Plasma Cell Gingivitis: Investigate products that cause gingival hypersensitivity
BY NANCY W. BURKHART, BSDH, EdD
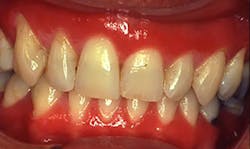
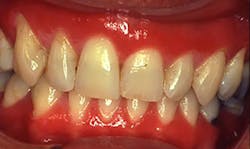
Plasma cell gingivitis (PCG) is a benign condition of the gingiva with characteristics of generalized edematous and erythematic gingival tissues. The edematous tissue often extends to the mucogingival junction with a deep red appearance.
Plasma cell gingivitis and allergic gingivostomatitis are terms that are associated with allergic responses to substances. Other terms that have been used are idiopathic gingivostomatitis, atypical gingivostomatitis, allergic gingivostomatitis, hypersensitivity, and plasmacytosis. Several contact disorders of the oral tissues are known and are called orofacial disorders.
Pathogenesis: Early reports in the dental literature found a number of patients with red, edematous gingiva who were using a particular type of gum. After eliminating the gum, the red, inflamed tissue subsided. It was thought that the irritated tissue was a result of some component in the gum. In earlier years, clove gums were popular.
--------------------------------------------
Other articles by Burkhart
- The Fissured Tongue: Patients may be concerned about oral cancer risk
- Reduction of Tooth Stains: Patient education is vital to preventing tooth stain
- Lichen planus pemphigoides: Diagnosis should be followed by referral
--------------------------------------------
Today, the term PCG is used when histological features denote an abundance of plasma cells as described in the next section. Type lV hypersensitivity is the reaction that is produced. Unlike the Type 1 reaction that can be life threatening, the Type lV reaction is a delayed, cell-mediated immune response.
Reactions to dental products such as toothpaste, mouth rinses, and additives have been reported. The reactions culminate in a gingival tissue response.
Dental materials such as crowns and restorations, food products, preservatives, and additives are reported to cause hypersensitivity as well. However, dental materials often produce a localized reaction rather than a generalized reaction of the tissue. Early publications by Silverman and Lozada, as well as Kerr et al., suggested that chewing gum was a major factor in reported cases cited within these publications. Specifically, those products with essential oils have been noted. Peppermint, wintergreen, menthol, spearmint, and cinnamon are known to cause tissue erythematic symptoms in some individuals.
Additionally, detergents used in toothpaste, flavoring agents, and preservatives may cause problems in some patients. Mints, gums, and candies with flavoring agents are also noted for causing problems. Discontinuation of the offending products promoted an elimination of the gingivitis.
Figure 1: Clinical image of plasma cell gingivitis. Courtesy of Dr. T. D. Rees, Baylor College of Dentistry.
A recent article by Joshi and Shukla (2015) reported a patient with plasma cell gingivitis after prolonged use of herbal toothpowder. Products are changed often, and new ones come on the market so fast that even the combinations of products may present a problem for anyone who is sensitive to a particular ingredient.
Perioral and intraoral characteristics: The gingiva has a fiery red color with a bulbous appearance that is dispersed throughout the gingival tissue. The reddened color is often the factor that brings the patient to the dental office. Frequently, others have noted the appearance, prompting the patient to find the cause during an appointment.
Histology: As the name denotes, plasma cells are numerous within the tissue when examined microscopically. The key features of the allergic response are the numerous plasma cells and the epithelium exhibiting spongiosis (inflammatory intercellular edema of the epidermis) and inflammatory cells. A common finding is elongation of the rete ridges. Plasma cells are B-lymphocytes involved in the synthesis, storage, and release of antibodies.
The goal of the immune response is to remove or neutralize antigenic substances. To accomplish this goal, the system must recognize the "invader," react to the invader, and remember the invader. A plasma cell results in the transformation of the B cell into an antibody-secreting lymphocyte (DeLong and Burkhart, 2013).
Factors to consider: Normally, candida infections and plaque-related issues are ruled out initially. Other mucosal and disease processes may be considered depending upon the clinical and health history findings:
• Mucous membrane pemphigoid
• Lichen planus
• Lupus
• Leukemia
• Pemphigus vulgaris
• Squamous cell carcinoma
• HIV infection
• Desquamative gingivitis
• Vitamin deficiency and anemia
• Crohn's disease
• Sarcoidosis
• Foreign body reaction
• Deep mycotic infections
Treatment and prognosis: The evaluation and elimination of disease states must be accomplished first, and then a careful evaluation of the environmental and lifestyle factors will be key in assisting the patient in recovery.
A careful assessment of the diet and any offending products is needed (a partial list of possible contributors to the PCG status is noted in the sidebar). A two-week diet assessment with elimination of these products is usually recommended. Children's toothpaste or dry-mouth toothpaste are frequently recommended for patients with PCG. Both usually have fewer additives and flavoring agents. The fewer additives found in the ingredients, the less chance of the patient reacting to the product.
A biopsy may not be needed if the tissue responds to elimination of the products that may be causing the reaction. However, the only way to know if the questionable tissue is plasma cell gingivitis is through examination of the tissue. A notable difference should occur within two weeks, if the inflammaion is due to a hypersensitivity reaction.
Patient education: A very soft-bristle brush is recommended until the inflamed gingiva is under control. There are some good brushes on the market called "surgical brushes" that are for patients who cannot use even a regular soft-bristle brush.
Retention of plaque causes the tissue to become even more irritated, and if the patient is unable to brush, the problem is compounded. Trying to identify the source of the PCG is key to recovery because the tissue will not respond as long as exposure to the item continues. A diet diary and complete assessment of any contact with foods and dental products is needed.
Dentists and hygienists can be very instrumental in assisting the patient in determining the offending product. Often, it is not an easy task. If PCG is the problem, a two-week limit of products usually produces some tissue changes. Careful listening to the patient is necessary so that a time line can be established, products can be eliminated, and prevention of further tissue inflammation can be accomplished.
New products come on the market daily and the patient may be reacting to one or several items that they are using. For example, cinnamon is not only sold as a spice; it is commonly added to many products that we consume daily, including dental products.
Assisting the patient in finding replacement products is needed as well. Products such as lip balms and lipsticks do not stay only on the lips, but are ingested as well. A careful look at cosmetics is also recommended.
As always, listen to your patients and always ask good questions! RDH
Possible Offending Products to Gingival Tissue
• Commercially available toothpaste (tartar-control additives and flavoring agents [possibly cinnamon] that mask the tartar control additives)
• Mouth rinses
• Cinnamon aldehyde
• Sodium benzoate and methyl paraben
• Food substances such as wheat, dairy, chocolate, eggs, peanuts, and monosodium glutamate
• Red wine (sulfides and tartrazine additives)
• Preservatives
• Essential oils such as peppermint, spearmint, and wintergreen found in gums, candy, and mouth rinses.
• Dark cola drinks
• Strong spices
• Chili peppers
• Clove
• Cardamom
References:
Burkhart NW. Toothpaste allergy. RDH. 2007; 27(6): 86,107-108.
DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist, Second Edition. 2013. Wolters Kluwer/Lippincott, Williams & Wilkins. Baltimore.
Endo H, Rees TD. Cinnamon products as a possible etiologic factor in orofacial granulomatosis. Med. Oral Patol Oral Cir Bucal. 2007. 12(6): E440-4.
Joshi C, Shukla P. Plasma cell gingivitis. Journal of Indian Society of Periodontology. 2015. 19(2), 221-223. doi:10.4103/0972-124X.145830.
Kerr DA, McClatchey KD, Regezi JA. Idiopathic gingivostomatitis. Oral Surg. 1971. 32(3): 402-423.
Palmer RM, Eveson JW. Plasma-cell gingivitis. Oral Surg. 1981. 51(2):187-189.
Rees TD. Orofacial granulomatosis and related conditions. Periodontology 2000.1999; 21:145-157.
Silverman S Jr, Lozada F. An epilogue to plasma-cell gingivostomatitis (allergic gingivostomatitis). Oral Surg. February 1977. 43(2): 211-217.
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com. She can be contacted at [email protected].