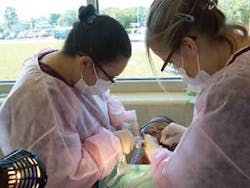
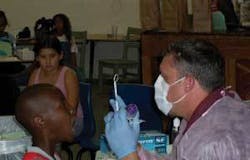
School-based sealant program
A public health opportunity whose time has come
Dental hygiene programs have community or public health dentistry as part of the curriculum. They assess, plan, implement, and evaluate programs and present them to local schools within their communities. Some dental hygiene programs take community dentistry one step further by providing as many opportunities as possible for students to experience various aspects of this component of dentistry.
Despite the number of dental hygienists employed in the United States and the number of dental hygiene schools across the country, there still exists a disparity among thousands of residents within various communities who lack access to adequate oral health services. Some states’ dental societies have reported perceived shortages in the dental hygiene workforce, thereby creating a proliferation of dental hygiene schools within those states. The issue does not appear to be lack of qualified personnel, but perhaps the inability of states to utilize the existing workforce to meet the oral health needs of its citizens.
Restrictive supervision laws generally prohibit dental hygienists from performing specific functions unless a dentist is present, and from reaching those with limited access, particularly those living in rural areas. While individual states work on revising their respective practice acts to ensure everyone has access to quality health-care services, dental hygiene programs have always sought to provide practical experiences in community health for students as part of the curriculum. This may serve as a temporary but consistent measure to add to the workforce to ensure individuals receive some services, although the services will be limited to those that fall within the dental hygiene scope of practice.
Recently, a colleague forwarded an article from The Dallas Morning News that was also posted on the Belleville.com Web site on Dec. 4, 2005, which cited using dental hygiene students to help provide services for residents in a local nursing home. According to the article, Diane Ring, an adjunct faculty member at Temple College, began a pilot program in a Texas nursing home. She had students working with her who helped set up portable equipment at the facility, provided dental health education to the caregivers and residents, and developed individual dental hygiene care plans based on their needs. Other examples of dental hygiene programs using dental hygiene students to assist in increasing access to care have been reported in the literature, and one such effort of a program in southern Illinois will be highlighted here.
The dental hygiene program at Southern Illinois University Carbondale (SIUC) received funding from the Illinois Department of Public Health/Division of Oral Health (IDPH/DOH) to establish and implement the Dental Sealant Grant Program (DSGP). A Maternal Child Health Preventive Block Grant enabled the IDPH/DOH to place a request for proposals (RFP) for local health departments or other agencies within the state to compete for funds to purchase portable equipment for use in providing oral exams, sealants, and oral hygiene education for children eligible for a free or reduced lunch or Medicaid.1
Several positive aspects are associated with the DSGP:
➊ The SIUC Dental Hygiene Program is the only grantee within the state that is not associated with a local health department. The program serves as the sponsoring agency, while across the state local health departments serve as sponsoring agencies. In another scenario such as at Lewis & Clark Community College, the students help run the sealant program for the local health department.1
➋Dental hygiene students comprise the bulk of human resources for the DSGP.
➌Dental hygiene students have unlimited service-learning opportunities.
➍The supervising dentist is a full-time faculty member, thus eliminating the burden of recruiting a dentist to work with the program.
➎Dental hygiene faculty can use the DSGP as part of their indirect teaching duties and service requirements for tenure and promotion.
➏Licensed dental hygienists who work under the general supervision of a dentist supervise the dental hygiene students. This has increased the number of hours, encounters/exams, and sealants placed, as well as eliminated the basic requirement of a dentist’s presence.
The dental hygiene students primarily perform preventive services. Beginning with the last academic year, the fourth-year students were assigned hours at various rotation sites, such as the Veterans Administration Hospital (VA), a nursing home, a clinic providing services for migrant farmworkers and their families, and the DSGP as part of a course in Rural Health and Geriatrics. Fourth-year dental hygiene students also provide preventive services for clients in the SIUC Dental Hygiene program-sponsored Community Dental Clinic (CDC). The CDC is for individuals who qualify for Medicaid under federal income guidelines. Students not only provide clinical services in a schedule that is much like that of private practice, but also acquire experience working with dental practice software like Dentrix®. This has all but forged opportunities to provide services within community entities, while allowing the hygienists to establish relationships with those who operate the agencies.
The theory of service-learning is not new. Fostering a sense of community through volunteerism and “giving back” to the community has been well-documented. But this theory was established in dental hygiene by Alfred C. Fones, the founder of dental hygiene, which said volunteering was to serve through “public education.”2 Dental hygiene education programs not only were initiated in the elementary schools, but school dental clinics were also established for children’s dental treatment.3
One definition of service-learning is: “A structured learning experience that combines community service with preparation and reflection. Students engaged in service-learning provide community service in response to community-identified concerns and learn about the context in which service is provided, the connection between their service and their academic coursework, and their roles as citizens.” (Community-Campus Partnerships for Health)
Several factors influence the effectiveness of service-learning experiences:
✵Students’ and community members’ shared perceptions that the project is valuable
✵Opportunities for students to be depended upon by others
✵Particular assignments that engage students to think critically and that have an ethical component
✵Responsibility for decision-making and determining the project’s direction
✵Young people and adults working together on common tasks
✵Systematic reflection on service experience
✵A final product representing the students’ efforts (Hedin,1989 as cited by Sandell, Denbow, Curtis & Crawford)4
One supervising dentist and third- and fourth-year dental hygiene students staff the DSGP. Two registered dental hygienists, who are also full-time faculty members with the dental hygiene program, serve as supervisors for the students. Third-year dental hygiene students were able to volunteer as their class schedules permitted and received credit toward requirements in their clinical course. Several students over the life of the DSGP have received credit through independent study (IS). The students have acquired a wealth of knowledge and experience working with a public health program. To avoid “double-dipping,” the IS student is not given clinical but rather course credit, since the duties outlined for them differ greatly from those receiving clinical credit.
The IS student is supervised by a dental hygiene faculty member who is also one of the principal investigators for the grant program. The student meets with the faculty member for a few hours each week to review the status of the program. Some of the duties typically performed by the IS student include but are not limited to: supply inventory, online billing (reimbursements are available through Doral Dental Services, Inc. - the Medicaid provider for Illinois), data entry, assistance in the preparation of state reports, equipment maintenance, dental assisting and dental hygiene functions (includes charting, record keeping, and sealant application), and maintaining the photo scrapbook (pictorial history) for the DSGP.
The dentist performs the examination and determines the teeth that need sealants. The dental hygiene faculty have requirements for tenure and promotion established by the academic institution. Their participation in the DSGP satisfies the service aspect and lends itself to other opportunities for teaching and research as well.
Finally, because Illinois has general supervision, the dentist is not required to be present during treatment, so this gives licensed dental hygienists and the dental hygiene students a greater opportunity to perform preventive services without the imposition of certain practice restrictions. It serves the DSGP well that the supervising dentist is “pro” dental hygienist and offers this comment on behalf of general supervision:
“It [general supervision] has been a great step in the right direction for the dental health-care profession. It has shown that dentists and dental hygienists can work together as one to help meet the dental needs of Americans. It has given the respect to dental hygienists that they so rightly deserve. It is only a step. The journey is not complete. There are still more steps needed to meet all the dental needs in the United States, especially those of the underserved.”
Because the SIUC Dental Hygiene Program is the only baccalaureate program in Illinois, it must position itself as the forerunner by working with local dental and dental hygienists’ societies and community organizations with the common goal of decreasing oral health disparities. Changes in the way dental hygienists will practice in the future are forthcoming as the interest in making the Advanced Dental Hygiene Practitioner (ADHP) becomes a reality. All baccalaureate and graduate dental hygiene programs in the nation must be prepared to work collaboratively with the members and leadership of the American Dental Hygienists’ Association and other like-minded groups to increase access to oral health care for those who are consistently left behind due to low socioeconomic status or limited knowledge of the need for good oral health.
As the ADHP continues to gain momentum legislatively, all health-care professions may or may not be prepared to embrace this concept as the answer to the oral health disparity problem. Regarding the future of the ADHP, the supervising dentist for the DSGP and one of the clinical dentists for the CDC, Dwayne Summers, DMD, renders this hopeful observation:
“I agree there is a great need for a trained professional to meet the dental needs of the underserved population of the United States. However, the patients whom I see in a public aid and low-income dental clinic (SIUC Community Dental Center) seldom need a simple restoration. They usually need a complex filling, root canal, or an extraction. Thus, I am not sure that an ADHP will solve the total problem. I do feel that the ADHP can be used to triage patients (diagnosis, preventive services, simple and medicated fillings, and antibiotic prescriptions). Dentists are still needed to complete the work. Being a public health dentist, I believe that there should be a commitment from private practice dentists throughout the United States to see these underserved patients in their own offices to completely solve this problem.”
In preparing the future dental hygiene workforce, dental hygiene programs should continue to encourage students to take on more active roles within their communities. This will not only make them more aware of the needs of their neighbors, but may create a cadre of compassionate health-care professionals who are willing to serve and bridge the gap in access to care among underinsured and uninsured citizens.
Additional resources
• http://depts.washington.edu/ccph/servicelearningres.html
• http://depts.washington.edu/ccph/servicelearningres.html#Dentistry
• http://www.compact.org/aboutcc/glossary/glossary.html#servicelearning
References
1 Miller FY. The utilization of dental hygiene students in school-based dental sealant programs. J Dent Hyg 2005; 70 (4):1-8. Available online at http://www.adha.org.
2 Wilkins EM. Clinical practice for the dental hygienist 1999; 8th ed Lippincott, Williams & Wilkins, Philadelphia.
3 Perry DA, Beemsterboer P, Taggart Jr EJ. Periodontology for the dental hygienist 2001; 2nd ed WB Saunders Company, Philadelphia.
4 Sandell K, Denbow H, Curtis L, Crawford M. Service-learning pedagogy: demonstrating increased learning and higher order thinking. Retrieved June 13, 2005, from http://www.units.mu ohio.edu/lillycon/old/00conabstract.htm#ap36.