface changes. Some shields can be fabricated and worn daily.
- If the patient is new, determine how long ago he or she had noticed the habit. If the tissue is being observed in a patient of record, review the history to determine if any notation is listed in prior visits. How long has it been documented? Chronic habits may take a long time to break.
- If it is determined to be a situational stress problem, suggest stress reduction techniques that may help the patient lower stressful situations. Additionally, forming new coping strategies is crucial in changing a chronic, negative habit and modifying the way that we react to stressors. Some helpful techniques may be exercise, prayer, meditation or other techniques such as biofeedback. Biofeedback will teach a person to use his or her breathing and focus to reduce stress. Personally, I like the hand-held, pocket size device called the EM-WAVE that can be carried by the person and is always available. The device and other relaxation products may be found at: www.stens-biofeedback.com/epistore/search.
- Most people with stress-related conditions are not aware they are stressed, and will tell you that they are no more stressed than anyone else. We all handle stress in different ways, and some techniques are better than others. Ultimately, success depends upon the individual. The good news is: stress reduction can be learned and coping skills can be developed.
- In certain situations, the patient may have taken antianxiety medications and since discontinued those medications, leading to poor health habits. Suggesting that they contact their physician or see a counselor may be appropriate, depending on the person and the clinical signs. In today’s society, many people are overwhelmed with everyday stress, and many offices report an increase in the number of people who are diagnosed with morsicatio buccarum, morsicatio linguarum, morsicatio labiorum and bruxism.
- Use intraoral photography to document the areas of concern, and use the images for future comparison at maintenance visits.
- If the patient uses tobacco and/or alcohol, there is further concern related to future changes in the tissue and oral cancer. If the patient has not had an oral cancer screening, perform one or suggest a biopsy if there is any indication that the area of concern has the possibility of a malignancy (see Dec. 2007 RDH, “Dental Exams: Are You Performing One?”). If changes occur or the habit continues, careful evaluation, referral, or future biopsy in some cases is always wise.
- Remind the patient that any irritation and inflammation in the body is detrimental to our health. Pathogens are able to enter the body and chronic inflammation places us at risk for other health-related disease states.
- Develop some techniques that will make the patient aware of the habit, including:
- Tying a ribbon, rubber band or string around the wrist, which is always helpful in behavior modification and used as a reminder to the person to check his or her own behavior.
- Placing strategically located stickers in the home and workplace to remind the person to check their progress.
Finally, have the patient visualize the word “No” circled with an X through it. This step will help the person eliminate the habit through visualization.
Disclaimer: The author has no affiliation with the Stens Corp.
Modified from Delong L. & Burkhart N. “General and Oral Pathology for the Dental Hygienist.” Lippincott, Williams and Wilkins, Baltimore, 2008.
Past RDH Issues