Preventing ringworm
by Noel Kelsch, RDHAP
[email protected]
Being a friend involves many things. Some of my favorites have been singing in the rain, helping deliver a baby, riding the skunk train through the redwoods, and laughing until it literally hurt.
At times being a friend involves sacrifice. I have pulled a dead frog out of a pool pump, killed a rattlesnake, and lectured on infection control in the middle of a mall when a dear friend insisted on a tattoo to mark a change in her life.
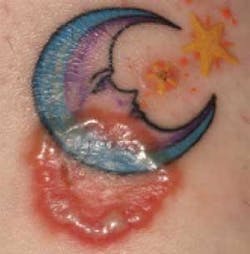
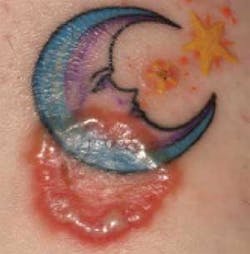
A week later she showed me a lesion on her tattoo. I knew immediately what it was. “:Oh, it couldn't be!” she insisted. “:The tattoo artist said it was just a reaction to the ink.” I insisted she see her doctor. What had my friend developed? She had developed tinea corporis (ringworm). Ringworm is not a worm at all, but a disease caused by fungi.
A fungus among us?
According to the Centers for Disease Control, this contagious disease is really caused by fungi (dermatophytes). It can be acute or chronic and usually affects exposed areas, but can also spread from other infected sites. Ringworm can affect your entire body, from the scalp (tinea capitis, which usually makes a bald patch of scaly skin), and groin area (tinea cruris, also called jock itch), to the feet (tinea pedis, also called athlete's foot). People with ringworm on other parts of their skin can have a ring-shaped rash that is red and itchy. The rash can be dry and scaly or wet and crusty.
How is it transferred?
My friend wanted to know how this happened. I explained cross contamination — the act of spreading bacteria and viruses from one surface to another. She was surprised that fungi, bacteria, and viruses can live on objects and surfaces for up to a week, and can be spread when surfaces are not disinfected correctly or equipment is not cleaned and sterilized between clients.
The fungi that cause ringworm thrive in warm, moist areas. Poor hygiene and long-term wetness of the skin create a perfect environment and raise the risk for a fungal infection. Ringworm is more likely when you have frequent wetness (such as sweating) and minor injuries to your skin, scalp, or nails (such as a tattoo or placement of artificial nails).
It can be passed from one person to the next by direct skin-to-skin contact or by contact with contaminated items such as combs, unwashed clothing, and shower or pool surfaces. In the dental setting this disease can be spread through cross contamination and skin-to-skin contact. Ringworm can also be caught from pets that carry the fungus.
Treatment
There are several medications, both systemic and topical. Antifungal creams such as miconazole and clotrimazole are effective in controlling the disease. Oral antifungal medication may be given. Antibiotics may be needed if a secondary bacterial infection occurs. It is important to see a dermatologist for definitive diagnosis of the lesion. Everyone in the family, including pets that carry the disease, must be treated or there is a good chance of the disease recurring.
How is ringworm prevented in the dental setting?
- Do not see patients who have exposed lesions.
- Practice standard infection precautions with all patients.
- If you have the disease, keep it covered or do not provide services.
- If it is on your hands, as with any open sore or weeping lesion, you may not provide direct patient services until it is resolved.
I love being a friend. Being there for the good times and sharing life challenges enriches my life every day. Meeting infection control guidelines and sharing prevention techniques can prevent disease for everyone we come in contact with in the dental setting.
About the Author
Noel Brandon Kelsch, RDHAP, is a syndicated columnist, writer, speaker, and cartoonist. She has received many national awards and owns her dental hygiene practice that focuses on access to care for all. She has devoted much of her 35 years in dentistry to educating people about the devastating effects of methamphetamine and drug use. She is immediate past president of the California Dental Hygienists' Association, on the board of directors for the Simi Valley Free Clinic, and is a five-time winner of the Castroville Artichoke Cook-off. She can be reached at [email protected].