Sentry duty: On guard for oral cancer
The dental hygiene professional is obligated to screen patients for oral cancer. A patient`s quality of life is dependent upon early detection.
Dawne E. Evans, RDH, BS, and
Joen Iannucci Haring, DDS, MS
The dental hygiene professional is committed to improving patients` oral health and providing quality patient care. As a part of that professional commitment, the dental hygienist has an obligation to screen patients for oral cancer. The hygienist must know the importance of oral cancer screening and be familiar with the steps used in cancer screening examination.
In addition, the hygienist must recognize the signs of oral cancer and be able to identify squamous cell carcinoma, the most common type of oral cancer.
Cancer screening involves soft tissue and not teeth. Diseases of the oral soft tissues are potentially deadly, whereas conditions of the teeth are not. As a result, cancer screening is of paramount importance, and the identification of oral cancer is the single most significant service that any dental professional can provide for a patient.
Initially, oral cancer is often asymptomatic. The lesions are not painful and go unnoticed. Many patients are simply unaware that any problem exists. Consequently, the dental professional may be the first person to identify oral cancer, long before the patient experiences any symptoms.
Early detection of these asymptomatic lesions is the key to successful treatment. The earlier oral cancer is detected, the better the chance for a cure. The early detection of oral cancer is critical in improving patient survival.
The cancer screening examination
By performing a cancer screening examination, the dental hygiene professional plays a vital role in the identification of oral cancer. A standardized exam for the detection of oral cancer is recommended by the World Health Organization, the Centers for Disease Control and Prevention, and, the National Institutes of Health. A color poster detailing and illustrating each step of the cancer screening examination is available, free of charge, from the National Institutes of Health. "Detecting Oral Cancer: A Guide For Health Care Professionals" can be obtained by contacting the National Oral Health Information Clearinghouse, 1 NOIHC Way, Bethesda, MD 20892-3500.
The detection of oral cancer begins with a thorough review of the medical history. Questions concerning any changes in the patient`s overall health are critical. Following the review of the medical history, the head and neck region must be examined for any enlarged and non-tender lymph nodes. The presence of such nodes may indicate the metastasis, or spread, of oral cancer.
Next, the oral tissues are carefully examined. The hygienist must take special care to examine the soft tissues of each patient at every appointment. Every appointment must begin with a thorough examination of the soft tissues, regardless of what treatment is scheduled to be performed. The soft tissue examination need not be time-consuming and should be completed within a few minutes.
Whenever a soft tissue lesion is detected, the dental professional must obtain additional information. How long has the lesion been present? Has the lesion changed in size, color, texture, or consistency? Are there any signs or symptoms present, such as pain or bleeding? Is there a history of injury or irritation to the area?
Additional questions must then be asked concerning risk factors. Does the patient smoke? If so, how much and for how long? Does the patient drink? If so, how much and for how long? If a lip lesion is noted, does the patient have a history of chronic sun exposure?
The dental professional must document all of these findings, along with information concerning the medical history and the extraoral and intraoral examinations in the patient record. In addition, the dental professional must recognize the need for further investigation of any lesion that lasts longer than 14 days. All oral lesions should resolve in two weeks and any lesion that persists longer must be further evaluated (biopsy, for example).
Signs of oral cancer
The hygiene professional`s awareness of oral cancer is fundamental to minimizing the time from the onset of symptoms and signs to diagnosis. Because oral cancer is typically asymptomatic, months or years may elapse before the patient seeks consultation. In the absence of symptoms, the hygiene professional must be able to recognize the most common signs of oral cancer. Oral cancer generally presents as a persistent lesion in one of the following forms:
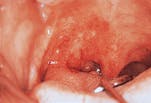
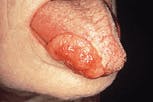
- Ulceration. The term ulceration is used to describe a lesion that is characterized by the complete loss of the outer layer of mucosa. An ulceration typically appears de-pressed with a yellow, necrotic center and an irregular outline. The borders are rolled and indurated, or hard, with a pink, red or white color.
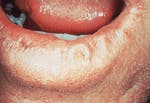
- Erythroplakia. The term erythroplakia is a clinical term that is used to describe a lesion that appears as a "red patch." The erythroplakia appears as a red, flat, well-defined area with a texture that resembles velvet.
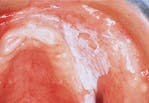
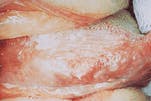
- Leukoplakia. The term leukoplakia is a clinical term that is used to describe a lesion that appears as a "white patch or plaque." The leukoplakia appears as a white, flat or slightly elevated area with a smooth or wrinkled surface.
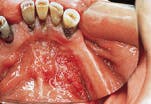
- Exophytic mass. The term exophytic is used to describe a mass that is "growing outward." An exophytic lesion exhibits an irregular surface and appears red, white, or red and white in color. Ul-ceration is often present.
In addition to the dental professional`s awareness, patient awareness concerning oral cancer is necessary. Patients should be educated concerning the warning signs of oral cancer and understand the importance of early detection. Patients should be encouraged to take an active role in cancer detection by performing monthly self-examinations of the oral soft tissues.
Common types of oral cancer
During this year, cancer of the oral cavity and pharynx is estimated to affect 30,000 Americans and cause approximately 8,000 deaths. Oral cancer, which includes lip cancer, accounts for 4 percent of all cancers in men and 2 percent in women.
Oral squamous cell carcinoma (SCC) is the most common oral cancer and comprises 90 to 95 percent of all the oral malignancies diagnosed in the United States. Twenty-five to 30 percent of all oral cancers involve the area around the lip. Although SCC may be found in any location, the tongue and floor of the mouth are also common sites. Because SCC behaves differently depending upon its location, a separate discussion of SCC of the lip and intraoral SCC is warranted.
Squamous cell carcinoma of the lip
Etiology. The risk for lip cancer increases as exposure to a precipitating factor increases. Although excessive sun exposure is the primary cause of SCC of the lip, tobacco use also plays a contributing role. Certain forms of tobacco use, such as pipe and cigar smoking, are most often linked to SCC of the lip. Alcohol consumption, poor oral hygiene, chronic irritation, and trauma may also serve as predisposing factors for SCC of the lip.
Clinical features. Although SCC of the lip may occur at any age, the lesion most often occurs in adults between the ages of 50 and 70. Men are twice as likely to be affected as women. The lower lip is the most frequent site of occurrence.
The lesion has a variety of clinical appearances. The usual presentation is that of a chronic non-healing ulceration and crust. Raised and indurated borders may be present. The size of SCC of the lip is also variable; a larger lesion may appear as a crater-like defect or an exophy-tic mass.
Squamous cell carcinoma of the lip is often asymptomatic. However, in some instances, pain and bleeding may be present. Invasion of underlying structures and metastasis to lymph nodes and other organs typically occurs late in the course of the disease.
Diagnosis and treatment. A biopsy is necessary to establish a diagnosis of SCC of the lip. All non-healing ulcerations and persistent lesions of the lip must be biopsied. If the result of the biopsy is negative and a strong clinical suspicion for SCC exists, the lesion should be re-biopsied. Once a definitive diagnosis of SCC is established and staging has been determined, treatment can be rendered.
Treatment options include surgical excision and radiation therapy. Smaller lesions may be surgically removed or irradiated while larger lesions may require a combination of both surgery and radiation therapy.
Prognosis and follow-up. Treatment success is based on the size of the lesion and metastasis. The overall prognosis for SCC of the lip is based on the presence of metastasis. Without metastasis to the lymph nodes and other organs, the prognosis is favorable with an 85 percent 5-year survival rate.
Following treatment, persons with SCC of the lip should receive frequent follow-up physical and oral examinations. Approximately 80 to 90 percent of all recurrences appear within the first two years.
Intraoral squamous cell carcinoma
Etiology. Tobacco use is the major predisposing factor linked to intraoral SCC. A correlation exists between the frequency and duration of all forms of tobacco use and incidence of this type of cancer; the longer and more frequent the use of tobacco products, the greater the risk of developing intraoral SCC. Excessive alcohol consumption is also a contributing factor for intraoral SCC.
Clinical features. Intraoral SCC is most often seen in individuals between the ages of 40 and 80; however, intraoral SCC may also occur in young adults and children. Men are affected more frequently than women. Although intraoral SCC can be found anywhere in the oral cavity, the most common locations include the tongue and floor of the mouth (excluding the lip).
The typical ton-gue lesion is seen on the the posterior lateral border, while the anterior floor of the mouth is involved more frequently than the posterior. Other locations include the soft palate, buccal mucosa, and gingiva.
Intraoral SCC has a variety of clinical appearances. While the usual presentation is that of a chronic non-healing ulceration, intraoral SCC may also appear as an exophytic mass, or a red, white, or red and white plaque. Raised and firm borders may be present.
Intraoral SCC is typically asymptomatic; however, in some instances, pain and difficulty in swallowing may occur. Unlike SCC of the lip, metastasis is common and involves the regional lymph nodes.
Diagnosis and treatment. As with SCC of the lip, a biopsy is necessary in order to establish a definitive diagnosis of intraoral SCC. Following diagnosis and staging, treatment can be rendered. Treatment options include surgery and/or radiation therapy. The location and microscopic appearance of the lesion will influence the treatment decision. For example, a lesion that exhibits poorly differentiated microscopic features will require more aggressive treatment than one that is well-differentiated.
Prognosis and follow-up. The prognosis for a patient with intraoral SCC is dependent upon the microscopic differentiation of the lesion and the presence of metastasis. With metastasis to regional lymph nodes, the prognosis is poor with a 20 percent 5-year survival rate. In addition, a factor which impacts the overall prognosis is the increased risk for a development of a second primary lesion. As a result, a physician who manages a patient with intraoral SCC must carefully evaluate the patient for other primary cancers (e.g. laryngeal, esophageal, lung). Careful follow-up by both the physician and dentist for all patients with a history of intraoral SCC is imperative.
Summary
The dental hygienist plays a critical role in identification of oral cancer. With early detection and prompt treatment, the number of patients that die as a result of oral cancer can be reduced. Consequently, there is no greater service a dental professional can provide for a patient.
The dental professional can obtain additional information concerning oral cancer from the following sources:
- Cancer Information Service, (800) 4-CANCER. The Cancer Information Service, a program of the National Cancer institute, provides a nationwide telephone service for cancer patients and their families, the public, and health care professionals.
- American Cancer Society, (800) 227-2345. The American Cancer Society is a voluntary organization with a national office and local units all over the country. It supports research, conducts educational programs and provides many services for patients with cancer. It also provides free booklets on cancer.
- National Oral Health Information Clearinghouse, (301) 402-7364. The National Oral Health Information Clearinghouse (NOHIC), a service of the National Institute of Dental Research, is a resource for oral health information concerning special care patients. NOHIC produces and distributes patient and professional education materials, including topics on oral cancer.
References available upon request. Definitions of important terms mentioned in this article include:
Asymptomatic: Without signs or symptoms.
Biopsy: Removal of tissue from the living body for microscopic examination in order to establish a diagnosis.
Cancer: A term for more than 100 diseases in which abnormal cells divide without control; cancer cells are capable of invading local tissues and spreading through the blood or lymph system to other parts of the body.
Cancer screening: Examination techniques used to detect oral cancer.
Erythroplakia: A red patch found in the oral cavity.
Exophytic: Growing outward.
Lesion: Any pathologic disturbance of a tissue with loss of continuity; a broad term that includes ulcers, tumors, etc.
Leukoplakia: A white patch or plaque found in the oral cavity that cannot be wiped off or diagnosed on a clinical basis.
Lymph node: A small nodular accumulation of lymphoid tissue that produces lymphocytes to combat infection and serve as a defense mechanism for the removal of noxious agents.
Malignant: Deadly; capable of causing death.
Metastasis: The spread of cancerous cells and the establishment of tumors to parts of the body remote from the original tumor.
Necrotic: Dead tissue.
Plaque: A slightly elevated, flat-topped lesion.
Prognosis: The probable outcome of a disease; the likelihood of survival.
Radiation therapy: A treatment for cancer that uses high-energy radiation to damage the cancer cells.
Risk factor: A factor that increases the chance of developing a disease.
Staging: Determining the extent of the disease present (orgingal site versus distant spread).
Squamous cell carcinoma: A malignancy (cancer) that begins in the epithelial cells that make up the lining of many areas of the body (including the oral cavity); most common form of oral cancer.
Tumor: Abnormal growth of tissue.
Ulceration: A depressed lesion that results from the entire loss of mucosa.
Dawne E. Evans, RDH, BS, is a 1996 graduate of The Ohio State University and a practicing hygienist in Columbus, Ohio. Joen Iannucci Haring, DDS, MS, is an associate professor of clinical dentistry in the Section of Primary Care at The Ohio State University College of Dentistry.
Ulceration
Erythroplakia
Leukoplakia
Exophytic mass
Squamous cell carcinoma of the lip
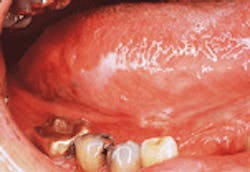
Intraoral SCC on the tongue
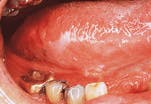
SCC on the anterior floor of mouth
Oral cancer...
- Is seen most often in adults aged 40 to 80.
- Is seen more often in males than females.
- Is one of the most preventable types of cancer.
- Is detected most often by inspection or palpation.
- Is often detected on the tongue or floor of mouth.
- Is responsible for an average of 16 years of life lost.
- Is deadly; only half of those with oral cancer live five years.
The cancer screening exam
Step 1: Review medical history. Question the patient concerning any changes in overall health since the last dental visit.
Step 2: Examine extraoral structures. Examine and palpate the head and neck region for any enlarged and non-tender lymph nodes.
Step 3: Examine soft tissue. Examine all soft tissue areas at every visit with special emphasis on the three most common locations for oral cancer: the lower lip, tongue, and floor of the mouth. If any suspicious soft tissue lesion is noted, proceed with the following steps.
Step 4: Question the patient. Question the patient to obtain the following information concerning the lesion: (1) duration (2) changes in size, color, texture, consistency. (3) signs or symptoms (for example, swelling, bleeding, pain), and (4) history of injury to the area.
Step 5: Identify risk factors. Question the patient to determine if there are risk factors for oral cancer, including a history of smoking, excessive alcohol consumption, or exposure to the sun.
Step 6: Identify sources of irritation. Examine the areas adjacent to the lesion in order to identify any potential sources of irritation. Eliminate any identified sources of irritation (for example, repair any chipped teeth or broken dentures).
Step 7: Re-evaluate the lesion. Instruct the patient to return in 10 to 14 days for follow-up evaluation of the lesion.
Step 8: Document findings. Document all findings in the patient record. Always include the following: (1) any changes in the medical history, (2) the appearance, location, size, and duration of the lesion, (3) any history of changes associated with the lesion, (4) any history of injury, signs or symptoms associated with the lesion, (5) any identified risk factors or sources of irritation, and (6) any instructions provided to the patient concerning re-evaluation of the lesion.
Step 9: Recognize need for biopsy: Recognize the need for further evaluation of any lesion that lasts longer than 14 days. All oral lesions should resolve in 14 days. Any lesion that persists longer must be further evaluated (biopsy, for example). The biopsy of a persistent lesion can be ordered by a dentist, oral pathologist, or physician.
Warning signs
Patients should watch for the following warning signs of oral cancer:
- An ulcer that does not heal.
- A red patch.
- A white patch.
- A lump or thickening.
- A persistent sore throat.
- Difficulty chewing or swallowing.
- Difficulty moving the tongue or jaw.
- Numbness of any area.
- Swelling of the jaws.
These symptoms may indicate cancer or other, less serious problems. Pain is usually not an early symptom. Encourage patients to see a dentist or physician if any of these conditions last longer than two weeks.