Antral pseudocysts
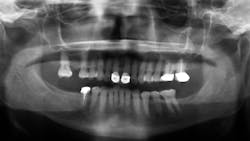
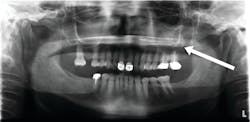
Antral pseudocysts are often discovered on panoramic radiographs during routine examinations. Inflammatory infiltrate causing irritation of the sinus lining is often implicated. They are one of the five most common incidental findings in cone-beam computed tomography.1
It is reported that pseudocysts are found in up to 14% of the population.2 Antral pseudocysts are formed by the inflammatory serous exudate accumulating below the sinus membrane and causing a dome- or sessile-like elevation with a faintly radiopaque and well-delineated dome appearance. Although the cause has not been definitively confirmed, antral pseudocysts have been associated with allergies, respiratory and viral infections, and forced-air heating (figure 1).2
Pseudocysts are not epithelial lined; true cysts are always epithelial lined. In the formation of a true cyst, inflammation is present, such as an infection of the pulp. The epithelium begins to proliferate, forms a distinct cyst, and eventually closes itself off from the surrounding tissue. The lumen, or center, of the cyst fills with fluid due to osmotic pressure in the core of the cyst. The membrane of the cyst allows fluid to enter the cyst core to equalize the osmotic pressure with that of the surrounding tissue, and the cyst continues to expand.3
Antral pseudocysts, on the other hand, are not true cysts and are not often associated with clinical symptoms. Antral pseudocysts arise from the floor of the maxillary sinus and form beneath the mucous membrane, but they are not surrounded by epithelium as a true cyst would be. The term pseudocyst may be confused with the diagnostic terms sinus mucocele and sinus retention cyst.3
A 2014 study of an orthodontic population noted 842 incidental findings in 427 subject cone beam computed tomography scans, with the most missed findings in the nasopharynx and the paranasal sinuses.4 The authors call attention to the need for more training in identifying incidental findings and noting them as they occur. Often, the areas of interest are not overtly apparent or may not be pursued as relevant. The authors recommend proficiency in interpreting all forms of radiographs.
The clinician may confuse the antral pseudocyst with a nonodontogenic cyst, an odontogenic cyst (such as a dentigerous cyst, an odontogenic keratocyst, or a residual cyst), or an inflammatory lesion (such as a radicular cyst, an odontogenic tumor, or a nonodontogenic tumor). When viewing the finding on a panoramic image, the next step is to acquire a periapical image of the area in question. The vitality of any teeth in the area should be determined, and unrestored teeth without evidence of pulpal or periodontal disease should test vital if the area in question is an antral pseudocyst of nondental origin and should allow the elimination of other entities in some cases. However, when the location or the presentation of the entity is in question, further testing is usually needed, such as advanced imaging, biopsy, or fine needle aspiration. Referral to an oral surgeon or an otolaryngologist would be appropriate.5,6
As the saying goes, “the eye does not see what the mind does not know,” and unless you are trained to see the antral pseudocyst, you might miss it or mistake it for another entity. When found inadvertently, a diagnosis should always be pursued.
As always, keep asking good questions and always listen to your patients.
References
1. Edwards R, Altalibi M, Flores-Mir C. The frequency and nature of incidental findings in cone-beam computed tomographic scans of the head and neck region: A systematic review. J Am Dent Assoc. 2013;144(2):161-170.
2. Neville BW, Damm DD, Allen CM, Chi AC. Oral and Maxillofacial Pathology. 4th ed. Philadelphia, PA: Saunders; 2015.
3. DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 3rd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2019.
4. Edwards R, Alsufyani N, Heo G, Flores-Mir C. The frequency and nature of incidental findings in large-field cone beam computed tomography scans of an orthodontic sample. Prog Orthod. 2014;15(1):37.
5. Sette-Dias AC, Naves MD, Mesquita RA, Abdo EM. Differential diagnosis of antral pseudocyst. A case report. Stomatologija. 2013;15(3):92-94.
6. Adibi SS, Johnson CD, Mukherji G, Ogbureke EI. Oral and maxillofacial pathology case of the month: Antral pseudocyst. Tex Dent J. 2015;132(4):240,272-273.
About the Author
Nancy W. Burkhart, EdD, MEd, BSDH, AAFAAOM
NANCY W. BURKHART, EdD, MEd, BSDH, AAFAAOM, is an adjunct professor in the Department of Periodontics-Stomatology, College of Dentistry, Texas A&M University, Dallas, Texas. She is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/) and coauthor of General and Oral Pathology for the Dental Hygienist, now in its third edition. Dr. Burkhart is an academic affiliate fellow with the American Academy of Oral Medicine, where she also serves as chair of the Affiliate Fellowship Program Committee. She was awarded the Dental Professional of the Year in 2017 through the International Pemphigus and Pemphigoid Foundation, and she is a 2017 Sunstar/RDH Award of Distinction recipient. Her professional interests are in the areas of oral medicine and the relationship between oral and whole-body health, with a focus on mucosal disease and early oral cancer detection. Contact her at [email protected].