What’s that pink spot on a tooth?
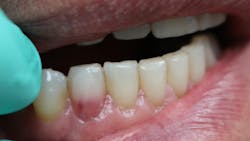
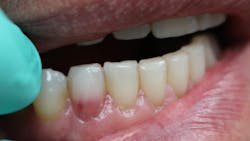
Have you ever laid the patient back, started your examination, and then noticed a tooth that just didn’t look right? You might even question what your eyes are seeing. Does that tooth look pink?
These pink spots are destructive and often insidious types of lesions that can occur either internally or externally on the tooth, resulting in significant loss of tooth structure. Both lesions have to do with a resorptive process that is occurring—often trauma-induced. When you discover these lesions, you can break down the resorptive processes based on their location: external or internal.
External cervical resorption
External cervical resorption (ECR) is a type of external resorption that begins at or near the cementoenamel junction. Typically, patients present asymptomatic, and the lesion is simply discovered on routine exams or at prophylactic appointments. This type of resorption can occur in any type of tooth throughout the mouth. Still, a higher percentage of these lesions is noted in the maxillary anterior teeth and the maxillary and mandibular first molars.
For this type of resorption to occur, some type of damage has happened to the periodontal ligament and protective cemental layer in that area. Factors such as trauma, orthodontics, bleaching, periodontal surgery, and therapy can predispose the patient to this resorptive process.1 Even the transmission of feline herpesvirus and herpes zoster virus has been mentioned as a possible cause.2,3 So don’t forget to check those fur babies, because felines can present with resorptive issues on their teeth too!
ECR can be differentiated from root caries due to its pink hue and tactile sensation. During the examination, you will find that the dentin surrounding an ECR lesion is usually hard, whereas decay/caries typically feels sticky. When a clinician performs probing around this type of lesion, it will typically bleed—often profusely—because of the highly vascular granulation tissue, a result of the resorptive process.
Schwartz et al. described the process, noting that “osteoclasts initially penetrate the tooth through a small entry point and colonize this region. Clastic cells in association with fibrovascular tissue then spread in a circumferential and apicocoronal direction around the root canal system. Numerous irregular resorptive channels are created that can interconnect apically with the periodontal ligament.”4 If caught early enough, removal of the granulation tissue and restoration may be sufficient to resolve the issue. More invasive resorptive processes sometimes involve trichloroacetic acid treatment for the resorptive lesion, root canal therapy, surgery, or even loss of the tooth to correct.5
To aid in deciding upon treatment, Heithersay developed a classification system from 1 to 4 based on the extent of the resorption into the tooth.6,7
- Class 1 is the best situation and is confined to a shallow portion of the dentin around the cervical area. As the resorption increases, so does the extent.
- Class 2 approaches the pulp chamber but shows little involvement into the radicular dentin.
- Class 3 extends more so into the coronal one-third of the root.
- Class 4 extends beyond this area, deeper into the root system.
Typically, class 1–3 lesions can be predictably treated. Class 4, which extends into the radicular dentin, has a poorer long-term prognosis, and extraction is usually the outcome. Technology is making it more straightforward to diagnose and treatment plan with newer classification systems combining CBCT technology now being used as a guide in practice.8
Internal resorption can also result in a pink spot
An internal resorption pink spot was historically referred to as the “pink tooth of Mummery,” named for the anatomist who described the condition. Like an ECRIn order for this type of resorption to occur, some type of damage had to take place inside the predentin layer, with inflammation present. Predisposing factors for this type of resorption include caries, trauma, restorative procedures, and heat. Vital pulp tissue is needed for this type of resorptive process to continue.9
If the lesion becomes significant in size, necrosis of the pulp usually occurs, at which point the patient will begin to have typical pulpitis-related symptoms. Since the vascular tissue becomes necrotic, the tooth’s color may appear darker or gray with discoloration. Root canal therapy will resolve this type of resorptive process. As long as the process has not resorbed a significant portion of the tooth, prognosis is favorable. Repairs can be made with bioceramics, even in situations where the lesion has perforated to the external surface.
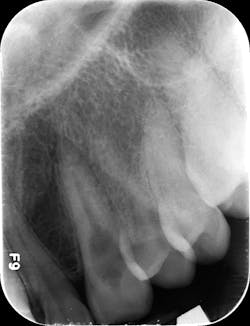
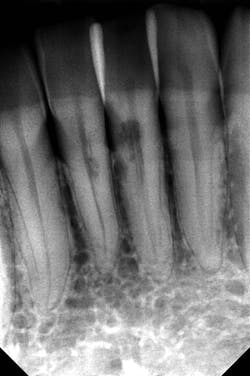
CBCT imaging or taking angled radiographs can help determine which type of resorptive process is being presented. Periapical radiographs are not great at giving you an accurate picture of the lesion’s size,4 but if you discover a possible resorption lesion upon clinical examination, you can use a periapical radiograph to determine if the lesion is indeed external or internal.
Start by taking a baseline radiograph of the lesion using a paralleling technique and a beam-aiming device, such as a Rinn instrument. With your second periapical radiograph, make a mesial horizontal shift with the tube head. If the process is on the tooth’s external surface, the resorptive lesion will move as the radiograph is shifted. Internal resorptive processes will always stay centered in the tooth when the angle is changed (figure 2). With external resorption, one canFinding a “pink spot” during an exam can be a little disheartening. Clinicians never like to deliver bad news or have to prepare a patient for a poor prognosis. Luckily, the incidence of both of these conditions is low; however, early diagnosis and treatment are always best to ensure your patients’ health and retention of their teeth. Cheers!
References
- Patel S, Kanagasingam S, Ford TP. External cervical resorption: a review. J Endod. 2009;35(5):616-625. doi:10.1016/j.joen.2009.01.015
- Solomon CS, Coffiner MO, Chalfin HE. Herpes zoster revisited: implicated in root resorption. J Endod. 1986;12(5):210-213. doi:10.1016/S0099-2399(86)80157-1
- von Arx T, Schawalder P, Ackermann M, Bosshardt DD. Human and feline invasive cervical resorptions: the missing link?—Presentation of four cases. J Endod. 2009;35(6):904-913. doi:10.1016/j.joen.2009.03.044
- Schwartz RS, Robbins JW, Rindler E. Management of invasive cervical resorption: observations from three private practices and a report of three cases. J Endod. 2010;36(10):1721-1730. doi:10.1016/j.joen.2010.06.011
- Patel S, Foschi F, Condon R, Pimentel T, Bhuva B. External cervical resorption: part 2 – management. Int Endod J. 2018;51(11):1224-1238. doi:10.1111/iej.12946
- Heithersay GS. Clinical, radiologic, and histopathologic features of invasive cervical resorption. Quintessence Int. 1999;30(1):27-37.
- Heithersay GS. Invasive cervical resorption: an analysis of potential predisposing factors. Quintessence Int. 1999;30(2):83-95.
- Patel S, Foschi F, Mannocci F, Patel K. External cervical resorption: a three-dimensional classification. Int Endod J. 2018;51(2):206-214. doi:10.1111/iej.12824
- Patel S, Ricucci D, Durak C, Tay F. Internal root resorption: a review. J Endod. 2010;36(7):1107-1121. doi:10.1016/j.joen.2010.03.014
- Gartner AH, Mack T, Somerlott RG, Walsh LC. Differential diagnosis of internal and external root resorption. J Endod. 1976;2(11):329-334. doi:10.1016/S0099-2399(76)80071-4
MICHELLE STRANGE, MSDH, RDH, has been a dental clinician since 2000 and is currently a practicing hygienist, speaker, writer, content developer, consultant, and podcast cohost for A Tale of Two Hygienists. With a master’s in dental hygiene education and a belief in lifelong learning, she hopes to continue to learn and grow within the dental profession and one day see the gap bridged between medicine and dentistry.
THEODORE RAVENEL, DMD, has been practicing endodontics since 2004. He is the current postgraduate program director for the Medical University of South Carolina and a diplomate of the American Board of Endodontics.
About the Author
Michelle Strange, RDH
Michelle Strange, RDH, is a dedicated dental hygienist and educator passionate about infection control and patient safety. With over 20 years of experience in clinical practice, Michelle is committed to sharing evidence-based solutions to improve dental care outcomes.

Theodore Ravenel, DMD
Theodore Ravenel, DMD, has been practicing endodontics since 2004. He is the current postgraduate program director for the Medical University of South Carolina and a diplomate of the American Board of Endodontics.