Keeping Yourself Safe and Healthy: Choose, then Use PPE
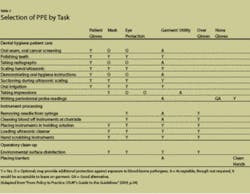
Many of us still remember the confusion and uncertainty when trying to comply with the personal protective equipment (PPE) section of the Bloodborne Pathogens Standard when it first came out in 1991. Fifteen years later, there are many more types of protective gear to choose from; but the basic premise of the Occupational Safety and Health Administration (OSHA) is the same today as it was then - whatever you choose to wear must protect you from the hazardous materials found in the workplace (see Table 1). For dental hygienists, that usually means taking steps to avoid the spray, splash and spatter of potentially infectious material encountered in direct patient care and reprocessing instruments.
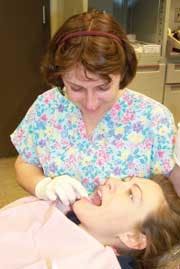
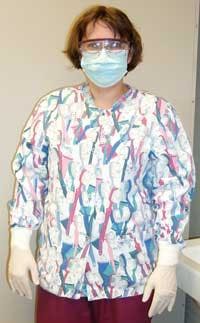
For some, wearing long sleeves, a face mask, and face shield have become a part of normal work practice. Others struggle with the discomfort, heat, or nuisance of personal protective equipment and have opted to not bother with certain items (see Figure 1). Still others wear “everything” only to remove it when the patient is dismissed and then go to process contaminated instruments thus exposing themselves to contaminated liquids. Another potential gap in adequate protection comes when equipment is cleaned such as the X-ray developer or draining and cleaning the ultrasonic unit.
So how do we decide what PPE to wear and when? The legal aspect of this comes from OSHA in the form of the personal protective equipment section of the Bloodborne Pathogen Standard 1910.1030 (found at http://www.osha.gov). This standard was unique when it came out in that it was performance-based rather than specifically stating what to wear and when. It laid out criteria on how to assess hazards then left it up to the employer and employee to choose the personal protective equipment that they deemed reasonable, necessary, and appropriate. This performance-based method left clinicians both confused and empowered to make their own choices. These many years later, we still have the power to evaluate our occupational hazards, and then make appropriate choices based on law, science and personal preference.
The Centers for Disease Control and Prevention (CDC), in their “Guidelines for Infection Control in Dental Health-Care Settings, 2003,” reviewed the scientific literature and presented evidence-based recommendations for PPE selection. If you have not obtained a copy of this excellent reference, you can go to http://www.cdc.gov/OralHealth/infectioncontrol/guidelines/index.htm and print your own copy. The CDC’s Guidelines offer excellent information on things to look for when selecting masks, protective eyewear/face shields, and protective clothing. In addition, there is a fairly extensive section discussing different types of gloves, glove integrity, and the pros and cons of double gloving.
Another excellent resource for looking further into the selection of PPE is the Organization for Safety and Asepsis Procedures workbook “From Policy to Practice: OSAP’s Guide to the Guidelines.” You can find detailed, easy to use guidance on how to follow the CDC’s Infection Control Guidelines. More information on this resource can be found at http://www.osap.org.
The goal in using personal protective equipment is to protect the skin and our mucous membranes - eyes, nose and mouth - from spray, splash and spatter of potentially contaminated material. Though the number of Americans infected annually with bloodborne pathogens has dropped, there still remains a risk of occupational exposure (see Table 2).
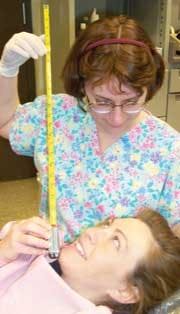
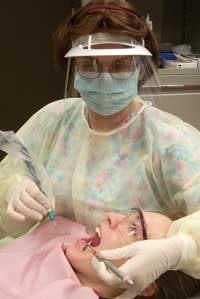
One way to decide what PPE to wear is to think of our work zone. When an ultrasonic scaler or prophy cup is used, large droplets of blood-containing spray and spatter drop onto the surrounding surfaces within a two-foot zone. Stop to think of what is within two feet of your patient’s mouth. You may even take a tape measure and try to picture what is “hit” with the contaminated, often blood containing, spray and spatter (Figure 2). It is safe to say that everything from the top of the clinician’s head to the hip area is within the two feet of the mouth. A direct hit of any generated spray and spatter should dictate the choice of PPE selected. Remember, the goal is keeping yourself safe and healthy at work as well as providing quality care for your patients (see Figure 3).
Protective eyewear
Eyes are large mucous membranes that viruses can penetrate. OSHA requires that eyewear be able to protect the eyes from spray, splash, and spatter. This general wording allows for a variety of ways to comply with the bloodborne standard.
Some options are:
• Goggles
• Safety glasses
• UV safety glasses
• Full face shields - chin length
• Prescription glasses with solid side shields attached
• Prescription glasses with removable side shields
To decide which is best for you, you need to think of what will provide the best coverage to protect your eyes. The PPE should be comfortable, provide undistorted visibility, and not put pressure or pinch the head.
Masks
Masks come in many types of shapes and filtrations. All surgical masks are considered medical devices and therefore are regulated by the Food & Drug Administration (FDA).
Masks were initially designed to reduce the potential cross-contamination from a surgeon to the patient during surgery. For the dental hygienist, the use of a mask is intended to protect the nose and the mouth from spray and spatter. Though the mask may offer some protection from airborne pathogens, it should not be relied upon to protect the patient or clinician from catching a cold or flu if one or the other is sick. The fit is just not tight enough around the face to prevent the inhalation and expiring of airborne pathogens.
When choosing a mask, there are several considerations. Masks should:
• Have a filtration level of at least 95%
• Offer a light seal over the nose and mouth
• Minimize eyewear fogging
• Allow for easy breathing and be comfortable.
Many distributors are happy to provide sample masks that you can try and see what is best for you. Another consideration is the latex content of the mask. You will limit your occupational latex exposure by choosing a latex-free mask. And finally, as a general rule, dental offices do not treat active tuberculosis cases and refer potential cases to specialized treatment centers. Therefore, the discussion of the use and selection of the N 95 respirator should be referred to the OSHA Respiratory Standard 1910.134 and the CDC web site at http://www.cdc.gov/nchstp/tb
Protective clothing
Once again, OSHA has set forth the requirement that protective clothing must protect the worker from exposure to hazardous material but does not state specifically what that garment must be made of or look like. When the Bloodborne Pathogens Standard came out - there was confusion whether the garment should be water-proof, full length, a lab coat, disposable or reusable and any number of other possibilities. The bottom line is that whatever you wear, it must protect your skin and work clothes (scrubs or street clothes) from being reached by spray, splash or spatter. A good way to see what is appropriate and complies with the law is to try out several different gowns for comfort, protection, and maintenance (laundering or disposal). It is important to remember that scrubs offer little or no protection from bloodborne pathogens. As to the length of the garment, test and see what is exposed or can be spattered two feet from the person’s mouth when you are sitting at your chair. This will help determine what you choose - full length gown or lab coat. If your legs are exposed within two feet of the patient’s mouth, you may consider more appropriate PPE.
Gloves
As with all PPE, gloves should be chosen with the task in mind in order to protect the clinician from biologic, physical, and/or chemical hazards. There are three basic types of gloves that are used in the dental setting to prevent occupational exposure to known hazards: patient care gloves, heavy-duty utility gloves and over-gloves.
Patient care gloves should be comfortable and not bind the hand’s movement. The glove should also be the right size and allow for good tactile sense. In order to reduce exposure to latex allergens, low-protein, powder-free latex gloves may be chosen. The CDC’s Infection Control Guidelines have an excellent decisional table to help you determine the pros and cons of different types of gloves. At the first sign of contact dermatitis or allergy, a dermatologist should be consulted as to the cause and the appropriate choice of patient care glove.
Puncture and chemical resistant utility gloves should be used when cleaning up at chairside, removing needles from a syringe, and manipulating contaminated instruments in the sterilization area. Latex gloves offer no real protection from cuts, punctures, or chemical exposure, they are not appropriate for clean-up or instrument reprocessing. Since utility gloves are never used for patient care, they can be washed, disinfected, and re-used until they become torn. These gloves should be worn when chemicals are changed or equipment is cleaned to protect the hygienist from chemical exposure. When in doubt, see the chemical’s Material Safety Data Sheet (MSDS) for proper PPE.
Over gloves are a great choice to reduce cross contamination in any dental setting. Food handler gloves or even a baggie can be placed over patient care gloves to retrieve forgotten supplies or write down probe readings. These thin plastic gloves should not be used for patient care, chairside clean-up, or disinfection procedures as they offer no protection from hazard in the dental operatory - just an easy way to cover contaminated gloves for an isolated need.
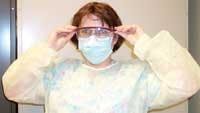
Donning PPE
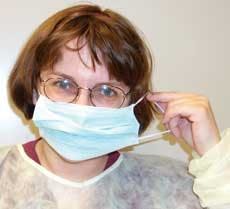
Donning the different components of protective equipment may seem straightforward. However, there are some basic steps and precautions to follow (see Figure 4): (An informative protective equipment poster and training program, “PPE Use in Healthcare Settings: How to Safely Don, Use, and Remove PPE,” can be downloaded from http://www.cdc.gov/ncidod/hip/ppe )
■ Step One: Wash hands at the beginning of the day
■ Step Two: Don lab coat, clinic jacket or gown with high neck
• Welcome patient
• Place patient bib
• Open sterile packages without touching the instruments or supplies
■ Step Three: Place mask - handle only straps
■ Step Four: Place goggles, safety glasses or face shield
• Perform hand hygiene - wash or use alcohol-based hand rub
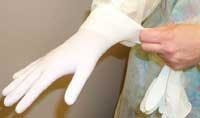
■ Step Five: Don patient care gloves - always place last
• Place gloves just prior to patient care
• Pull glove cuff over gown or lab coat cuff for better protection
• Use over-gloves to write probe readings or retrieve any forgotten items
This sequence will minimize or eliminate touching gloved hands to the face or hair when putting on eyewear or mask. Changing specific PPE throughout the day will depend on the level of spray and spatter, but for the most part, gloves are changed the most, face protection less often and gown the least. However, OSHA requires that if any article of PPE becomes visibly soiled, it must be changed.
Removing PPE
As with donning PPE, there are basic steps and precautions to follow when removing PPE:
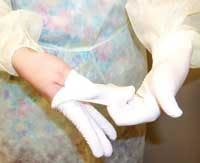
■ Step One: Remove glove
•Grasp outside edge near wrist (see Figure 5)
• Peel away from hand, turning glove inside out
• Hold in opposite gloved hand
• Slide ungloved finger under the wrist of the remaining glove
• Peel off from inside to create a bag for both gloves
• Discard
■ Step Two: Remove face shield or goggles
■ Step Three: Remove mask and discard
• Perform hand hygiene - wash or use alcohol-based hand rub
• Write chart notes
• Dismiss patient
■ Step Four: Remove gown before breaks, lunch or using the restroom
• Remove and fold contaminated sides of gown together and discard
• Perform hand hygiene - wash or use alcohol-based hand rub
Following dismissal of the patient, protective eyewear, safety glasses and chemical resistant utility gloves offer the best protection from sharps injuries and chemical exposure. Your safety and health will be better protected if you put your PPE back on before handling sharp instruments and using disinfectants.
Use and limitations of PPE
▼ Protective clothing (lab coat or gown) - Protective clothing is often the first piece of PPE put on by a clinician. This covering must be removed when the hygienist uses the restroom, goes on break or leaves the office. The protective gown or lab coat should be left in the operatory. Food or drink should not be consumed while wearing a contaminated lab coat. Also, hands should be washed following the removal of any contaminated PPE to avoid the spread of pathogens.
If a lab coat or clinic jacket is chosen, the neck should be closed to protect the neck area, scrub or uniform top. If the neck area is open, then the garment underneath also becomes PPE and must be laundered according to the bloodborne pathogens standard. Clothing used as PPE cannot be taken home and laundered by the employee. It must be placed in a designated contaminated laundry container, then laundered on site or by a professional laundry service.
▼ Mask - The mask protects the hygienist’s nose and mouth from spray, splash and spatter during patient care and reprocessing of instruments. Since the outer surface of the mask can become contaminated with material during patient care, it should be changed between patients. A mask touched by contaminated fingers may become compressed or damp. This causes airflow to decrease through the mask and unfiltered air to increase around the edges of the mask, therefore it should not be touched during treatment.
A mask also becomes damp from exhaled breath or patient material spatter. In this case, the mask should be changed immediately to maintain the highest level of filtration.
A surgical mask is not tight enough around the face to prevent the inhalation and expiration of airborne pathogens, so it should not be used to prevent airborne pathogens from going from patient to clinician or clinician to patient. To avoid compressing the materials in the mask that may result in reduced airflow, it should be placed on the face using only the strings or elastic bands.
If there is any question whether a patient may have active tuberculosis, a surgical mask should immediately be given to the patient, and he/she should arrange to see a specialist. The surgical mask offers little or no protection from airborne mycobacterium tuberculosis pathogens.
▼ Protective eyewear - Protective eyewear (goggles, safety glasses with side shields, or full face shield) is designed to protect the clinician from spray, splash and spatter. If personal eyeglasses are used, they should be evaluated for adequate protection against spatter as well as flying objects such as dislodged calculus or prophy paste. Even with side-shields, small frames may offer little protection from these hazards.
Another potential problem with personal eyewear is that it should be treated the same as other protective eyewear and cleaned and disinfected between patients. Few personal glasses can withstand decontamination day after day. If personal eyewear is not disinfected, then all the day’s spatters go home with the clinician. Protect personal eyewear with a full-face shield or clip-on shield. This may also be appropriate when protecting loupes from contamination.
Chin length face shields offer the hygienist the widest area of coverage to protect the face, mucous membranes and part of the neck. This may be the most appropriate PPE for an ultrasonic device due to the high degree of spray (as shown in Figure 1). Since face shields do not fully protect the mucous membranes, a facemask should be worn under the shield. It is important to use proper eyewear for the hazard. When placing sealants, the hygienist should use specialized protective glasses or a shield intended to protect the eyes from damaging UV light, since the area being cured should be monitored at all times.
Patients should be encouraged to wear personal eyewear or be given safety glasses when spray or spatter may be generated. Patients will appreciate the steps taken to protect their safety and health.
▼ Gloves - Gloves should be chosen to protect the clinician from biologic, physical or chemical hazards. There are three basic types of gloves used in the dental setting: patient care gloves, heavy-duty utility gloves and over-gloves.
Patient care gloves provide adequate protection from contaminated patient material, though they may have small pinholes or develop micro tears during treatment. Hands may become contaminated from leakage through compromised gloves and should always be washed immediately after gloves are removed. Also, avoid rings or long nails since these may cause micro tears in patient care gloves. Gloves need to be changed immediately if torn or compromised and never washed or reused.
Storage, cleaning and disposal of PPE
In general, supplies, including PPE, should be stored in a clean, dry location without high temperatures to avoid the breakdown of latex or other components. As with patient care items, PPE should be stored away from any source of contaminated spray and spatter. Protective equipment should be stored in the operatory so as to avoid splatter from patient treatment or hand washing.
Reusable protective eyewear and utility gloves should be cleaned and disinfected with a mid-level tuberculocidal disinfectant. Lab coats used as protective garments should be placed in a designated contaminated laundry bag and laundered on site or by a medical laundry service. OSHA does not allow contaminated PPE to be laundered by the employee.
Though used PPE is contaminated, it is not considered regulated waste and can be placed in the regular trash. It is important to be aware of your local regulations since some states may require special handling of contaminated “medical waste.”
Conclusion
Dental hygienists should educate themselves on how to avoid the hazards faced daily in the dental office. Though OSHA requires employers to provide information, training and personal protective equipment to address hazards in the workplace, employees should use PPE appropriately so that they can practice in a healthy and safe environment.
Resources
• The Centers for Disease Control and Prevention (CDC), in their “Guidelines for Infection Control in Dental Health-Care Settings, 2003,” reviewed the scientific literature and presented evidence-based recommendations for PPE use and selection (http://www.cdc.gov/Oral Health/infectioncontrol/guidelines/index.htm)
• Organization for Safety and Asepsis Procedures workbook “From Policy to Practice: OSAP’s Guide to the Guidelines.” You can find detailed, easy to use guidance on how to follow the CDC’s Infection Control Guidelines. More information on this resource can be found at http://www.osap.org.